Abstract
Purpose
Breast cancer is the most frequently diagnosed tumour, representing nearly 30% of all new cases in women. Radiotherapy (RT) plays a crucial role in the management of breast cancer. The objective of this study is to assess modesty in patients undergoing RT for breast cancer and take their suggestions and ideas into consideration to enhance the quality of treatment in this regard.
Methods
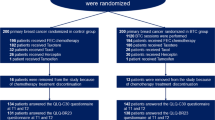
The study enrolled 555 breast cancer patients undergoing adjuvant RT in three Italian centres. Patients completed a self-test questionnaire assessing their comfort level concerning modesty during therapy and their relationship with strangers and healthcare professionals. The impact of religious views and potential changes in sexuality were also examined.
Results
Results showed that modesty was a common concern across the overall cohort of patients, with discomfort in being undressed during RT correlating with discomfort experienced in other daily life situations. Most patients felt more at ease with same sex healthcare workers. Age was also a major factor with younger patients generally feeling more comfortable with healthcare workers of the same age group. Interestingly, the surgical technique used (mastectomy vs. quadrantectomy) did not significantly influence modesty perceptions. Patients provided valuable suggestions to improve privacy and modesty during RT.
Conclusion
This study demonstrates that modesty is an important issue for women undergoing RT, which can be influenced by personal characteristics and hospital-related factors. A reflection about the need to address modesty concerns and to incorporate dedicated interventions for protecting patients’ physical and emotional well-being is warranted. Initiatives to improve communication, involvement, and body image support should also be integrated into the care path of patients to better their overall therapeutic experience. This study paves the way for broader research and interventions in daily cancer care.



Similar content being viewed by others
Data availability
Enquiries about data availability should be directed to the authors.
References
Dafni U, Tsourti Z, Alatsathianos I (2019) Breast cancer statistics in the European Union: incidence and survival across European countries. Breast Care (Basel) 14:344–353. https://doi.org/10.1159/000503219
Gradishar WJ, Moran MS, Abraham J et al (2023) NCCN Guidelines® insights: breast cancer, version 4.2023. Natl Compr Canc Netw 21:594–608. https://doi.org/10.6004/jnccn.2023.0031
Probst H, Rosbottom K, Crank H, Stanton A, Reed H (2021) The patient experience of radiotherapy for breast cancer: a qualitative investigation as part of the SuPPORT 4 All study. Radiography (Lond) 27:352–359. https://doi.org/10.1016/j.radi.2020.09.011
Gregucci F, Fozza A, Falivene S, Italian Society of Radiotherapy and Clinical Oncology (AIRO) Breast Group et al (2020) Present clinical practice of breast cancer radiotherapy in Italy: a nationwide survey by the Italian Society of Radiotherapy and Clinical Oncology (AIRO) Breast Group. Radiol Med 125:674–682. https://doi.org/10.1007/s11547-020-01147-5
Meattini I, Palumbo I, Becherini C et al (2022) The Italian Association for Radiotherapy and Clinical Oncology (AIRO) position statements for postoperative breast cancer radiation therapy volume, dose, and fractionation. Radiol Med 127:1407–1411. https://doi.org/10.1007/s11547-022-01563-9
Carnevale A, Scaringi C, Scalabrino G et al (2013) Radiation therapy after breast reconstruction: outcomes, complications, and patient satisfaction. Radiol Med 11:1240–1250. https://doi.org/10.1007/s11547-013-0947-6
Kim K, Park H (2021) Factors affecting anxiety and depression in young breast cancer survivors undergoing radiotherapy. Eur J Oncol Nurs 50:101898. https://doi.org/10.1016/j.ejon.2021.101898
Hauth F, De-Colle C, Weidner N, Heinrich V, Zips D, Gani C (2021) Quality of life and fatigue before and after radiotherapy in breast cancer patients. Strahlenther Onkol 197:281–287. https://doi.org/10.1007/s00066-020-01700-1
Halkett GK, Kristjanson LJ, Lobb E, O’Driscoll C, Taylor M, Spry N (2010) Meeting breast cancer patients’ information needs during radiotherapy: what can we do to improve the information and support that is currently provided? Eur J Cancer Care (Engl) 19:538–547. https://doi.org/10.1111/j.1365-2354.2009
Andrews CS (2011) Defining and exploring modesty in Jewish American women. J Religion Health 50:818–834. https://doi.org/10.1007/s10943-010-9435-7
Grilo AM, Gomes AI, Monsanto F, Albino D, Augusto C, Pragana C (2020) First day of radiotherapy for women with breast cancer: predictors of anxiety. Support Care Cancer 28(3):1241–1248. https://doi.org/10.1007/s00520-019-04902-1.
Grilo AM, Vieira L, Carolino E, Costa M, Galaio S, Melo I, Geão A, Santos A, Colarinha P (2020) Cancer patient experience in a nuclear medicine department: comparison between bone scintigraphy and 18F-FDG PET/CT. J Nucl Med Technol 48(3):254–262. https://doi.org/10.2967/jnmt.119.239285.
Reagan LJ (1997) Engendering the dread disease: women, men, and cancer. Am J Public Health 87:1779–1787. https://doi.org/10.2105/ajph.87.11.1779
Epstein RM, Borrell i Carrió F (2001) Pudor, honor, and autoridad: the evolving patient-physician relationship in Spain. Patient Educ Couns 45:51–57. https://doi.org/10.1016/s0738-3991(01)00143-4
Padela AI et al (2012) Religious values and healthcare accommodations: voices from the American Muslim community. J Gen Intern Med 27:708–715. https://doi.org/10.1007/s11606-011-1965-5
Yosef AR (2008) Health beliefs, practice, and priorities for health care of Arab Muslims in the United States. J Transcult Nurs 19:284–291. https://doi.org/10.1177/1043659608317450
National Radiotherapy Advisory Group, Breakthrough Breast Cancer, Breast Cancer Care (2005) What breast cancer patients want from a world class radiotherapy service
Kim HY (2017) Statistical notes for clinical researchers: Chi-squared test and Fisher’s exact test. Restor Dent Endod 42:152–155. https://doi.org/10.5395/rde.2017.42.2.152.
Guimond ME, Salman K (2013) Modesty matters: cultural sensitivity and cervical cancer prevention in Muslim women in the United States. Nurs Womens Health 17:210–216. https://doi.org/10.1111/1751-486X.12034.
Dareng EO, Jedy-Agba E, Bamisaye P et al (2015) Influence of spirituality and modesty on acceptance of self-sampling for cervical cancer screening. PLoS ONE 10:e0141679. https://doi.org/10.1371/journal.pone.0141679
Gabel P, Larsen MB, Nielsen PB, Svendstrup DB, Andersen B (2017) Satisfaction, discomfort, obligations, and concerns in population-based breast cancer screening: cross-sectional study in a Danish population. BMC Health Serv Res 17:489. https://doi.org/10.1186/s12913-017-2438-2
Hughes MK, Lacy S, Nelson CJ (2015) “Sexual dysfunction” in geriatric psycho-oncology: a quick reference on the psychosocial dimensions of cancer symptom management. In: Holland JC, Weiss Wiesel T, Nelson CJ, Roth AJ, Alici Y. Oxford University Press
Dinapoli L, Colloca G, Di Capua B, Valentini V (2021) Psychological aspects to consider in breast cancer diagnosis and treatment. Curr Oncol Rep 23(3):38. https://doi.org/10.1007/s11912-021-01049-3
Barbagli M, Dalla Zuanna G, Garelli F (2010) La sessualità degli italiani. Il Mulino, Bologna
Garelli F, Ferrero Camoletto R (2017) Oltre il comune senso del pudore? Riflessioni a margine di una ricerca sociologica sulla sessualità. Spazio Filosofico. (ISSN: 2038-6788)
Palmisano S, Todesco L (2021) Modernizzazione e differenze di genere nella religiosità: il caso italiano. 87-XLV 2021 Quaderni di Sociologia
Chan CW, Choi KC, Wong RS et al (2016) Examining the cervical screening behaviour of women aged 50 or above and its predicting factors: a population-based survey. Int J Environ Res Public Health 13:1195. https://doi.org/10.3390/ijerph13121195
Hewitt M, Devesa SS, Breen N (2004) Cervical cancer screening among U.S. women: analyses of the 2000 National Health Interview Survey. Prev Med 39:270–278. https://doi.org/10.1016/j.ypmed.2004.03.035
Kołodziejczyk A, Pawłowski T (2019) Negative body image in breast cancer patients. Adv Clin Exp Med 28:1137–1142. https://doi.org/10.17219/acem/103626
Janz NK, Mujahid M, Lantz PM et al (2005) Population-based study of the relationship of treatment and sociodemographics on quality of life for early stage breast cancer. Qual Life Res 14:1467–1479. https://doi.org/10.1007/s11136-005-0288-6
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, Carbone PP (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by LD, MC, SPC, CE, VP, GS. Statistical analysis was performed by EB. Data interpretation: LB, EB and LB. The first draft of the manuscript was written by LB, LD and EB. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Boldrini, L., Dinapoli, L., Boccia, E. et al. Coping with modesty during radiotherapy for breast cancer: a multicentric study. Breast Cancer Res Treat (2024). https://doi.org/10.1007/s10549-024-07365-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10549-024-07365-z