Abstract
Purpose
Limited research has been conducted to describe the geographical clustering and distribution of prostate cancer (PrCA) incidence in Georgia (GA). This study describes and compares the temporal and geographic trends of PrCA incidence in GA with a specific focus on racial disparities.
Methods
GA Comprehensive Cancer Registry PrCA incidence data were obtained for 1998–2008. Directly standardized age-adjusted PrCA incidence rates per 100,000 were analyzed by race, stage, grade, and county. County-level hotspots of PrCA incidence were analyzed with the Getis-Ord Gi* statistic in a geographic information system; a census tract-level cluster analysis was performed with a Discrete Poisson model and implemented in SaTScan® software.
Results
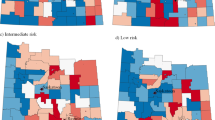
Significant (p < 0.05) hotspots of PrCA incidence were observed in nine southwestern counties and six centrally located counties among men of both races. Six significant (p < 0.1) clusters of PrCA incidence rates were detected for men of both races in north and northwest central Georgia. When stratified by race, clusters among white and black men were similar, although centroids were slightly shifted. Most notably, a large (122 km radius) cluster in northwest central Georgia was detected only in whites, and two smaller clusters (0–32 km radii) were detected in Southwest Georgia only in black men. Clusters of high-grade and late-stage tumors were identified primarily in the northern portion of the state among men of both races.
Conclusions
This study revealed a pattern of higher incidence and more advanced disease in northern and northwest central Georgia, highlighting geographic patterns that need more research and investigation of possible environmental determinants.







Similar content being viewed by others
References
National Cancer Institute: Cancer Topics: Prostate Cancer. http://cancer.gov/cancertopics/types/prostate. Accessed 15 March 2012
Surveillance Epidemiology and End Results (SEER) Stat fact sheets: prostate. http://seer.cancer.gov/statfacts/html/prost.html. Accessed 15 March 2012
McNamara C, Davis V, Bayakly AR, Moon T (2010) Prostate cancer in Georgia, 2002–2006. Georgia Department of Community Health, Division of Public Health, Chronic Disease, Healthy Behaviors, and Injury Epidemiology
Drake BF, Keane TE, Mosley CM, Adams SA, Elder KT, Modayil MV (2006) Prostate cancer disparities in South Carolina: early detection, special programs, and descriptive epidemiology. J S C Med Assoc 102:241–249
U.S. Census Bureau: State and County QuickFacts: Georgia. http://quickfacts.census.gov/qfd/states/13000.html. Accessed 15 March 2012
Wagner SE, Hurley DM, Hebert J, McNamara C, Bayakly AR, Vena JE (2012) Cancer mortality-to-incidence ratios in Georgia: describing racial cancer disparities and potential geographic determinants. Cancer 118(16):4032–4045
Steenland K, Goodman M, Liff J, Diiorio C, Butler S, Roberts P, et al (2011) The effect of race and rural residence on prostate cancer treatment choice among men in Georgia. Urology 77(3):581–587
DiIorio C, Steenland K, Goodman M, Butler S, Liff J, Roberts P (2011) Differences in treatment- based beliefs and coping between African American and white men with prostate cancer. J Commun Health 36(4): 505–512
Butler S, Owen-Smith A, DiIorio C, Goodman M, Liff J, Steenland K (2011) Use of complementary and alternative medicine among men with prostate cancer in a rural setting. J Commun Health 36(6):1004–1010
Steenland K, Goodman M, Liff J, Diiorio C, Butler S, Roberts P (2011) Quality of life among men with prostate cancer in rural Georgia. Urology 77(4):927–933
Lefevre ML (1998) Prostate cancer screening: more harm than good? Am Fam Physician 58(2):432–438
Kulldorff M (1997) A spatial scan statistic. Commun Stat Theory Methods 26:1481–1496
Ward E, Jemal A, Cokkinides V, Singh GK, Cardinez C, Ghafoor A et al (2004) Cancer disparities by race/ethnicity and socioeconomic status. CA Cancer J Clin 54(2):78–93
Catalona WJ, Smith DS, Ornstein DK (1997) Prostate cancer detection in men with serum PSA concentrations of 2.6 to 4.0 ng/mL and benign prostate examination. Enhancement of specificity with free PSA measurements. JAMA 277:1452–1455
Dagnelie PC, Schuurman AG, Goldbohm RA, Van den Brandt PA (2004) Diet, anthropometric measures and prostate cancer risk: a review of prospective cohort and intervention studies. BJU Int 93(8):1139–1150
Lambert JD, Yang CS (2003) Mechanisms of cancer prevention by tea constituents. J Nutr 133(10):3262S–3267S
Nelson WG, DeWeese TL, DeMarzo AM (2002) The diet, prostate inflammation, and the development of prostate cancer. Cancer Metastasis Rev 21:13–16
Sinha R, Anderson DE, McDonald SS, Greenwald P (2003) Cancer risk and diet in India. J Postgrad Med 49(3):222–228
Sommer F, Klotz T, Schmitz-Drager BJ (2004) Lifestyle issues and genitourinary tumours. World J Urol 21(6):402–413
Torti DC, Matheson GO (2004) Exercise and prostate cancer. Sports Med 34(6):363–369
Platz EA, Giovannucci E (2004) The epidemiology of sex steroid hormones and their signaling and metabolic pathways in the etiology of prostate cancer. J Steroid Biochem Mol Biol 92(4):237–253
Soronen P, Laiti M, Torn S, Harkonen P, Patrikainen L, Li Y et al (2004) Sex steroid hormone metabolism and prostate cancer. J Steroid Biochem Mol Biol 92(4):281–286
Turesky RJ (2004) The role of genetic polymorphisms in metabolism of carcinogenic heterocyclic aromatic amines. Curr Drug Metab 5(2):169–180
USDA State Fact Sheets: Georgia. http://www.ers.usda.gov/statefacts/ga.htm. Accessed 14 March 2012
State of Georgia Rural Health Plan. http://dch.georgia.gov/vgn/images/portal/cit_1210/21/19/970432432007_Rural_Health_Plan.pdf. Accessed 14 March 2012
42 Code of Federal Regulations (CFR), Chapter 1, Part 5, Appendix A (October 1, 1993, pp. 34–48) Criteria for designation of areas having shortages of primary medical care professionals [45 FR 76000, Nov. 17, 1980, as amended at 54 FR 8737, Mar. 2, 1989; 57 FR 2480, Jan. 22, 1992]
Doescher MP, Fordyce MA, Skillman SM, Jackson JE, Rosenblatt RA (2009) Persistent primary care health professional shortage areas (HPSAs) and health care access in rural America. In: Rural health research center policy brief. http://depts.washington.edu/uwrhrc/uploads/Persistent_HPSAs_PB.pdf. Accessed 15 March 2012
Hartley D (2004) Rural health disparities, population health, and rural culture. Am J Public Health 94(10):1675–1678
Bynum J, Song Y, Fisher E (2010) Variation in prostate-specific antigen screening in men aged 80 and older in fee-for-service Medicare. J Am Geriatr Soc 58(4):674–680
Smith RA, Cokkinides V, Brawley OW (2008) Cancer screening in the United States, 2008: a review of current American Cancer Society guidelines and cancer screening issues. CA Cancer J Clin 58:161–179
US Preventive Services Task Force (2011) Screening for prostate cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med 149:185–191
Barry MJ (2009) Screening for prostate cancer—the controversy that refuses to die. N Engl J Med 360:13
Zhu X, Albertsen PC, Andriole GL, Roobol MJ, Schroder FH, Vickers AJ (2012) Risk- based prostate cancer screening. Eur Urol 61(4):652–661
Greenberg RS, Stevens JA, Whitaker JP (1985) Cancer incidence aong blacks in urban and rural Georgia, 1978–1982. Am J Public Health 75:683–684
Mordukhovich I, Reiter PL, Backes DM, Family L, McCullough LE, O’Brien KM, et al (2011) A review of African American-white differences in risk factors for cancer: prostate cancer. Cancer Causes Control 22(3):341–357
Byers T, Nestle M, McTiernan A, Doyle C, Currie-Williams A, Gansler T et al (2002) American Cancer Society guidelines on nutrition and physical activity for cancer prevention: reducing the risk of cancer with healthy food choices and physical activity. CA Cancer J Clin 52(2):92–119
Beebe-Dimer JL, Dunn RL, Sarma AV, Montie JE, Cooney KA (2007) Features of the metabolic syndrome and prostate cancer in African-American men. Cancer 109:875–881
Hayes RB, Liff JM, Pottern LM, Greenberg RS, Schoenberg JB, Schwartz AG et al (1995) Prostate cancer risk in U.S. blacks and whites with a family history of cancer. Int J Cancer 60(3):361–364
Chang BL, Spangler E, Gallagher S, Haiman CA, Henderson B, Isaacs W, et al (2011) Validation of genome-wide prostate cancer associations in men of African descent. Cancer Epidemiol Biomarkers Prev 20(1):23–32
Allen JD, Kennedy M, Wilson-Glover A, Gilligan TD (2007) African-American men’s perceptions about prostate cancer: implications for designing educational interventions. Soc Sci Med 64(11):2189–2200
Glicksman AS, Meyer A, DiPiero M (2012) Tailored community cancer education programs: pawsox and prostates. J Cancer Educ 25(2):180–183
http://www.palmettohealth.org/body.cfm?id=489. Accessed 17 May 2012
http://www.tellusdetroit.com/health/100-black-men-up.html. Accessed 17 May 2012
http://www.pintsforprostates.org/?page_id=2. Accessed 17 May 2012
Georgia’s Comprehensive Cancer Control Plan 2008–2012. Georgia Cancer Coalition and the Georgia Department of Human Resources, Division of Public Health October 29, 2007. Available at: http://www.georgiacancer.org/gcccp/pdfs/GA_Cancer_Plan.pdf
Jemal A, Center MM, DeSantis C, Ward EM (2010) Global patterns of cancer incidence and mortality rates and trends. Cancer Epidemiol Biomarkers Prev 19(8):1893–1907
Hsing AW, Tsao L, Devesa SS (2000) International trends and patterns of prostate cancer incidence and mortality. Int J Cancer 85(1):60–67
Acknowledgments
Dr. Wagner is partially sponsored by a grant from the Georgia Cancer Coalition (Proposal 038505) to the Cancer Epidemiology, Prevention and Control Program (CEPC) at the Georgia Cancer Center (Dr. John Vena).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wagner, S.E., Bauer, S.E., Bayakly, A.R. et al. Prostate cancer incidence and tumor severity in Georgia: descriptive epidemiology, racial disparity, and geographic trends. Cancer Causes Control 24, 153–166 (2013). https://doi.org/10.1007/s10552-012-0101-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10552-012-0101-0