Abstract
Purpose
Experimental laboratory data have indicated a protective effect of vitamin D on breast cancer progression, while epidemiological evidence is growing. Using pharmacy claims data, this study investigates the association between vitamin D supplement use initiated after a breast cancer diagnosis and associated mortality.
Methods
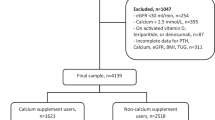
Women aged 50–80 years with a record of invasive breast cancer were identified on the National Cancer Registry Ireland database (n = 5417). Initiation of de novo vitamin D post-diagnosis was identified from linked national prescription data (n = 2581, 49%). Multivariate Cox proportional hazards models were used to estimate adjusted HRs (95% CIs) for breast cancer-specific mortality.
Results
There was a 20% reduction in breast cancer-specific mortality in de novo vitamin D users (modelled as a time-varying variable) compared to non-users (HR 0.80; 95% CI 0.64–0.99, p = 0.048) and the reduction was greater at 49% (HR 0.51; 95% CI 0.34–0.74, p < 0.001), if vitamin D was initiated soon after the breast cancer diagnosis (within 6 months).
Conclusions
In this large national breast cancer cohort, de novo vitamin D use post-diagnosis was found to be associated with a reduction in breast cancer-specific mortality. Vitamin D, therefore, has the potential as a non-toxic and inexpensive agent to improve survival in breast cancer patients. Findings support the need for RCTs exploring the effect of vitamin D supplementation on breast cancer survival.



Similar content being viewed by others
Data availability
Data used in this research are stored and governed by the National Cancer Registry of Ireland.
References
Cashman KD, Dowling KG, Skrabakova Z, Gonzalez-Gross M, Valtuena J, De Henauw S et al (2016) Vitamin D deficiency in Europe: pandemic? Am J Clin Nutr 103(4):1033–1044
Theodoratou E, Tzoulaki I, Zgaga L, Ioannidis JP (2014) Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials. BMJ 348:g2035
Duffy MJ, Murray A, Synnott NC, O’Donovan N, Crown J (2017) Vitamin D analogues: potential use in cancer treatment. Crit Rev Oncol/Hematol 112:190–197
Kim Y, Je Y (2014) Vitamin D intake, blood 25(OH)D levels, and breast cancer risk or mortality: a meta-analysis. Br J Cancer 110(11):2772–2784
Vaughan-Shaw PG, O’Sullivan F, Farrington SM, Theodoratou E, Campbell H, Dunlop MG et al (2017) The impact of vitamin D pathway genetic variation and circulating 25-hydroxyvitamin D on cancer outcome: systematic review and meta-analysis. Br J Cancer 116(8):1092–1110
Bolland MJ, Grey A, Gamble GD, Reid IR (2011) Calcium and vitamin D supplements and health outcomes: a reanalysis of the Women’s Health Initiative (WHI) limited-access data set. Am J Clin Nutr 94(4):1144–1149
Sperati F, Vici P, Maugeri-Sacca M, Stranges S, Santesso N, Mariani L et al (2013) Vitamin D supplementation and breast cancer prevention: a systematic review and meta-analysis of randomized clinical trials. PloS ONE 8(7):e69269
Keum N, Giovannucci E (2014) Vitamin D supplements and cancer incidence and mortality: a meta-analysis. Br J Cancer 111(5):976–980
Pradhan AD, Manson JE (2016) Update on the Vitamin D and OmegA-3 trial (VITAL). J Steroid Biochem Mol Biol 155(Pt B):252–256
Augustin LSA, Libra M, Crispo A, Grimaldi M, De Laurentiis M, Rinaldo M et al (2017) Low glycemic index diet, exercise and vitamin D to reduce breast cancer recurrence (DEDiCa): design of a clinical trial. BMC Cancer 17:69
Poole EM, Shu X, Caan BJ, Flatt SW, Holmes MD, Lu W et al (2013) Postdiagnosis supplement use and breast cancer prognosis in the after breast cancer pooling project. Breast Cancer Res Treat 139(2):529–537
Gallagher CM, More K, Kamath T, Masaquel A, Guerin A, Ionescu-Ittu R et al (2016) Delay in initiation of adjuvant trastuzumab therapy leads to decreased overall survival and relapse-free survival in patients with HER2-positive non-metastatic breast cancer. Breast Cancer Res Treat 157(1):145–156
Raphael MJ, Biagi JJ, Kong W, Mates M, Booth CM, Mackillop WJ (2016) The relationship between time to initiation of adjuvant chemotherapy and survival in breast cancer: a systematic review and meta-analysis. Breast Cancer Res Treat 160(1):17–28
Mazidi M, Rezaie P, Vatanparast H, Kengne AP (2017) Effect of statins on serum vitamin D concentrations: a systematic review and meta-analysis. Eur J Clin Investig 47(1):93–101
O’Brien K, Comber H, Sharp L (2014) Completeness of case ascertainment at the Irish National Cancer Registry. Ir J Med Sci 183(2):219–224
Barron TI, Cahir C, Sharp L, Bennett K (2013) A nested case-control study of adjuvant hormonal therapy persistence and compliance, and early breast cancer recurrence in women with stage I-III breast cancer. Br J Cancer 109(6):1513–1521
Sinnott SJ, Bennett K, Cahir C (2017) Pharmacoepidemiology resources in Ireland-an introduction to pharmacy claims data. Eur J Clin Pharmacol 73(11):1449–1455
Velentgas P, Dreyer NA, Nourjah P, Smith SR, Torchia MM (2013) Developing a protocol for observational comparative effectiveness research: A user’s guide. Agency for Healthcare Research and Quality
Lund JL, Richardson DB, Sturmer T (2015) The active comparator, new user study design in pharmacoepidemiology: historical foundations and contemporary application. Curr Epidemiol Rep 2(4):221–228
Suissa S (2008) Immortal time bias in pharmaco-epidemiology. Am J Epidemiol 167(4):492–499
Vitamin D and Health (2016) The Scientific Advisory Committee on Nutrition (SACN) UK
Barron TI, Murphy LM, Brown C, Bennett K, Visvanathan K, Sharp L (2015) De novo post-diagnosis aspirin use and mortality in women with stage i–iii breast cancer. Cancer Epidemiol Biomark Prev 24(6):898–904
Coleman R, Powles T, Paterson A, Gnant M, Anderson S, Diel I et al (2015) Adjuvant bisphosphonate treatment in early breast cancer: meta-analyses of individual patient data from randomised trials. Lancet 386(10001):1353–1361
Marshall SF, Bernstein L, Anton-Culver H, Deapen D, Horn-Ross PL, Mohrenweiser H et al (2005) Nonsteroidal anti-inflammatory drug use and breast cancer risk by stage and hormone receptor status. J Natl Cancer Inst 97(11):805–812
Schneeweiss S, Maclure M (2000) Use of comorbidity scores for control of confounding in studies using administrative databases. Int J Epidemiol 29(5):891–898
Schneeweiss S, Seeger JD, Maclure M, Wang PS, Avorn J, Glynn RJ (2001) Performance of comorbidity scores to control for confounding in epidemiologic studies using claims data. Am J Epidemiol 154(9):854–864
Howlader N, Ries LA, Mariotto AB, Reichman ME, Ruhl J, Cronin KA (2010) Improved estimates of cancer-specific survival rates from population-based data. J Natl Cancer Inst 102(20):1584–1598
Smith A, Murphy L, Bennett K, Barron TI (2017) Patterns of statin initiation and continuation in patients with breast or colorectal cancer, towards end-of-life. Supportive Care Cancer 25(5):1629–1637
Austin PC (2011) An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res 46(3):399–424
Jeffreys M, Redaniel MT, Martin RM (2015) The effect of pre-diagnostic vitamin D supplementation on cancer survival in women: a cohort study within the UK Clinical Practice Research Datalink. BMC Cancer 15:670
Li M, Chen P, Li J, Chu R, Xie D, Wang H (2014) Review: the impacts of circulating 25-hydroxyvitamin D levels on cancer patient outcomes: a systematic review and meta-analysis. J Clin Endocrinol Metab 99(7):2327–2336
Maalmi H, Ordonez-Mena JM, Schottker B, Brenner H (2014) Serum 25-hydroxyvitamin D levels and survival in colorectal and breast cancer patients: systematic review and meta-analysis of prospective cohort studies. Eur J Cancer 50(8):1510–1521
Greenlee H, Kwan ML, Ergas IJ, Strizich G, Roh JM, Wilson AT et al (2014) Changes in vitamin and mineral supplement use after breast cancer diagnosis in the Pathways Study: a prospective cohort study. BMC Cancer 14:382
Heaney RP (2008) Vitamin D in health and disease. Clin J Am Soc Nephrol 3(5):1535–1541
Rose AA, Elser C, Ennis M, Goodwin PJ (2013) Blood levels of vitamin D and early stage breast cancer prognosis: a systematic review and meta-analysis. Breast Cancer Res Treat 141(3):331–339
Zeichner SB, Koru-Sengul T, Shah N, Liu Q, Markward NJ, Montero AJ et al (2015) Improved clinical outcomes associated with vitamin D supplementation during adjuvant chemotherapy in patients with HER2+ nonmetastatic breast cancer. Clin Breast Cancer 15(1):e1–e11
Chubak J, Boudreau DM, Wirtz HS, McKnight B, Weiss NS (2013) Threats to validity of nonrandomized studies of postdiagnosis exposures on cancer recurrence and survival. J Natl Cancer Inst 105(19):1456–1462
Muscogiuri G, Sorice GP, Prioletta A, Policola C, Della Casa S, Pontecorvi A et al (2010) 25-Hydroxyvitamin D concentration correlates with insulin-sensitivity and BMI in obesity. Obesity 18(10):1906–1910
Kennel KA, Drake MT (2013) Vitamin D in the cancer patient. Curr Opin Support Palliat Care 7(3):272–277
Chen P, Hu P, Xie D, Qin Y, Wang F, Wang H (2010) Meta-analysis of vitamin D, calcium and the prevention of breast cancer. Breast Cancer Res Treat 121(2):469–477
Acknowledgements
We would like to thank the National Cancer Registry in Ireland (NCRI), the General Registry Office and the Irish HSE-PCRS for providing access to the data upon which this study was based. In particular, we are grateful to the Data Team at the NCRI for linking the datasets and Dr. Sandra Deady and Mr. Christopher Brown for preparing these for analysis. The interpretation and reporting of these data are the responsibility of the authors and should in no way be seen as the official policy or interpretation of the NCRI or the Irish HSE-PCRS. The authors would also like to thank Prof Michael J. Duffy for his advice and input while preparing the manuscript and Dr. Ian Barron who originally proposed the manuscript.
Funding
This work was supported by the Irish Cancer Society Collaborative Cancer Research Centre BREAST-PREDICT (CCRC13GAL) and the Health Research Board Ireland (HRB-RL/2015/1579). The Health Research Board Ireland and the Irish Cancer Society had no role in the study design; collection, analysis, and interpretation of data; writing of the report; or the decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no competing interest.
Ethical approval
The use for research of anonymised data held by the NCRI and PCRS is covered by the Health (Provision of Information) Act 1997.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Madden, J.M., Murphy, L., Zgaga, L. et al. De novo vitamin D supplement use post-diagnosis is associated with breast cancer survival. Breast Cancer Res Treat 172, 179–190 (2018). https://doi.org/10.1007/s10549-018-4896-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-018-4896-6