Abstract
Aim
To investigate the social contact patterns of Chinese residents in the post COVID-19 pandemic period, explore the associations between the different contact patterns and incidence of influenza.
Subject and methods
A cross-sectional social contact survey was conducted on Chinese residents from December 9, 2021, to January 20, 2022. The contact was divided into participant–acquaintance (P–A) and participant–stranger (P–S), and the generalized linear model (GLM) was used to explore their impact on the incidence of influenza.
Results
The contact frequency of P–S was higher than that of P–A (3.41 V.S. 1.94), but the average contact duration of P–S was much shorter than that of P–A (0.20 h V.S. 5.53 h). P–A contact mainly occurred among peers as well as family members. However, P–S contact was concentrated in the middle-aged population. In GLM, the influence of P–S on the incidence of influenza was higher (OR = 2.63, 95% CI 2.29–3.02) than that of P–A (OR = 1.82, 95% CI 1.56–2.13), especially on the weekend (P–S OR = 4.31, 95% CI 2.31–8.01) and in recreation places (P–S OR = 4.94, 95% CI 2.26–10.78).
Conclusions
Social contact will increase the incidence rate of influenza. Therefore, when contacting with strangers, especially in recreation places, personal protective behavior should be strengthened.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The novel coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has caused over 670 million cases and over 6.8 million deaths worldwide since December 2019 (Johns Hopkins University 2020). To reduce the health threat of COVID-19 to the public, a series of non-pharmaceutical interventions (NPIs) have been implemented worldwide, including strict physical distancing measures, large-scale mobility restrictions, wearing masks in public places, etc. (World Health Organization 2020a). These measures have greatly changed the contact patterns of the population. For example, after the NPIs was implemented, the daily contact between the populations in Wuhan and Shanghai had decreased by 7–8 times, with most of the contacts occurring in households (Zhang et al. 2020). In the UK, a study also found that the average daily number of contacts of each participant decreased by 74.0% during the COVID-19 pandemic (Jarvis et al. 2020). Since the contact patterns of the population are the basis of the dynamic transmission of infectious diseases, such as influenza (Ibuka et al. 2016; Kucharski et al. 2014; Kwok et al. 2014; Eames et al. 2012), SARS-CoV-2 (Jarvis et al. 2020), respiratory syncytial virus (Yamin et al. 2016) and varicella (Ogunjimi et al. 2009), the change of the contact patterns of the population and the reduction of the the number of daily contacts not only reduced the basic reproduction number of SARS-CoV-2 by 76.2% (Jarvis et al. 2020) but also led to a sharp reduction of the seasonal influenza activities during the COVID-19 pandemic (Youssef et al. 2022; Soo et al. 2020; Kuo et al. 2020; Lei et al. 2020).
Several studies have investigated the contact patterns of the population during the early stage of the COVID-19 pandemic (Zhang et al. 2020; Jarvis et al. 2020). However, with the gradual control of the pandemic and the relaxation of the top-down (i.e., governmental measures) restrictions, people have had “pandemic fatigue,” referring to the demotivation to follow recommended protective behaviors, emerging gradually over time and affected by emotions, experiences and perceptions (World Health Organization 2020b), which have happened in many countries (Ilesanmi et al. 2020; Majumdar et al. 2020; Labrague and Ballad. 2021). Therefore, activities related to infectious diseases such as influenza have rebounded in China in 2022 (China National Influenza Center 2023), indicating that the contact patterns of the population may change again. However, few studies have investigated the contact patterns of the population in the post COVID-19 pandemic period, and currently, there is no research separately exploring the contact patterns of the population with acquaintances and strangers. Therefore, the objective of our study was to explore the contact patterns of the participants with acquaintances and strangers in the post COVID-19 pandemic period, and their impact on the incidence rate of influenza. Thus, the government can lay particular emphasis on implementing various intervention measures in different places when preventing and controlling infectious diseases, so as to achieve the goal of infectious disease prevention and control more efficiently.
Materials and methods
Study design
From December 9, 2021, to January 20, 2022, a cross-sectional online survey was conducted in all age groups in three regions of mainland China (northern, central and southern), including Beijing (northern China), Hangzhou (central China), Chengdu (central China), and Guangzhou (southern China). We aimed to investigate the social contact patterns with acquaintances and strangers related to the incidence rate of influenza, which consisted of seven parts: demographic, family structure, influenza vaccination behavior, mask-wearing habits, influenza-like symptoms, daily contact, and scope of daily activities. The design of the survey questionnaire on daily contact mainly referred to Mossong et al. (2008). We defined acquaintances as individuals known by participants, including spouse, family members, friends, neighbour, colleagues, etc., and defined strangers as people who do not know basic information such as name, age, etc. (Karriker-Jaffe et al. 2017). In this study, the incidence rate of influenza-like illness (ILI) represented the incidence rate of influenza. Definition of ILI: fever with a body temperature of 38.0 ºC or above, accompanied by respiratory symptoms such as sneeze, sore throat, nasal congestion, chills, fatigue, headache, etc. Detailed information of the online survey can be found in Supplementary Materials Text S1.
Information collection
Our survey was conducted by the ePanel (2021) data company, which maintains a national online survey panel with individual’ phone numbers, email addresses, and basic information (Hou et al. 2021). This survey panel included millions of residents from Beijing, Hangzhou, Chengdu, and Guangzhou, who were randomly chosen from the survey panel. After agreeing to participate in the survey and providing informed consent, the questionnaire would be completed. Children aged 0–14 and individuals aged 60 and above who have difficulty completing the survey independently were helped by other family members to fill out the questionnaire. Based on local census data of each city, the proportional quota sampling (Sedgwick 2021) was used to ensure that respondents were demographically representative of the population. In other words, the proportions of participants’ age groups and genders were aligned with those of the four cities. Finally, approximately 1000 samples were collected from each city. The study was approved by the Clinical Research Ethics Committee of the First Affiliated Hospital of Zhejiang University School of Medicine (2021-IIT rapidly review-285).
Between December 9, 2021, to January 20, 2022, the survey was emailed to 51,570 residents in four cities. Finally, 4322 residents completed the survey, of whom 25 residents either did not finish or had missing data in their responses, leaving data from 4297 respondents in the final analytic sample, including 1083 from Beijing (25.2%) and 1074 from Hangzhou (24.99%), 1063 from Chengdu (24.74%), and 1077 from Guangzhou (25.06%).
Statistic analysis
The participants in this study were divided into the following 14 age groups: 0–4, 5–9, 10–14, 15–19, 20–24, 25–29, 30–34, 35–39, 40–44, 45–49, 50–54, 55–59, 60–64, and 65+. We calculated the average number of social contacts per person per day with total contact objects, acquaintances and strangers, respectively, and stratified them by gender, whether they are floating population, day of the week, location of contact, and type of contact. The social contact matrices for the age-specific social contacts, adjusting for the age distribution in the study population were calculated, using the “socialmixr” package in R (Jarvis et al. 2020).
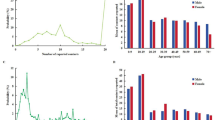
The participants did not record the exact age of each stranger contact, so we modeled the distribution of acquaintance contact age groups using Gaussian kernel function (Zhang et al. 2019), stratified by different age groups of participants (Supplementary Fig. S1). Then we randomly selected the possible age groups of the stranger contacts from the model referring to the age groups of participants and repeated this process 200 times to reduce uncertainty. The model was established through “e1071” package in R.
Since the basic reproduction number (R0) was proportional to the dominant eigenvalues [normalization (Q)] of the contact matrices (Wallinga et al. 2006; Diekmann et al. 2010), Wilcoxon rank sum was used to test the difference in Q of stranger contacts and acquaintance contacts, to test whether contact with strangers or acquaintances will significantly affect the transmission of infectious diseases.
In this study, the presence of influenza in the survey were represented by binary variables. If the participant had ILI in the past year, its value was 1, otherwise it was 0. The generalized linear binomial model was used to explore the relationship between the incidence rate of influenza and age, gender, income, household size, influenza vaccines, and contacts (with acquaintances and strangers) (Ibuka et al. 2016). In addition, the data was further divided according to gender, whether they are floating population, day of the week, location of contact, and performed model fitting separately.
All statistical analyses were carried out in R 4.0.5.
Results
Demographics characteristics and contact pattern of participants
Overall, 4297 participants were included in this study, Supplementary Table S1 presented detailed demographic characteristics of the participants. We recorded a total of 23,090 contacts from 2155 male respondents and 2142 female respondents, including 7519 (32.6%) acquaintance contacts and 15,571 (67.4%) stranger contacts. Young and middle-aged participants reported higher number of daily contacts and higher proportion of stranger contacts, with participants aged 30–34 years reporting the highest number of contacts, those aged 20–24 years reporting the highest proportion of stranger contacts and aged 0–4 years reporting the lowest proportion of stranger contacts (Fig. 1a, b). Similarly, young and middle-aged participants reported longer total contact duration and participants of all ages had a low proportion of total contact duration with strangers, with participants aged 30–34 years reporting the longest total contact duration and those aged 20–24 years reporting the highest proportion of total contact duration with strangers, but the highest proportion of total contact duration with strangers was still less than 20% (Fig. 1c, d). Participants generally had contact with acquaintances at home, teenagers also often had contact with acquaintances at classroom, young, and middle-aged people had a higher proportion of contact with acquaintances in the workplace, and the proportion of elderly people having contact with acquaintances in recreation places and other places (parks, food markets, etc.) obviously increased (Fig. 1e, f). The contact between children and strangers mainly occurred in mass transit, while the contact between teenagers and strangers mainly occurred in the classroom, the contact between middle-aged and young people and strangers mainly happened in the workplace, and as age increased, the proportion of contact with strangers in supermarkets increased (Fig. 1g, h). In the past year, the daily activities of participants per week were mainly cross villages or cross towns, with few cross provincial or cross national activities, the longest weekly activity was across counties (Fig. 1i, j).
Participant contact matrix
For the Participant–Total (P–T) contact, the matrix presented typical features of age-mixing patterns. This matrix had three distinct diagonals, with the middle diagonal representing contacts between the same age group, with female being more pronounced than male. The other two diagonals indicated contact between family members. The middle part of the matrix represented more contact between young and middle-aged people, with male being more pronounced than female (Fig. 2a). In addition, men had more mean daily contact than women (5.80 V.S. 4.89), mainly because they had more contact with strangers (3.86 V.S. 2.96) (Table 1). For the participant–acquaintance (P–A) contact, regardless of gender, the matrix exhibited a three diagonals phenomenon, that was, the contact mainly occurred among peers and between family members. (Fig. 2b). For participant–stranger (P–S) contact, the matrix had a clear central clustering characteristic, especially for male, indicating more contact happened between young and middle-aged people (Fig. 2c). The difference matrix also showed that participants’ contact with strangers is mainly concentrated in young and middle-aged people, especially for men (Fig. 2d). The contact matrix of contact duration had similar features to P–T, P–A, and P–S (Fig. 2e, f, g) and the average contact duration of P–A was much longer than that of P–S (5.53 h V.S. 0.20 h).
Contact matrix between participants and different contacts: (a) total population; (b) acquaintance; (c) stranger; (d) differences in the contact matrix between acquaintance and stranger. Contact duration matrix between participants and different contacts: (e) total population; (f) acquaintance; (g) stranger
For P–T and P–A contact, weekday contact had more obvious contact characteristics among peers and between family members than weekend contact. For P–A contact, there was a very obvious feature of contacts among young children on weekends (Fig. 3a, b). For P–S contact, the weekday contact displayed a more obvious characteristic of contact between middle-aged and young people than weekend contact. On weekends, mainly participants aged 30–34 years were in contact with strangers (Fig. 3c). The difference matrix also showed more central clustering on weekdays than on weekends (Fig. 3d). In addition, weekdays had more mean number of contacts than weekend (5.47 V.S. 4.11), mainly with stranger (3.50 V.S. 2.25) (Table 1). For the P–T and P–A contact, the resident population presented more obvious contact characteristics among peers and between family members than that of floating population (Fig. 3e, f). For the P–S contact, the resident population exhibited a more obvious phenomenon of contact between middle-aged and young people than that of the floating population (Fig. 3g). The difference matrix also showed more central clustering in the resident population than the floating population (Fig. 3h). Moreover, the resident population had more mean number of contacts than the floating population (5.59 V.S. 3.73) (Table 1). Finally, the non-physical contact reported by participants generally exceeded physical contact, whether in P–A or P–S contact (Fig. 3i, j, k) (Table 1). The difference matrix of physical contact was mainly concentrated in middle-aged people and the elderly (Fig. 3l).
For P–T contact, contacts mainly occurred in workplaces, classrooms, mass transits and restaurants (Fig. 4a, Table 1). For P–A contact, there was obvious characteristic of family member contact in home. In the workplace, contacts mainly occurred between colleagues, and in the classroom, contacts mainly happened between classmates. Except for irregular contact pattern in hospitals, there was a clear feature of same-age contact in mass transits, recreation places, restaurants, and other places (Fig. 4b). For P–S contact, stranger contact commonly occurred in workplaces, classrooms, mass transits, restaurants, and supermarkets and mostly concentrated in the middle-aged groups (Fig. 4c, Table 1). For the difference matrix, in recreation places, there was an obvious same-age contact characteristic, while in workplaces, mass transits and restaurants, the differences were mainly concentrated among young and middle-aged people (Fig. 4d). Finally, the Wilcoxon rank sum test showed a statistically significant difference in Q of P–A and P–S contact (Table 1).
The influencing factor of the incidence rate of influenza
In general, female (Odds rate (OR) = 0.67, 95% confidence interval (CI) 0.58–0.77), those with higher monthly income (OR = 0.82, 95% CI 0.77–0.88), and those who received influenza vaccines (OR = 0.65, 95% CI 0.57–0.74) had lower incidence rate of influenza, while social contact was the risk factor of the incidence rate of influenza, and the OR of stranger contact (OR = 2.63, 95% CI 2.29–3.02) was greater than that of acquaintance contact (OR = 1.82, 95% CI 1.56–2.13). In addition, monthly income level and influenza vaccination had impacts on the incidence rate of influenza in men, but not in women. Social contact, whether they are strangers or acquaintances, had a higher impact on the incidence rate of influenza in women than in men (Stranger 2.76 V.S. 2.46, Acquaintance 1.98 V.S. 1.70). On weekdays, women (OR = 0.65, 95% CI 0.57–0.75), high-income people (OR = 0.87, 95% CI 0.81–0.93), people with more co-habitations (OR = 0.89, 95% CI 0.84–0.94), and people who have received influenza vaccines (OR = 0.63, 95% CI 0.55–0.72) had a lower incidence rate of influenza. Social contact, especially with strangers (OR = 2.56, 95% CI 2.22–2.95), would increase the incidence rate of influenza on weekdays, which was more significant on weekends (OR = 4.31, 95% CI 2.31–8.01). In the floating population, higher monthly income level (OR = 0.48, 95% CI 0.35–0.65) would reduce the incidence rate of influenza. In the resident population, female (OR = 0.63, 95% CI 0.54–0.72), high monthly income (OR = 0.86, 95% CI 0.80–0.92), large family size (OR = 0.90, 95% CI 0.85–0.95), and influenza vaccination (OR = 0.63, 95% CI 0.54–0.72) could achieve the same goal, while social contact was the opposite (Stranger OR = 2.66, 95% CI 2.30–3.07, Acquaintance OR = 1.95, 95% CI 1.65–2.30). Similar phenomena could be found in different contact places. In general, social contact in workplaces (Stranger OR = 3.70, 95% CI 2.62–5.22, Acquaintance OR = 4.58, 95% CI 2.49–8.44), classrooms (Stranger OR = 3.61, 95% CI 2.30–5.66), recreation places (Stranger OR = 4.94, 95% CI 2.26–10.78), and home (Stranger OR = 2.54, 95% CI 2.09–3.07) would increase the incidence rate of influenza, while influenza vaccination could reduce the incidence rate of influenza in workplaces (OR = 0.27, 95% CI 0.21–0.35) and mass transit (OR = 0.41, 95% CI 0.27–0.63) (Fig. 5).
Discussion
This study presented the contact patterns of Chinese residents between December 9, 2021, and January 20, 2022: each participant had a mean number of daily contacts of 5.35 people, including 1.94 acquaintances and 3.41 strangers. The average contact duration with acquaintances was 5.53 h and the average contact duration with strangers was 0.20 h. Compared to the beginning of the COVID-19 pandemic, the mean number of daily contacts was increased, but it was still significantly lower than that before the COVID-19 pandemic (Zhang et al. 2019, 2020; Jarvis et al. 2020; Ibuka et al. 2016; Fu et al. 2012; Read et al. 2014), indicating that residents’ health behaviors have relaxed compared to the early stage of the pandemic, but it is still significantly better than that before the pandemic. Our study was the first to explore the contact patterns between P–S, and the results showed that the mean number of daily contacts of P–S is higher than of P–A, but the average contact duration of P–S is much lower than the that of P–A. Since R0 was proportional to the Q of the contact matrices and the Wilcoxon rank sum test showed that the Q of P–S is significantly higher than that of P–A, it is indicated that contact with strangers is a more important factor in influenza transmission than contact with acquaintances.
In this study, the P–A contact matrix displayed a typical age-mixing contact pattern feature, with a long diagonal indicating contacts between the same age group, and two short diagonals indicating contacts between family members, which was consistent with the results of other studies (Zhang et al. 2019, 2020; Jarvis et al. 2020; Ibuka et al. 2016; Fu et al. 2012; Read et al. 2014). However, the P–S contact matrix exhibited a completely different contact pattern: contact was mainly concentrated between middle-aged people, especially between the 30–34 years old age group. This might be because middle-aged people contact with more strangers during work and their range of activity might also be larger than those of other age groups due to work needs. In addition, the P–A and P–S contact of different sub-groups also showed very interesting results: compared to weekdays, the weekend P–A contact matrix presented more significant contact features in the younger children, and the contact between parents and younger children obviously increased; and on weekends, P–S contact significantly decreased. This is consistent with the reality of more parent–child communication and less communication with strangers on weekends. The discovery of differences in mean number of contacts and contact patterns between weekdays and weekends was consistent with research in Japan and Europe (Ibuka et al. 2016; Mossong et al. 2008), which suggested that the effectiveness of control measures for infectious disease may vary between weekdays and weekends. Compared to the resident population, the mean number of contacts of the floating population was lower (3.73 V.S. 5.59), which may be the low number of participants (469/4297). However, the floating population had a higher Q value (1.60 V.S. 1.41), especially when in contact with strangers (2.24 V.S. 1.72), which might be due to the fact that the majority of the floating population are migrant workers with lower education levels and lower personal health protection awareness. The characteristics of the P–A contact in different contact places also showed significant changes: in the family, contact mainly occurred between parents and children; in the workplace, it mainly happened between middle-aged colleagues; in the classroom, it mainly occurred between classmates of the same age; and in dining and entertainment places, it mainly happened between friends of similar ages, which was consistent with other studies and the reality (Ajelli and Litvinova 2017). While P–S contact mainly occurred in densely populated places such as workplaces, classrooms, mass transit, supermarkets, restaurants, etc., with the highest Q value in restaurants, indicating that personal hygiene protection should be strengthened when having meals in restaurants.
The results of the generalized linear model showed that generally, being female, higher monthly income and having influenza vaccines are protective factors for the incidence rate of influenza, which was similar to the results of other studies (Ibuka et al. 2016), probably because those people have a higher awareness of personal health protection and their living environment might be different (Mousa et al. 2021). Additionally, social contact was a risk factor for the incidence rate of influenza, and stranger contact was more dangerous than acquaintance contact. This may be the mean number of daily contacts of P–S is higher than that of P–A, and the living environment of strangers may be more diverse and complex, which is more likely to cause the transmission of influenza. Moreover, we found that the larger the household size, the lower the incidence rate of influenza in the weekday, which was contrary to other research results (Ibuka et al. 2016). It may be due to people’s awareness of health behavior has generally improved during the COVID-19 pandemic, and people who has larger household size will pay more attention to their personal health protection. Moreover, stranger contact in recreation places and on weekends are very significant risk factors for the increases of incidence rate of influenza, possibly due to the high density of population in such situations, and people are generally in a very relaxed state, and personal protective behavior is not sufficient. Therefore, when preventing and controlling infectious diseases, it is important to pay more attention to personal protective behavior on weekends and in recreation places, and reduce stranger contact.
There are several limitations to this study. First, the data collection of this study was the self-completed contact diaries of the participants, which may have recall bias and result in incorrect estimates of the mean number of daily contacts and the average contact duration (Zhang et al. 2019; Mousa et al. 2021). In the future, we will consider using the form of interviewer-completed contact diaries to reduce the recall bias (Hoang et al. 2019) when conducting similar surveys. Second, we allowed each respondent to record the contact with strangers in a one row table on the questionnaire, including the number of strangers, approximate age range, whether it was physical contact, contact location, contact duration, etc. However, due to insufficient detail, statistical models were used to estimate the age of each stranger, which might deviate from the reality. We will strive to improve the questionnaire to more truthfully investigate the contact patterns between participants and strangers. Finally, the questionnaire limited the report of acquaintance contacts to 20 people, which might lead to some omissions of acquaintance contacts.
Conclusions
Our research provides patterns of the daily contacts of Chinese residents in the post COVID-19 pandemic period. The different contact patterns of participants with acquaintances and strangers: P–A had a typical age-mixing contact pattern feature, with contact mainly occurring among peers as well as between middle-aged people and children, while P–S contact was mainly concentrated in middle-aged people, with more mean number of daily contacts but much shorter average contact duration. In addition, social contact, especially with strangers, is an important risk factor for the increase of incidence rate of influenza. Therefore, when in contact with strangers, especially in recreation places, personal protective behavior should be strengthened.
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due to the fact that neither the document approved by the Clinical Research Ethics Committee of the First Affiliated Hospital of Zhejiang University School of Medicine (2021-IIT rapidly review-285) nor the author’s institution has granted researchers the authority to publish the data and the data contained potentially identifying or sensitive patient information. However, the data are available from the corresponding author on reasonable request.
Code availability
The code for the current study are not publicly available but are available from the corresponding author on reasonable request.
References
Ajelli M, Litvinova M (2017) Estimating contact patterns relevant to the spread of infectious diseases in Russia. J Theor Biol 419:1–7. https://doi.org/10.1016/j.jtbi.2017.01.041
China National Influenza Center (2023) Influenza Weekly Report in China National Influenza Center. https://ivdc.chinacdc.cn/cnic/zyzx/lgzb/202303/t20230330_264734.htm. Access on 5 July 2023
Diekmann O, Heesterbeek JA, Roberts MG (2010) The construction of next-generation matrices for compartmental epidemic models. J R Soc Interface 7(47):873–885. https://doi.org/10.1098/rsif.2009.0386
Eames KT, Tilston NL, Brooks-Pollock E, Edmunds WJ (2012) Measured dynamic social contact patterns explain the spread of H1N1v influenza. PLoS Comput Biol 8(3):e1002425. https://doi.org/10.1371/journal.pcbi.1002425
ePanel (2021) URL: https://www.epanel.cn/. Accessed 6 May 2021
Fu YC, Wang DW, Chuang JH (2012) Representative contact diaries for modeling the spread of infectious diseases in Taiwan. PLoS ONE 7(10):e45113. https://doi.org/10.1371/journal.pone.0045113
Hoang T, Coletti P, Melegaro A, Wallinga J, Grijalva CG, Edmunds JW et al (2019) A systematic review of social contact surveys to inform transmission models of close-contact infections. Epidemiology 30(5):723–736. https://doi.org/10.1097/EDE.0000000000001047
Hou Z, Song S, Du F, Shi L, Zhang D, Lin L et al (2021) The influence of the COVID-19 epidemic on prevention and vaccination behaviors among Chinese children and adolescents: cross-sectional online survey study. JMIR Public Health Surveill 7(5):e26372. https://doi.org/10.2196/26372
Ibuka Y, Ohkusa Y, Sugawara T, Chapman GB, Yamin D, Atkins KE et al (2016) Social contacts, vaccination decisions and influenza in Japan. J Epidemiol Community Health 70(2):162–167. https://doi.org/10.1136/jech-2015-205777
Ilesanmi OS, Bello AE, Afolabi AA (2020) COVID-19 pandemic response fatigue in Africa: causes, consequences, and counter-measures. Pan Afr Med J 37(Suppl 1):37. https://doi.org/10.11604/pamj.supp.2020.37.37.26742
Jarvis CI, Van Zandvoort K, Gimma A, Prem K; CMMID COVID-19 working group; Klepac P et al (2020) Quantifying the impact of physical distance measures on the transmission of COVID-19 in the UK. BMC Med 18(1):124. https://doi.org/10.1186/s12916-020-01597-8
Johns Hopkins University (2020) COVID-19 Dashboard. https://coronavirus.jhu.edu/map.html. Accessed 6 July 2023
Karriker-Jaffe KJ, Greenfield TK, Kaplan LM (2017) Distress and alcohol-related harms from intimates, friends, and strangers. J Subst Use 22(4):434–441. https://doi.org/10.1080/14659891.2016.1232761
Kucharski AJ, Kwok KO, Wei VW, Cowling BJ, Read JM, Lessler J et al (2014) The contribution of social behaviour to the transmission of influenza A in a human population. PLoS Pathog 10(6):e1004206. https://doi.org/10.1371/journal.ppat.1004206
Kuo SC, Shih SM, Chien LH, Hsiung CA (2020) Collateral benefit of COVID-19 control measures on influenza activity. Taiwan Emerg Infect Dis 26(8):1928–1930. https://doi.org/10.3201/eid2608.201192
Kwok KO, Cowling BJ, Wei VW, Wu KM, Read JM, Lessler J et al (2014) Social contacts and the locations in which they occur as risk factors for influenza infection. Proc Biol Sci 281(1789):20140709. https://doi.org/10.1098/rspb.2014.0709
Labrague LJ, Ballad CA (2021) Lockdown fatigue among college students during the COVID-19 pandemic: predictive role of personal resilience, coping behaviors, and health. Perspect Psychiatr Care 57(4):1905–1912. https://doi.org/10.1111/ppc.12765
Lei H, Xu M, Wang X, Xie Y, Du X, Chen T et al (2020) Nonpharmaceutical interventions used to control COVID-19 reduced seasonal influenza transmission in China. J Infect Dis 222(11):1780–1783. https://doi.org/10.1093/infdis/jiaa570
Majumdar P, Biswas A, Sahu S (2020) COVID-19 pandemic and lockdown: cause of sleep disruption, depression, somatic pain, and increased screen exposure of office workers and students of India. Chronobiol Int 37(8):1191–1200. https://doi.org/10.1080/07420528.2020.1786107
Mossong J, Hens N, Jit M, Beutels P, Auranen K, Mikolajczyk R et al (2008) Social contacts and mixing patterns relevant to the spread of infectious diseases. PLoS Med 5(3):e74. https://doi.org/10.1371/journal.pmed.0050074
Mousa A, Winskill P, Watson OJ, Ratmann O, Monod M, Ajelli M et al (2021) Social contact patterns and implications for infectious disease transmission - a systematic review and meta-analysis of contact surveys. Elife 10:e70294. https://doi.org/10.7554/eLife.70294
Ogunjimi B, Hens N, Goeyvaerts N, Aerts M, Van Damme P, Beutels P (2009) Using empirical social contact data to model person to person infectious disease transmission: an illustration for varicella. Math Biosci 218(2):80–87. https://doi.org/10.1016/j.mbs.2008.12.009
Read JM, Lessler J, Riley S, Wang S, Tan LJ, Kwok KO et al (2014) Social mixing patterns in rural and urban areas of southern China. Proc Biol Sci 281(1785):20140268. https://doi.org/10.1098/rspb.2014.0268
Sedgwick P (2021) Proportional quota sampling. BMJ 345(sep26 3):e6336-e6336. https://doi.org/10.1136/bmj.e6336
Soo RJJ, Chiew CJ, Ma S, Pung R, Lee V (2020) Decreased influenza incidence under COVID-19 control measures. Singapore Emerg Infect Dis 26(8):1933–1935. https://doi.org/10.3201/eid2608.201229
Wallinga J, Teunis P, Kretzschmar M (2006) Using data on social contacts to estimate age-specific transmission parameters for respiratory-spread infectious agents. Am J Epidemiol 164(10):936–944. https://doi.org/10.1093/aje/kwj317
World Health Organization (2020a) Report of the WHO-China joint mission on coronavirus disease 2019 (COVID-19). https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf. Accessed 6 July 2023
World Health Organization (2020b) Pandemic Fatigue: Reinvigorating the Public to Prevent COVID-19. https://apps.who.int/iris/bitstream/handle/10665/335820/WHO-EURO-2020-1160-40906-55390-eng.pdf. Accessed 7 July 2023
Yamin D, Jones FK, DeVincenzo JP, Gertler S, Kobiler O, Townsend JP et al (2016) Vaccination strategies against respiratory syncytial virus. Proc Natl Acad Sci U S A 113(46):13239–13244. https://doi.org/10.1073/pnas.1522597113
Youssef D, Issa O, Kanso M, Youssef J, Abou-Abbas L, Abboud E (2022) Practice of non-pharmaceutical interventions against COVID-19 and reduction of the risk of influenza-like illness: a cross-sectional population-based study. J Pharm Policy Pract 15(1):54. https://doi.org/10.1186/s40545-022-00450-y
Zhang J, Klepac P, Read JM, Rosello A, Wang X, Lai S et al (2019) Patterns of human social contact and contact with animals in Shanghai. China Sci Rep 9(1):15141. https://doi.org/10.1038/s41598-019-51609-8
Zhang J, Litvinova M, Liang Y, Wang Y, Wang W, Zhao S et al (2020) Changes in contact patterns shape the dynamics of the COVID-19 outbreak in China. Science 368(6498):1481–1486. https://doi.org/10.1126/science.abb8001
Acknowledgements
We are grateful to the staff and participants who helped with the investigation.
Funding
This study was supported by grants from the National Natural Science Foundation of China (Grant Numbers: U23A20496, 82173577, 81672005, U1611264, 81001271, and 81721091); the Mega-Project of National Science and Technology for the 12th and 13th Five-Year Plan of China (Grant Numbers: 2018ZX10715-014-002 and 2014ZX10004008).
Author information
Authors and Affiliations
Contributions
SY designed and supervised this study. CC, YD, KC, RY, DJ, XZ,XW, MC, YY, WZ, DC, JQ collected and cleaned the data. SY, MY, and CC analyzed and interpreted the data. SY, MY, and CC wrote the manuscript. SY revised the manuscript from preliminary draft to submission. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (the Clinical Research Ethics Committee of the First Affiliated Hospital of Zhejiang University School of Medicine, reference number: 2021-IIT rapidly review-285).
Consent to participate
Informed consent was obtained from all participants (from a parent/guardian if participant was below 18 years old).
Consent for publication
Not applicable.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yang, M., Chen, C., Zhang, X. et al. Social contact patterns with acquaintances and strangers related to influenza in the post-pandemic era. J Public Health (Berl.) (2024). https://doi.org/10.1007/s10389-024-02213-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10389-024-02213-2