Abstract
Purpose
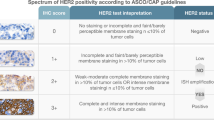
Treatment for HER2-low [defined as ImmunoHistoChemistry (IHC) 1 + or 2 + and negative/normal in Situ Hybridization (ISH)] breast cancer patients is rapidly evolving, yet we lack critical information about the HER2-low population.
Methods
We conducted a retrospective cohort study of women aged 18 years or older diagnosed with breast cancer between 2010 and 2016 in North Carolina. Analyses were conducted for the overall cohort and a stage IV sub-cohort. We examined demographic and clinical characteristics, and characterized prevalence of HER2-low disease and healthcare utilization. We estimated adjusted rate ratios for the association between HER2 classifications and utilization outcomes, and hazard ratios for 3-year all cause mortality (stage IV only).
Results
The overall and stage IV cohorts included 12,965 and 635 patients, respectively. HER2-low patients represented more than half of both cohorts (59% overall, 53% stage IV). HER2-low patients were more likely than IHC 0 patients to have hormone receptor (HR)-positive disease. In the stage IV cohort, HER2-low patients were more likely to be Black (26% vs. 16% IHC 0, p = 0.0159). In both cohorts, rates of hospitalizations were slightly higher among HER2-low patients. There were no survival differences between HER2-low and IHC 0 among stage IV patients.
Conclusion
New treatment options for HER2-low breast cancer may have potential for significant impact at the population level particularly for patients with stage IV disease. In light of racial differences between HER2-low and IHC 0 patients observed in our cohort, research- and practice-based efforts to ensure equitable adoption of new treatment guidelines for patients with HER2-low metastatic breast cancer will be essential.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the Cancer Information & Population Health Resource (CIPHR) at the University of North Carolina Lineberger Cancer Center, but restrictions apply to the availability of these data, which were used under agreement for the current study, and so are not publicly available. Data are however available from the authors upon entering into usage agreements as managed by CIPHR.
References
Siegel RL, Miller KD, Fuchs HE, Jemal A (2021) Cancer Statistics, 2021. CA Cancer J Clin 71(1):7–33
Testa U, Castelli G, Pelosi E (2020) Breast cancer: a molecularly heterogenous disease needing subtype-specific treatments. Med Sci (Basel) 8(1):18
Liang Y, Zhang H, Song X, Yang Q (2020) Metastatic heterogeneity of breast cancer: molecular mechanism and potential therapeutic targets. Semin Cancer Biol 60:14–27
Tarantino P, Hamilton E, Tolaney SM, Cortes J, Morganti S, Ferraro E, Marra A, Viale G, Trapani D, Cardoso F et al (2020) HER2-low breast cancer: pathological and clinical landscape. J Clin Oncol 38(17):1951–1962
Marchio C, Annaratone L, Marques A, Casorzo L, Berrino E, Sapino A (2021) Evolving concepts in HER2 evaluation in breast cancer: heterogeneity, HER2-low carcinomas and beyond. Semin Cancer Biol 72:123–135
Gilcrease MZ, Woodward WA, Nicolas MM, Corley LJ, Fuller GN, Esteva FJ, Tucker SL, Buchholz TA (2009) Even low-level HER2 expression may be associated with worse outcome in node-positive breast cancer. Am J Surg Pathol 33(5):759–767
Wolff AC, Hammond MEH, Allison KH, Harvey BE, McShane LM, Dowsett M (2018) HER2 testing in breast cancer: american society of clinical oncology/college of american pathologists clinical practice guideline focused update summary. J Oncol Pract 14(7):437–441
Modi S, Jacot W, Yamashita T, Sohn J, Vidal M, Tokunaga E, Tsurutani J, Ueno NT, Prat A, Chae YS et al (2022) Trastuzumab deruxtecan in previously treated HER2-low advanced breast cancer. N Engl J Med 387(1):9–20
National Comprehensive Cancer Network (NCCN). Breast Cancer (Version 4.2023). Retrieved February 17, 2023 from https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf
Meyer AM, Olshan AF, Green L, Meyer A, Wheeler SB, Basch E, Carpenter WR (2014) Big data for population-based cancer research: the integrated cancer information and surveillance system. N C Med J 75(4):265–269
U.S. Department of Agriculture (2010) Rural-urban commuting area codes https://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes/. Accessed 17 Feb 2023
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
American Cancer Society (2022) Survival rates for breast cancer. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html. Accessed 17 Feb 2023
Schettini F, Chic N, Braso-Maristany F, Pare L, Pascual T, Conte B, Martinez-Saez O, Adamo B, Vidal M, Barnadas E et al (2021) Clinical, pathological, and PAM50 gene expression features of HER2-low breast cancer. NPJ Breast Cancer 7(1):1
Viale G, Niikura N, Tokunaga E, Aleynikova O, Hayashi N, Sohn J, O’Brien C, Higgins G, Varghese D, James GD et al (2022) Retrospective study to estimate the prevalence of HER2-low breast cancer (BC) and describe its clinicopathological characteristics. J Clin Oncol 40(16):1087
Ren JX, Gong Y, Ling H, Hu X, Shao ZM (2019) Racial/ethnic differences in the outcomes of patients with metastatic breast cancer: contributions of demographic, socioeconomic, tumor and metastatic characteristics. Breast Cancer Res Treat 173(1):225–237
DeSantis CE, Ma J, Gaudet MM, Newman LA, Miller KD, Goding Sauer A, Jemal A, Siegel RL (2019) Breast cancer statistics, 2019. CA Cancer J Clin 69(6):438–451
Jatoi I, Anderson WF, Rao SR, Devesa SS (2005) Breast cancer trends among black and white women in the United States. J Clin Oncol 23(31):7836–7841
Reeder-Hayes K, Peacock Hinton S, Meng K, Carey LA, Dusetzina SB (2016) Disparities in use of human epidermal growth hormone receptor 2-targeted therapy for early-stage breast cancer. J Clin Oncol 34(17):2003–2009
Acknowledgements
Work on this study was supported by the Cancer Information and Population Health Resource, UNC Lineberger Comprehensive Cancer Center, with funding provided by the University Cancer Research Fund via the state of North Carolina. We would also like to thank Amy Clark for project support and assistance with manuscript formatting and submission. The findings and conclusions in this presentation are those of the author(s) and do not necessarily represent the views of the North Carolina Department of Health and Human Services, Division of Public Health.
Funding
This study was funded by AstraZeneca and Daiichi Sankyo, Inc.
Author information
Authors and Affiliations
Contributions
MAD, DKC, LEW, SBW, CL: contributed to the conception and design of the study. BEJ: conducted data analyses. All authors contributed toward the interpretation of the findings. DKC: created the initial draft, while all authors contributed to critical review and revision of this manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
DKC, BEJ, LS, LEW received research funding from AstraZeneca. CL, EF are employed by AstraZeneca. JK, SM are employed by Daiichi Sankyo, Inc.
Ethical approval
The University of North Carolina at Chapel Hill Biomedical Institutional Review Board and Duke University Health System Institutional Review Boards reviewed/approved the study.
Consent to participate
This study was conducted under a waiver of the informed consent requirement by the University of North Carolina at Chapel Hill Biomedical Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Check, D.K., Jackson, B.E., Reeder-Hayes, K.E. et al. Characteristics, healthcare utilization, and outcomes of patients with HER2-low breast cancer. Breast Cancer Res Treat 203, 329–338 (2024). https://doi.org/10.1007/s10549-023-07142-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-023-07142-4