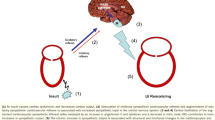
Abstract
Bisoprolol and nebivolol are highly selective β1-adrenoceptor antagonists, with clinical indications in many countries within the management of heart failure with reduced left ventricular ejection fraction (HFrEF), ischaemic heart disease (IHD), and hypertension. Nebivolol has additional vasodilator actions, related to enhanced release of NO in the vascular wall. In principle, this additional mechanism compared with bisoprolol might lead to more potent vasodilatation, which in turn might influence the effectiveness of nebivolol in the management of HFrEF, IHD and hypertension. In this article, we review the therapeutic properties of bisoprolol and nebivolol, as representatives of “second generation” and “third generation” β-blockers, respectively. Although head-to-head trials are largely lacking, there is no clear indication from published studies of an additional effect of nebivolol on clinical outcomes in patients with HFrEF or the magnitude of reductions of BP in patients with hypertension.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction: differentiating between individual β-blockers
A variety of different therapeutic mechanisms exist within the β-blocker class. The prototype β-blocker, propranolol, and later agents such as bucindolol, carvedilol, labetolol, oxprenolol, nadolol, pindolol, sotalol, and timolol, do not demonstrate clinically significant differences in their selectivity for β1 and β2 adrenoreceptors [1,2,3,4]. By contrast, other β-blockers (e.g. acebutolol, atenolol, betaxolol, bisoprolol, celiprolol, esmolol, metoprolol, nebivolol, and xamoterol) are more or less selective for blockade of the β1 adrenoceptors found mainly in the heart over blockade of the β2 receptors that contribute to dilation of vascular and airway smooth muscle [1,2,3,4]. Some β-blockers (e.g. celiprolol, pindolol, acebutolol, and oxprenolol) induce some activation of β1-receptors (“intrinsic sympathomimetic activity” [ISA]), which tends to limit reductions in myocardial performance and heart rate during β-blockade, and reduces the potential for peripheral vasoconstriction, if directed against peripheral β2 adrenoreceptors [5]. The presence of ISA vs. no ISA does not appear to confer clinical benefit in patients with ischaemic heart disease (IHD) [6] or heart failure with reduced left ventricular ejection fraction (HFrEF) [7], however.
Other vasodilatory mechanisms expressed by individual β-blockers are additional blockade of α-adrenoceptors (bucindolol, carvedilol, celiprolol, labetalol) [1, 5, 8, 9], or promotion of release of nitric oxide (NO); by nebivolol, secondary to activation of β3-adrenoceptors nebivolol) [10,11,12]. These groups of β-blockers have been described as “first generation” (non-selective), “second generation” cardio/β1-selective, and “third generation” (with additional vasodilatory properties) [13].
Purpose of this review
The differences between individual β-blockers, in terms of their mechanisms, selectivity and pharmacokinetic properties (among others) both facilitate to and complicate the design of individualised regimens for people with cardiovascular diseases [14, 15]. The purpose of our narrative review is to compare the therapeutic properties of a second generation and third generation cardioselective β-blocker in patients with hypertension, IHD and HFrEF. It is important to note that agents with lower β1-selectivity begin to block β2-adrenoceptors at higher doses (e.g. the European Summary of Product Characteristics for atenolol notes in this context that “selectivity decreases with increasing dose”). Accordingly, we have chosen two of the most highly selective β-blockers for this purpose, bisoprolol (second generation) and nebivolol (third generation).
Methods
The review is based on literature searches for research articles with “bisoprolol” or “nebivolol” in the title. Priority is given to inclusion of randomised, active-controlled trials, given the extensive database of literature on β-blockers (placebo-controlled outcomes trials are included, as head-to-head comparative studies powered for clinical outcomes are lacking). References identified within these articles are also used in some cases. In each section, any available head-to-head comparisons between these agents will be reviewed first, followed by randomised, controlled comparisons of bisoprolol with nebivolol, as per above, with the structure of each subsection determined by the published evidence available. Other clinical trial evidence with bisoprolol or nebivolol is included at lower priority, where this sheds light on the overall therapeutic properties of these β-blockers.
Properties of bisoprolol and nebivolol
Relative selectivity for blockade of β1- vs. other adrenoceptors
Selectivity for the β1 adrenoreceptor has emerged as a key property within the β-blocker class, as described above and summarised in Table 1 [16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45]. Studies of the β1- vs. β2-adrenoceptor selectivity of bisoprolol and nebivolol have provided conflicting results. Nebivolol was found to be about threefold more selective than bisoprolol for the β1- vs. β2-adrenoceptor in human myocardium [46, 47], with similar findings reported from a study in humans which measured the effects of selective β-blockers on physiological responses to the β2-adrenoceptor agonist, terbutaline (both were more β1-selective than atenolol) [48]. However, other studies in human myocardium or cultured cells expressing human β1- or β2-adrenoceptorsfound that bisoprolol was more β1-selective than nebivolol [49]. An experimental study showed that bisoprolol and xamoterol were about 14-fold selective for the human β1- vs. the β2-adrenoceptor, compared with lower ratios for atenolol (~ fivefold), acebutolol and metoprolol (~ twofold) [50].
The heart also contains β3-adrenoceptors. Binding studies showed that bisoprolol was 31-fold selective for blockade of β1-adrenoceptors vs. β3-adrenoceptors [51]. Nebivolol is a partial agonist at β3-receptors (see below).
Intrinsic sympathomimetic activity
A number of β-blockers demonstrate intrinsic sympathomimetic activity, i.e. they have partial agonist activity at different β-adrenoceptors [52,53,54,55]. Neither bisoprolol nor nebivolol has intrinsic sympathomimetic activity at the β1- or β2-adrenoceptor [52,53,54,55].
Nebivolol (but not bisoprolol) exerts intrinsic sympathomimetic activity at the β3-adrenoceptor, which is associated with a vasodilator action secondary to increased production of nitric oxide [12, 56, 57]. This action may account for observations of a lesser effect of nebivolol in reducing heart rate, compared with bisoprolol (see below) [51, 55, 56, 58].
Inverse agonism at the β1-adrenoceptor
Constitutive activity (some level of activation of a receptor in the absence of its specific agonist) has been demonstrated for β1-adrenoceptors [59]. An inverse β1 agonist can suppress the level of activation of a receptor to a level below that seen in the absence of an agonist [59]. Both bisoprolol and nebivolol are inverse agonists at the β1- receptor (as are most β1-adrenoceptor blockers [49, 56]); however, the level of inverse agonism of these drugs appears to be similar and therefore unlikely to contribute to differences in their therapeutic actions [49]. The phenomenon of inverse agonism has been associated with prevention of desensitisation of receptors, and thus with increased numbers of β1-adrenoceptors [56]. While this is of theoretical benefit in the setting of HFrEF, variations in the ability of different β-blockers to upregulate β1-adrenoceptor numbers have not been associated with differences in their beneficial effects on cardiac performance [56].
Other sympatholytic actions
β-blockers are sympatholytic, in that they inhibit the actions of the sympathetic neurotransmitters at the level of the β-adrenoceptors [51,52,53,54,55]. Additional mechanisms may be at play, including blockade of α-adrenoceptors (labetalol, carvedilol), modulation of baroreflex function, effects on presynaptic β1-adrenoceptors that modulate sympathetic neurotransmitter release, or actions to limit sympathetic outflow from the brain (for lipophilic agents that cross the blood–brain barrier) [52,53,54,55].
Pharmacokinetics
Table 2 summarises the pharmacokinetics of bisoprolol and nebivolol [12, 60,61,62,63]. Both drugs have elimination half life (T½) consistent with once-daily dosing, and are absorbed relatively rapidly. Nebivolol, but not bisoprolol, is subject to an extensive, but variable, first pass metabolism, with potential for pharmacokinetic interactions with other inhibitors of CYP450 2D6 noted in the European labelling for nebivolol. Differences in the rate of metabolism of nebivolol between individuals affect the pharmacokinetics of nebivolol, with longer time to maximal plasma concentration (Tmax) and a longer T½. In addition, there is a ~ eightfold difference in bioavailability and ~ 15-fold difference in exposure to nebivolol between extensive and poor metabolisers of the drug, and the mode of elimination differs according to metaboliser phenotype. The level of overall β1-blockade is similar between these metaboliser phenotypes following a dose of nebivolol; however, due to the greater presence of active metabolites of nebivolol in extensive metabolisers. Nebivolol is almost completely protein bound, compared with only about 30% for bisoprolol.
Variations in renal function have been observed to contribute to variability of plasma concentrations of orally-administered bisoprolol in a population with diabetes, and it may be useful to measure renal function to support individualised dosing with bisoprolol [64]. Another study analysed 31 covariates and found that only higher bisoprolol doses and cigarette smoking (both of which were postulated to induce enzymes in the cytochrome P450 system) influenced the PK of bisoprolol [65].
The pharmacokinetic profile of nebivolol is therefore complex, compared with bisoprolol. A recent study showed that exposure to nebivolol (and metoprolol, propranolol, and carvedilol) in pharmacokinetic studies was more variable than exposure to bisoprolol (and atenolol, sotalol, labetalol, nadolol, and pindolol), based on the coefficient of variation of the area under the plasma-concentration–time curve after oral dosing of these drugs [66].
Genome-wide association studies (GWAS) have demonstrated an association between effects on blood pressure of β-blockers in general and single nucleotide polymorphisms (SNPs) in the BST1 or PTPRD gene, although there was no suggestion of differences between the antihypertensive efficacy of individual β-blockers according to the presence or absence of this mutation [67, 68]. It has also been suggested that common variations in the enzyme CYP2D6 may alter the efficacy of safety of metoprolol to a significant extent in patients in certain geographical regions. This may be expected to hold true also for other β-blockers subjected to extensive metabolism by the cytochrome P450 system [69]. One GWAS identified SNPs in three genes that appeared to modulate the antihypertensive response to bisoprolol but not to atenolol, although the functional significance of this is unclear at present [70]. Elsewhere, a SNP (Arg189Gly) influenced heart rate responses to carvedilol, but not to bisoprolol [71].
Bisoprolol and nebivolol in heart failure
Randomised head-to-head comparisons and meta-analyses
A randomised crossover study evaluated 2 months treatment with each of carvedilol, bisoprolol and nebivolol in 61 patients with HFrEF of moderate severity [72]. There were some differences between groups in oxygen perfusion and response to hypoxia, in which the authors considered could contribute to individualised patient care, but there were no significant differences between treatments for NYHA classification, Minnesota heart failure questionnaire scores, renal function, levels of B-type natriuretic peptide, echocardiography findings, or lung mechanics. One small study showed that treatment for 2 weeks with nebivolol increased left ventricular function in comparison with bisoprolol, celiprolol or carvedilol, in healthy volunteers, apparently associated with improved diastolic function and myocardial compliance, although the relevance of this study to patients with HFrEF is unclear [73].
A network meta-analysis of outcomes trials in HFrEF [74]included the CIBIS trials with bisoprolol [75,76,77] and the SENIORS trial with nebivolol [78] (see below for more details of these trials). There was no significant difference between bisoprolol and nebivolol for effects on overall mortality, cardiovascular mortality, or sudden death (Fig. 1).
Comparison of the effects of bisoprolol and nebivolol on mortality outcomes from a network meta-analysis. Odds ratios < 1 favour bisoprolol. Drawn from data presented in reference [74]
Other randomised outcomes trials
No randomised, head-to-head outcomes trials have compared bisoprolol and nebivolol in patients with HFrEF. Accordingly, this section reviews briefly the outcomes trials that have been conducted separately with these agents.
Three randomised outcomes trials [75,76,77] have evaluated bisoprolol in comparison with placebo (each plus standard of care) in patients with HFrEF (Table 3). The first of these, the Cardiac Insufficiency Bisoprolol Study (CIBIS) trial demonstrated symptomatic improvement in patients randomised to bisoprolol vs. placebo, but the small patient population precluded demonstration of improved clinical outcomes [75]. CIBIS II recruited a larger population, and this trial concluded prematurely following the emergence of a significant reduction in mortality (the primary outcome of the trial) in the bisoprolol vs. placebo group [76]. Post-hoc analyses from these trials showed that outcome benefits were similar whether or not patients had diabetes, renal impairment, or NYHA class IV symptoms, were elderly, or were also receiving digitalis, amiodarone or aldosterone antagonists [79].
The third trial, CIBIS III, was designed to evaluate whether starting therapy with bisoprolol and then adding enalapril was superior to starting with enalapril and subsequently adding bisoprolol [77]. There were no differences in clinical outcomes between either method of achieving this evidence-based combination. However, a post-hoc analysis of CIBIS III showed that titration of either therapy to at least half-maximal dose was more likely for the treatment that was prescribed first, suggesting that education of physicians on optimisation of heart failure therapies is required [80].
The Study of the Effects of Nebivolol Intervention on Outcomes and Rehospitalization in Seniors with Heart Failure (SENIORS) trial evaluated nebivolol in an elderly population with heart failure (Table 3) [78, 81]. Randomisation to nebivolol vs. placebo for an average of 21 months significantly reduced the risk of the primary composite endpoint (all cause mortality or cardiovascular hospital admission) vs. placebo, and this effect was independent of gender, age or LVEF. There was no significant effect on all-cause mortality, a secondary endpoint, however. Sub-analyses from SENIORS showed that nebivolol improved clinical outcomes similarly in patients with and without moderate renal dysfunction [81], or low SBP at baseline, a risk factor for adverse clinical outcomes in this population [82].
Bisoprolol and nebivolol in ischaemic heart disease
Randomised outcomes trials
No outcome trial has compared bisoprolol with nebivolol directly in patients with IHD. The Total Ischemic Burden Bisoprolol Study randomised 330 patients with CHD (defined as stable angina, a positive exercise test and at ≥ 2 transient episodes of myocardial ischaemia during 48 h of ambulatory ECG recording) to bisoprolol or nifedipine [83, 84]. Bisoprolol reduced the number of episodes of ischaemia vs. nifedipine at 4 weeks. Follow-up at one year revealed a lower rate of a composite of major adverse cardiac events (MACE; cardiac and non-cardiac death, nonfatal acute MI, hospital admission for unstable angina, or revascularisation) in the bisoprolol (22%) vs. nifedipine groups (22 vs. 33%, p = 0.03).
Other randomised trials
A randomised trial found that treatment with bisoprolol was associated with improved survival of myocardium (assessed using 99Tcm-sestamibi uptake) in patients with angina pectoris [85]. The efficacy of bisoprolol in managing anginal attacks has been shown to be comparable to that of atenolol [86,87,88,89,90] or verapamil [91] in randomised trials.
ECG ST segment elevation was significantly lower after randomisation to nebivolol vs. atenolol, in patients with documented CHD in patients undergoing exercise testing within a randomised trial [92]. A one-year randomised trial evaluated nebivolol in comparison with metoprolol and carvedilol in 172 patients with acute MI complicated by left ventricular dysfunction [93]. A composite outcome of nonfatal MI, cardiovascular death, hospitalisation for unstable angina pectoris or heart failure, stroke or revascularisation was significantly lower in the nebivolol vs. metoprolol groups (14.5 vs. 31.5%; p = 0.03), with no significant (p > 0.05) trends for benefit with for nebivolol vs. carvedilol (14.5 vs. 20.3%) and carvedilol vs. metoprolol (20.3 vs. 31.5%, p > 0.05).
Bisoprolol and nebivolol in hypertension
Head-to-head comparisons and meta-analyses
Similar magnitudes of blood pressure (BP) lowering were observed in patients (N = 273) randomised to bisoprolol (mean change –16/–7 mmHg) or nebivolol (mean change –16/–6 mmHg) for 12 weeks in a randomised, single-blind trial (the NEBIS study) [59]. Another small, randomised, crossover trial compared the effects of nebivolol and bisoprolol on endothelial function in 25 patients with hypertension [94]. Effects on endothelial function (forearm flow-mediated vasodilatation) were larger in the nebivolol group, consistent with its additional mechanism of enhanced synthesis of NO in the vasculature (see above). This did not translate into a statistically significant difference between groups for effects on BP, however: mean BP was reduced from 152/99 mmHg at baseline to 132/82 mmHg for nebivolol and to 130/83 mmHg for bisoprolol. Clinical outcomes after one year of treatment were evaluated in another head-to-head comparison of bisoprolol and nebivolol, conducted in 1056 patients with hypertension [95]. Randomisation to nebivolol vs. bisoprolol was associated with small and statistically non-significant differences between groups for overall mortality (9.8 vs. 11.5%), cardiovascular mortality (5.4 vs. 7.0%), hospitalisation for any cause (14.4 vs. 16.3%), and hospitalization cardiovascular for a cardiovascular cause (9.8 vs. 12.1%).
A meta-analysis showed that the proportion of patients achieving BP targets was similar for nebivolol and other β-blockers [49]. Statistically significantly higher percentages of patients achieving these targets were observed for nebivolol vs. ACE inhibitors and ARBs in this analysis [96].
Reductions in the resting heart rate are an important determinant of improved prognosis in patients at risk of adverse cardiovascular outcomes who receive cardioselective β-blockade [97]. As above, head-to-head data on the effects of these β-blockers on heart rate is lacking. However, there was a strong trend (p = 0.06) towards a larger decrease in heart rate 3 h after administration with bisoprolol (mean change –24 bpm) vs. nebivolol (mean change –15 bpm) in the randomised NEBIS study [58].
Limitations of these head-to-head comparisons in patients with hypertension included a relatively short duration (16 weeks or less [58, 93], or small patient populations (25 or less) [94]. The randomised outcomes trial that compared these agents was conducted in a single centre, with a short follow-up duration (one year), and differences in BMI at baseline between groups may have confounded outcomes to some extent [95]. Longer, better powered, head-to-head comparisons of bisoprolol and nebivolol are required in patients with hypertension.
Other randomised, active-controlled trials
An overview of the results of randomised, active-controlled evaluations of bisoprolol and nebivolol given as monotherapy to patients with hypertension is shown in Table 4 [20, 23, 98,99,100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123,124,125,126,127,128,129,130,131,132,133,134,135]. In general, the efficacy on BP of these drugs was similar to comparators, except for a greater effect on BP (especially 24-h BP) with bisoprolol vs. atenolol.
A meta-analysis showed that nebivolol reduces BP effectively across age groups, though with slightly less efficacy in older patients [20]. Nebivolol was also shown to be effective in African-American patients with hypertension, who have been identified as a population who respond less to beta-blockade than people of other ethnicities [136]. Clinical pharmacology studies showed that nebivolol improved the function of large [124, 137] or small [138] arteries more than atenolol, despite a similar overall effect on BP, consistent with the results of the clinical comparison with bisoprolol, described above [58]. Such an effect was not seen in a randomised comparison with metoprolol, however [139]. Another mechanistic study showed that nebivolol, but not metoprolol, reduced BP in hypertensive patients with autonomic failure, a condition that is known to respond to NO [140].
Nebivolol and bisoprolol are effective in combination with other antihypertensive agents for the management of hypertension, consistent with other drugs used for this purpose [141,142,143,144,145,146]. A full account of such studies is beyond the scope of this review.
Discussion
How do these second- and third-generation β-blockers compare?
The use of both bisoprolol and nebivolol for the management of HFrEF is supported by the results of randomised, placebo-controlled outcomes trials (the CIBIS programme for bisoprolol and the SENIORS trial for nebivolol). We have no head-to-head outcomes trials between these drugs in this (or any other) indication, although one such trial revealed little difference between them in terms of effects on clinically important and commonly measured parameters relevant to heart failure [72]. A network meta-analysis of the CIBIS programme and SENIORS did not reveal any sign of a clinically or statistically significant difference in heart failure outcomes between these agents (see Fig. 1) [76].
β-blockade is firmly established within the management of HFrEF, and both bisoprolol and nebivolol (along with carvedilol and metoprolol) are identified as evidence-based treatments in major European guidelines for HFrEF management [147], while bisoprolol is among medications “commonly used for HFrEF” in US guidelines [148]. Similarly, β-blockade is recommended as a first-line therapy option for chronic IHD and following an acute coronary syndrome in Europe [149,150,151], and in the USA [152]. No individual β-blocker is specified in these guidelines, so that the efficacy of β-blockade is essentially regarded as a class effect. Similarly, guidelines for the management of hypertension note that β-blockers in general have been shown to reduce the risk of MACE [153], consistent with the conclusion from a large meta-analysis that the magnitude of BP reduction per se may be the main driving force in reducing the risk of MACE [154]. The European guidelines point out that neither bisoprolol nor nebivolol is currently supported by a cardiovascular outcomes trials [151].
Finally, we have concentrated on evidence from randomised outcomes trials wherever possible in this article, and have not addressed real-world evidence, which is increasingly influential in the evaluation o the effects of therapies in routine care. One real world analysis conducted in more than 7500 patients with hypertension treated for up to 14 years, found that treatment with bisoprolol was associated with reduced mortality compared with pooled data for other β-blockers (HR 0.45 [95%CI 0.34 to 0.61) or pooled non-β-blocker therapies (HR 0.50 [95%CI: 0.38 to 0.66]) [155]. A fuller consideration of real-world evidence in this area would be an interesting subject for review elsewhere.
Knowledge gaps and outstanding research questions
The only reliable comparison of the effects of two drugs on a given disease is within a head-to-head randomised clinical trial. We have only one small trial comparing bisoprolol and nebivolol in HFrEF [72], and no such trials in patients with IHD or hypertension. The evidence base for improved clinical outcomes with bisoprolol and nebivolol is strongest in patients with HFrEF, and more information is required on the effects of these outcomes in patients with IHD and, especially, hypertension. In addition, the possible place of β-blockade in heart failure with preserved ejection fraction remains controversial: data to date from trials of β-blockers in these patients have been inconsistent [156], although a recent registry study suggested benefit from this approach [157]. Further studies in these patients are required.
Conclusions
A high level of β1-adrenoceptor selectivity is contributes importantly to the utility of β-blockers in the management of hypertension and cardiovascular disease. This will be especially so outside the tightly controlled environments of clinical trials, where patients may have (or develop over time) comorbidities such as dysglycaemia, obstructive pulmonary disease or erective dysfunction. Bisoprolol and nebivolol are both highly cardioselective β-blockers, rendering them suitable for use in many patients with such comorbidities, compared with non-selective (first-generation) β-blockers. Nebivolol, a third-generation β-blocker, has additional vasodilator actions, related to enhanced release of NO in the vascular wall, compared with bisoprolol, a second-generation agent. The additional NO-releasing effect of nebivolol may underlie reports of improvements in erectile function in patients receiving this agent. Available evidence, summarised in this review, does not provide evidence of either a superior effect on clinical outcomes in HFrEF, or a greater effect on BP in hypertension, for nebivolol vs. bisoprolol, although head-to-head trials are lacking.
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Andreka P, Aiyar N, Olson LC, et al. Bucindolol displays intrinsic sympathomimetic activity in human myocardium. Circulation. 2002;105:2429–34.
Poirier L, Tobe SW. Contemporary use of β-blockers: clinical relevance of subclassification. Can J Cardiol. 2014;30(5 Suppl):S9–15.
MacCarthy EP, Bloomfield SS. Labetalol: a review of its pharmacology, pharmacokinetics, clinical uses and adverse effects. Pharmacotherapy. 1983;3:193–219.
Nawarskas JJ, Cheng-Lai A, Frishman WH. Celiprolol: a unique selective adrenoceptor modulator. Cardiol Rev. 2017;25:247–53.
National Institute for Health and Care Excellence. Beta-adrenoceptor blocking drugs. Overview. Available at https://bnf.nice.org.uk/treatment-summary/beta-adrenoceptor-blocking-drugs.html (accessed April 2021).
Freemantle N, Cleland J, Young P, Mason J, Harrison J. Beta Blockade after myocardial infarction: systematic review and meta regression analysis. BMJ. 1999;318:1730–7.
Cruickshank JM. Are we misunderstanding beta-blockers. Int J Cardiol. 2007;120:10–27.
Marwood JF, Stokes GS. Studies on the vasodilator actions of bucindolol in the rat. Clin Exp Pharmacol Physiol. 1986;13:59–68.
Farzam K. Beta blockers. Stat Pearls (internet). Available at https://www.statpearls.com/kb/viewarticle/18241 (accessed April 2021).
Maffei A, Lembo G. Nitric oxide mechanisms of nebivolol. Ther Adv Cardiovasc Dis. 2009;3:317–27.
Ritter JM. Nebivolol: endothelium-mediated vasodilating effect. J Cardiovasc Pharmacol. 2001;38(Suppl 3):S13–6.
Fongemie J, Felix-Getzik E. A review of nebivolol pharmacology and clinical evidence. Drugs. 2015;75:1349–71.
Stoschitzky K. Individual beta-blockers for individual patients. e-journal of the ESC Council for Cardiology Practice. 2008;6:15 Jan 2008. Available at https://www.escardio.org/Journals/E-Journal-of-Cardiology-Practice/Volume-6/Individual-beta-blockers-for-individual-patients-Title-Individual-beta-blocke (accessed April 2021).
Koracevic G, Micic S, Stojanovic M, et al. Compelling indications should be listed for individual beta-blockers (due to diversity), not for the whole class [published online ahead of print, 2020 May 18]. Curr Vasc Pharmacol. 2021;19:343–46.
Sinagra G, Corrà U, Contini M, et al. Choosing among β-blockers in heart failure patients according to β-receptors’ location and functions in the cardiopulmonary system. Pharmacol Res. 2020;156:104785.
Marshall AJ, Roberts CJ, Barritt DW. Raynaud’s phenomenon as side effect of beta-blockers in hypertension. Br Med J. 1976;1:1498–9.
Fonseca VA. Effects of beta-blockers on glucose and lipid metabolism. Curr Med Res Opin. 2010;26:615–29.
Hirst JA, Farmer AJ, Feakins BG, Aronson JK, Stevens RJ. Quantifying the effects of diuretics and β-adrenoceptor blockers on glycaemic control in diabetes mellitus — a systematic review and meta-analysis. Br J Clin Pharmacol. 2015;79:733–43.
Van de Ven LL, Van Leeuwen JT, Smit AJ. The influence of chronic treatment with betablockade and angiotensin converting enzyme inhibition on the peripheral blood flow in hypertensive patients with and without concomitant intermittent claudication. A comparative cross-over trial. Vasa. 1994;23:357–62.
Germino FW, Lin Y, Pejović V, Bowen L. Efficacy and tolerability of nebivolol: does age matter? A retrospective analysis of three randomized, placebo-controlled trials in stage I-II hypertension. Ther Adv Cardiovasc Dis. 2012;6:185–99.
Barron AJ, Zaman N, Cole GD, Wensel R, Okonko DO, Francis DP. Systematic review of genuine versus spurious side-effects of beta-blockers in heart failure using placebo control: recommendations for patient information. Int J Cardiol. 2013;168:3572–9.
Shen L, Shah BR, Reyes EM, et al. Role of diuretics, β blockers, and statins in increasing the risk of diabetes in patients with impaired glucose tolerance: reanalysis of data from the NAVIGATOR study. BMJ. 2013;347:f6745.
Dhakam Z, Yasmin, McEniery CM, Burton T, Brown MJ, Wilkinson IB. A comparison of atenolol and nebivolol in isolated systolic hypertension. J Hypertens. 2008;26:351–6.
Wai B, Kearney LG, Hare DL, Ord M, Burrell LM, Srivastava PM. Beta blocker use in subjects with type 2 diabetes mellitus and systolic heart failure does not worsen glycaemic control. Cardiovasc Diabetol. 2012;11:14.
Janka HU, Ziegler AG, Disselhoff G, Mehnert H. Influence of bisoprolol on blood glucose, glucosuria, and haemoglobin A1 in noninsulin-dependent diabetics. J Cardiovasc Pharmacol. 1986;8(Suppl 11):S96–9.
Van Bortel LM. Efficacy, tolerability and safety of nebivolol in patients with hypertension and diabetes: a post-marketing surveillance study. Eur Rev Med Pharmacol Sci. 2010;14:749–58.
Ayers K, Byrne LM, DeMatteo A, Brown NJ. Differential effects of nebivolol and metoprolol on insulin sensitivity and plasminogen activator inhibitor in the metabolic syndrome. Hypertension. 2012;59:893–8.
Deedwania P, Shea J, Chen W, Brener L. Effects of add-on nebivolol on blood pressure and glucose parameters in hypertensive patients with prediabetes. J Clin Hypertens (Greenwich). 2013;15:270–8.
Marketou M, Gupta Y, Jain S, Vardas P. Differential metabolic effects of beta-blockers: an updated systematic review of nebivolol. Curr Hypertens Rep. 2017;19:22.
Lipworth B, Wedzicha J, Devereux G, Vestbo J, Dransfield MT. Beta-blockers in COPD: time for reappraisal. Eur Respir J. 2016;48:880–8.
Morales DR, Lipworth BJ, Donnan PT, Jackson C, Guthrie B. Respiratory effect of beta-blockers in people with asthma and cardiovascular disease: population-based nested case control study. BMC Med. 2017;15:18.
Bennett MR, Chang CL, Tuffery C, Hopping S, Hancox RJ. The impact of regular bisoprolol on the response to salbutamol in asthma: a double-blind randomized placebo-controlled crossover trial. Respirology. 2021;26:225–32.
Lim KP, Loughrey S, Musk M, Lavender M, Wrobel JP. Beta-blocker under-use in COPD patients. Int J Chron Obstruct Pulmon Dis. 2017;12:3041–6.
Espinola-Klein C, Weisser G, Jagodzinski A, et al. β-Blockers in patients with intermittent claudication and arterial hypertension: results from the nebivolol or metoprolol in arterial occlusive disease trial. Hypertension. 2011;58:148–54.
Mustafaev II, Nurmamedova GS. Effect of monotherapy with nebivolol, bisoprolol, carvedilol on the state of vegetative nervous system and sexual function in men with arterial hypertension. Kardiologiia. 2013;53:48–54.
Broekman CP, Haensel SM, Van de Ven LL, Slob AK. Bisoprolol and hypertension: effects on sexual functioning in men. J Sex Marital Ther. 1992;18:325–31.
Riva N, Lip GY. Nebivolol for the treatment of heart failure. Expert Opin Investig Drugs. 2011;20:1733–46.
Brixius K, Middeke M, Lichtenthal A, Jahn E, Schwinger RH. Nitric oxide, erectile dysfunction and beta-blocker treatment (MR NOED study): benefit of nebivolol versus metoprolol in hypertensive men. Clin Exp Pharmacol Physiol. 2007;34:327–31.
Gür Ö, Gurkan S, Yumun G, Turker P. The comparison of the effects of nebivolol and metoprolol on erectile dysfunction in the cases with coronary artery bypass surgery. Ann Thorac Cardiovasc Surg. 2017;23:91–5.
Boydak B, Nalbantgil S, Fici F, et al. A randomised comparison of the effects of nebivolol and atenolol with and without chlorthalidone on the sexual function of hypertensive men. Clin Drug Investig. 2005;25:409–16.
Cordero A, Bertomeu-Martínez V, Mazón P, et al. Erectile dysfunction in high-risk hypertensive patients treated with beta-blockade agents. Cardiovasc Ther. 2010;28:15–22.
Doumas M, Tsakiris A, Douma S, et al. Beneficial effects of switching from beta-blockers to nebivolol on the erectile function of hypertensive patients. Asian J Androl. 2006;8:177–82.
Sharp RP, Gales BJ. Nebivolol versus other beta blockers in patients with hypertension and erectile dysfunction. Ther Adv Urol. 2017;9:59–63.
Aydın K, Gökçen K, Yıldırım Ş, Bagcivan İ, Parlak M, Gökçe G. In vitro evaluation of nebivolol effects on nonadrenergic noncholinergic responses in rabbit corpus cavernosum. Andrologia. 2018;50:e13062.
Martínez-Salamanca JI, La Fuente JM, et al. Nebivolol potentiates the efficacy of PDE5 inhibitors to relax corpus cavernosum and penile arteries from diabetic patients by enhancing the NO/cGMP pathway. J Sex Med. 2014;11:1182–92.
Brixius K, Bundkirchen A, Bölck B, Mehlhorn U, Schwinger RH. Nebivolol, bucindolol, metoprolol and carvedilol are devoid of intrinsic sympathomimetic activity in human myocardium. Br J Pharmacol. 2001;133:1330–8.
Bundkirchen A, Brixius K, Bölck B, Nguyen Q, Schwinger RH. Beta 1-adrenoceptor selectivity of nebivolol and bisoprolol. A comparison of [3H]CGP 12.177 and [125I]iodocyanopindolol binding studies. Eur J Pharmacol. 2003;460:19–26.
Nuttall SL, Routledge HC, Kendall MJ. A comparison of the beta1-selectivity of three beta1-selective beta-blockers. J Clin Pharm Ther. 2003;28:179–86.
Maack C, Tyroller S, Schnabel P, et al. Characterization of beta(1)-selectivity, adrenoceptor-G(s)-protein interaction and inverse agonism of nebivolol in human myocardium. Br J Pharmacol. 2001;132:1817–26.
Baker JG. The selectivity of beta-adrenoceptor antagonists at the human beta1, beta2 and beta3 adrenoceptors. Br J Pharmacol. 2005;144:317–22.
Schnabel P, Maack C, Mies F, Tyroller S, Scheer A, Böhm M. Binding properties of beta-blockers at recombinant beta1-, beta2-, and beta3-adrenoceptors. J Cardiovasc Pharmacol. 2000;36:466–71.
Lymperopoulos A, Rengo G, Koch WJ. Adrenergic nervous system in heart failure: pathophysiology and therapy. Circ Res. 2013;113:739–53.
Feldman DS, Carnes CA, Abraham WT, Bristow MR. Mechanisms of disease: beta-adrenergic receptors–alterations in signal transduction and pharmacogenomics in heart failure. Nat Clin Pract Cardiovasc Med. 2005;2:475–83.
Grassi G. Sympathomodulatory effects of antihypertensive drug treatment. Am J Hypertens. 2016;29:665–75.
Cruickshank J. Nebivolol, a third generation beta-blocker. J Signs Symptoms. 2014;3:380–91.
Oliver E, Mayor F Jr, D’Ocon P. Beta-blockers: historical perspective and mechanisms of action. Rev Esp Cardiol (Engl Ed). 2019;72:853–62.
Cruickshank J. Nebivolol, a third generation beta-blocker. J Symptoms Signs. 2014;3:380–91.
Czuriga I, Riecansky I, Bodnar J, et al. Comparison of the new cardioselective beta-blocker nebivolol with bisoprolol in hypertension: the Nebivolol, Bisoprolol Multicenter Study (NEBIS). Cardiovasc Drugs Ther. 2003;17:257–63.
Khilnani G, Khilnani AK. Inverse agonism and its therapeutic significance. Indian J Pharmacol. 2011;43:492–501.
Cheymol G, Woestenborghs R, Snoeck E, et al. Pharmacokinetic study and cardiovascular monitoring of nebivolol in normal and obese subjects. Eur J Clin Pharmacol. 1997;51:493–8.
Leopold G, Pabst J, Ungethüm W, Bühring KU. Basic pharmacokinetics of bisoprolol, a new highly beta 1-selective adrenoceptor antagonist. J Clin Pharmacol. 1986;26:616–21.
Hilas O, Ezzo D. Nebivolol (bystolic), a novel Beta blocker for hypertension. P T. 2009;34:188–92.
Briciu C, Neag M, Muntean D, et al. Phenotypic differences in nebivolol metabolism and bioavailability in healthy volunteers. Clujul Med. 2015;88:208–13.
Momčilović S, Jovanović A, Radojković D, et al. Population pharmacokinetic analysis of bisoprolol in type 2 diabetic patients with hypertension. Eur J Clin Pharmacol. 2020;76:1539–46.
Momčilović S, Milovanović JR, Janković SM, et al. Population pharmacokinetic analysis of bisoprolol in patients with acute coronary syndrome. J Cardiovasc Pharmacol. 2019;73:136–42.
Ågesen FN, Weeke PE, Tfelt-Hansen P, Tfelt-Hansen J. Pharmacokinetic variability of beta-adrenergic blocking agents used in cardiology. Pharmacol Res Perspect. 2019;7:e00496.
Singh S, Warren HR, Hiltunen TP, et al. Genome-wide meta-analysis of blood pressure response to β1-blockers: results from ICAPS (International Consortium of Antihypertensive Pharmacogenomics Studies). J Am Heart Assoc. 2019;8:e013115.
Gong Y, McDonough CW, Beitelshees AL, et al. PTPRD gene associated with blood pressure response to atenolol and resistant hypertension. J Hypertens. 2015;33:2278–85.
Ingram A, Valente M. Genetic variation of hepatic enzymes influence on β-blocker dose in patients with reduced ejection fraction heart failure. J Pharm Pract. 2020;33:96–8.
Hiltunen TP, Donner KM, Sarin AP, et al. Pharmacogenomics of hypertension: a genome-wide, placebo-controlled cross-over study, using four classes of antihypertensive drugs. J Am Heart Assoc. 2015;4:e001521.
Rau T, Düngen HD, Edelmann F, et al. Impact of the β1-adrenoceptor Arg389Gly polymorphism on heart-rate responses to bisoprolol and carvedilol in heart-failure patients. Clin Pharmacol Ther. 2012;92:21–8.
Contini Apostolo A, Cattadori G, et al. Multiparametric comparison of CARvedilol, vs. NEbivolol, vs. BIsoprolol in moderate heart failure: the CARNEBI trial. Int J Cardiol. 2013;168:2134–40.
De Cree J, Van Nueten L, Geukens H, Verhaegen H. Comparative cardiac haemodynamics of bisoprolol, celiprolol, carvedilol and nebivolol in normal volunteers. Int J Clin Pharmacol Res. 1992;12:159–63.
Chatterjee S, Biondi-Zoccai G, Abbate A, et al. Benefits of β blockers in patients with heart failure and reduced ejection fraction: network meta-analysis. BMJ. 2013;346:f55.
CIBIS Investigators and Committees. A randomized trial of beta-blockade in heart failure. The Cardiac Insufficiency Bisoprolol Study (CIBIS). Circulation. 1994;90:1765–73.
CIBIS Investigators. The Cardiac Insufficiency Bisoprolol Study II (CIBIS-II): a randomised trial. Lancet. 1999;353:9–13.
Willenheimer R, van Veldhuisen D, Silke B, et al. Effect on survival and hospitalization of initiating treatment for chronic heart failure with bisoprolol followed by enalapril, as compared with the opposite sequence: results of the randomized Cardiac Insufficiency Bisoprolol Study (CIBIS) III. Circulation. 2005;112:2426–35.
Flather MD, Shibata MC, Coats AJ, Van Veldhuisen DJ, Parkhomenko A, Borbola J, et al, for the SENIORS Investigators. Randomized trial to determine the effect of nebivolol on mortality and cardiovascular hospital admission in elderly patients with heart failure (SENIORS). Eur Heart J. 2005;26:215–25
Erdmann E, Lechat P, Verkenne P, Wiemann H. Results from post-hoc analyses of the CIBIS II trial: effect of bisoprolol in high-risk patient groups with chronic heart failure. Eur J Heart Fail. 2001;3:469–79.
Funck-Brentano C, van Veldhuisen DJ, van de Ven LL, et al. Influence of order and type of drug (bisoprolol vs. enalapril) on outcome and adverse events in patients with chronic heart failure: a post hoc analysis of the CIBIS-III trial. Eur J Heart Fail. 2011;13:765–72.
Cohen-Solal A, Kotecha D, van Veldhuisen DJ, et al. Efficacy and safety of nebivolol in elderly heart failure patients with impaired renal function: insights from the SENIORS trial. Eur J Heart Fail. 2009;11:872–80.
Montero-Perez-Barquero M, Flather M, Roughton M, et al. Influence of systolic blood pressure on clinical outcomes in elderly heart failure patients treated with nebivolol: data from the SENIORS trial. Eur J Heart Fail. 2014;16:1009–15.
Von Arnim T. Prognostic significance of transient ischemic episodes: response to treatment shows improved prognosis. Results of the Total Ischemic Burden Bisoprolol Study (TIBBs) follow-up. J Am Coll Cardiol. 1996;28:20–4.
von Arnim T. Medical treatment to reduce total ischemic burden: total ischemic burden bisoprolol study (TIBBS), a multicenter trial comparing bisoprolol and nifedipine. The TIBBS Investigators. J Am Coll Cardiol. 1995;25:231–8.
Lin ZP, Dong M, Liu J. Bisoprolol improved endothelial function and myocardium survival of hypertension with stable angina: a randomized double-blinded trial. Eur Rev Med Pharmacol Sci. 2013;17:794–801.
de Muinck ED, Buchner-Moell D, van de Ven LL, Lie KI. Comparison of the safety and efficacy of bisoprolol versus atenolol in stable exercise-induced angina pectoris: a Multicenter International Randomized Study of Angina Pectoris (MIRSA). J Cardiovasc Pharmacol. 1992;19:870–5.
Dorow P, Thalhofer S, Bethge H, Disselhoff G, Wagner G. Long-term treatment of angina pectoris with bisoprolol or atenolol in patients with chronic obstructive bronchitis: a randomized, double-blind crossover study. J Cardiovasc Pharmacol. 1990;16(Suppl 5):S36-44.
Maltz MB, Dymond DS, Nathan AW, Camm AJ. A comparison of once daily bisoprolol, 5 and 10 mg, and atenolol 100 mg in the treatment of angina pectoris. Eur Heart J. 1987;8 Suppl M:37–42.
Kohli RS, Lahiri A, Raftery EB. Management of chronic stable angina with once-daily bisoprolol or atenolol and long-term efficacy of bisoprolol. J Cardiovasc Pharmacol. 1986;8(Suppl 11):S148–53.
Kohli RS, Khurmi NS, Kardash MM, Hughes LO, Lahiri A, Raftery EB. Efficacy of once daily bisoprolol in stable angina pectoris: an objective comparison with atenolol and long term follow-up. Eur Heart J. 1985;6:845–50.
De Divitiis O, Liguori V, Di Somma S, et al. Bisoprolol in the treatment of angina pectoris: a double blind comparison with verapamil. Eur Heart J. 1987;8 Suppl M:43–54.
Ruf G, Trenk D, Jähnchen E, Roskamm H. Determination of the anti-ischemic activity of nebivolol in comparison with atenolol. Int J Cardiol. 1994;43:279–85.
Ozaydin M, Yucel H, Kocyigit S, et al. Nebivolol versus carvedilol or metoprolol in patients presenting with acute myocardial infarction complicated by left ventricular dysfunction. Med Princ Pract. 2016;25:316–22.
Simova II, Todorova-Konstantinova RR, Denchev SV. Effects of nebivolol versus bisoprolol on endothelial function in hypertensive patients. Exp Clin Cardiol. 2009;14:45–9.
Kumar R, Mal K, Begum J, Shaukat F. Comparison of nebivolol and bisoprolol for cardiovascular mortality in hypertensive patients. Cureus. 2019;11:e6453.
Van Bortel LM, Fici F, Mascagni F. Efficacy and tolerability of nebivolol compared with other antihypertensive drugs: a meta-analysis. Am J Cardiovasc Drugs. 2008;8:35–44.
Chen YD, Yang XC, Pham VN, et al. Resting heart rate control and prognosis in coronary artery disease patients with hypertension previously treated with bisoprolol: a sub-group analysis of the BISO-CAD study. Chin Med J (Engl). 2020;133:1155–65.
Bouvier JM, Rabot D, Herrero G. Effect of bisoprolol and acebutolol on resting blood pressure and on exercise blood pressure profile in hypertensive patients: a comparative, single-blind study. J Cardiovasc Pharmacol. 1990;16(Suppl 5):S179–83.
Zhou WJ, Wang RY, Li Y, et al. A randomized controlled study on the effects of bisoprolol and atenolol on sympathetic nervous activity and central aortic pressure in patients with essential hypertension. PLoS One. 2013;8:e72102.
Wheeldon NM, MacDonald TM, Prasad N, Maclean D, Peebles L, McDevitt DG. A double-blind comparison of bisoprolol and atenolol in patients with essential hypertension. QJM. 1995;88:565–70.
Leeman M, van de Borne P, Collart F, et al. Bisoprolol and atenolol in essential hypertension: effects on systemic and renal hemodynamics and on ambulatory blood pressure. J Cardiovasc Pharmacol. 1993;22:785–91.
Neutel JM, Smith DH, Ram CV, Lefkowitz MP, Kazempour MK, Weber MA. Comparison of bisoprolol with atenolol for systemic hypertension in four population groups (young, old, black and nonblack) using ambulatory blood pressure monitoring. Bisoprolol Investigators Group. Am J Cardiol. 1993;72:41–6.
Lithell H, Selinus I, Hosie J, Frithz G, Weiner L. Efficacy and safety of bisoprolol and atenolol in patients with mild to moderate hypertension: a double-blind, parallel group international multicentre study. Eur Heart J. 1987;8 Suppl M:55–64.
Neutel JM, Smith DH, Ram CV, et al. Application of ambulatory blood pressure monitoring in differentiating between antihypertensive agents. Am J Med. 1993;94:181–7.
Lewis R, Maclean D, Ioannides C, Johnston A, McDevitt DG. A comparison of bisoprolol and atenolol in the treatment of mild to moderate hypertension. Br J Clin Pharmacol. 1988;26:53–9.
Bühler FR, Berglund G, Anderson OK, et al. Double-blind comparison of the cardioselective beta-blockers bisoprolol and atenolol in hypertension: the Bisoprolol International Multicenter Study (BIMS). J Cardiovasc Pharmacol. 1986;8(Suppl 11):S122–7.
Dixon MS, Thomas P, Sheridan DJ. A randomized double-blind study of bisoprolol versus atenolol in mild to moderate essential hypertension. Eur J Clin Pharmacol. 1990;38:21–4.
Eguchi K, Hoshide S, Kario K. Effects of celiprolol and bisoprolol on blood pressure, vascular stiffness, and baroreflex sensitivity. Am J Hypertens. 2015;2:858–67.
Yang T, Jiang Y, Hao Y, et al. Comparison of bisoprolol to a metoprolol CR/ZOK tablet for control of heart rate and blood pressure in mild-to-moderate hypertensive patients: the CREATIVE study. Hypertens Res. 2017;40:79–86.
Haasis R, Bethge H. Exercise blood pressure and heart rate reduction 24 and 3 hours after drug intake in hypertensive patients following 4 weeks of treatment with bisoprolol and metoprolol: a randomized multicentre double-blind study (BISOMET). Eur Heart J. 1987;8 Suppl M:103–13.
Bracchetti D, Gradnik R, Alberti A, et al. A double-blind comparison of bisoprolol and captopril for treatment of essential hypertension in the elderly. Cardiovasc Drugs Ther. 1990;4:261–4.
Vaïsse B, Herpin D, Asmar R, et al. Assessment of antihypertensive effect by blood pressure monitoring: applications to bisoprolol and lisinopril in a double-blind study. J Cardiovasc Pharmacol. 1997;29:612–7.
Saku K, Liu K, Takeda Y, Jimi S, Arakawa K. Effects of lisinopril and bisoprolol on lipoprotein metabolism in patients with mild-to-moderate essential hypertension. Clin Ther. 1995;17:1136–46.
Gosse P, Roudaut R, Herrero G, Dallocchio M. Beta-blockers vs. angiotensin-converting enzyme inhibitors in hypertension: effects on left ventricular hypertrophy. J Cardiovasc Pharmacol. 1990;16 (Suppl 5):S145–50.
Liu G, Li M, Shi X, et al. Efficacy of domestic bisoprolol, enalapril and nifedipine retard in mild to moderate hypertension: a randomized double-blind multicenter clinical trial in China. Zhonghua Nei Ke Za Zhi. 2002;41:450–2.
Radchenko GD, Sirenko YM, Kushnir SM, Torbas OO, Dobrokhod AS. Comparative effectiveness of a fixed-dose combination of losartan + HCTZ versus bisoprolol + HCTZ in patients with moderate-to-severe hypertension: results of the 6-month ELIZA trial. Vasc Health Risk Manag. 2013;9:535–49.
Parrinello G, Paterna S, Torres D, et al. One-year renal and cardiac effects of bisoprolol versus losartan in recently diagnosed hypertensive patients: a randomized, double-blind study. Clin Drug Investig. 2009;29:591–600.
Oliván Martinez J, Garcia MJ, Rodriguez Botaro A, Pizarro JL, Carretero J, Garrido M. Bisoprolol and nifedipine SR in the treatment of hypertension in the elderly. J Cardiovasc Pharmacol. 1990;16(Suppl 5):S95–9.
Amabile G, Serradimigni A. Comparison of bisoprolol with nifedipine for treatment of essential hypertension in the elderly: comparative double-blind trial. Eur Heart J. 1987;8 Suppl M:65–9.
Bueno J, Amiguet JA, Carasusan J, Cebollada J, Carretero J. Bisoprolol vs. chlorthalidone: a randomized, double-blind, comparative study in arterial hypertension. J Cardiovasc Pharmacol. 1990;16 Suppl 5:S189–92.
Williams B, MacDonald TM, Morant S, et al. Spironolactone versus placebo, bisoprolol, and doxazosin to determine the optimal treatment for drug-resistant hypertension (PATHWAY-2): a randomised, double-blind, crossover trial. Lancet. 2015;386:2059–68.
Van Nueten L, Taylor FR, Robertson JI. Nebivolol vs atenolol and placebo in essential hypertension: a double-blind randomised trial. J Hum Hypertens. 1998;12:135–40.
Simon G, Johnson ML. Comparison of antihypertensive and beta 1-adrenoceptor antagonist effect of nebivolol and atenolol in essential hypertension. Clin Exp Hypertens. 1993;15:501–9.
Badar VA, Hiware SK, Shrivastava MP, Thawani VR, Hardas MM. Comparison of nebivolol and atenolol on blood pressure, blood sugar, and lipid profile in patients of essential hypertension. Indian J Pharmacol. 2011;43:437–40.
Fogari R, Zoppi A, Lazzari P, et al. Comparative effects of nebivolol and atenolol on blood pressure and insulin sensitivity in hypertensive subjects with type II diabetes. J Hum Hypertens. 1997;11:753–7.
Arosio E, De Marchi S, Prior M, Zannoni M, Lechi A. Effects of nebivolol and atenolol on small arteries and microcirculatory endothelium-dependent dilation in hypertensive patients undergoing isometric stress. J Hypertens. 2002;20:1793–7.
Erdoğan O, Ertem B, Altun A, et al. Comparison of antihypertensive efficacy of carvedilol and nebivolol in mild-to-moderate primary hypertension: a randomized trial. Anadolu Kardiyol Derg. 2011;11:310–3.
Grassi G, Seravalle G, Brambilla G, et al. Multicenter randomized double-blind comparison of nebivolol plus HCTZ and Irbesartan plus HCTZ in the treatment of isolated systolic hypertension in elderly patients: results of the NEHIS study. Adv Ther. 2017;33:2173–87.
Heitmann J, Greulich T, Reinke C, et al. Comparison of the effects of nebivolol and valsartan on BP reduction and sleep apnoea activity in patients with essential hypertension and OSA. Curr Med Res Opin. 2010;26:1925–32.
Rosei EA, Rizzoni D, Comini S, et al. Evaluation of the efficacy and tolerability of nebivolol versus lisinopril in the treatment of essential arterial hypertension: a randomized, multicentre, double-blind study. Blood Press Suppl. 2003;1:30–5.
Van Nueten L, Rishøj Nielsen M, Vertommen C, et al. Nebivolol versus enalapril in essential hypertension: a long-term double-blind comparative trial. Acta Clin Belg. 1999;54:19–25.
Van Nueten L, Schelling A, Vertommen C, Dupont AG, Robertson JI. Nebivolol vs enalapril in the treatment of essential hypertension: a double-blind randomised trial. J Hum Hypertens. 1997;11:813–9.
Mazza A, Gil-Extremera B, Maldonato A, Toutouzas T, Pessina AC. Nebivolol vs amlodipine as first-line treatment of essential arterial hypertension in the elderly. Blood Press. 2002;11:182–8.
Lacourcière Y, Poirier L, Lefebvre J, Provencher P, Arnott W. Comparative effects of a new cardioselective beta-blocker nebivolol and nifedipine sustained-release on 24-hour ambulatory blood pressure and plasma lipoproteins. J Clin Pharmacol. 1992;32:660–6.
Van Nueten L, Lacourcière Y, Vyssoulis G, et al. Nebivolol versus nifedipine in the treatment of essential hypertension: a double-blind, randomized, comparative trial. Am J Ther. 1998;5:237–43.
Saunders E, Smith WB, DeSalvo KB, Sullivan WA. The efficacy and tolerability of nebivolol in hypertensive African American patients. J Clin Hypertens (Greenwich). 2007;9:866–75.
Tzemos N, Lim PO, MacDonald TM. Nebivolol reverses endothelial dysfunction in essential hypertension: a randomized, double-blind, crossover study. Circulation. 2001;104:511–4.
Duprez DA, Florea N, Duval S, Koukol C, Cohn JN. Effect of nebivolol or atenolol vs. placebo on cardiovascular health in subjects with borderline blood pressure: the EVIDENCE study. J Hum Hypertens. 2017;32:20–5.
Hayek SS, Poole JC, Neuman R, et al. Differential effects of nebivolol and metoprolol on arterial stiffness, circulating progenitor cells, and oxidative stress. J Am Soc Hypertens. 2015;9:206–13.
Okamoto LE, Gamboa A, Shibao CA, et al. Nebivolol, but not metoprolol, lowers blood pressure in nitric oxide-sensitive human hypertension. Hypertension. 2014;64:1241–7.
Lacourcière Y, Arnott W. Placebo-controlled comparison of the effects of nebivolol and low-dose hydrochlorothiazide as monotherapies and in combination on blood pressure and lipid profile in hypertensive patients. J Hum Hypertens. 1994;8:283–8.
Lacourcière Y, Lefebvre J, Poirier L, Archambault F, Arnott W. Treatment of ambulatory hypertensives with nebivolol or hydrochlorothiazide alone and in combination. A randomized, double-blind, placebo-controlled, factorial-design trial. Am J Hypertens. 1994;7:137–45.
Papademetriou V. Comparison of Nebivolol monotherapy versus Nebivolol in combination with other antihypertensive therapies for the treatment of hypertension. Am J Cardiol. 2009;103:273–8.
Neutel JM, Smith DH, Gradman AH. Adding nebivolol to ongoing antihypertensive therapy improves blood pressure and response rates in patients with uncontrolled stage I-II hypertension. J Hum Hypertens. 2010;24:64–73.
Frishman WH, Bryzinski BS, Coulson LR, et al. A multifactorial trial design to assess combination therapy in hypertension. Treatment with bisoprolol and hydrochlorothiazide. Arch Intern Med. 1994;154:1461–8.
Frishman WH, Burris JF, Mroczek WJ, et al. First-line therapy option with low-dose bisoprolol fumarate and low-dose hydrochlorothiazide in patients with stage I and stage II systemic hypertension. J Clin Pharmacol. 1995;35:182–8.
Ponikowski P, Voors AA, Anker SD, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37:2129–200.
Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. Circulation. 2017;136:e137–61.
Knuuti J, Wijns W, Saraste A, Capodanno D, et al. 2019 ESC Guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J. 2020;41:407–77.
Roffi M, Patrono C, Collet JP, et al. 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: task force for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J. 2016;14(37):267–315.
Ibanez B, James S, Agewall S, et al. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J. 2018;39:119–77.
O’Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;127:e362-425.
Williams B, Mancia G, Spiering W, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39:3021–104.
Law MR, Morris JK, Wald NJ. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ. 2009;338:b1665.
Sabidó M, Thilo H, Guido G. Long-term effectiveness of bisoprolol in patients with angina: a real-world evidence study. Pharmacol Res. 2019;139:106–12.
Cho JY. Beta-blockers in heart failure with preserved ejection fraction: could their use be vindicated as an acceptable option in the future treatment guideline? Korean Circ J. 2019;49:249–51.
Kim SH, Yun SC, Park JJ, et al. Beta-blockers in patients with heart failure with preserved ejection fraction: results from the Korea Acute Heart Failure (KorAHF) registry. Korean Circ J. 2019;49:238–48.
Acknowledgements
A medical writer (funded by Merck) provided editorial assistance in the development of the manuscript. The authors retained full control over the content of the manuscript.
Author information
Authors and Affiliations
Contributions
AA took the lead role in guiding the scope and overall content of the paper. All authors contributed material for the review, contributed to the development of the review and approved its submission.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
All authors reviewed the manuscript and approved its submission.
Conflict of Interest
WAlH reports receiving honorarium from Merck Serono Middle East FZ LTD, Novo Nordisk, Sanofi Aventis, Boehringer-ingelheim, Servier, outside the submitted work. AAIA and SM are employees of Merck Serono Middle East FZ-LLC, an affiliate of Merck KGaA, Germany.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
AlHabeeb, W., Mrabeti, S. & Abdelsalam, A.A.I. Therapeutic Properties of Highly Selective β-blockers With or Without Additional Vasodilator Properties: Focus on Bisoprolol and Nebivolol in Patients With Cardiovascular Disease. Cardiovasc Drugs Ther 36, 959–971 (2022). https://doi.org/10.1007/s10557-021-07205-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-021-07205-y