Abstract
The global COVID-19 pandemic and associated lockdown measures have caused disruptions to sexual health services and created additional barriers to the continuity of HIV pre-exposure prophylaxis (PrEP) among key populations. This review provides an examination of the influences of the pandemic on engagement in the PrEP care continuum. Using the PRISMA guideline, 46 studies were included in this review and the synthesis. Most of the studies were conducted in high-income settings through quantitative analysis. A majority of studies examining the changes in PrEP use suggested a decline or discontinuation in PrEP uptake during the pandemic. The most common reasons for stopping using PrEP were perceived barriers to PrEP-related care, having reduced sexual behaviors and fewer sexual partners, and reduced perceived risk of HIV infection. Limited studies documenting an increase in PrEP uptake were all in specific PrEP optimizing programs. During the pandemic, there is also an emerging trend of switching to on-demand PrEP from daily oral PrEP. Future studies should understand the mechanism of strategies that facilitated the improvements during the pandemic. PrEP implementation programs should consider alternative PrEP modalities and provide consistent and comprehensive knowledge about correct information.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The COVID-19 pandemic and its associated measures have posed significant challenges to health systems and access to healthcare services across the globe. These unprecedented consequences may increase health inequality and exacerbate the disparities that already exist among the most vulnerable populations, such as people living with and are at risk of HIV infection. Since the beginning of the COVID-19 crisis, there has accelerating evidence suggesting that the ongoing pandemic has changed the provision of sexual health services and created additional social and structural barriers to HIV prevention services[1]. These consequences could not only threaten the public health gains in HIV prevention in the past decade but also severely impact the overall progress of the HIV/AIDS 90-90-90 targets[2, 3]. For example, in a recent report published by the United States (U.S.) Centers for Disease Control and Prevention (CDC), HIV testing had dropped dramatically in both healthcare and non-healthcare settings during the first year of the pandemic[4], particularly among priority populations such as men who have sex with men (MSM) and transgender individuals. Similarly, data from 65 primary care clinics in South Africa showed a nearly 50% decrease in HIV testing at the beginning of the lockdown measures[5]. Results from multiple mathematical models also suggested that the potential COVID-19 related effects of disruptions to the HIV program could lead to increased HIV incidence and population-level mortality[6]. Urgent programmatic and policy responses are needed to mitigate the negative effects of the COVID-pandemic on the existing HIV epidemic.
One key strategy to prevent HIV transmission and End the HIV Epidemic is to scale up and implement pre-exposure prophylaxis (PrEP) among the key community and populations[7]. PrEP is a medicine taken to prevent getting HIV infection and reduce the risk of getting HIV when taken as prescribed[8]. Both clinical trials and real-world longitudinal studies have shown the effectiveness of PrEP in reducing HIV incidence among populations at elevated HIV risk[9,10,11,12,13,14]. Previous modeling work has also demonstrated the potential benefit of scaling-up PrEP and expanding PrEP coverage in averting HIV infections across different countries and settings[15,16,17,18,19]. Until the 1st quarter of 2022, it is estimated that nearly 2.3 million individuals had initiated PrEP worldwide[20]. Undoubtedly, the pandemic and associated measures also disrupted the continuity of PrEP care across the globe among priority populations. For example, in the U.S., one in 7 young MSM PrEP users stopped using it during the pandemic[21]. In Wales, the introduction of COVID-19 related measures was associated with reducing PrEP use and PrEP adherence[22], and similar phenomena were reported in many other settings[23,24,25,26]. The report from U.S. CDC also suggests a slowing PrEP prescription in 2020. However, these findings were not consistent. In fact, one study in South Africa observed more PrEP initiation, improved persistence, and lower risks of client-initiated stops among female sex workers in 2020, compared to the pre-pandemic period[27].
Importantly, ten years after oral PrEP was approved for HIV prevention, there is still a critical gap in implementing this biomedical intervention, including lower utilization among key populations and suboptimal PrEP adherence around the globe. The ongoing pandemic and associated measures may pose increased HIV risk and additional barriers to the broader use of PrEP among those in need. Understanding these barriers, particularly during the COVID-19 pandemic, and examining the changes in PrEP use are paramount to ensuring its effective implementation and public health benefit. Therefore, the objectives of this review are (1) collectively describe the changes in PrEP use and persistence during the pandemic; (2) to summarize the factors associated with and reasons for these changes, and (3) to describe the emerging PrEP modalities during the COVID-19 pandemic. The results of this review will provide experiences and lessons we learned from the pandemic, which could support the optimization of future programs and policy changes, especially for the preparation of future endemics and pandemics that might reduce the delivery and use of sexual health care services.
Methods
This review was conducted in line with the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) guideline[28]. A comprehensive database search was performed in the following databases in July 2022: PubMed, Embase, PsycInfo, CINAHL, Web of Science, and Medline for articles published since 2020. The search terms include (COVID-19 OR SARS-CoV-2 OR Severe acute respiratory syndrome coronavirus 2 OR 2019nCoV OR HCoV-19) AND (Pre-exposure prophylaxis OR PrEP OR pre-exposure chemoprophylaxis OR Truvada OR Descovy). A manual search was also conducted for other relevant studies using reference lists of retrieved citations and Google Scholar. Additionally, conference abstracts for major HIV conferences (AIDS 2020, CROI 2021, Adherence 2021) were searched to identify additional relevant records.
To be eligible for inclusion, studies had to be (1) in the English language or have an English Abstract; (2) study data were collected since March 2020, when the World Health Organization declared a global pandemic or associated lock-down measures were implemented in the study setting; (3) have at least one outcome of PrEP use and/or (dis)continuation in their study findings. To characterize the impact of COVID-19, studies that described the changes or disruptions in the delivery of PrEP were also included. Besides, all types of studies were included if they provided empirical data.
All database search records were imported to Covidence (Veritas Health Innovation Ltd), a software that removes duplicate studies automatically. After duplicates were removed, all article titles and abstracts were screened for eligibility, and if they met the inclusion criteria, the study was included for full-text review. Any studies that cannot be decided solely by title and abstract were also progressed to full-text review. Next step, all articles were screened to determine whether they met all the eligibility, and those that met all the criteria were included in the final data extraction. For each selected article, standard data (author, year published, study design, study population) and study-specific information (PrEP use and (dis)continuation, changes in PrEP delivery, behaviors among PrEP users, etc.) were imported into a standardized data extraction form. Descriptive statistics were used to present the characteristics of included studies, including study location, population, and study design. Inductive thematic analysis was used to qualitatively identify themes across article findings, which are reported by overarching themes along with supporting evidence and quotes extracted from included articles.
Results
Study Selection
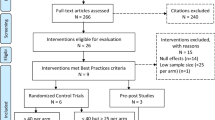
The initial database search yielded 1106 records. After removing duplicates, 963 studies were processed for the title and abstract review. Among those, 74 records met the eligibility and therefore were included for full-text review. After reviewing the full article, 46 studies met the inclusion criteria and were included in the final data extract and synthesis. Study selection was presented in a modified PRISMA flowchart (see Fig. 1).
Characteristics of Included Studies
A full description and details of included studies’ characteristics are summarized (see Table 1). These studies were conducted in the United States (n = 18)[21, 29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45], United Kingdom (n = 6)[22, 46,47,48,49,50], Australia (n = 4)[23, 51,52,53], Brazil (n = 4)[54,55,56,57], Portugal (n = 3)[54, 56, 58], Kenya (n = 2)[59, 60], Belgium (n = 2)[24, 26], South Africa (n = 2)[25, 27]. The rest of the studies were conducted in Canada[61], Croatia[62], Ireland[63], Zimbabwe[64], Netherlands[65], the Philippines[66], France[67]. One study included data from 20 different countries[68]. Most studies (n = 42) utilized quantitative methods, with 2 qualitative studies[29, 43] and 2 mixed-method designs [39, 60]. A majority of studies (n = 27) were comprised of MSM, three of which explicitly focused on young MSM[21, 29, 30]. Four studies included transgender women, two among female sex workers[27, 64], one study was conducted among people who inject drugs (opioid-dependent individuals)[38], and one among pregnant women[25].
Changes in PrEP use and Continuation
Many studies documented the decline or discontinuation of PrEP uptake among individuals who used PrEP pre-pandemic worldwide. Chan et al. found that 12% of individuals discontinued PrEP after the shelter-in-place order was initiated in San Francisco[45]. In a national cohort of cisgender men, transgender women, and transgender men who have sex with men in the U.S., nearly 30% of the sample completed stopped taking PrEP[41]. Studies in Australia and France noted even higher rates of PrEP discontinuation during the pandemic, with 41.8% and 58.8% of MSM stopping PrEP during the lockdown and COVID-19-related restrictions[52, 67]. In Amsterdam, Netherlands, Jongen et al. suggested that among MSM reported study data before and after March 15th 2020, two in three (67%) decreased PrEP uptake after March 15th, 2020[65]. Similarly, researchers in Wales also found that the odds of participants taking PrEP on a given day were 56% lower after introducing COVID-19 measures[22]. These changes have been noted among several populations at high risk for HIV infection. Among a national sample of YMSM aged 17–24 years old in the U.S., Hong et al. found that 1 in 7 YMSM stopped using PrEP during the pandemic[21]. Two studies conducted in Australia and France also discovered that compared to those who continued using PrEP, those who had discontinued PrEP during the COVID-19 restrictions were younger[52, 67].
Conversely, one study in San Francisco suggested that, based on their data from the San Francisco primary care clinics, there was no reduction in PrEP use after the shelter-in-place orders were implemented[33]. Three other studies found that PrEP uptake had increased since the pandemic began. According to Muhula et al. (2021), PrEP uptake had increased by 24% among the various population in Kibera, Kenya, adjusting for other study variables[59]. Matambanadzo et al. (2021) discovered that among female sex workers in Zimbabwe, PrEP uptake has increased monthly since May 2020 and peaked at an initiation rate in September 2020[64]. Lastly, among female sex workers at TB HIV care in eThekwini, South Africa, researchers observed more PrEP initiation, improved PrEP persistence, and lower discontinuation during the pandemic[27] (see Table 2).
Reasons for Changing PrEP Uptake and Persistence
The most commonly reported reasons for changes in PrEP use and persistence are limited access to healthcare services, and changes in sexual behaviors and perceived risk of HIV. First, the pandemic and associated measures placed additional barriers to routine healthcare services. PrEP users said they were unable to get providers’ appointments or unable to communicate with their providers[44, 45]. Many also reported having difficulty refilling the prescription and getting their medication[21, 31, 32, 37, 55]. Qualitative results also further illustrated these barriers,
“I couldn’t get PrEP filled because my appointment was cancelled because of the pandemic.”[29]
Besides, the closure of the clinic and reduced hours of operation also negatively impacted PrEP persistence among PrEP users. Camp and Saberi found that the top PrEP challenge during the pandemic was laboratory testing[44], also suggested by Chan et al. [45]. On the other hand, studies also found that PrEP-related clinic visits had declined significantly. For example, in Belgium, PrEP users visited the clinic less frequently in 2020 than in 2019[24], and PrEP service had a 50% decline in visits in Croatia[62]. In South Africa, missed PrEP visits among pregnant women increased significantly during the nationwide lockdown[25]. In addition, one study in Providence, Rhode Island, discovered that based on their patient record in a PrEP program, there was a decrease in PrEP visits over time during three distinct phases of COVID-19. This decrease, however, was not statistically significant[35]. In a qualitative study among opioid-dependent individuals who inject drugs, a quarter of the participants said they had difficulty getting their PrEP prescription and had trouble refilling the medication at their pharmacy[38].
The other main reason for changes in PrEP use and persistence during COVID-19 was changes in sexual behaviors and perceived risk of HIV infection. Specifically, many studies found that those individuals who stopped using PrEP reported stopping sexual encounters or decreasing sexual activities[21, 44, 53, 55] and having a reduced number of casual sexual partners[39, 52, 53]. In a qualitative study, MacCarthy et al. discovered that PrEP discontinuation was related to a substantial decrease in the number of participants’ sexual partners, and these individuals, therefore, felt like they no longer needed to take PrEP[39]. Indeed, reduced sexual activities and the number of sexual partners also changed their perceived risk of HIV. In Ireland, the number of individuals seeking PrEP & PEP decreased dramatically during the pandemic. Some patients stopped PrEP themselves as they were not at risk of HIV and did not want to take unnecessary medication[63]. Another study also found that discontinuing PrEP during the lockdown was less likely to receive an HIV test recently[52].
Other factors associated with changes in PrEP use and persistence include younger age and financial vulnerability. For example, one study in Australia found that men who discontinued PrEP during the restrictions were significantly younger than those who continued using PrEP (mean age: 42.44 vs. 45.24, p = 0.0031). Rao et al. also found that younger women were more likely to discontinue PrEP by not returning compared to 25 years and older[27]. In a sample of Black MSM and transgender women in Chicago, the financial travel burden since the lockdown was significantly associated with perceived difficulty accessing PrEP[42].
Very few studies have identified the facilitators of PrEP use during the COVID-19 pandemic. One study in Brazil found that the main reasons for individuals continuing PrEP were fear of HIV infection, having sex with casual partners, having HIV-positive partners, and believing that PrEP protected against COVID-19[55]. A similar study also suggested nearly half of MSM in Brazil were taking PrEP to prevent COVID-19[54]. In South Africa, the most common reasons pregnant women start PrEP were preventing infant HIV and unknown or positive partner serostatus[25]. Chone et al. (2021) also found that using PrEP was associated with having chemsex during the pandemic in Portugal[58].
Switch to on-demand PrEP
One emerging theme is that individuals switched oral-daily PrEP dosing to ‘event-driven’ or on-demand PrEP to continue the PrEP care during the pandemic[23, 37, 44, 50, 53, 63]. Among men who have sex with men who attended PrEP care at the Melbourne Sexual Health Centre, two studies found that 5% and 2% of the PrEP users switched to on-demand PrEP[23, 53]. Similar results were found in studies in the Southern U.S. and Ireland[37, 63]. One study further examined the barriers and facilitators of using the on-demand PrEP dosing option. According to Camp and Saberi[44], the most common reasons for switching from daily PrEP to on-demand PrEP were having sex less frequently and wanting to take less pills. The main barriers to using this dosing option include unexpected sexual behaviors that result in missing the first dose, difficulty remembering the dosing after the double dose, and lack of provider knowledge[44]. Their results also revealed high medication adherence based on the 2-1-1 component. Lastly, a study in the U.K. found that the uptake of on-demand PrEP had increased significantly since the pandemic began, and clinicians were confident to discuss this dosing option with the clients[50].
Discussion
This review of 46 studies suggests that the global COVID-19 pandemic and associated measures have disrupted the continuity of PrEP care across various at-risk populations. Research has already suggested the negative impact of the COVID-19 pandemic on the HIV care and prevention continuum, including additional barriers to HIV and other STI testing, difficulties refilling antiretroviral therapy and seeing HIV care providers [4, 69]. Our results add to the evidence by suggesting disruptions in PrEP use and continuation. Most studies found that individuals in PrEP care stopped using PrEP or indicated difficulties in getting PrEP care. The most common reasons for stopping using PrEP were experiencing barriers to PrEP care services, reduced sexual behaviors, and lowered self-perceived risk of HIV. Only a few studies observed increased PrEP initiation and persistent PrEP use during the pandemic. However, these studies were conducted in a PrEP optimization or an integrated PrEP service program. Future research should investigate which implementation strategies these programs enacted had facilitated the positive changes, and such strategies should be continued and taken forward for improvement.
Of note, most of the included studies were cross-sectional and quantitative designs. Despite the fact that many studies asked their participants how PrEP use and persistence had changed since the pandemic, our knowledge of the longitudinal effect of the pandemic on PrEP care engagement is still limited. Future studies may consider utilizing longitudinal or cohort data to assess the pandemic’s long-term impact. Additional research using a qualitative approach may be a better way of more fully understanding the impact of the pandemic on PrEP use. Besides, a vast majority of the studies were conducted in high-income and developed countries and areas and only a handful of studies examined the changes in PrEP use and persistence in low- and middle-income countries and the Global South. Compared to high-income settings, PrEP scale up and implementation for HIV prevention have been slow, but a growing number of countries are adopting the WHO PrEP guidelines and recommendations[70]. In addition, researchers and policymakers must examine the changes in PrEP use and persistence in these areas to maintain the public health gains in global PrEP use and achieve greater PrEP equity, especially given the already existing barriers to PrEP implementation before the pandemic.
Despite most studies documenting the decrease in PrEP use, very few studies assessed PrEP eligibility and identified PrEP candidates during the pandemic. HIV risk should be evaluated in the context of behavioral risk exposure. For example, one study in the U.S. found that among those MSM who met the CDC’s PrEP criteria, 86.5% were not using PrEP[21]. To maximize the public health benefit of this biomedical intervention, assessments on PrEP eligibility should be conducted regularly to assess one’s need for PrEP care. During the pandemic, many PrEP clinics and organizations have limited operating hours and capacities for individual HIV risk assessment. Virtual services such as eHealth, telehealth, and technology-based intervention may mitigate the negative impacts of the COVID-19 pandemic on PrEP-related services[71, 72]. In addition, recent literature also suggests utilizing data science approaches to predict HIV risk behaviors and deliver individualized messages and interventions[73, 74]. Such novel approach may have the potential to maintain comprehensive HIV and PrEP prevention service delivery and address potential COVID-19 related service interruptions.
Consistent with pre-pandemic, young people continue to experience barriers to PrEP care. Despite being limited, several studies found that young MSM and young women were more likely to stop using PrEP during the pandemic. Globally, adolescents and young adults bear a disproportionately high burden of HIV infection [75] and continue to experience difficulty accessing and maintaining PrEP care[76, 77]. The ongoing pandemic could further exacerbate their already existing vulnerabilities. PrEP initiation for adolescents and young adults may have been delayed due to the pandemic, which could have long-term effects on PrEP use and persistence among this population. A recent study among adolescents aged 13–18 found that PrEP use was extremely low among sexually active YMSM, while risk behaviors such as condomless anal sex persist during the pandemic[78]. Public health programs and providers should prioritize this population for future HIV prevention efforts.
Lastly, there is a growing trend of switching to on-demand PrEP from daily dosing among PrEP users during the pandemic. On-demand PrEP or event-driven PrEP is an alternative dosing option for individuals with less frequent sexual encounters and fewer risk exposures[79]. This involves taking 2 pills 2–24 h before sex and 1 pill daily for the next 2 days and is therefore known as the “2-1-1” PrEP. It was first incorporated into European clinical guidelines in 2015 and endorsed by the World Health Organization in 2019[79, 80]. This change may be explained by the fact PrEP users only use PrEP when they are in need because of the shortage of medication supply and having difficulty refilling their pills due to the lockdown measures across the globe. It could also reflect the changes in one’s perceived risk of HIV and risk evaluation. Indeed, due to decreased frequency of sexual behaviors and the number of sexual partners, PrEP users may only intake the pills when needed. As the interest and demand for this dosing option are growing, it is critical for public health officials and providers to offer different options matching one’s needs and implement consistent and comprehensive knowledge and education about correct dosing and adherence for on-demand PrEP users. Areas and settings that bear a high HIV burden should work with their Public Health agencies to endorse on-demand PrEP dosing options and provide alternative PrEP modalities based on individual unique needs. Future studies should continue exploring novel PrEP modalities that will combat the barriers to traditional daily oral PrEP.
This review has several limitations. First, this review focused on reviewing the literature and summarizing the emerging evidence instead of providing a rigorous assessment of the quality of included studies. Secondly, only published studies in English were screened. It is possible that some studies in other languages were inadvertently missed. Lastly, due to the heterogeneity of the included studies, a meta-analysis was not performed to derive aggregate statistical evidence about the changes in PrEP use and persistence. Despite these limitations, this review highlighted the impact of the global COVID-19 pandemic on the engagement of PrEP care across different settings and populations and provided insights and evidence for future PrEP implementation programs and interventions.
References
Santos G-M, Hong C, Wilson N, et al. Persistent disparities in COVID-19-associated impacts on HIV prevention and care among a global sample of sexual and gender minority individuals. Glob Public Health. 2022;0:1–16.
Guaraldi G, Borghi V, Milic J, et al. The impact of COVID-19 on UNAIDS 90-90-90 targets: calls for New HIV Care Models. In: Open Forum Infectious Diseases. Oxford University Press US; 2021. p. ofab283.
The Joint United Nations Programme on HIV/AIDS. 90-90-90: An ambitious treatment target to help end the AIDS epidemic. 2014; 40.
DiNenno EA. HIV Testing Before and During the COVID-19 Pandemic—United States, 2019–2020. MMWR Morbidity and Mortality Weekly Report; 71.
Dorward J, Khubone T, Gate K, et al. The impact of the COVID-19 lockdown on HIV care in 65 south african primary care clinics: an interrupted time series analysis. The Lancet HIV. 2021;8:e158–65.
Jewell BL, Mudimu E, Stover J, et al. Potential effects of disruption to HIV programmes in sub-saharan Africa caused by COVID-19: results from multiple mathematical models. The Lancet HIV. 2020;7:e629–40.
Fauci AS, Redfield RR, Sigounas G, et al. Ending the HIV Epidemic: a plan for the United States. JAMA. 2019;321:844–5.
Guidance on Pre-Exposure Oral Prophylaxis (PrEP) for Serodiscordant Couples, Men and Transgender Women Who Have Sex with Men at High Risk of HIV: Recommendations for Use in the Context of Demonstration Projects. Geneva: World Health Organization, http://www.ncbi.nlm.nih.gov/books/NBK132003/ (2012, accessed 9 July 2020).
Grant RM, Lama JR, Anderson PL, et al. Preexposure Chemoprophylaxis for HIV Prevention in Men who have sex with men. N Engl J Med. 2010;363:2587–99.
Baeten JM, Donnell D, Ndase P, et al. Antiretroviral prophylaxis for HIV Prevention in Heterosexual Men and Women. N Engl J Med. 2012;367:399–410.
Heffron R, MUGO N. WERE E, et al. PrEP is efficacious for HIV-1 prevention among women using DMPA for Contraception. AIDS. 2014;28:2771–6.
Grulich AE, Jin F, Bavinton BR, et al. Long-term protection from HIV infection with oral HIV pre-exposure prophylaxis in gay and bisexual men: findings from the expanded and extended EPIC-NSW prospective implementation study. The Lancet HIV. 2021;8:e486–94.
Koss CA, Havlir DV, Ayieko J, et al. HIV incidence after pre-exposure prophylaxis initiation among women and men at elevated HIV risk: a population-based study in rural Kenya and Uganda. PLoS Med. 2021;18:e1003492.
Estcourt C, Yeung A, Nandwani R, et al. Population-level effectiveness of a national HIV preexposure prophylaxis programme in MSM. AIDS. 2021;35:665–73.
Jenness SM, Goodreau SM, Rosenberg E, et al. Impact of the Centers for Disease Control’s HIV Preexposure Prophylaxis Guidelines for Men who have sex with men in the United States. J Infect Dis. 2016;214:1800–7.
Hamilton DT, Rosenberg ES, Jenness SM, et al. Modeling the joint effects of adolescent and adult PrEP for sexual minority males in the United States. PLoS ONE. 2019;14:e0217315.
Khanna AS, Schneider JA, Collier N, et al. A modeling framework to inform PrEP initiation and retention scale-up in the context of Getting to Zero Initiatives. AIDS (London, England) 2019; 33: 1911.
Nichols BE, Boucher CA, van Dijk JH, et al. Cost-effectiveness of pre-exposure prophylaxis (PrEP) in preventing HIV-1 infections in rural Zambia: a modeling study. PLoS ONE. 2013;8:e59549.
Zhang L, Peng P, Wu Y, et al. Modelling the epidemiological impact and cost-effectiveness of PrEP for HIV Transmission in MSM in China. AIDS Behav. 2019;23:523–33.
PrEP Watch. A map-based tool to explore trends in oral PrEP use globally as countries introduce and scale up PrEP programs., https://data.prepwatch.org/ (accessed 22 November 2021).
Hong C, Horvath KJ, Stephenson R, et al. PrEP Use and Persistence Among Young Sexual Minority Men 17–24 Years Old During the COVID-19 Pandemic. AIDS Behav. Epub ahead of print 13 August 2021. DOI: https://doi.org/10.1007/s10461-021-03423-5.
Gillespie D, Couzens Z, de Bruin M, et al. PrEP use, sexual Behaviour, and PrEP Adherence among Men who have sex with men living in Wales Prior to and during the COVID-19 pandemic. AIDS and Behavior 2022; 1–12.
Chow EPF, Hocking JS, Ong JJ, et al. Changing the Use of HIV Pre-exposure Prophylaxis Among Men Who Have Sex With Men During the COVID-19 Pandemic in Melbourne, Australia. Open Forum Infectious Diseases; 7. Epub ahead of print 1 July 2020. DOI: https://doi.org/10.1093/ofid/ofaa275.
De Baetselier I, Apers L, Platteau T, et al. The impact of physical restriction measures imposed during the two waves of COVID-19 on chlamydia and gonorrhea diagnoses in Belgium. Results of an sexually transmitted infection clinic. Int J STD AIDS. 2021;32:998–1003.
Davey DLJ, Bekker L-G, Mashele N, et al. PrEP retention and prescriptions for pregnant women during COVID-19 lockdown in South Africa. The Lancet HIV. 2020;7:e735.
Reyniers T, Rotsaert A, Thunissen E, et al. Reduced sexual contacts with non-steady partners and less PrEP use among MSM in Belgium during the first weeks of the COVID-19 lockdown: results of an online survey. Sex Transm Infect. 2021;97:414–9.
Rao A, Mhlophe H, Comins C, et al. Persistence on oral pre-exposure prophylaxis (PrEP) among female sex workers in eThekwini, South Africa, 2016–2020. PLoS ONE. 2022;17:e0265434.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
Zapata JP, Dang M, Quinn KG, et al. COVID-19-Related disruptions to HIV Testing and Prevention among young sexual minority men 17–24 Years Old: a qualitative study using Synchronous Online Focus Groups, April-September 2020. Arch Sex Behav. 2022;51:303–14.
Xavier Hall CD, Javanbakht M, Iyer C, et al. Examining the impact of social distancing and methamphetamine use on sexual risk and intimate partner violence in sexual and gender minority young adults during the COVID-19 pandemic. Drug Alcohol Depend. 2022;232:109231.
Stephenson R, Sullivan SP, Pitter RA, et al. Are We Still Having Sex? Results of Round Two of the Love and Sex in the Time of COVID Survey with Gay, Bisexual and Other Men Who Have Sex with Men. AIDS Behav. Epub ahead of print 19 January 2022. DOI: https://doi.org/10.1007/s10461-022-03580-1.
Stephenson R, Chavanduka TMD, Rosso MT, et al. Sex in the Time of COVID-19: results of an online survey of Gay, bisexual and other men who have sex with men’s experience of sex and HIV Prevention during the US COVID-19 Epidemic. AIDS Behav. 2021;25:40–8.
Saberi P, Ming K, Hojilla JC, et al. HIV Preexposure Prophylaxis in the Time of COVID-19: how a robust and responsive HIV Preexposure Prophylaxis intervention can avert loss of HIV Prevention Coverage during a global pandemic. J Acquir Immune Defic Syndr. 2021;87:e173–6.
Saberi P, Ming K, Shrestha I, et al. Feasibility and acceptability of home-collected samples for human immunodeficiency virus preexposure prophylaxis and severe Acute Respiratory Syndrome Coronavirus 2 Laboratory tests in San Francisco Primary Care clinics. Open Forum Infect Dis. 2022;9:ofab657.
Rogers BG, Tao J, Maynard M, et al. Characterizing the impact of COVID-19 on Pre-Exposure Prophylaxis (PrEP) care. AIDS Behav. 2021;25:3754–7.
Rogers BG, Tao J, Darveau SC, et al. The impact of COVID-19 on sexual behavior and psychosocial functioning in a clinical sample of men who have sex with men using HIV pre-exposure Prophylaxis. AIDS Behav. 2022;26:69–75.
Pampati S, Emrick K, Siegler AJ, et al. Changes in sexual behavior, PrEP adherence, and Access to sexual Health Services because of the COVID-19 pandemic among a cohort of PrEP-Using MSM in the South. JAIDS J Acquir Immune Defic Syndr. 2021;87:639–43.
Mistler CB, Curley CM, Rosen AO, et al. The impact of COVID-19 on Access to HIV Prevention Services among opioid-dependent individuals. J Community Health. 2021;46:960–6.
MacCarthy S, Izenberg M, Barreras JL, et al. Rapid mixed-methods assessment of COVID-19 impact on Latinx sexual minority men and latinx transgender women. PLoS ONE. 2020;15:e0244421.
Hill BJ, Anderson B, Lock L. COVID-19 Pandemic, pre-exposure Prophylaxis (PrEP) care, and HIV/STI Testing among Patients receiving care in three HIV Epidemic Priority States. AIDS Behav. 2021;25:1361–5.
Grov C, Zohra F, Westmoreland DA, et al. Sex in the era of COVID-19 in a US national cohort of cisgender men, transgender women, and transgender men who have sex with men: April–May 2020. Arch Sex Behav. 2022;51:343–54.
Chen Y-T, Duncan DT, Del Vecchio N, et al. COVID-19–Related Stressors, Sex Behaviors, and HIV Status Neutral Care Among Black Men Who Have Sex With Men and Transgender Women in Chicago, USA. Journal of Acquired Immune Deficiency Syndromes (1999) 2021; 88: 261.
Bellman R, Mohebbi S, Nobahar N, et al. An observational survey assessing the extent of PrEP and PEP furnishing in San Francisco Bay Area pharmacies. J Am Pharmacists Association. 2022;62:370–7. e3.
Camp C, Saberi P. Facilitators and barriers of 2-1-1 HIV pre-exposure prophylaxis. PLoS ONE. 2021;16:e0251917.
Chan CT, Ming K, Camp C, et al. Sexual behaviors, Substance Use, and Quality of Life among individuals using PrEP in San Francisco during the COVID-19 pandemic shelter-in-place orders: a cross-sectional survey. JAIDS J Acquir Immune Defic Syndr. 2022;89:e39–42.
Gillespie D, Knapper C, Hughes D, et al. Early impact of COVID-19 social distancing measures on reported sexual behaviour of HIV pre-exposure prophylaxis users in Wales. Sex Transm Infect. 2021;97:85–7.
Sex Transm Infect 2021; sextrans-2021-055039.
Hyndman I, Nugent D, Whitlock GG, et al. COVID-19 restrictions and changing sexual behaviours in HIV-negative MSM at high risk of HIV infection in London, UK. Sex Transm Infect. 2021;97:521–4.
Ringshall M, Cooper R, Rawdah W, et al. Chemsex, sexual behaviour and STI-PrEP use among HIV-PrEP users during the COVID-19 pandemic in Brighton, UK. Sex Transm Infect 2021; sextrans-2021-055216.
Richardson D, Buck E, Parkhouse A, et al. Increased clinician confidence and uptake of event-based PrEP by men who have sex with men during the COVID-19 pandemic. Sex Transm Infect. 2022;98:152.
Traeger MW, Patel P, Guy R, et al. Changes in HIV preexposure prophylaxis prescribing in australian clinical services following COVID-19 restrictions. AIDS. 2021;35:155–7.
Hammoud MA, Grulich A, Holt M, et al. Substantial decline in use of HIV preexposure prophylaxis following introduction of COVID-19 physical distancing restrictions in Australia: results from a prospective observational study of gay and bisexual men. Journal of acquired immune deficiency syndromes (1999) 2021; 86: 22.
Chow EP, Hocking JS, Ong JJ, et al. Brief report: changes in PreP use, sexual practice, and use of face mask during sex among MSM during the second wave of COVID-19 in Melbourne, Australia. J Acquir Immune Defic Syndr. 2021;86:153.
de Sousa AFL, de Oliveira LB, Queiroz AAFLN, et al. Casual sex among men who have sex with men (MSM) during the period of sheltering in place to prevent the spread of COVID-19. Int J Environ Res Public Health. 2021;18:3266.
Torres TS, Hoagland B, Bezerra DRB, et al. Impact of COVID-19 pandemic on sexual minority populations in Brazil: an analysis of Social/Racial disparities in maintaining Social Distancing and a description of sexual behavior. AIDS Behav. 2021;25:73–84.
Sousa ÁFL de, Queiroz AAFLN, Lima SVMA, et al. Chemsex practice among men who have sex with men (MSM) during social isolation from COVID-19: multicentric online survey. Cad Saude Publica. 2020;36:e00202420.
Hoagland B, Torres TS, Bezerra DRB, et al. Telemedicine as a tool for PrEP delivery during the COVID-19 pandemic in a large HIV prevention service in Rio de Janeiro-Brazil. Brazilian J Infect Dis. 2020;24:360–4.
Chone JS, Lima SVMA, Fronteira I, et al. Factors associated with chemsex in Portugal during the COVID-19 pandemic. Revista Latino-Americana de Enfermagem; 29.
Muhula S, Opanga Y, Oramisi V, et al. Impact of the First Wave of the COVID-19 pandemic on HIV/AIDS programming in Kenya: evidence from Kibera Informal Settlement and COVID-19 Hotspot Counties. Int J Environ Res Public Health. 2021;18:6009.
Roche SD, Odoyo J, Irungu E, et al. A one-stop shop model for improved efficiency of pre-exposure prophylaxis delivery in public clinics in western Kenya: a mixed methods implementation science study. J Int AIDS Soc. 2021;24:e25845.
O’Byrne P, Musten A, Orser L, et al. At-home HIV self-testing during COVID: implementing the GetaKit project in Ottawa. Can J Public Health. 2021;112:587–94.
Bogdanić N, Javorić I, Belak Škugor S, et al. Initial impact of COVID-19 epidemic on HIV services in Croatia. Infektološki glasnik. 2020;40:79–80.
Quirke S, Quinn L, Hegarty D, et al. Virtual HIV pre-exposure prophylaxis outpatient service in the era of COVID-19. Int J STD AIDS. 2021;32:100–3.
Matambanadzo P, Busza J, Mafaune H, et al. ‘It went through the roof’: an observation study exploring the rise in PrEP uptake among zimbabwean female sex workers in response to adaptations during Covid-19. J Int AIDS Soc. 2021;24(Suppl 6):e25813.
Jongen VW, Zimmermann HML, Boyd A, et al. Transient changes in Preexposure Prophylaxis Use and daily sexual Behavior after the implementation of COVID-19 Restrictions among Men who have sex with men. J Acquir Immune Defic Syndr. 2021;87:1111–8.
Eustaquio PC, Figuracion R, Izumi K, et al. Outcomes of a community-led online-based HIV self-testing demonstration among cisgender men who have sex with men and transgender women in the Philippines during the COVID-19 pandemic: a retrospective cohort study. BMC Public Health. 2022;22:1–11.
Di Ciaccio M, Villes V, Michels D, et al. Impact of the early 2020 COVID-19 crisis and lockdown on PrEP use among men who have sex with men (MSM) in France. Sexually Transmitted Infections.
Rao A, Rucinski K, Jarrett BA, et al. Perceived Interruptions to HIV Prevention and Treatment Services Associated with COVID-19 for Gay, Bisexual, and other men who have sex with men in 20 countries. JAIDS J Acquir Immune Defic Syndr. 2021;87:644–51.
Meyer D, Slone SE, Ogungbe O, et al. Impact of the COVID-19 Pandemic on HIV Healthcare Service Engagement, Treatment Adherence, and Viral Suppression in the United States: A Systematic Literature Review. AIDS Behav. Epub ahead of print 2 August 2022. DOI: https://doi.org/10.1007/s10461-022-03771-w.
Global State of PrEP. https://www.who.int/groups/global-prep-network/global-state-of-prep (accessed 18 July 2022).
Patel P, Kerzner M, Reed JB, et al. Public Health Implications of adapting HIV pre-exposure Prophylaxis Programs for virtual service delivery in the context of the COVID-19 pandemic: systematic review. JMIR Public Health and Surveillance. 2022;8:e37479.
Hong C, Abrams LS, Holloway IW. Technology-based interventions to promote the HIV Preexposure Prophylaxis (PrEP) care continuum: protocol for a systematic review. JMIR Res Protoc. 2022;11:e33045.
Marcus JL, Sewell WC, Balzer LB, et al. Artificial Intelligence and Machine Learning for HIV Prevention: emerging approaches to ending the Epidemic. Curr HIV/AIDS Rep. 2020;17:171–9.
Ovalle A, Goldstein O, Kachuee M, et al. Leveraging Social Media Activity and Machine Learning for HIV and Substance abuse Risk Assessment: Development and Validation Study. J Med Internet Res. 2021;23:e22042.
UNAIDS U. All in to end adolescent AIDS. Geneva: Joint United Nations Programme on HIV/AIDS & United Nations Children’s Fund.
Owens C, Moran K, Mongrella M, et al. “It’s very inconvenient for Me”: a mixed-method study assessing barriers and facilitators of adolescent sexual minority males attending PrEP Follow-Up appointments. AIDS Behav. 2022;26:21–34.
Muhumuza R, Ssemata AS, Kakande A, et al. Exploring Perceived Barriers and Facilitators of PrEP Uptake among Young People in Uganda, Zimbabwe, and South Africa. Arch Sex Behav. 2021;50:1729–42.
Hong C, Huh D, Schnall R, et al. Changes in high-risk sexual behavior, HIV and other STI testing, and PrEP use during the COVID-19 pandemic in a longitudinal cohort of adolescent men who have sex with men 13 to 18 years old in the United States. AIDS Behav. Epub ahead of print 26 September 2022. DOI: https://doi.org/10.1007/s10461-022-03850-y.
World Health Organization. What’s the 2 + 1 + 1 Event-driven oral pre-exposure prophylaxis to prevent HIV for men who have sex with men: update to WHO’s recommendation on oral PrEP 2019.
Society EEAC. EACS Guidelines Version 8.0-October 2015. European AIDS Clinical Society (EACS).
Acknowledgements
I would like to thank all the researchers and practitioners who committed themselves to delivering and promoting PrEP care during the global COVID-19 pandemic. I also want to thank all the authors and participants of included studies.
Funding
N/A.
Author information
Authors and Affiliations
Contributions
CH conceptualized the research questions, conducted the literature review, synthesized the data, and written up the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The author declared no conflict of interest.
Ethics Approval
N/A.
Informed Consent
N/A.
Consent for Publication
N/A.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hong, C. Characterizing the Impact of the COVID-19 Pandemic on HIV PrEP care: A Review and Synthesis of the Literature. AIDS Behav 27, 2089–2102 (2023). https://doi.org/10.1007/s10461-022-03941-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-022-03941-w