Abstract
Purpose
Little is known about racial variations in the financial impact of cancer care. Using data from a national survey of racially diverse patients with metastatic breast cancer, we examined racial/ethnic patterns in employment and cost-management (i.e., financial coping) behaviors.
Methods
We conducted an online survey of patients with metastatic breast cancer. Participants reported on socio-demographic characteristics, employment, and financial coping behaviors. We employed adjusted modified Poisson regressions to evaluate racial/ethnic differences in changes in work for pay and financial coping.
Results
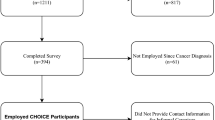
Our analysis included 1052 respondents from 41 states, including Non-Hispanic Blacks (NHB, 9%), Hispanics (7%), Asians/Pacific Islanders/Native Hawaiians (API/NH, 10%), American Indians/Alaskan Natives (AI/AN, 8%), and Non-Hispanic Whites (NHW, 66%). In adjusted analyses comparing NHWs with patients of color, patients of color were more likely to take unpaid leave (NHB Adjusted Risk Ratio [ARR] = 2.27; 95% CI 1.54, 3.34), take paid leave (Hispanic ARR = 2.27; 95% CI 1.54, 1.29), stop work (AI/AN ARR = 1.22; 95% CI 1.05, 1.41), and reduce work hours (AI/AN ARR = 1.33; 95% CI 1.14, 1.57). Patients of color were more likely than NHWs to stop treatment (NHB ARR = 1.22; 95% CI 1.08, 1.39), borrow money from friends/family (Hispanic ARR = 1.75; 95% CI 1.25, 2.44), skip other medical bills (API/NH ARR = 2.02; 95% CI 1.54, 2.63), and skip non-medical bills (AI/AN ARR = 1.67 95% CI 1.06, 2.63). Non-Hispanic Whites more commonly reported using savings or skipping a vacation to help manage costs.
Conclusions
Racial/ethnic differences exist in employment changes and financial coping among metastatic breast cancer patients, with patients of color experiencing worse consequences. Equity must be a guiding principle in strategies addressing financial burden during cancer care.




Similar content being viewed by others
References
Miller JW, Smith JL, Ryerson AB et al (2017) Disparities in breast cancer survival in the United States (2001–2009): findings from the CONCORD-2 study. Cancer 123:5100–5118. https://doi.org/10.1002/cncr.30988
DeSantis CE, Fedewa SA, Goding Sauer A et al (2016) Breast cancer statistics, 2015: convergence of incidence rates between black and white women. CA Cancer J Clin 66:31–42. https://doi.org/10.3322/caac.21320
Iqbal J, Ginsburg O, Rochon PA et al (2015) Differences in breast cancer stage at diagnosis and cancer-specific survival by race and ethnicity in the United States. JAMA 313:165. https://doi.org/10.1001/jama.2014.17322
Zafar SY (2016) Financial toxicity of cancer care: it’s time to intervene. J. Natl, Cancer Inst, p 108
Kent EE, Forsythe LP, Yabroff KR et al (2013) Are survivors who report cancer-related financial problems more likely to forgo or delay medical care? Cancer. https://doi.org/10.1002/cncr.28262
Lathan CS, Cronin A, Tucker-Seeley R et al (2016) Association of financial strain with symptom burden and quality of life for patients with lung or colorectal cancer. J Clin Oncol 34:1732–1740. https://doi.org/10.1200/JCO.2015.63.2232
Zafar SY, McNeil RB, Thomas CM et al (2015) Population-based assessment of cancer survivors’ financial burden and quality of life: a prospective cohort study. J Oncol Pract 11:145–150. https://doi.org/10.1200/JOP.2014.001542
Zafar SY, Peppercorn JM, Schrag D et al (2013) The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist 18:381–390. https://doi.org/10.1634/theoncologist.2012-0279
Yabroff KR, Dowling EC, Guy GP et al (2016) Financial hardship associated with cancer in the United States: findings from a population-based sample of adult cancer survivors. J Clin Oncol. https://doi.org/10.1200/JCO.2015.62.0468
Ramsey S, Blough D, Kirchhoff A et al (2013) Washington State cancer patients found to be at greater risk for bankruptcy than people without a cancer diagnosis. Heal Aff 32:1143–1152. https://doi.org/10.1377/hlthaff.2012.1263
Clark CR, Ommerborn MJ, Coull B et al (2016) Income inequities and medicaid expansion are related to racial and ethnic disparities in delayed or forgone care due to cost. Med Care 54:555–561. https://doi.org/10.1097/MLR.0000000000000525
Wheeler SB, Spencer JC, Pinheiro LC et al (2018) Financial impact of breast cancer in black versus white women. J Clin Oncol 36:1695–1701. https://doi.org/10.1200/JCO.2017.77.6310
Jagsi R, Pottow JAE, Griffith KA et al (2014) Long-term financial burden of breast cancer: experiences of a diverse cohort of survivors identified through population-based registries. J Clin Oncol. https://doi.org/10.1200/JCO.2013.53.0956
Yousuf Zafar S, Peppercorn JM, Schrag D et al (2013) The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist. https://doi.org/10.1634/theoncologist.2012-0279
Altice CK, Banegas MP, Tucker-Seeley RD, Yabroff KR (2017) Financial hardships experienced by cancer survivors: a systematic review. J. Natl, Cancer Inst, p 109
Irwin B, Kimmick G, Altomare I et al (2014) Patient experience and attitudes toward addressing the cost of breast cancer care. Oncologist 19:1135–1140. https://doi.org/10.1634/theoncologist.2014-0117
Zafar SY, Peppercorn JM, Schrag D et al (2013) The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist 18:381–390. https://doi.org/10.1634/theoncologist.2012-0279
Bureau-of-Labor-Statistics, U. (2015) Labor force characteristics by race and ethnicity, 2014. US Bur Labor Stat
Swanberg JE, Pitt-Catsouphes M, Drescher-Burke K (2005) A question of justice : disparities in employees’ access to flexible schedule arrangements. J Fam Issues 26:866–895. https://doi.org/10.1177/0192513X05277554
Jeszeck C (2015) Contingent workforce: size, characteristics, earnings, and benefits (GAO-15-168R). Washington, DC
Spelten ER, Sprangers MAG, Verbeek JHA (2002) Factors reported to influence the return to work of cancer survivors: a literature review. Psychooncology 11:124–131. https://doi.org/10.1002/pon.585
Disability discrimination. In: US Equal Employ. Oppor. Commission. https://www.eeoc.gov/laws/types/disability.cfm. Accessed 15 May 2019
Bickell NA, LePar F, Wang JJ, Leventhal H (2007) Lost opportunities: physicians’ reasons and disparities in breast cancer treatment. J Clin Oncol 25:2516–2521
Bickell NA (2002) Race, ethnicity, and disparities in breast cancer: victories and challenges. Women’s Heal Issues 12:238–251
Spencer JC, Samuel CA, Rosenstein DL et al (2018) Oncology navigators’ perceptions of cancer-related financial burden and financial assistance resources. Support Care Cancer 26:1315–1321. https://doi.org/10.1007/s00520-017-3958-3
US Census Bureau. Wealth, asset ownership, & debt of household details tables: 2015. https://www.census.gov/data/tables/2015/demo/wealth/wealth-asset-ownership.html. Accessed 15 July 2019
Williams DR, Priest N, Anderson NB (2016) Understanding associations among race, socioeconomic status, and health: patterns and prospects. Health Psychol 35:407–411. https://doi.org/10.1037/hea0000242
Chen M-T, Sun H-F, Zhao Y et al (2017) Comparison of patterns and prognosis among distant metastatic breast cancer patients by age groups: a SEER population-based analysis. Sci Rep 7:9254. https://doi.org/10.1038/s41598-017-10166-8
Banegas MP, Guy GP, de Moor JS et al (2016) For working-age cancer survivors, medical debt and bankruptcy create financial hardships. Health Aff 35:54–61. https://doi.org/10.1377/hlthaff.2015.0830
Funding
This work was supported by the National Comprehensive Cancer Network and Pfizer Independent Grants for Learning & Change (no grant number); and the National Cancer Institute (1 K01CA218473-01A1 to C.A.S).
Author information
Authors and Affiliations
Contributions
Conceptualization: CAS, DLR, KERH, MLM, JBS, SBW. Data Curation: CAS, JCS. Formal analysis: JCS. Methodology: CAS, JCS. Visualization: JCS. Project administration: MLM. Writing review and editing: CAS, JCS, DLR, KERH, MLM, JBS, SBW. Final approval of manuscript: CAS, JCS. Financial acquisition: DLR, SBW
Corresponding author
Ethics declarations
Conflict of interest
Ms. Sellers reports payment as a consultant with Pfizer which was unrelated to the submitted work. None of the other study authors have any conflicts of interest to disclose, beyond receiving independent grant funding from Pfizer.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The experiments conducted in this study comply with the current laws of the country in which they were performed.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Samuel, C.A., Spencer, J.C., Rosenstein, D.L. et al. Racial differences in employment and cost-management behaviors in patients with metastatic breast cancer. Breast Cancer Res Treat 179, 207–215 (2020). https://doi.org/10.1007/s10549-019-05449-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-019-05449-9