Abstract
Aim
This study aimed to ascertain the impact of high intensity interval training (HIIT) on physical, mental, and overall quality of life (QoL) through a comprehensive systematic review and meta-analysis.
Subject and methods
A systematic search for relevant trials was performed via PubMed, the Cochrane Library and Web of science as well as the manual screening of prior meta-analyses and their respective reference lists (PROSPERO reference: CRD42022326576). Adult controlled trials investigating the effects of a >2-week HIIT intervention with an eligible non-intervention control group were considered. As the primary outcome, studies were required to include at least one measure of physical and/or mental and/or overall QoL, on any validated QoL domain, pre and post intervention.
Results
Twenty-two studies with twenty-four effect sizes were included; seventeen comparing HIIT and overall QoL, fourteen comparing HIIT and physical QoL and thirteen studies comparing HIIT and mental QoL. There was a statistically significant improvement in physical (SMD= 0.405, 95% CI: 0.110- 0.700, p= 0.007), mental (SMD= 0.473, 95% CI: 0.043 –0.902, p=0.031) and overall QoL (SMD= 0.554, 95% CI 0.210-0.898, p=0.002) following a program of HIIT. Secondary analysis of 5 studies comparing HIIT against moderate intensity continuous training demonstrated no significant difference in improvement between the two modes (SMD= -0.094, CI= -0.506-0.318, p=0.655).
Conclusion
Engaging in HIIT produces statistically significant improvements in physical, mental, and overall quality of life in clinical and non-clinical populations at a small to moderate effect size. Furthermore, HIIT appears as effective as MICT in improving overall QoL, offering a more time-efficient exercise option.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
High intensity interval training (HIIT), defined as exercise containing short intervals of vigorous physical activity (PA) with alternate periods of passive or active rest (Gibala et al. 2012), is a well-established training mode in healthy individuals, with a more recent expansion into clinical populations (Cassidy et al. 2017). Previous work has evidenced the effectiveness of HIIT in improving numerous health parameters (Ito 2019), including blood pressure regulation (Edwards et al. 2021, 2022), body composition (Wewege et al. 2017), and other important risk factors of cardiovascular disease (Batacan et al. 2017a). Furthermore, HIIT provides greater improvements in VO2 peak in a 6–8-week intervention when compared to a moderate intensity continuous training (MICT) intervention of the same length (Ito 2019). Importantly, although not to statistical significance, the recent ‘Generation 100’ study demonstrated a 37% and 49% lower all-cause mortality risk following HIIT compared to both the current physical activity guidelines and MICT programmes; respectively (Stensvold et al. 2020).
Currently 1 in 4 adults do not meet the current international PA guidelines (Bull et al. 2020), with lack of time being one of the most frequently reported barriers to exercise (Withall et al. 2011). Indeed, HIIT is a short, time-efficient mode of exercise, increasing its accessibility and potential for increased adherence across clinical and non-clinical populations (Vella et al. 2017). Previous HIIT research has largely focused on physiological adaptations, with primary and secondary disease prevention remaining the predominant interest (Ito 2019). However, as a measure concerned with a person’s perception of self-well-being, the ‘ultimate’ goal of patient care for health practitioners is to improve and maintain Quality of Life (QoL) (Jacobs 2009).
Prior research has shown promise regarding the role of HIIT in improving QoL, particularly in specific clinical groups (Lavín-Pérez et al. 2021; Reed et al. 2022); however, there are no large-scale pooled analyses investigating its effects across varying populations. The use of HIIT to improve QoL may provide an avenue of non-pharmaceutical treatment, which can be individually tailored using a variety of protocols and approaches (Cassidy et al. 2017). Therefore, the aim of this study was to establish the effectiveness of HIIT on physical, mental, and overall QoL in both clinical and non-clinical participant groups compared to a non-intervention control.
Methodology
This review was performed according to the Preferred reporting items for Systematic Reviews and Meta-analyses (PRISMA) guidelines (Page et al. 2021).
Search strategy
This work is a sub-study of a larger systematic review and meta-analysis registered to PROSPERO (CRD42022326576). As such, a systematic search of PubMed (MEDLINE), the Cochrane Library and Web of Science was conducted using the key words ‘high-intensity interval training’ and ‘HIIT’ to broadly identify all published HIIT trials of varying outcomes in which QoL data was later extracted from. Studies published before June 2022 were considered. Prior meta-analyses and their respective reference lists were also rigorously screened for any relevant HIIT and QoL research not identified within the broad search.
Screening, eligibility and data extraction
Following conduction of the search, Rayyan was used by two authors (MG and JE) who independently screened all studies for eligibility. All studies were screened by title and abstract for initial relevance. Those studies included following the initial inclusion phase were screened by full text. Subsequently, the QoL, study characteristic and intervention-specific data of all included studies was extracted via Microsoft Excel and any inconsistencies in data collection or confliction regarding study eligibility were discussed by the researchers until a consensus was reached. The opinion of a third researcher (JOD) was provided if necessary.
Studies were considered eligible if they reported the pre and post HIIT intervention changes in questionnaire QoL across any validated domain or scale with a corresponding non-intervention control group. Validated domains included SF-36, SF-12, HRQOL, WHOQOL, WEMBES, MLHFQ, MSqOL-54, KCCQ, EQ-5D, EQ-5D-5L and IBDQ. Participants were required to be ≥18 years of age with no predetermined limitations on health or disease state. The non-intervention control groups of the included papers were required to minimise confounders, with any dietary, counselling or exercise influence resulting in exclusion. Where applicable, studies that included an MICT group adjacent to HIIT and control were included. HIIT was defined as an exercise intervention performed in high intensity intervals that contained active or passive rest periods (Gibala et al. 2012). Exercise intervals were considered high intensity according to the EXPERT tool (Hansen et al. 2017) at intensity metrics falling within the categories of ‘High intensity, vigorous effort’ or ‘Very hard effort’.
Due to variation in QoL instruments and scoring across different studies, data extraction was standardised for consistency. If a specific physical QoL value was not given, then physical functioning/health was used depending on the questionnaire measuring QoL. If a sole mental QoL measure was not available, then a mental/emotional wellbeing value was used. If overall QoL was not available, then a general health value was used.
Methodological quality of studies
Study quality was measured via the ‘Tool for the assEssment of Study qualiTy and reporting in EXercise’ (TESTEX) (Smart et al. 2015). The TEXTEX scale is a 15-point scoring tool, with 5 points allocated for study quality and 10 points for reporting. Full TESTEX scores for the included studies can be found in the supplementary file (Table S1).
Statistical analysis
Pooled analyses of all studies were performed individually for overall, physical, and mental QoL. Owing to variances in QoL instruments used across the different studies, the standardised mean difference (SMD) was selected as the appropriate outcome measure. SMD effect thresholds were as follows: 0.2-0.5 small effect, 0.5-0.8 medium effect and above 0.8 as a large effect (Cohen 1988). The SMD between the HIIT group and non-intervention control group was measured for each QoL category. Separate secondary analyses were also performed comparing HIIT and MICT. Data was synthesised using Comprehensive Meta-Analysis (Comprehensive Meta-Analysis Version 3, Biostat, Englewood, NJ, USA). Statistical heterogeneity was performed alongside the pooled analysis and reported as the I2 statistic. If the I2 statistic is >40% it was considered significant. Past the I2 threshold, Eggers Regression Test (Egger et al. 1997) was systematically planned to create a funnel plot looking for asymmetry related to potential publication bias. Random effects analysis was conducted when interstudy variability was confirmed through significant heterogeneity. Pooled analysis results were considered significant if the P value was <0.05 and the Z-Value >2.
Results
Search selection
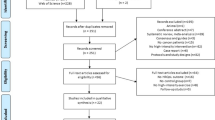
Figure 1 details the PRISMA flowchart. 4033 papers were identified through the systematic search. Following duplicate removal, 2508 papers remained, which then underwent abstract and title screening. 258 papers were full text screened against the inclusion criteria with 9 studies included from the search. Subsequent screening of previous meta-analyses and their respective reference lists identified a further 18 papers, of which 13 were included in the final pool. Ultimately, 22 studies constituting 24 effect sizes were analysed.
Study characteristics
1322 individuals participated in the included studies. The included studies contain a wide variety of populations, QoL instruments and training characteristics, as seen in Tables 1 and 2. All studies except one (Burn et al. 2021) were randomised trials. 14 studies compared the effects of HIIT on physical QoL, 13 on mental QoL and 17 studies on overall QoL. Five studies additionally compared HIIT vs MICT, constituting the secondary analysis of this work. As demonstrated in the study TESTEX scoring, common limitations include limited activity monitoring in the control groups, no blinding of assessors and participants, and a lack of intention to treat analysis.
HIIT and overall, physical and mental QoL
Figures 2, 3 and 4 detail the overall, physical and mental QoL SMD between the HIIT and non-intervention control groups, respectively. There was a statistically significant ‘medium’ improvement in overall QoL in HIIT compared to the control group (SMD: 0.554, CI= 0.210-0.898, p=0.002). There was a statistically significant ‘small’ improvement in physical QoL following HIIT compared to the control group (SMD: 0.405, CI= 0.110- 0.700, p=0.007). Finally, there was also a significant ‘small’ improvement in mental QoL in HIIT compared to the control group (SMD: 0.473, CI= 0.043-0.902, p=0.031).
HIIT Vs MICT on overall QoL
The secondary analysis of 5 studies comparing HIIT against MICT demonstrated no significant difference in improvement between the two modes (SMD= -0.094, CI= -0.506-0.318, p=0.655).
Publication bias and heterogeneity
All analyses demonstrated significant statistical heterogeneity (I2: overall QoL= 70.319%, physical QoL= 83.605%, mental QoL= 78.737% and HIIT vs MICT= 51.067%). Eggers Regression test demonstrated funnel plot asymmetry and therefore evidence of publication bias for the physical QoL domain (p=0.0085, Figure S1). Overall QoL, mental QoL, and HIIT vs MICT showed no evidence of publication bias.
Discussion
This work aimed to measure the effects of HIIT on physical, mental, and overall QoL in both clinical and non-clinical populations. The findings of this meta-analysis demonstrate statistically significant improvements in all domains of QoL across different instruments. As determined by Cohen’s SMD effect thresholds (Cohen 1988), the improvements observed in this work are of a ‘small’ to ‘medium’ effect size. Specifically, physical QoL and mental QoL individually produced small effect sizes, while overall QoL elicited a medium effect size. Furthermore, HIIT appears as effective as MICT in improving overall QoL, offering a more time-efficient exercise option. As the largest-scale analysis to-date, these findings support earlier preliminary evidence in the potential utility of HIIT in improving QoL across different populations.
Several reviews and large-scale trials have supported the effectiveness of HIIT for improving physical, mental and overall domains of QoL in various populations, with particular research interest on its role in clinical groups such as those with cancer (Lavín-Pérez et al. 2021), atrial fibrillation (Reed et al. 2022) and heart transplant recipients (Yu et al. 2022). Furthermore, the capacity for HIIT to produce QoL improvements similar to that of MICT is also well-supported in the broad literature, with several meta-analyses demonstrating no significant differences between HIIT and MICT on QoL in clinical populations (Gomes-Neto et al. 2017, 2018; Lavín-Pérez et al. 2021; Anjos et al. 2022). Given the impairment in QoL in patients with debilitating chronic diseases, these findings may be of clinical importance. This is particularly true considering the poor adoption and adherences rates to traditionally recommended MICT in these populations (Argent et al. 2018), highlighting the potential utility of HIIT as an alternative exercise intervention with similar QoL-enhancing capabilities.
In understanding the mechanistic underpinnings of QoL improvements, it is important to consider the probable confounding and interdependence between all domains of QoL, with improvements in any given single domain likely translating into changes in all domains (Post 2014). Physically, the well-established physiological adaptations frequently seen following HIIT may translate into improvements, particularly in older groups and/or those suffering from debilitating chronic conditions, in the capacity to complete more activities of daily living. In clinical populations such as heart failure, QoL is profoundly impaired (in both preserved and reduced ejection fraction) (Hobbs et al. 2002; Stewart et al. 2010), largely owing to patient symptoms and limited functional capacity. Therefore, the frequently described improvements in cardiometabolic health and peak VO2 (Batacan et al. 2017b) following HIIT may be of particular importance regarding the QoL of such patient groups, as has been demonstrated in previous exercise training studies (Edwards and O’Driscoll 2022).
Regarding mental QoL, these findings support that of a recent large-scale systematic review and meta-analysis (Martland et al. 2022) in clinical and non-clinical populations. This work from Martland et al. (2022) reported significant improvements in mental well-being, depression severity and perceived stress, with suggestions of sleep and psychological distress improvements. Alike the current analysis, Martland et al. (2022) found these improvements to be of a small to medium effect size. Combined with the findings of the present study, HIIT certainly appears an effective strategy to elicit improvements in psychological well-being. However, further research into populations with psychological disorders is warranted to establish the transferability of this data into specific clinical sub-groups.
Limitations
We found significant statistical heterogeneity across all analyses in this work. This is likely attributable to inter-study methodological differences such as the utilised QoL instruments and HIIT protocols, as well as wide population variation in the inclusion of clinical and non-clinical populations. We subsequently performed random-effects analyses in an attempt to account for this, and explored the Eggers regression tests for publication bias. We did indeed find publication bias for the physical QoL domain which should be appropriately considered in the interpretation of these results. Furthermore, some studies (Madssen et al. 2014; Malmo et al. 2016; Ellingsen et al. 2017; Mokhtarzade et al. 2017; Romain et al. 2019; Atan and Karavelioğlu 2020; Burn et al. 2021; Mueller et al. 2021; Ochi et al. 2022; Woodfield et al. 2022) measured QoL as a secondary outcome so may not have been appropriately powered.
Future implications
Only 5 studies included both HIIT and MICT QoL data. As such, future research is needed to assess the efficacy of HIIT compared to the traditionally recommended MICT. Additionally, larger-scale homogenous research is needed in specific populations before these findings can be extrapolated to specified clinical and non-clinical groups. Further research into varying HIIT protocols, with specific comparative data between sprint interval training and aerobic interval training protocols are needed to truly discern optimal HIIT prescription practices.
Conclusion
HIIT produces statistically significant improvements in physical, mental and overall QoL at a small to medium effect size across a range of QoL instruments in clinical and non-clinical populations. Furthermore, HIIT appears as effective as MICT in improving overall QoL, offering a more time-efficient non-pharmacological option. As the largest-scale analysis to-date, these findings support earlier preliminary evidence regarding the potential utility of HIIT in improving QoL across different populations.
Data availability
Available on request from corresponding author.
Code availability
Not applicable.
References
Adams SC, DeLorey DS, Davenport MH et al (2018) Effects of high-intensity interval training on fatigue and quality of life in testicular cancer survivors. Br J Cancer 118:1313–1321. https://doi.org/10.1038/s41416-018-0044-7
Alarcón-Gómez J, Chulvi-Medrano I, Martin-Rivera F, Calatayud J (2021) Effect of high-intensity interval training on quality of life, sleep quality, exercise motivation and enjoyment in sedentary people with type 1 diabetes mellitus. Int J Environ Res Public Health 18. https://doi.org/10.3390/ijerph182312612
Anjos JM, Neto MG, dos Santos FS et al (2022) The impact Of high-intensity interval training On functioning And health-related quality Of life In post-stroke patients: A systematic review With meta-analysis. Clin Rehabil 36:726–739. https://doi.org/10.1177/02692155221087082
Argent R, Daly A, Caulfield B (2018) Patient involvement with home-based exercise programs: Can connected health interventions influence adherence? JMIR Mhealth Uhealth 6. https://doi.org/10.2196/MHEALTH.8518
Atan T, Karavelioğlu Y (2020) Effectiveness of High-Intensity Interval Training vs Moderate-Intensity Continuous Training in Patients With Fibromyalgia: A Pilot Randomized Controlled Trial. Arch Phys Med Rehabil 101:1865–1876. https://doi.org/10.1016/j.apmr.2020.05.022
Ballin M, Lundberg E, Sörlén N et al (2019) Effects of interval training on quality of life and cardiometabolic risk markers in older adults: a randomized controlled trial. Clin Interv Aging 14:1589–1599. https://doi.org/10.2147/CIA.S213133
Batacan RB, Duncan MJ, Dalbo VJ et al (2017a) Effects of high-intensity interval training on cardiometabolic health: a systematic review and meta-analysis of intervention studies. Br J Sports Med 51:494–503. https://doi.org/10.1136/bjsports-2015-095841
Batacan RB, Duncan MJ, Dalbo VJ et al (2017b) Effects of high-intensity interval training on cardiometabolic health: A systematic review and meta-analysis of intervention studies. Br J Sports Med 51:494–503
Bull FC, Al-Ansari SS, Biddle S et al (2020) World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br J Sports Med 54:1451–1462. https://doi.org/10.1136/bjsports-2020-102955
Burn NL, Weston M, Atkinson G et al (2021) Brief Exercise at Work (BE@Work): A Mixed-Methods Pilot Trial of a Workplace High-Intensity Interval Training Intervention. Front Sports Act Living 3:699608. https://doi.org/10.3389/fspor.2021.699608
Cassidy S, Thoma C, Houghton D, Trenell MI (2017) High-intensity interval training: a review of its impact on glucose control and cardiometabolic health. Diabetologia 60:7–23. https://doi.org/10.1007/s00125-016-4106-1
Chrysohoou C, Tsitsinakis G, Vogiatzis I et al (2014) High intensity, interval exercise improves quality of life of patients with chronic heart failure: a randomized controlled trial. QJM 107:25–32. https://doi.org/10.1093/qjmed/hct194
Cohen J (1988) Statistical Power analysis for the behavioral sceinces, 2nd edn. Erlbaum, Hillsdale
Connolly LJ, Bailey SJ, Krustrup P et al (2017) Effects of self-paced interval and continuous training on health markers in women. Eur J Appl Physiol 117:2281–2293. https://doi.org/10.1007/s00421-017-3715-9
Connolly LJ, Scott S, Morencos CM et al (2020) Impact of a novel home-based exercise intervention on health indicators in inactive premenopausal women: a 12-week randomised controlled trial. Eur J Appl Physiol 120:771–782. https://doi.org/10.1007/s00421-020-04315-7
Edwards JJ, O’Driscoll JM (2022) Exercise Training in Heart failure with Preserved and Reduced Ejection Fraction: A Systematic Review and Meta-Analysis. Sports Med Open 8:1–11. https://doi.org/10.1186/S40798-022-00464-5/FIGURES/4
Edwards JJ, Taylor KA, Cottam C et al (2021) Ambulatory blood pressure adaptations to high-intensity interval training: a randomized controlled study. J Hypertens 39:341–348. https://doi.org/10.1097/HJH.0000000000002630
Edwards J, De Caux A, Donaldson J et al (2022) Isometric exercise versus high-intensity interval training for the management of blood pressure: a systematic review and meta-analysis. Br J Sports Med 56:506–514. https://doi.org/10.1136/bjsports-2021-104642
Egger M, Smith GD, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634. https://doi.org/10.1136/BMJ.315.7109.629
Ellingsen Ø, Halle M, Conraads V et al (2017) High-Intensity Interval Training in Patients With Heart Failure With Reduced Ejection Fraction. Circulation 135:839–849. https://doi.org/10.1161/CIRCULATIONAHA.116.022924
Engel FA, Rappelt L, Held S, Donath L (2019) Can high-intensity functional suspension training over eight weeks improve resting blood pressure and quality of life in young adults? A Randomized Controlled Trial. Int J Environ Res Public Health 16. https://doi.org/10.3390/ijerph16245062
GHRAM A, JENAB Y, SOORI R et al (2021) High-Intensity Interval Training in Patients with Pulmonary Embolism: A Randomized Controlled Trial. Med Sci Sports Exerc 53:2037–2044. https://doi.org/10.1249/MSS.0000000000002680
Gibala MJ, Little JP, MacDonald MJ, Hawley JA (2012) Physiological adaptations to low-volume, high-intensity interval training in health and disease. J Physiol 590:1077–1084. https://doi.org/10.1113/jphysiol.2011.224725
Gomes Neto M, Durães AR, Conceição LSR et al (2018) High intensity interval training versus moderate intensity continuous training on exercise capacity and quality of life in patients with heart failure with reduced ejection fraction: A systematic review and meta-analysis. Int J Cardiol 261:134–141. https://doi.org/10.1016/J.IJCARD.2018.02.076
Gomes-Neto M, Durães AR, dos Reis HFC et al (2017) High-intensity interval training versus moderate-intensity continuous training on exercise capacity and quality of life in patients with coronary artery disease: A systematic review and meta-analysis. Eur J Prev Cardiol 24:1696–1707. https://doi.org/10.1177/2047487317728370
Hansen D, Dendale P, Coninx K et al (2017) The European Association of Preventive Cardiology Exercise Prescription in Everyday Practice and Rehabilitative Training (EXPERT) tool: A digital training and decision support system for optimized exercise prescription in cardiovascular disease. Concept, definitions and construction methodology. Eur J Prev Cardiol 24:1017–1031. https://doi.org/10.1177/2047487317702042
Hobbs FDR, Kenkre JE, Roalfe AK et al (2002) Impact of heart failure and left ventricular systolic dysfunction on quality of life: A cross-sectional study comparing common chronic cardiac and medical disorders and a representative adult population. Eur Heart J 23:1867–1876. https://doi.org/10.1053/euhj.2002.3255
Ito S (2019) High-intensity interval training for health benefits and care of cardiac diseases - The key to an efficient exercise protocol. World J Cardiol 11:171–188. https://doi.org/10.4330/wjc.v11.i7.171
Jacobs JE (2009) Quality of life: what does it mean for general practice? Br J Gen Pract 59:807–808. https://doi.org/10.3399/bjgp09X472854
Lavín-Pérez AM, Collado-Mateo D, Mayo X, et al (2021) Effects of high-intensity training on the quality of life of cancer patients and survivors: a systematic review with meta-analysis. Scientific Reports 11:1–19. https://doi.org/10.1038/s41598-021-94476-y
Madssen E, Arbo I, Granøien I et al (2014) Peak Oxygen Uptake after Cardiac Rehabilitation: A Randomized Controlled Trial of a 12-Month Maintenance Program versus Usual Care. PLoS One 9:e107924. https://doi.org/10.1371/journal.pone.0107924
Malmo V, Nes BM, Amundsen BH et al (2016) Aerobic Interval Training Reduces the Burden of Atrial Fibrillation in the Short Term. Circulation 133:466–473. https://doi.org/10.1161/CIRCULATIONAHA.115.018220
Martland R, Korman N, Firth J et al (2022) Can high-intensity interval training improve mental health outcomes in the general population and those with physical illnesses? A systematic review and meta-analysis. Br J Sports Med 56:279–291. https://doi.org/10.1136/BJSPORTS-2021-103984
Mokhtarzade M, Ranjbar R, Majdinasab N et al (2017) Effect of aerobic interval training on serum IL-10, TNFα, and adipokines levels in women with multiple sclerosis: possible relations with fatigue and quality of life. Endocrine 57:262–271. https://doi.org/10.1007/s12020-017-1337-y
Mueller S, Winzer EB, Duvinage A et al (2021) Effect of High-Intensity Interval Training, Moderate Continuous Training, or Guideline-Based Physical Activity Advice on Peak Oxygen Consumption in Patients With Heart Failure With Preserved Ejection Fraction. JAMA 325:542. https://doi.org/10.1001/jama.2020.26812
Ochi E, Tsuji K, Narisawa T et al (2022) Cardiorespiratory fitness in breast cancer survivors: a randomised controlled trial of home-based smartphone supported high intensity interval training. BMJ Support Palliat Care 12:33–37. https://doi.org/10.1136/bmjspcare-2021-003141
Page MJ, McKenzie JE, Bossuyt PM, et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ n71. https://doi.org/10.1136/bmj.n71
Post MWM (2014) Definitions of quality of life: what has happened and how to move on. Top Spinal Cord Inj Rehabil 20:167–180. https://doi.org/10.1310/sci2003-167
Reed JL, Terada T, Vidal-Almela S et al (2022) Effect of High-Intensity Interval Training in Patients With Atrial Fibrillation: A Randomized Clinical Trial. JAMA Netw Open 5:e2239380–e2239380. https://doi.org/10.1001/JAMANETWORKOPEN.2022.39380
Romain AJ, Fankam C, Karelis AD et al (2019) Effects of high intensity interval training among overweight individuals with psychotic disorders: A randomized controlled trial. Schizophr Res 210:278–286. https://doi.org/10.1016/j.schres.2018.12.021
Smart NA, Waldron M, Ismail H et al (2015) Validation of a new tool for the assessment of study quality and reporting in exercise training studies: TESTEX. Int J Evid Based Healthc 13:9–18. https://doi.org/10.1097/XEB.0000000000000020
Stavrinou PS, Bogdanis GC, Giannaki CD et al (2018) High-intensity Interval Training Frequency: Cardiometabolic Effects and Quality of Life. Int J Sports Med 39:210–217. https://doi.org/10.1055/s-0043-125074
Stavrinou PS, Bogdanis GC, Giannaki CD et al (2019) Effects of high-intensity interval training frequency on perceptual responses and future physical activity participation. Appl Physiol Nutri Metab 44:952–957. https://doi.org/10.1139/apnm-2018-0707
Stensvold D, Viken H, Steinshamn SL, et al (2020) Effect of exercise training for five years on all cause mortality in older adults—the Generation 100 study: randomised controlled trial. BMJ 371. https://doi.org/10.1136/BMJ.M3485
Stewart S, Ekman I, Ekman T et al (2010) Population impact of heart failure and the most common forms of cancer: A study of 1 162 309 hospital cases in Sweden (1988 to 2004). Circ Cardiovasc Qual Outcomes 3:573–580. https://doi.org/10.1161/CIRCOUTCOMES.110.957571
Tew GA, Batterham AM, Colling K et al (2017) Randomized feasibility trial of high-intensity interval training before elective abdominal aortic aneurysm repair. British J Surg 104:1791–1801. https://doi.org/10.1002/bjs.10669
Tew GA, Leighton D, Carpenter R et al (2019) High-intensity interval training and moderate-intensity continuous training in adults with Crohn’s disease: a pilot randomised controlled trial. BMC Gastroenterol 19:19. https://doi.org/10.1186/s12876-019-0936-x
Vella CA, Taylor K, Drummer D (2017) High-intensity interval and moderate-intensity continuous training elicit similar enjoyment and adherence levels in overweight and obese adults. Eur J Sport Sci 17:1203–1211. https://doi.org/10.1080/17461391.2017.1359679
Wewege M, van den Berg R, Ward RE, Keech A (2017) The effects of high-intensity interval training vs. moderate-intensity continuous training on body composition in overweight and obese adults: a systematic review and meta-analysis. Obesity Rev 18:635–646. https://doi.org/10.1111/OBR.12532
Withall J, Jago R, Fox KR (2011) Why some do but most don’t. Barriers and enablers to engaging low-income groups in physical activity programmes: a mixed methods study. BMC Public Health 11:507. https://doi.org/10.1186/1471-2458-11-507
Woodfield JC, Clifford K, Wilson GA et al (2022) Short-term high-intensity interval training improves fitness before surgery: A randomized clinical trial. Scand J Med Sci Sports 32:856–865. https://doi.org/10.1111/sms.14130
Yu AKD, Kilic F, Dhawan R et al (2022) High-intensity interval training among heart failure patients and heart transplant recipients: A Systematic Review. Cureus 14. https://doi.org/10.7759/CUREUS.21333
Funding
The authors declare that no funds, grants or other support were received in the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception, design and search strategy. MG and JE conducted the systematic review and acquisition of data. JE and JOD performed the data analysis. MG, JE, JM, AG, SBL and JOD all assisted with the interpretation and written development of the manuscript. MG, JE, JM, AG, SBL and JOD all contributed to the drafting and revision of the final article. All authors approved the final submitted version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no financial or non-financial interests to disclose.
Ethics approval
This work is a systematic review and meta-analysis and thus no ethical approval is required.
Consent to participate and publish
All analysed studies were responsible for acquiring written informed consent from the respective participants.
Consent for publication
All analysed studies were responsible for acquiring written informed consent from the respective participants.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 143 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Griffiths, M., Edwards, J.J., McNamara, J. et al. The effects of high intensity interval training on quality of life: a systematic review and meta-analysis. J Public Health (Berl.) (2024). https://doi.org/10.1007/s10389-024-02192-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10389-024-02192-4