Abstract
Background
Both child temperament (specifically high shyness and fear) and environmental stressors like the COVID-19 pandemic are known to confer risk for elevated anxiety symptoms in children. However, few studies have examined the long-term impact of the pandemic on young children’s anxiety.
Objective
We examined the moderating effects of disruptions experienced during the early months of the pandemic on the longitudinal association between shy and fearful temperament at age 2 pre-pandemic and anxiety symptoms in the year following the start of the pandemic.
Methods
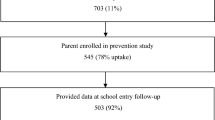
Participants were 125 parents of toddlers (Mage = 26 months, 54% girls, 80% White) who were participating in an ongoing anxiety screening study when the pandemic started in 2020. Shy and fearful temperament were assessed pre-pandemic at age 2 years using the Early Childhood Behavior Questionnaire and anxiety symptoms were assessed within the first post-pandemic year (at ages 3 or 4) using the Spence Preschool Anxiety Scale. Parents completed the Epidemic-Pandemic Impacts Inventory at the start of the pandemic to assess types of disruptions experienced.
Results
Shyness predicted higher anxiety symptoms among children whose parents experienced more work-related disruptions. Fear was associated with higher anxiety symptoms at lower levels of social activities disruption but was unrelated to anxiety symptoms at high levels of these disruptions.
Conclusions
Results suggest that anxious temperament may serve as a meaningful screening target for identifying the children most in need of support during times of major stress.


Similar content being viewed by others
References
Abel, M. R., Vernberg, E. M., Lochman, J. E., McDonald, K., Jarrett, M., Powell, N., & Hendrickson, M. (2020). Co-reminiscing with a caregiver about a devastating tornado: Association with adolescent anxiety symptoms. Journal of Family Psychology, 34(7), 846–856. https://doi.org/10.1037/fam0000683.
Abel, M. R., Hambrick, E., & Vernberg, E. M. (2021). Talking with children about natural disasters: The link between maternal acknowledgment and youth posttraumatic stress symptoms. Child & Youth Care Forum, 50(6), 947–968. https://doi.org/10.1007/s10566-021-09605-5.
Adegboye, D., Williams, F., Collishaw, S., Shelton, K., Langley, K., Hobson, C., Burley, D., & van Goozen, S. (2021). Understanding why the COVID-19 pandemic-related lockdown increases mental health difficulties in vulnerable young children. JCPP Advances, 1, e12005. https://doi.org/10.1111/jcv2.12005.
Alves, J. M., Yunker, A. G., DeFendis, A., Ziang, A. G., & Page, K. A. (2021). BMI status and associations between affect, physical activity and anxiety amount U.S. children during COVID-19. Pediatric Obesity, 16(9), e12786. https://doi.org/10.1111/ijpo.12786.
Athavale, P., Kumar, V., Clark, J., Mondal, S., & Sur, S. (2021). Differential impact of COVID- 19 risk factors on ethnicities in the United States. Frontiers in Public Health, 9, 1–16. https://doi.org/10.3389/fpubh.2021.743003.
Benga, O., Tincas, I., & Visu-Petra, L. (2010). Investigating the structure of anxiety symptoms among Romanian preschoolers using the Spence Preschool anxiety scales. Cognition Brain & Behavior, 14(2), 159–182.
Biederman, J., Hirshfeld-Becker, D. R., Rosenbaum, J. F., Herot, C., Friedman, D., Snidman, N., Kagan, J., & Faraone, S. V. (2001). Further evidence of association between behavioral inhibition and social anxiety in children. The American Journal of Psychiatry, 158, 1673–1679. https://doi.org/10.1176/appi.ajp.158.10.1673.
Blöte, A. W., Miers, A. C., Van den Bos, E., & Westenberg, P. M. (2019). Negative social self-cognitions: How shyness may lead to social anxiety. Journal of Applied Developmental Psychology, 63, 9–15. https://doi.org/10.1016/j.appdev.2019.05.003.
Bonanno, G. A., Brewin, C. R., Kaniasty, K., & La Greca, A. M. (2010). Weighing the costs of disaster: Consequences, risks, and resilience in individuals, families, and communities. Psychological Science in the Public Interest, 11(1), 1–49. https://doi.org/10.1177/1529100610387086.
Brown, S. M., Doom, J. R., Lechuga-Pena, S., Watamura, S. E., & Koppels, T. (2020). Stress and parenting during the global COVID-19 pandemic. Child Abuse & Neglect, 110(2), 104699. https://doi.org/10.1016/j.chiabu.2020.104699.
Brownell, C. A., Svetlova, M., Anderson, R., Nichols, S. R., & Drummond, J. (2012). Socialization of early prosocial behavior: Parents’ talk about emotions is associated with sharing and helping in toddlers. Infancy, 18(1), 91–119. https://doi.org/10.1111/j.1532-7078.2012.00125.x.
Buss, K. A. (2011). Which fearful toddlers should we worry about? Context, fear regulation, and anxiety risk. Developmental Psychology, 47, 804–819. https://doi.org.19.1937/a0023227.
Buss, K. A., & McDoniel, M. E. (2016). Improving the prediction of risk for anxiety development in temperamentally fearful children. Current Directions in Psychological Science, 25(1), 14–20. https://doi.org/10.1177/0963721415611601.
Buss, K. A., Cho, S., Morales, S., McDoniel, M., Webb, A. F., Schwartz, A., Cole, P. M., Dorn, L. D., Gest, S., & Teti, D. M. (2021). Toddler dysregulated fear predicts continued risk for social anxiety symptoms in early adolescence. Development and Psychopathology, 33(1), 252–263. https://doi.org/10.1017/S0954579419001743.
Chronis-Tuscano, A., Degnan, K. A., Pine, D. S., Perez-Edgar, K., Henderson, H. A., Diaz, Y., Raggi, V. L., & Fox, N. A. (2009). Stable early maternal report of behavioral inhibition predicts lifetime social anxiety disorder in adolescence. Journal of the American Academy of Child & Adolescent Psychiatry, 48(9), 928–935. https://doi.org/10.1097/CHI.0b013e3181ae09df.
Cobham, V. E., McDermott, B., Haslam, D., & Sanders, M. R. (2016). The role of parents, parenting and the family environment in children’s post-disaster mental health. Current Psychiatry Reports, 18(6), 53. https://doi.org/10.1007/s11920-016-0691-4.
Cohodes, E. M., McCauley, S., & Gee, D. G. (2021). Parental buffering of stress in the time of COVID-19: Family-level factors may moderate the association between pandemic-related stress and youth symptomatology. Research on Child and Adolescent Psychopathology, 49, 935–948. https://doi.org/10.1007/s10802-020-00732-6.
Davidson, B., Schmidt, E., Mallar, C., Mahmound, F., Rothenberg, W., Hernandez, J., Berkovits, M., Jent, J., Delamater, A., & Natale, R. (2021). Risk and resilience of well-being in caregivers of young children in response to the COVID-19 pandemic. Translational Behavioral Medicine, 11(2), 305–313. https://doi.org/10.1093/tbm/ibaa124.
Ellis, W. E., Dumas, T. M., & Forbes, L. M. (2020). Physically isolated by socially connected: Psychological adjustment and stress among adolescents during the initial COVID-19 crisis. Canadian Journal of Behavioural Science, 52(3), 177–187. https://doi.org/10.1037/cbs0000215.
Eustis, E. H., Cardona, N., Nauphal, M., Sauer-Zavala, S., Rosellini, A. J., Farchione, T. J., & Barlow, D. H. (2020). Experiential avoidance as a mechanism of change across cognitive-behavioral therapy in a sample of participants with heterogeneous anxiety disorders. Cognitive Therapy and Research, 44, 275–286. https://doi.org/10.1007/s10608-019-10063-6.
Felix, E., Hernández, L. A., Bravo, M., Ramirez, R., Cabiya, J., & Canino, G. (2011). Natural disaster and risk of psychiatric disorders in Puerto Rican children. Journal of Abnormal Child Psychology, 39, 589–600. https://doi.org/10.1007/s10802-010-9483-1.
Felix, E., You, S., Vernberg, E., & Canino, G. (2013). Family influences on the long-term post disaster recovery of Puerto Rican youth. Journal of Abnormal Child Psychology, 41, 111–124. https://doi.org/10.1007/s10802-012-9654-3.
Fox, N. A. (2004). Temperament and early experience form social behavior. Annals of the New York Academy of Sciences, 1038(1), 171–178. https://doi.org/10.1196/annals.1315.025.
Gassman-Pines, A., Ananat, E. O., & Fitz-Henley, J. (2020). COVID-19 and parent-child psychological well-being. Pediatrics, 146(4), e2020007294. https://doi.org/10.1542/peds.2020-007294.
Gil-Rivas, V., Silver, R. C., Holman, E. A., McIntosh, D. N., & Poulin, M. (2007). Parental response and adolescent adjustment to the September 11, 2001 terrorist attacks. Journal of Traumatic Stress, 20(6), 1063–1068. https://doi.org/10.1002/jts.20277.
Gilbert, R., Abel, M. R., Vernberg, E. M., & Jacobs, A. K. (2021). The use of Psychological First Aid in children exposed to mass trauma. Current Psychiatry Reports, 23, 53–62. https://doi.org/10.1007/s11920-021-01270-8.
Goldsmith, H. H., & Lemery, K. S. (2000). Linking temperamental fearfulness and anxiety symptoms: A behavior-genetic perspective. Biological Psychiatry, 48(12), 1199–1209. https://doi.org/10.1016/S0006-32230001003-9.
Grasso, D. J., Briggs-Gowan, M. J., Carter, A. S., Goldstein, B., & Ford, J. D. (2020). A person -centered approach to profiling COVID-related experiences in the United States: Preliminary findings from the Epidemic-Pandemic Impacts Inventory. https://doi.org/10.31234/osf.io/v36hj.
Hendrickson, M., Abel, M. R., Vernberg, E., McDonald, K., & Lochman, J. (2020). Caregiver adolescent co-reminiscing and adolescents’ individual recollections of a devastating tornado: Associations with enduring post-traumatic stress symptoms. Development and Psychopathology, 32(1), 151–161. https://doi.org/10.1017/S0954579418001487.
Hirshfeld, D. R., Rosenbaum, J. F., Biederman, J., Bolduc, E. A., Faraone, S. V., Snidman, N., Reznick, J. S., & Kagan, J. (1992). Stable behavioral inhibition and its association with anxiety disorder. Journal of the American Academy of Child & Adolescent Psychiatry, 31(1), 103–111. https://doi.org/10.1097/00004583-1992201000-00016.
Hirshfeld-Becker, D. R., Biederman, J., Henin, A., Faraone, S. V., Davis, S., Harrington, K., & Rosenbaum, J. F. (2007). Behavioral inhibition in preschool children at risk is a specific predictor of middle childhood social anxiety: A five-year follow-up. Journal of Developmental Behavioral Pediatrics, 28(3), 225–233. https://doi.org/10.1097/01.DBP.0000268559.34463.d0.
Hirshfeld-Becker, D. R., Micco, J. A., Simoes, N. A., & Henin, A. (2008). High risk studies and developmental antecedents of anxiety disorders. American Journal of Medical Genetics: Seminars in Medical Genetics, 148(2), 99–117. https://doi.org/10.1002/ajmg.c.30170.
Hudson, J. L., Dodd, H. F., & Bovopoulos, N. (2011). Temperament, family environment, and anxiety in preschool children. Journal of Abnormal Child Psychology, 39(7), 939–951. https://doi.org.10.1007/s10802-011-9502-x.
Hudson, J. L., Murayama, K., Meteyard, L., Morris, T., & Dodd, H. F. (2019). Early childhood predictors of anxiety in early adolescence. Journal of Abnormal Child Psychology, 47, 1121–1133. https://doi.org/10.1007/s10802-018-0495-6.
Kagan, J., Snidman, N., Kahn, V., & Towsley, S. (2007). The preservation of two infant temperaments into adolescence. Monographs of the Society for Research in Child Development, 72(2), 1–75.
Katikireddi, S. V., Lal, S., Carrol, E. D., Niedzwiedz, C. L., Khunti, K., Dundas, R., & Barr, B. (2021). Unequal impact of the COVID-19 crisis on minority ethnic groups: A framework for understanding and addressing inequalities. Journal of Epidemiological Community Health, 75(10), 970–974.
Kerr, M. L., Fanning, K. A., Huynh, T., Botto, I., & Kim, C. N. (2021). Parents’ self-reported psychological impacts of COVID-19: Associations with parental burnout, child behavior, and income. Journal of Pediatric Psychology, 46, 1162–1171. https://doi.org/10.1093/kpedpsy/jsab089.
Kline, R. B. (2016). Principles and practice of structural equation modeling (4th ed.).). The Guildford Press.
Kohler-Dauner, F., Clemens, V., Lange, S., Ziegenhain, U., & Fegert, J. M. (2021). Mothers’ daily perceived stress influences their children’s mental health during SARS-CoV-2- pandemic—an online survey. Child and Adolescent Psychiatry and Mental Health, 15, 1–31. https://doi.org/10.1186/s13034-021-00385-3.
Kourti, A., Stavridou, A., Panagouli, E., Psaltopoulou, T., Tsolia, M., Sergentanis, T. N., & Tsitsika, A. (2021). Play behaviors in children during the COVID-19 pandemic: A review of the literature. Children, 8, 706. https://doi.org/10.3390/children8080706.
La Greca, A. M., Lai, B. S., Llabre, M. M., Silverman, W. K., Vernberg, E. M., & Prinstein, M. J. (2013). Children’s postdisaster trajectories of PTS symptoms: Predicting chronic distress. Child & Youth Care Forum, 42(4), 351–369. org/https://doi.org/10.1007/s10566-013-9206-1.
Lai, B. S., Lewis, R., Livings, M. S., La Greca, A. M., & Esnard, A. M. (2017). Posttraumatic stress symptom trajectories among children after disaster exposure: A review. Journal of Traumatic Stress, 30(6), 571–582. https://doi.org/10.1002/jts.22242.
Lai, B. S., Osborne, M. C., Piscitello, J., Self-Brown, S., & Kelley, M. L. (2018). The relationship between social support and posttraumatic stress symptoms among youth exposed to a natural disaster. European Journal of Psychtraumatology, 9(sup2), 1450042. https://doi.org/10.1080/2008198.2018.1450042.
Lemstra, M., Neudorf, C., D’Arcy, C., Kunst, A., Warren, L. M., & Bennett, N. R. (2008). A systematic review of depressed mood and anxiety by SES in youth aged 10–15 years. Canadian Journal of Public Health, 99, 125–129. https://doi.org/10.1007/BF03405459.
Masarik, A. S., & Conger, R. D. (2017). Stress and child development: A review of the family stress model. Current Opinions in Psychology, 13, 85–90. https://doi.org/10.1016/j.copsyc.2015.05.008.
Masten, A. S., & Narayan, A. J. (2012). Child development in the context of disaster, war, and terrorism: Pathways of risk and resilience. Annual Review of Psychology, 63(1), 227–257. https://doi.org/10.1146/annurev-psych-120710-100356.
McArthur, B. A., Racine, N., McDonald, S., Tough, S., & Madigan, S. (2021). Child and family factors associated with child mental health and well-being during COVID-19. European Child & Adolescent Psychiatry, 32, 223–233. https://doi.org/10.1007/s00787-021-01849-9.
McDonald, K., Vernberg, E., Lochman, J. E., Abel, M. R., Jarrett, M., Kassing, F., et al. (2019). Trajectories of tornado-related post-traumatic stress symptoms and pre-exposure predictors in a sample of at-risk youth. Journal of Consulting and Clinical Psychology, 87(11), 1003–1018. https://doi.org/10.1037/ccp0000432.
McNeely, C. L., Schintler, L. A., & Stabile, B. (2020). Social determinants and COVID-19 disparities: Differential pandemic effects and dynamics. World Medical & Health Policy, 12(3), 206–217. https://doi.org/10.1002/wmh3.370.
Ng, C. S. M., & Ng, S. S. L. (2022). Impact of the COVID-19 pandemic on children’s mental health: A systematic review. Frontiers in Psychiatry, 13, 975936. https://doi.org/10.3389/fpsyt.2022.975936.
Ollendick, T. H., & Hirshfeld-Becker, D. R. (2002). The developmental psychopathology of social anxiety disorder. Biological Psychiatry, 51, 44–58. https://doi.org/10.1016/S0006-32230101305-1.
Patrick, S. W., Henkhaus, L. E., Zickafoose, J. S., Lovell, K., Halvorson, A., Loch, S., Letterie, M., & Davis, M. M. (2020). Well-being of parents and children during the COVID-19 pandemic: A national survey. Pediatrics, 146(4), e2020016824. https://doi.org/10.1542/peds.2020.016824.
Paulus, M. (2014). The emergence of prosocial behavior: Why do infants and toddlers help, comfort, and share? Child Development Perspectives, 8(2), 77–81. https://doi.org/10.1111/cdep.12066.
Prior, M., Smart, D., Sanson, A. N. N., & Oberklaid, F. (2000). Does shy-inhibited temperament in childhood lead to anxiety problems in adolescence? Journal of the American Academy of Child & Adolescent Psychiatry, 39(4), 461–468. https://doi.org/10.1097/00004583-200004000-00015
Puttnam, S. P., Gartstein, M. A., & Rathbart, M. K. (2006). Measurement of fine-grained aspects of toddler temperament: The early childhood Behavior Questionnaire. Infant Behavior and Development, 29(3), 386–401. https://doi.org/10.1002/icd.582.
Racine, N., McArthur, B. A., Cooke, J. E., Eirich, R., Zhu, J., & Madigan, S. (2021). Global prevalence of depressive and anxiety symptoms in children and adolescents during COVID-19: A meta-analysis. JAMA Pediatrics, 175(11), 1142–1150. https://doi.org/10.1001/jamapediatriacs.2021.2481.
Robertson, E. L., Piscitello, J., Schmidt, E., Mallar, C., Davison, B., & Natale, R. (2021). Longitudinal transactional relationships between caregiver and child mental health during the COVID-19 global pandemic. Child and Adolescent Psychiatry and Mental Health, 15, 66. https://doi.org.10.1186/s13034-021-00422-1.
Rothbart, M., Ahadi, S., & Hershey, K. (1994). Temperament and social behavior in childhood. Merrill-Palmer Quarterly, 40(1), 21–29.
Rubens, S., Felix, L., D, E., & Hambrick, E. (2018). A meta-analysis of the impact of natural disasters on internalizing and externalizing problems in youth. Journal of Traumatic Stress, 31(3), 332–341. https://doi.org/10.1002/jts.22292.
Samji, H., Wu, J., Ladak, A., Vossen, C., Stewart, E., Dove, N., Long, D., & Snell, G. (2022). Mental health impacts of the COVID-19 pandemic on children and youth: A systematic review. Child and Adolescent Mental Health, 27(2), 173–189. https://doi.org/10.1111/camh.12501.
Schwartz, C. E., Snidman, N. S., & Kagan, J. (1999). Adolescent social anxiety as an outcome of inhibited temperament in childhood. Journal of the American Academy of Child and Adolescent Psychiatry, 38(8), 1008–1015. https://doi.org/10.1097/00004583-199908000-00017.
Spence, S. H., Rapee, R., McDonald, C., & Ingram, M. (2001). The structure of anxiety symptoms among preschoolers. Behaviour Research and Therapy, 39(11), 1293–1316. https://doi.org/10.1016/s0005-79670000098-x.
Spence, S. H., Najman, J. M., Bor, W., O’Callaghan, M. J., & Williams, G. M. (2002). Maternal anxiety and depression, poverty and marital relationship factors during early childhood as predictors of anxiety and depressive symptoms in adolescence. Journal of Child Psychology and Psychiatry, 43(4), 457–469. https://doi.org/10.1111/1469-7610.00037.
United Nations Office for Disaster Risk Reduction (UNISDR) (2019). Global Assessment Report on Disaster Risk Reduction Geneva, Switzerland. Retrieved from https://www.undrr.org/publication/global-assessment-report-disaster-risk-reduction-2019.
Vernberg, Hambrick, E. P., Cho, B., & Hendrickson, M. L. (2016). Positive psychology and disaster mental health: Strategies for working with children and adolescents. Journal of Clinical Psychology, 72(12), 1333–1347. https://doi.org/10.1002/jclp.22289.
Volbrecht, M. M., & Goldsmith, H. H. (2010). Early temperamental and family predictors of shyness and anxiety. Developmental Psychology, 46(5), 192–1205. https://doi.org/10.1037/a0020616.
Walsh, K., Furey, W. J., & Malhi, N. (2021). Narrative review: COVID-19 and pediatric anxiety. Journal of Psychiatric Research, 144, 421–426. https://doi.org/10.1016/j.jpsychires.2021.10.013.
Wang, M., & Zhao, J. (2015). Anxiety disorder symptoms in Chinese preschool children. Child Psychiatry & Human Development, 46(1), 158–166. https://doi.org/10.1007/s10578-014-0461-7.
Weems, C. F. (2015). Biological correlates of child and adolescent responses to disaster exposure: A bio-ecological model. Current Psychiatry Report, 17(7), 51–58. https://doi.org/10.1007/s11920-015-0588-7.
Zdebik, B. M., Battaglia, M., Tremblay, R. E., Falissard, B., & Cote, S. M. (2019). Childhood multi-trajectories of shyness, anxiety, and depression: Associations with adolescent internalizing problems. Journal of Applied Developmental Psychology, 64, 101050. https://doi.org/10.1016/j.appdev.2019.101050.
Zhang, X., Zhu, W., Kang, S., Qiu, L., Lu, Z., & Sun, Y. (2020). Association between physical activity and mood states of children and adolescents in social isolation during the COVID-19 pandemic. International Journal of Environmental Research and Public Health, 17(2), 7666. https://doi.org/10.3390/ijerph17207666.
Acknowledgements
The research in this paper was supported by a philanthropic donation by Mrs. Eleanor Spencer.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional review board at Massachusetts General Hospital and conducted in accordance with the ethical standards of the American Psychological Association.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Competing Interests
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Abel, M.R., Dai, Y.G., Henin, A. et al. Exposure to COVID-19 Disruptions Moderates the Effect of Temperament on Anxiety in Preschool-Age Children. Child Youth Care Forum (2024). https://doi.org/10.1007/s10566-024-09794-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s10566-024-09794-9