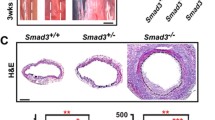
In patients with an ascending aorta aneurysm, restructuring of all its layers and, first of all, the intima and media was revealed. The thickness of the intima was 79.3±63.1 μm in patients with aortic diameter <55 mm (group Ao<55) and 162.7±177.4 μm (p<0.05) in patients with aortic diameter ⩾55 mm (Ao⩾55 group), the thickness of the aortic media was 1184.0±198.2 and 1144.3±288.4 μm, respectively. In patients of the Ao<55 group, aortic dilatation was accompanied by compensatory thickening of the inner and middle layers of the aorta. In the Ao⩾55 group, thinning of the aortic media, fragmentation of elastic fibers, and its cystic degeneration were revealed. c-kit+ Stem cells were detected in the subendothelium of the thickened intima of the dilated ascending aorta. The appearance of c-kit+ cells correlated with intimal remodeling and its colonization with CD34+ and CD44+ myofibroblast-like cells.
Similar content being viewed by others
References
Erbel R, Aboyans V, Boileau C, Bossone E, Bartolomeo RD, Eggebrecht H, Evangelista A, Falk V, Frank H, Gaemperli O, Grabenwöger M, Haverich A, Iung B, Manolis AJ, Meijboom F, Nienaber CA, Roffi M, Rousseau H, Sechtem U, Sirnes PA, Allmen RS, Vrints CJ; ESC Committee for Practice Guidelines. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases: Document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult. The Task Force for the Diagnosis and Treatment of Aortic Diseases of the European Society of Cardiology (ESC). Eur. Heart J. 2014;35(41):2873-2926. https://doi.org/10.1093/eurheartj/ehu281
Zhang J, Wang L, Fu W, Wang C, Guo D, Jiang J, Wang Y. Smooth muscle cell phenotypic diversity between dissected and unaffected thoracic aortic media. J. Cardiovasc. Surg. (Torino). 2013;54(4):511-521.
Malashicheva A, Kostina D, Kostina A, Irtyuga O, Voronkina I, Smagina L, Ignatieva E, Gavriliuk N, Uspensky V, Moiseeva O, Vaage J, Kostareva A. Phenotypic and functional changes of endothelial and smooth muscle cells in thoracic aortic aneurysms. Int. J. Vasc. Med. 2016;2016:3107879. https://doi.org/10.1155/2016/3107879
An Z, Liu Y, Song ZG, Tang H, Yuan Y, Xu ZY. Mechanisms of aortic dissection smooth muscle cell phenotype switch. J. Thorac. Cardiovasc. Surg. 2017;154(5):1511-1521.e6. https://doi.org/10.1016/j.jtcvs.2017.05.066
Yuan SM, Wu N. Aortic α-smooth muscle actin expressions in aortic disorders and coronary artery disease: An immunohistochemical study. Anatol. J. Cardiol. 2018;19(1):11-16. https://doi.org/10.14744/AnatolJCardiol.2017.7839
Wang L, Zhang J, Fu W, Guo D, Jiang J, Wang Y. Association of smooth muscle cell phenotypes with extracellular matrix disorders in thoracic aortic dissection. J. Vasc. Surg. 2012;56(6):1698-1709, 1709.e1. https://doi.org/10.1016/j.jvs.2012.05.084
Bode-Jänisch S, Schmidt A, Günther D, Stuhrmann M, Fieguth A. Aortic dissecting aneurysms — histopathological findings. Forensic Sci. Int. 2012;214(1-3):13-17. https://doi.org/10.1016/j.forsciint.2011.07.006
Belov IuV, Fedorov DN, Taaev BK, Daabul’ AS. Specifics of histological structure of ascending aortic wall in aneurysm. Kardiol. Serd.-Sosud. Khir. 2013;6(2):34-36. Russian.
Luneva EB, Uspenskyi VE, Mitrofanova LB, Paidimirova MI, Kandinskyi AV, Zemtsovsky EV. Causal factors in the development of thoracic aortic aneurysm. Ross. Kardiol. Zh. 2013;18(1):19-22. https://doi.org/10.15829/1560-4071-2013-1-19-22
Grewal N, Velders BJJ, Gittenberger-de Groot AC, Poelmann R, Klautz RJM, Van Brakel TJ, Lindeman JHN. A systematic histopathologic evaluation of type-A aortic dissections implies a uniform multiple-hit causation. J. Cardiovasc. Dev. Dis. 2021;8(2):12. https://doi.org/10.3390/jcdd8020012
Tang PC, Coady MA, Lovoulos C, Dardik A, Aslan M, Elefteriades JA, Tellides G. Hyperplastic cellular remodeling of the media in ascending thoracic aortic aneurysms. Circulation. 2005;112(8):1098-1105. https://doi.org/10.1161/CIRCULATIONAHA.104.511717
Takaichi S, Yutani C, Fujita H, Yamamoto A. Ultrastructural studies on the phenotypic modulation of human intimal smooth muscle cells. Atherosclerosis. 1993;100(2):197-211. https://doi.org/10.1016/0021-9150(93)90206-a
Rao RN, Falls DG, Gerrity RG, Sethuraman SN, Thiruvaiyaru DS. Intimal thickness and layering, and smooth muscle cell phenotypes in aorta of youth. Pathobiology. 2000;68(1):18-28. https://doi.org/10.1159/000028111
Orlandi A, Bochaton-Piallat ML, Gabbiani G, Spagnoli LG. Aging, smooth muscle cells and vascular pathobiology: implications for atherosclerosis. Atherosclerosis. 2006;188(2):221-230. https://doi.org/10.1016/j.atherosclerosis.2006.01.018
Grewal N, Girdauskas E, DeRuiter M, Goumans MJ, Poelmann RE, Klautz RJM, Gittenberger-de Groot AC. The role of hemodynamics in bicuspid aortopathy: a histopathologic study. Cardiovasc. Pathol. 2019;41:29-37. https://doi.org/10.1016/j.carpath.2019.03.002
Klima T, Spjut HJ, Coelho A, Gray AG, Wukasch DC, Reul GJ Jr, Cooley DA. The morphology of ascending aortic aneurysms. Hum. Pathol. 1983;14(9):810-817. https://doi.org/10.1016/s0046-8177(83)80303-7
Sagakyants AB, Kit OI, Ulyanova EP, Zlatnik EYu, Novikova IA, Shulgina OG, Gevorkyan YA, Soldatkina NV, Samoylenko NS, Dzhenkova EA, Shaposhnikov AV. Features of expression of CD133 and CD44 markers of tumor stem cells with metastatic and non-metastatic gastric cancer. Sib. Onkol. Zh. 2021;20(1):97-104. https://doi.org/10.21294/1814-4861-2021-20-1-97-104
Yousef S, Matsumoto N, Dabe I, Mori M, Landry AB, Lee SR, Kawamura Y, Yang C, Li G, Assi R, Vallabhajosyula P, Geirsson A, Moeckel G, Humphrey JD, Tellides G. Quantitative not qualitative histology differentiates aneurysmal from nondilated ascending aortas and reveals a net gain of medial components. Sci. Rep. 2021;11(1):13185. https://doi.org/10.1038/s41598-021-92659-1
Bockeria LA, Serov RA, Rychin SV. Morphological changes characteristic of the ascending aorta wall at its aneurysmal dilatation in patients with Marfan syndrome. Byull. Nauch. Tsentr Serd.-Sosud. Khirurg im. A. N. Bakuleva Ross. Akad. Med. Nauk. 2016;17(5):19-28. Russian.
Matthias Bechtel JF, Noack F, Sayk F, Erasmi AW, Bartels C, Sievers HH. Histopathological grading of ascending aortic aneurysm: comparison of patients with bicuspid versus tricuspid aortic valve. J. Heart Valve Dis. 2003;12(1):54-59; discussion 59-61.
Chen PY, Qin L, Li G, Malagon-Lopez J, Wang Z, Bergaya S, Gujja S, Caulk AW, Murtada SI, Zhang X, Zhuang ZW, Rao DA, Wang G, Tobiasova Z, Jiang B, Montgomery RR, Sun L, Sun H, Fisher EA, Gulcher JR, Fernandez-Hernando C, Humphrey JD, Tellides G, Chittenden TW, Simons M. Smooth muscle cell reprogramming in aortic aneurysms. Cell Stem Cell. 2020;26(4):542-557.e11. https://doi.org/10.1016/j.stem.2020.02.013
Della Corte A, Quarto C, Bancone C, Castaldo C, Di Meglio F, Nurzynska D, De Santo LS, De Feo M, Scardone M, Montagnani S, Cotrufo M. Spatiotemporal patterns of smooth muscle cell changes in ascending aortic dilatation with bicuspid and tricuspid aortic valve stenosis: focus on cell-matrix signaling. J. Thorac. Cardiovasc. Surg. 2008;135(1):8-18, 18.e1-2. https://doi.org/10.1016/j.jtcvs.2007.09.009
Ishii T, Asuwa N. Collagen and elastin degradation by matrix metalloproteinases and tissue inhibitors of matrix metalloproteinase in aortic dissection. Hum. Pathol. 2000;31(6):640-346. https://doi.org/10.1053/hupa.2000.7642
Maurel E, Shuttleworth CA, Bouissou H. Interstitial collagens and ageing in human aorta. Virchows Arch. A Pathol. Anat. Histopathol. 1987;410(5):383-390. https://doi.org/10.1007/BF00712757
Novikova EG, Galankina IE. Age-related morphological changes in the aortic wall in dissecting aneurysm. Arkh. Patol. 2015;77(1):18-22. Russian. https://doi.org/10.17116/patol201577118-22
Yutani C, Takaichi S, Yamamoto A. The role of vascular smooth-muscle cells in atherogenesis: phenotypic modulation of the medial smooth-muscle cells in the aortic bifurcation. Jpn Circ. J. 1991;55(10):1003-1009. https://doi.org/10.1253/jcj.55.1003
Lesauskaite V, Tanganelli P, Sassi C, Neri E, Diciolla F, Ivanoviene L, Epistolato MC, Lalinga AV, Alessandrini C, Spina D. Smooth muscle cells of the media in the dilatative pathology of ascending thoracic aorta: morphology, immunoreactivity for osteopontin, matrix metalloproteinases, and their inhibitors. Hum. Pathol. 2001;32(9):1003-1011. https://doi.org/10.1053/hupa.2001.27107
Ikonomidis JS, Jones JA, Barbour JR, Stroud RE, Clark LL, Kaplan BS, Zeeshan A, Bavaria JE, Gorman JH 3rd, Spinale FG, Gorman RC. Expression of matrix metalloproteinases and endogenous inhibitors within ascending aortic aneurysms of patients with bicuspid or tricuspid aortic valves. J. Thorac. Cardiovasc. Surg. 2007;133(4):1028-1036. https://doi.org/10.1016/j.jtcvs.2006.10.083
Blunder S, Messner B, Aschacher T, Zeller I, Türkcan A, Wiedemann D, Andreas M, Blüschke G, Laufer G, Schachner T, Bernhard D. Characteristics of TAV-and BAV-associated thoracic aortic aneurysms — smooth muscle cell biology, expression profiling, and histological analyses. Atherosclerosis. 2012;220(2):355-361. https://doi.org/10.1016/j.atherosclerosis.2011.11.035
Zhao G, Lu H, Chang Z, Zhao Y, Zhu T, Chang L, Guo Y, Garcia-Barrio MT, Chen YE, Zhang J. Single-cell RNA sequencing reveals the cellular heterogeneity of aneurysmal infrarenal abdominal aorta. Cardiovasc. Res. 2021;117(5):1402-1416. https://doi.org/10.1093/cvr/cvaa214
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Kletochnye Tekhnologii v Biologii i Meditsine, No. 1, pp. 52-61, March, 2023
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sukhacheva, T.V., Penyaeva, E.V., Soborov, M.A. et al. Morphological Features of the Ascending Aorta Remodeling and Activation of Regeneratory Potential in Intima when Forming Aneurysm. Bull Exp Biol Med 175, 162–171 (2023). https://doi.org/10.1007/s10517-023-05829-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10517-023-05829-8