Abstract
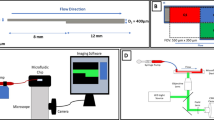
Microscopic steps and crevices are inevitable features within prosthetic blood-contacting devices. This study aimed to elucidate the thrombogenicity of the associated microscopic flow features by studying the transport of fluorescent platelet-sized particles in a suspension of red blood cells (RBCs) flowing through a 100 μm:200 μm sudden expansion. Micro-flow visualization revealed a strong influence of hematocrit upon the path of RBCs and spatial concentration of particles. At all flow rates studied (Re = 8.3–41.7) and hematocrit 20% and lower, RBC streamlines were found to detach from the microchannel wall creating an RBC-depleted zone inside the step that was much larger than the cells themselves. However, the observed distribution of particles was relatively homogeneous. By contrast, the RBC streamlines of samples with hematocrit equal to or greater than 30% more closely followed the contour of the microchannel, yet exhibited enhanced concentration of particles within the corner. The corresponding size of the cell depletion layer was comparable with the size of the cells. This study implies that local platelet concentration in blood within the physiological range of hematocrit can be elevated within the flow separation region of a sudden expansion and implicates the role of RBCs in causing this effect.













Similar content being viewed by others
References
Aarts P. A., P. A. Bolhuis, K. S. Sakariassen, R. M. Heethaar, J. J. Sixma. Red blood cell size is important for adherence of blood platelets to artery subendothelium. Blood 62: 214–217, 1983
Aarts P. A., R. M. Heethaar, J. J. Sixma. Red blood cell deformability influences platelets – vessel wall interaction in flowing blood. Blood 64: 1228–1233, 1984
Aarts P. A., S. A. van den Broek, G. W. Prins, G. D. Kuiken, J. J. Sixma, R. M. Heethaar. Blood platelets are concentrated near the wall and red blood cells, in the center in flowing blood. Arteriosclerosis 8: 819–824, 1988
Ahn T., E. Shin, Y. Merhi, P. Thai, L. Bilodeau. Influence of stent expansion states on platelet deposition in an extracorporeal porcine arteriovenous shunt model using a multichannel perfusion chamber. J. Korean Med. Sci. 16: 31–38, 2001
Alemu Y., D. Bluestein. Flow-induced platelet activation and damage accumulation in a mechanical heart valve: numerical studies. Artif. Organs 31: 677–688, 2007
Armaly B. F., F. Durst, J. C. F. Pereira, B. Schonung. Experimental and theoretical investigation of backward-facing step flow. J. Fluid Mech. 172: 473–496, 1983
Arslan S., F. Gundogdu, E. Bozkurt. Images in cardiology. Permanent pacemaker lead thrombosis leading to recurrent pulmonary embolism. Heart 92: 597, 2006
Bachmann C., G. Hugo, G. Rosenberg, S. Deutsch, A. Fontaine, J. M. Tarbell. Fluid dynamics of a pediatric ventricular assist device. Artif. Organs 24: 362–372, 2000
Burgreen G. W., J. F. Antaki, J. Wu, P. Le Blanc, K. C. Butler. A computational and experimental comparison of two outlet stators for the Nimbus LVAD. Left ventricular assist device. ASAIO J. 45: 328–333, 1999
Burgreen G. W., H. M. Loree II, K. Bourque, C. Dague, V. L. Poirier, D. Farrar, E. Hampton, Z. J. Wu, T. M. Gempp, R. Schob. Computational fluid dynamics analysis of a maglev centrifugal left ventricular assist device. Artif. Organs 28: 874–880, 2004
Crewe K. H., I. A. Feuerstein. Platelet adhesion to fibrinogen-coated glass at an abrupt tubular expansion viewed with fluorescent video-microscopy. Biorheology 23: 443–452, 1986
David T., S. Thomas, P. G. Walker. Platelet deposition in stagnation point flow: an analytical and computational simulation. Med. Eng. Phys. 23: 299–312, 2001
Denham M. K., M. A. Patrick. Laminar flow over a downstream-facing step in a two-dimensional flow channel. Trans. Inst. Chem. Eng. 52: 361–367, 1974
Dumont K., J. Vierendeels, R. Kaminsky, G. van Nooten, P. Verdonck, D. Bluestein. Comparison of the hemodynamic and thrombogenic performance of two bileaflet mechanical heart valves using a CFD/FSI model. J. Biomech. Eng. 129: 558–565, 2007
Eckstein E. C., F. Belgacem. Model of platelet transport in flowing blood with drift and diffusion terms. Biophys. J. 60: 53–69, 1991
Eckstein E. C., A. W. Tilles, F. J. Millero III. Conditions for the occurrence of large near-wall excesses of small particles during blood flow. Microvasc. Res. 36: 31–39, 1988
Fabijanic D., L. Giunio, M. Vujicic, I. Vukovic, R. Ermacora, N. Knezevic. Right atrial pacemaker lead thrombosis incidentally detected by transesophageal echocardiography. Coll. Antropol. 29: 159–161, 2005
Ge L., S. C. Jones, F. Sotiropoulos, T. M. Healy, A. P. Yoganathan. Numerical simulation of flow in mechanical heart valves: grid resolution and the assumption of flow symmetry. J. Biomech. Eng. 125: 709–718, 2003
Ge L., H. L. Leo, F. Sotiropoulos, A. P. Yoganathan. Flow in a mechanical bileaflet heart valve at laminar and near-peak systole flow rates: CFD simulations and experiments. J. Biomech. Eng. 127: 782–797, 2005
Goldsmith, H. L. The microrheology of human erythrocyte suspensions. In: Theoretical and Applied Mechanics Proceedings of the 13th IUTAM Congress. New York: Springer, 1972
Goldsmith H. L., V. T. Turitto. Rheological aspects of thrombosis and haemostasis: basic principles and applications. ICTH-Report – Subcommittee on Rheology of the International Committee on Thrombosis and Haemostasis. Thromb. Haemost. 55: 415–435, 1986
Goldstein D. J. Coagulation and thrombotic complications associated with ventricular assist devices. Clin. Adv. Hematol. Oncol. 3: 766–768, 2005
Goodman P. D., E. T. Barlow, P. M. Crapo, S. F. Mohammad, K. A. Solen. Computational model of device-induced thrombosis and thromboembolism. Ann. Biomed. Eng. 33: 780–797, 2005
Jordan A., T. David, S. Homer-Vanniasinkam, A. Graham, P. Walker. The effects of margination and red cell augmented platelet diffusivity on platelet adhesion in complex flow. Biorheology 41: 641–653, 2004
Karino T., H. L. Goldsmith. Flow behaviour of blood cells and rigid spheres in an annular vortex. Philos. Trans. R. Soc. Lond. B. Biol. Sci. 279: 413–445, 1977
Karino T., H. L. Goldsmith. Aggregation of human platelets in an annular vortex distal to a tubular expansion. Microvasc. Res. 17: 217–237, 1979
Karino T., H. L. Goldsmith. Adhesion of human platelets to collagen on the walls distal to a tubular expansion. Microvasc. Res. 17: 238–262, 1979
LaDisa J. F. Jr., I. Guler, L. E. Olson, D. A. Hettrick, J. R. Kersten, D. C. Warltier, P. S. Pagel. Three-dimensional computational fluid dynamics modeling of alterations in coronary wall shear stress produced by stent implantation. Ann. Biomed. Eng. 31: 972–980, 2003
LaDisa, J. F., Jr., L. E. Olson, I. Guler, D. A. Hettrick, S. H. Audi, J. R. Kersten, D. C. Warltier, and P. S. Pagel. Stent design properties and deployment ratio influence indexes of wall shear stress: a three-dimensional computational fluid dynamics investigation within a normal artery. J. Appl. Physiol. 97:424–430; discussion 416, 2004
Lassila R., J. J. Badimon, S. Vallabhajosula, L. Badimon. Dynamic monitoring of platelet deposition on severely damaged vessel wall in flowing blood. Effects of different stenoses on thrombus growth. Arteriosclerosis 10: 306–315, 1990
Leonard E. Principles of cardiovascular design. Cardiovasc. Pathol. 2: 3s–10s, 1993
Moraczewski T., H. Tang, N. C. Shapley. Flow of a concentrated suspension through an abrupt axisymmetric expansion measured by nuclear magnetic resonance imaging. J. Rheol. 49: 1409–1428, 2005
Rosamond W., K. Flegal, G. Friday, K. Furie, A. Go, K. Greenlund, N. Haase, M. Ho, V. Howard, B. Kissela, S. Kittner, D. Lloyd-Jones, M. McDermott, J. Meigs, C. Moy, G. Nichol, C. J. O'Donnell, V. Roger, J. Rumsfeld, P. Sorlie, J. Steinberger, T. Thom, S. Wasserthiel-Smoller, Y. Hong. Heart disease and stroke statistics – 2007 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 115: e69–171, 2007
Sato M., N. Ohshima. Hemodynamics at stenoses formed by growing platelet thrombi in mesenteric microvasculature of rat. Microvasc. Res. 31: 66–76, 1986
Sorensen E. N., G. W. Burgreen, W. R. Wagner, J. F. Antaki. Computational simulation of platelet deposition and activation: I. Model development and properties. Ann. Biomed. Eng. 27: 436–448, 1999
Sorensen, E. N., G. W. Burgreen, W. R. Wagner, and J. F. Antaki. Simulation of platelet deposition in disturbed flow. In: Second Joint EMBS-BMES Conference, Houston, TX, 2002
Wootton D. M., C. P. Markou, S. R. Hanson, D. N. Ku. A mechanistic model of acute platelet accumulation in thrombogenic stenoses. Ann. Biomed. Eng. 29: 321–329, 2001
Xu C., D. M. Wootton. Platelet near-wall excess in porcine whole blood in artery-sized tubes under steady and pulsatile flow conditions. Biorheology 41: 113–125, 2004
Yamanaka H., G. Rosenberg, W. J. Weiss, A. J. Snyder, C. M. Zapanta, C. A. Siedlecki. Multiscale analysis of surface thrombosis in vivo in a left ventricular assist system. ASAIO J. 51: 567–577, 2005
Yamanaka H., G. Rosenberg, W. J. Weiss, A. J. Snyder, C. M. Zapanta, C. A. Siedlecki. Short-term in vivo studies of surface thrombosis in a left ventricular assist system. ASAIO J. 52: 257–265, 2006
Yin W., Y. Alemu, K. Affeld, J. Jesty, D. Bluestein. Flow-induced platelet activation in bileaflet and monoleaflet mechanical heart valves. Ann. Biomed. Eng. 32: 1058–1066, 2004
Zhao R., M. V. Kameneva, J. F. Antaki. Investigation of platelet margination phenomena at elevated shear stress. Biorheology 44: 161–177, 2007
Acknowledgments
The authors gratefully acknowledge Dr. Sachin Velankar for his help in design of the microchannel. This study was supported in part by grants from the Department of Defense, US Army through Pittsburgh Tissue Engineering Initiative.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, R., Marhefka, J., Shu, F. et al. Micro-Flow Visualization of Red Blood Cell-Enhanced Platelet Concentration at Sudden Expansion. Ann Biomed Eng 36, 1130–1141 (2008). https://doi.org/10.1007/s10439-008-9494-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-008-9494-z