Abstract
Most competitive social health insurance markets include risk equalization to compensate insurers for predictable variation in healthcare expenses. Empirical literature shows that even the most sophisticated risk equalization models—with advanced morbidity adjusters—substantially undercompensate insurers for selected groups of high-risk individuals. In the presence of premium regulation, these undercompensations confront consumers and insurers with incentives for risk selection. An important reason for the undercompensations is that not all information with predictive value regarding healthcare expenses is appropriate for use as a morbidity adjuster. To reduce incentives for selection regarding specific groups we propose overpaying morbidity adjusters that are already included in the risk equalization model. This paper illustrates the idea of overpaying by merging data on morbidity adjusters and healthcare expenses with health survey information, and derives three preconditions for meaningful application. Given these preconditions, we think overpaying may be particularly useful for pharmacy-based cost groups.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Most competitive social health insurance markets include risk equalization (RE) to compensate insurers for predictable variation in medical spending. In the past decades RE models have evolved from simple demographic models—using risk adjusters based on age and gender—to more sophisticated models using risk adjusters based on (prior) healthcare utilization and expenses (henceforth called morbidity adjusters). For example, the RE model used in the health insurance exchanges in the United States and the one used in the German sickness fund market include morbidity adjusters based on diagnoses obtained from healthcare utilization [1, 2]. The RE model used in the Dutch basic health insurance includes morbidity adjusters based on diagnoses, drug prescriptions, durable medical equipment and prior expenses. Even these sophisticated RE models substantially undercompensate insurers for selected groups of high-risk individuals [3, 4]. With undercompensation we mean that the predicted expenses (according to the relevant RE model) systematically fall below the actual expenses. The opposite is referred to as overcompensation. Under premium regulation, as applied in all aforementioned countries, under- and overcompensations confront consumers and insurers with incentives for risk selection [5]. Risk selection is undesirable since it may reduce (1) the quality of healthcare (since insurers have a disincentive to meet the preferences of the chronically ill), (2) the efficiency of healthcare (since risk selection may be a more cost-effective strategy for insurers to make profits than improving the efficiency of care), (3) the efficient sorting of consumers among health plans (when market segmentation distorts the premium levels of health plans), and (4) solidarity (when the same market segmentation causes the chronically ill to face higher premiums than the healthy).
An important reason for the remaining undercompensations is that morbidity adjusters in RE models are—to some extent—incomplete since not all information with predictive value regarding healthcare expenses is considered appropriate for use as a morbidity adjuster. For example, Dutch enrollees are classified in a pharmacy-based cost group (PCG) for Parkinson’s disease only if they used at least 181 of the DDD (defined daily dose) of the relevant drugs in the previous year. The rationale for this 181-DDD threshold is to mitigate perverse incentives for insurers to provide enrollees with additional drugs with the goal of receiving higher RE payments in later years. With a threshold of 1 DDD, for instance, it would be relatively easy and profitable for insurers to provide additional drugs to some enrollees in order to have them classified in a PCG for next year. Although the 181-DDD threshold mitigates perverse incentives it also results in undercompensation of enrollees with Parkinson’s disease who did not exceed this threshold. As a result the entire group of enrollees who have used the relevant drugs (i.e. those who used ≥181 DDD plus those who used <181 DDD in the previous year) will on average be undercompensated, leaving insurers with incentives for risk selection against the entire group.
To reduce incentives for risk selection regarding specific groups we propose ‘overpaying’ morbidity adjusters that are already in the RE model. With overpaying we mean that the group of individuals scoring on a particular morbidity adjuster is provided with an explicit extra compensation on top of their average expenses. In other words, this group is ‘overcompensated’ on purpose. This explicit extra compensation is referred to as ‘overpayment’. In the example of the PCG for Parkinson’s disease, overpaying could mean that individuals in this PCG are overpaid to such an extent that the entire group of people who used the relevant drugs in the previous year (i.e. including those who did not reach the 181-DDD threshold) is sufficiently compensated. The goal of this paper is to illustrate and discuss the effects of overpaying and to derive preconditions for meaningful real-world application of this concept.
The paper is structured as follows. “Criteria for morbidity adjusters in risk equalization models” provides some examples of restrictions applied to morbidity adjusters used in practice over the past two decades. “The essence of overpaying morbidity adjusters” describes the essence of overpaying morbidity adjusters and “Empirical illustration” provides a simplified empirical illustration. To indicate the potential for real-world application, “Preconditions for overpaying morbidity adjusters” formulates three preconditions and “Possible applications” applies these to some morbidity adjusters used in practice. “Overpaying versus optimal risk adjustment” discusses the similarities and differences between the ideas presented here and the concept of optimal risk adjustment proposed by Glazer and McGuire [6, 7]. “Conclusion” summarizes the main conclusions and “Discussion” provides issues for discussion and further research.
Criteria for morbidity adjusters in risk equalization models
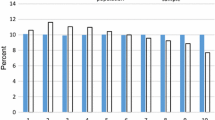
For meaningful use in RE models, risk factors should at least have some predictive value regarding future healthcare expenses. Predictive value is not the only criterion, however. Other relevant criteria are validity, appropriateness of incentives and feasibility [8]. Validity implies that a morbidity adjuster should strongly relate to a chronic condition. If this is not the case, inclusion of the morbidity adjuster in the RE model may lead to overcompensation of people without chronic conditions. Appropriateness of incentives implies that inclusion of a morbidity adjuster in the RE model should not reduce health insurers’ incentives for efficiency. Morbidity adjusters directly based on prior expenses, for instance, may be considered inappropriate since these would punish efficient insurers with lower RE payments. Moreover, morbidity adjusters should not create incentives for insurers to provide additional—but therapeutically unnecessary—healthcare. For example, if use of only one DDD of a certain drug is needed for classification in a PCG, insurers may be confronted with incentives to provide enrollees with some additional drugs in order to receive higher RE payments in later years. Feasibility implies that the information must be obtainable for all (potential) enrollees without undue expenditures of time or money. Table 1 provides six examples of how these criteria led to restrictions of morbidity adjusters developed and applied in the United States and/or Europe over the past decades. While these restrictions are justified by the aforementioned criteria, they may result in selection incentives regarding specific groups. Hence we show how overpaying can mitigate this problem.
The essence of overpaying morbidity adjusters
Let us illustrate our framework for a pharmacy-based cost group, which we refer to as ‘PCG-P’, that is included in the RE model in the form of a dummy variable. Under the conventional RE estimation procedure of ordinary least-squares regression (OLS), the group of enrollees classified in PCG-P (group X) is sufficiently compensated. This will probably not be the case for another group that also used the relevant drugs for PCG-P but stayed below the 181-DDD threshold (group Y). Though this group did not reach the threshold, it is likely to be overrepresented with high-risk individuals. Exclusion of group Y from PCG-P probably leads to undercompensation of this group. As a result, the entire group that used the relevant drugs (i.e. XY) will also be undercompensated. Given that the model is estimated with OLS and based on a zero-sum principle, as is common in practice, the complementary group of people who did not use any DDD of the drugs relevant for PCG-P (group Z) will be overcompensated. The essence of our proposal is that undercompensation of XY and overcompensation of Z can be removed by overpaying X. For a single set of X, Y and Z, the height of overpayment can be calculated easily.
In case of zero-sum RE, an increase of the RE payment for group X implies a decrease of the RE payment for the complementary group YZ. If C denotes the change in average RE payment for X, and D denotes the average payment change for YZ, the association between C and D reads:
where n x , n y and n z represent the number of individuals in groups X, Y and Z. If the regulator wants to reduce undercompensation for XY to zero, C should be such that:
where the left-hand side represents the average per person actual expenses in group XY and the right-hand side represents the average per person predicted expenses for group XY plus the net effect of overpayment C and underpayment D. In case of the zero-sum RE, Eq. (2) implies that the overcompensation on the complementary Z is reduced to zero as well, i.e.:
where the left-hand side represents the average per person actual expenses in group Z and the right-hand side represents the average per person predicted expenses for group Z minus D. Integration of Eqs. (1, 3) reveals the overpayment C that is necessary for reducing the undercompensation for XY (and the overcompensation for Z) to zero:
Equation (4) implies a first precondition for overpaying: availability of information on population frequency, average expenses and predicted expenses (according to the relevant RE model) for the relevant X, Y and Z groups. The next section provides an empirical illustration in which this information is obtained from administrative data and health survey information.
Empirical illustration
For an empirical illustration of our framework we merge administrative data with health survey information. The administrative data include individual-level information on annual healthcare expenses and risk characteristics for almost the entire Dutch population in 2011 (N = 16.4 million) and have been used in practice for estimating the Dutch RE model of 2014. The information comes from various administrative sources, including insurers, the tax collector and the registration service for social benefits. The health survey information comes from a representative sample of the Dutch population in 2010 (N = 16,061). This survey is held on an annual basis by Statistics Netherlands and includes questions on general health status, physical and mental impairments, particular diseases and prior utilization of healthcare. The combination of this administrative and survey information allows (1) estimating the RE model of 2014 on data from year t, (2) predicting individual expenses for year t, (3) calculating individual residual expenses for year t, (4) defining selective groups of high-risk individuals using the survey information from year t−1, and (5) calculating the average under/overcompensation for these groups. Table 2 shows the average undercompensation for six groups of relatively high-risk individuals. Although the Dutch RE model succeeds in compensating for a major share of the above-average expenses for these risk groups, substantial undercompensations remain.
The Dutch RE model of 2014 is the product of more than 20 years of research and experience and includes the following risk classes: 40 classes based on interactions between age and gender; 24 risk classes based on the use of specific prescription drugs in the previous year, referred to as pharmacy-based cost groups or PCGs; 16 risk classes based on diagnostic information from hospital treatment in the previous year, referred to as diagnoses-based cost groups or DCGs; 7 risk classes for people with high healthcare expenses in multiple prior years, referred to as multiple-year high cost groups or MHCGs; 5 risk classes based on the use of durable medical equipment in the previous year, referred to as durable medical equipment cost groups or DMEGs; 12 risk classes based on interactions between socioeconomic status and age; 10 risk classes based on regional characteristics; and 19 risk classes based on interactions between source of income and age. All risk adjusters have been carefully developed in research programs initiated by the Dutch Ministry of Health. In this empirical illustration we will not question the appropriateness of these risk adjusters in terms of the criteria described in “Criteria for morbidity adjusters in risk equalization models”.
Of all risk adjusters in the Dutch RE model, PCGs, DCGs, DMEGs and MHCGs are the most direct indicators of health status and are denoted as ‘morbidity’ adjusters. A reason for the undercompensations in Table 2 is that these morbidity adjusters do not identify all high-risk individuals. This can be illustrated by a simple crossing of two classifications: (1) yes/no classified in a PCG, DCG, DMEG and/or MHCG (i.e. information obtained from the administrative data) and (2) yes/no self-reported chronic condition (i.e. information obtained from the survey data). Table 3 shows the population frequency, average actual expenses, average predicted expenses by the Dutch RE model of 2014 and the average under- or overcompensation per group, conditional on the survey sample (because the information on self-reported chronic condition is only available for survey respondents). As was already shown in Table 2, the group with a self-reported chronic condition (31.5 % of the population) is undercompensated by 331 euros per person per year. The complementary group with no chronic condition (68.5 %) is overcompensated by 153 per person per year. More remarkable is the undercompensation of 112 euros for the group with a ‘PCG, DCG, DMEG and/or MHCG’ (22 %) and the overcompensation of 32 euros for the complementary group (78 %), though these over- and undercompensations are not statistically significant from zero. Looking at crossings of ‘PCG, DCG, DMEG and/or MHCG’ and ‘self-reported chronic condition’, it is not surprising that the average expenses are highest (5337 euros) for the group scoring on both items (16.2 %) and lowest (785 euros) for the group scoring on none of these items (62.6 %). The groups scoring on only one of the two items (5.8 and 15.4 %) have average expenses somewhere in between, i.e. 2990 and 1524 euros, respectively. Table 3 clearly shows that not all individuals with a self-reported chronic condition are identified by PCG, DCG, DMEG and/or MHCG. As a result, the entire group of relatively high-risk individuals, i.e. those with a PCG, DCG, DMEG, MHCG and/or a self-reported chronic condition (5.8 + 15.4 + 16.2 = 37.4 %), is undercompensated (by 215 euros per person per year). The complementary group, i.e. those without a PCG, DCG, DMEG, MHCG and without a self-reported chronic condition (62.6 %) is overcompensated (by 129 euros per person per year).
Though we are aware that a sample with ‘just’ 16,061 records is probably not appropriate for real-world applications of overpaying (see next section), it provides a good basis for illustrating the effects of overpaying. Let us assume the regulator wants to remove the undercompensation on the total group with a PCG, DCG, DMEG, MHCG and/or a self-reported chronic condition (37.4 % of the population). In the terminology of the previous section this would be the XY group. The complementary group of people without a PCG, DCG, DMEG, MHCG and without a self-reported chronic condition (62.6 %) would be the Z group. Table 4 presents the results for both the XY and the Z group, which are no more than weighted averages derived from Table 3. The Dutch RE model undercompensates the XY group by 215 euros and overcompensates the Z group by 129 euros per person per year. When we enter the information from Table 3 into Eq. (4), the necessary overpayment for X (those with a PCG, DCG, DMEG and/or MHCG) appears to be 454.5 euros, on average, per person per year. This implies an underpayment of 128.2 euros for the complementary group (those without a PCG, DCG, DMEG and MHCG).
As expected, the overpayment for X (and underpayment for the complementary group) reduces the undercompensation for XY to zero (see also bottom row of Table 4). The same holds for the overcompensation of Z. As shown in Table 5, however, this is not true for the X and Y groups separately. For X, the initial undercompensation of 112 euros changes into an overcompensation of 342 euros, while for Y the initial undercompensation of 361 euros increases to an undercompensation of 490 euros. As a result, incentives for selection against Y and in favor of X increase. This implies a second pre-condition for overpaying morbidity adjuster X: risk selection against XY (and in favor of Z) must be considered more likely/problematical than risk selection against Y (and in favor of X). The next section elaborates on this and other preconditions.
Preconditions for overpaying morbidity adjusters
As concluded in “The essence of overpaying morbidity adjusters”, a first precondition for meaningful application of overpaying is availability of information on average expenses, predicted expenses and population frequency of the relevant X, Y and Z groups. For X this information is probably inherently available in the datasets used for RE, since X is included as a morbidity adjuster in the RE model. In case of explicit restrictions applied to morbidity adjusters (like the examples in Table 1) this may also be true for Y and Z, since these restrictions require availability of information to distinguish between X and Y. If information on Y and Z is not available for the entire population, it could be sufficient to subtract population frequency and average actual and predicted expenses from a sample. It should be said, however, that in the case of relatively small samples, such as the survey used in this paper (N = 16,061), these parameters may be influenced by random variation. Our empirical application may therefore not be feasible for real-world implementation.
As concluded in “Empirical illustration”, a second precondition is that risk selection against XY (and in favor of Z) must be considered more likely/problematical than risk selection against Y (and in favor of X). The reason is that overpaying improves compensations at the level of XY and Z, but worsens them at the level of X and Y. As a result, incentives for selection against Y and in favor of X increase. The likelihood of risk selection regarding a specific group does not only depend on the level of under- or overcompensation and the size of the group, but also on the possibilities for risk selection against or in favor of that group. Social health insurance markets often include open enrollment requirements, implying that insurers are not allowed to explicitly deter individuals. Nevertheless, insurers often have possibilities of exploiting subtle forms of risk selection via coverage, quality and service levels. For example, if patients with a certain disease are undercompensated by the RE model, and these patients have a preference for a specialist with the best reputation in treating this disease, insurers can discourage these patients from enrolling by not contracting this specialist. Such subtle forms of risk selection, however, are only possible if the preferences (in terms of coverage, quality and service levels) of overcompensated risk groups differ from those of the undercompensated risk groups. In the case of groups X and Y, this implies that risk selection may only occur if these groups are heterogeneous in their preferences.
The extent to which risk selection regarding a group is considered problematical depends on the potential selection actions and their effects. Some selection actions may be considered more problematical than others. For example, ‘quality skimping’ may be considered worse than ‘selective advertising’. The reason is that quality skimping may not only reduce solidarity but also the efficiency and quality of healthcare, contrary to selective advertising which will not directly affect efficiency and quality of care. Judging whether risk selection regarding X and Y is more problematical than risk selection regarding XY requires an evaluation of the potential selection actions regarding these groups and the consequences of these actions.
A third precondition is that X itself sufficiently fulfills the criteria for morbidity adjusters as listed in “Criteria for morbidity adjusters in risk equalization models”. Though all morbidity adjusters used in RE models have been (implicitly) approved by the regulator, a new round of evaluation may be necessary when considering overpaying. The reason is that overpayment of X intensifies incentives for insurers to have enrollees classified in group X. More specifically, incentives for insurers to avoid healthcare utilization that leads to classification in group X decrease (i.e. a loss of efficiency incentives) while incentives to provide additional—but therapeutically unnecessary—healthcare increase (i.e. an increase in perverse incentives). These intensified perverse incentives require reconsidering the likelihood that insurers will influence healthcare provision this way.
Possible applications
In theory overpaying can be applied to any type of morbidity adjuster. Let us define some possible modalities for the six cases in Table 1. For all these cases, group X could include the individuals classified under a morbidity adjuster. In case 1, group Y could include individuals with a diagnosis explicitly excluded from the relevant classification (but with predictive value for future healthcare expenses). In case 2, group Y could include individuals with an outpatient diagnosis of which the ‘inpatient counterpart’ (i.e. the same diagnosis for inpatient care) is included in the relevant classification. In case 3, group Y could include individuals with utilization of drugs explicitly excluded from the PCGs. In case 4, group Y could include users of the relevant drugs who did not reach the 181-DDD threshold. In case 5, group Y could include individuals with utilization of durable medical equipment (DME) explicitly excluded from the DMEGs. In case 6, group Y would include individuals with moderately high healthcare expenses in previous years. In all cases Z would be the complementary group of XY.
Real-world application of overpaying is only meaningful if the three preconditions mentioned in the previous section are sufficiently fulfilled. Availability of information is a ‘conditio sine qua non’. The other two preconditions may involve trade-offs, e.g. between the positive effects of avoiding risk selection and the negative effect of intensifying perverse incentives. The net benefit from overpaying morbidity adjusters is the balance of these positive and negative effects and may differ across types of morbidity adjusters and characteristics of healthcare schemes. With respect to the morbidity adjusters presented in Table 1, the net benefit of overpaying may be largest for the Dutch PCGs (case 4). In this case, group X includes individuals with 181 DDD or more of the relevant drug and group Y includes those with ‘just’ 1-180 DDD. In this particular case, risk selection against XY (and in favor of Z) may be more likely than risk selection against Y (and in favor of X). Moreover, the possibilities for providing additional drugs in order to have more enrollees classified in a PCG are minor (given the 181-DDD threshold). For the other cases the benefit may be smaller (but not necessarily negative). In case 2 it may be possible for insurers to substitute outpatient treatments with inpatient treatments. In the other cases, preferences of X and Y are likely to be heterogeneous to some extent, implying possibilities for risk selection against Y (and in favor of X). The latter also holds for the groups in our empirical illustration.
Overpaying versus optimal risk adjustment
The ideas presented in this paper relate to the concept of optimal risk adjustment proposed by Glazer and McGuire [6, 7]. Glazer and McGuire have advocated optimal risk adjustment as a remedy for the problem that risk adjusters used in RE models are often imperfect signals of individuals’ true risk. This remedy can be illustrated with the following example. Let us assume that ‘age’ is included as a risk adjuster in the RE model, but true type ‘yes/no suffering from Parkinson’s disease’ is not. Although the two variables are correlated, age is an imperfect signal of ‘yes/no suffering from Parkinson’s disease’ since the correlation is not perfect. Consequently, conventional RE (in which RE payments are based on the expected expenses for risk adjusters included in the model) will undercompensate for Parkinson’s disease. This undercompensation provides insurers with incentives for risk selection, for instance by skimping on (quality of) services that are specifically used by people suffering from Parkinson’s disease. In order to reduce such incentives, Glazer and McGuire propose to overpay the high age groups. Thus, the concept of optimal risk adjustment is based on the correlation between risk adjusters included in the RE model and true risk (for which the model does not compensate explicitly).
A similarity between the idea of overpaying (this paper) and the concept of optimal risk adjustment is the principle that the RE payment for a morbidity group included in the RE model does not necessarily equal the mean actual expenses of that group (i.e. conventional risk adjustment). An important difference, however, is that the concept of overpaying is not based on the idea that risk adjusters (e.g. age) in the RE model are imperfect signals of true risk (e.g. Parkinson’s disease), but on the observation that risk adjusters in the RE model (e.g. PCG for Parkinson’s disease) are incomplete due to explicit restrictions (e.g. classification in PCG for Parkinson’s disease only if an individual has used ≥181 DDD of the relevant drugs).
Another difference concerns the criterion and information needed for determining the overpayment. Glazer and McGuire [7] propose to overpay risk adjusters in the RE model such that insurers are sufficiently compensated at the level of healthcare services at which insurers make decisions about resource allocation. For each healthcare service insurers should be compensated sufficiently for the total healthcare expenses of the group using that service, thereby avoiding incentives to skimp on (quality of) services specifically used by high-risk consumers. A difficulty for implementation of this approach may be that the level of healthcare services at which insurers make decisions about resource allocation is unknown to the regulator. In the concept of overpaying (this paper), the overpayment for a risk adjuster should be such that on average the entire group of individuals identified by the information underlying this risk adjuster (i.e. those classified by this risk adjuster—group X—plus those not classified due to explicit restrictions—group Y) is sufficiently compensated. Since explicit restrictions require availability of information for making a distinction between groups X and Y, we expect the data needed for applying the concept of overpaying is probably inherently available in existing databases.
Despite the differences between the concept of overpaying proposed in this paper and the concept of optimal risk adjustment proposed by Glazer and McGuire, they probably work in the same direction. The reason is that both measures generally increase RE payments for individuals classified as high risk in terms of the risk adjusters included in the RE model and decrease them for those classified as low risks in terms of these risk adjusters. More specifically, this means that RE payments will increase for the elderly and individuals scoring on morbidity indicators and decrease for the complementary groups. Given this pattern, it is interesting to mention that overpaying and optimal risk adjustment will probably improve compensation for many high-risk groups that are not explicitly included as risk adjusters in the RE model. This is illustrated by Table 6, which shows the effect of the overpayment (and underpayment) derived in our empirical illustration on the six groups from Table 2. The direction of the effects is clear: the increase in RE payment for morbidity adjusters does not only improve compensation for those with a self-reported chronic condition, but also for the other five groups. The simple explanation is that individuals classified in (one or more) morbidity classes of the RE model are likely to be overrepresented in (almost) any identifiable group of high-risk individuals that is not explicitly included in the RE model. Consequently, groups of high-risk individuals profit from overpaying morbidity adjusters since for them the total compensation from the RE model increases. The opposite holds for groups of low-risk individuals for whom the total compensation decreases.
Conclusion
Several morbidity adjusters used in risk equalization models are subject to explicit restrictions, since not all information with predictive value regarding healthcare expenses is considered appropriate for the purpose of risk equalization. In general, this could mean that a certain morbidity class (e.g. PCG for Parkinson’s disease) includes group X (individuals who used ≥181 DDD of the relevant drugs) but explicitly excludes group Y (individuals who used only 1–180 DDD of the relevant drugs). Under conventional risk equalization this implies that X will be sufficiently compensated, but Y will be undercompensated. As a result, group XY (all individuals who used the relevant drugs) will also be undercompensated. This paper proposed to reduce incentives for risk selection against XY by overpaying X to such an extent than the total group XY (as well as the complementary group Z) is sufficiently compensated. For meaningful real-world applications, three preconditions should be sufficiently fulfilled: (1) for groups X, Y and Z information must be available on population frequency and average expenses, (2) risk selection against XY (and in favor of Z) must be considered more likely/problematical than risk selection against Y (in favor of X), and (3) morbidity adjuster X should sufficiently fulfil the common criteria for risk adjusters such as appropriateness of incentives and feasibility. Given these preconditions, overpaying may be particularly useful for the Dutch PCGs.
Discussion
An open question is how to calculate the overpayment for morbidity adjusters. Eqs. (1– 4) allow calculating a ‘second-stage’ per person overpayment for individuals with morbidity adjuster X. With second-stage we mean that the overpayment is calculated after a first stage in which the risk equalization model is estimated and the predicted expenses are calculated. This approach has an important shortcoming: the sum of predicted healthcare expenses and the over/underpayment probably does not comply with the least-squares criterion on which most risk equalization models rely in the first stage. Moreover, the equations do not allow calculating multiple overpayments (e.g. separately for PCG-A and PCG-B) simultaneously. A promising measure to overcome these complications is to estimate risk equalization models by ‘constrained least-squares regression’ instead of ‘ordinary least-squares regression’. The former method allows constraining the estimated coefficients such that the over- or undercompensation of certain risk groups (e.g. XY) equals zero. Under this procedure the estimation of predicted costs and the calculation of the overpayment are integrated in a single-stage procedure. This results in a risk equalization model that hits the desired payment target (e.g. no under/overcompensation for XY) and complies with the least-squares criterion. This innovative method has been proposed and illustrated by McGuire et al. [9], though for other purposes than overpaying.
This paper has focused on the effects of overpaying on incentives for risk selection. From this perspective, overpaying a morbidity group (e.g. PCG for Parkinson’s disease) is interesting when risk selection against XY (all individuals who used the relevant drugs) is considered more likely/problematical than risk selection against Y (individuals who used the relevant drugs but stayed below the 181-DDD threshold) and in favor of X (individuals who reached the 181-DDD threshold). In most countries, however, the goal of risk equalization is not only to reduce incentives for risk selection but also to achieve a level playing field for insurers. From the latter perspective, a point of attention is to what extent the ratio of ‘the number of individuals in group X’ and ‘the number of individuals in group Y’ varies across insurers. Insurers for whom this ratio is relatively high would benefit more from overpaying than insurers for whom this ratio is relatively low. Ceteris paribus, overpaying would then distort the level playing field.
Overpaying morbidity adjusters because of explicit restrictions applied to these risk adjusters is just one motive for overpaying. Existing literature provides other motives. As discussed above, Glazer and McGuire [7] have proposed overpaying in order to directly mitigate incentives for skimping on (quality of) services that are specifically used by high-risk individuals. Jack [10] and Bijlsma et al. [11] have proposed overpaying in order to take into account differences in switching costs between low-risk and high-risk individuals. Further research is necessary to assess the compatibility of these different motives for overpaying.
Given the ideas presented in this paper, we believe it is a missed opportunity that in current risk equalization practices the information explicitly excluded from morbidity classifications is considered redundant. As far as this information contains additional predictive value regarding healthcare expenses, it can be used for the purpose of overpaying. In the Netherlands, for instance, prior-year utilization of less than 181 DDD of drugs relevant for the PCG ‘Parkinson’s disease’ does not play any role in the calculation of risk equalization payments. This is a pity since it contains valuable information on future healthcare expenses of individuals suffering from Parkinson’s disease. By using this information for overpaying the Parkinson-PCG, incentives for selection against the entire group suffering from Parkinson’s disease (as well as the incentives for selection in favor of the group not suffering from Parkinson’s disease) can be mitigated.
References
Federal register: Patient Protection and Affordable Care Act; HHS notice of benefit and payment parameters for 2014. Federal Register vol. 77, No. 236, December 7 (2012)
Buchner, F., Goepffarth, D., Wasem, J.: The new risk adjustment formula in Germany: implementation and first experiences. Health Policy 109, 253–262 (2013)
Van Kleef, R.C., Van Vliet, R.C.J.A., Van de Ven, W.P.M.M.: Risk equalization in the Netherlands: an empirical evaluation. Expert Rev. Pharmacoecon. Outcome Res. 13, 829–839 (2013)
Ellis, R.P., McGuire, T.G.: Predictability and predictiveness in health care spending. J. Health Econ. 26, 25–48 (2007)
Newhouse, J.P.: Reimbursing health plans and health providers: efficiency in production versus selection. J. Econ. Lit. 34, 1236–1263 (1996)
Glazer, J., McGuire, T.G.: Optimal risk adjustment in markets with adverse selection: an application to managed care. Am. Econ. Rev. 90, 1055–1071 (2000)
Glazer, J., McGuire, T.G.: Setting health plan premiums to ensure efficient quality in health care: minimum variance optimal risk adjustment. J. Public Econ. 84, 153–173 (2002)
Van de Ven, W.P.M.M., Ellis, R.P.: Risk adjustment in competitive health insurance markets. In: Culyer, A.J., Newhouse, J.P. (eds.) Handbook of health economics, pp. 755–845. North-Holland, Amsterdam (2000)
McGuire, T.G., Glazer, J., Newhouse, J.P., Normand, S.L., Shi, J., Sinaiko, A.D., Zuvekas, S.: Integrating risk adjustment and enrollee premiums in health plan payment. J. Health Econ. 32, 1263–1277 (2013)
Jack, W.: Optimal risk adjustment with adverse selection and spatial competition. J. Health Econ. 25, 908–926 (2006)
Bijlsma, M., Boone, J., Zwart, G.: Competition leverage: how the demand side affects optimal risk adjustment. RAND J. Econ. 45, 792–815 (2014)
Pope, G.C., Ellis, R.P., Ash, A.S., Liu, C.F., Ayanian, J.Z., Bates, D.W., Burstin, H., Iezzoni, L.I., Ingber, M.J.: Principal inpatient diagnostic cost group model for medicare risk adjustment. Health Care Financ. Rev. 21, 93–118 (2000)
Van Kleef, R.C., Van Vliet, R.C.J.A., Van Rooijen, E.M.: Diagnoses-based cost groups in the Dutch risk-equalization model: the effects of including outpatient diagnoses. Health Policy 115, 52–59 (2014)
Pope, G.C., Kautter, J., Ellis, R.P., Ash, A.S., Ayanian, J.Z., Lezzoni, L.I., Ingber, M.J., Levy, J.M., Robst, J.: Risk adjustment of medicare capitation payments using the CMS-HCC model. Health Care Financ. Rev. 25, 119–141 (2004)
Hughes, J.S., Averill, R.F., Eisenhandler, J., Goldfield, N.I., Muldoon, J., Neff, J.M., Gay, J.C.: Clinical Risk Groups (CRGs)—a classification system for risk-adjusted capitation-based payment and health care management. Med. Care 42, 81–90 (2004)
Kronick, R., Gilmer, T., Dreyfus, T., Lee, L.: Improving health-based payment for medicaid beneficiaries: chronic illness and disability payment system. Health Care Financ. Rev. 21, 29–64 (2000)
Prinsze, F.J., Van Vliet, R.C.J.A.: Health-based risk adjustment: improving the pharmacy-based cost group model by adding diagnostic cost groups. Inquiry 44, 469–480 (2007)
Zhao, Y., Ellis, R.P., Ash, A.S., Calabrese, D., Ayanian, J.Z., Slaugther, J.P., Weyuker, L., Bowen, B.: Measuring population health risks using inpatient diagnoses and outpatient pharmacy data. Health Serv. Res. 36, 180–193 (2001)
Lamers, L.M., Van Vliet, R.C.J.A.: The pharmacy-based cost group model: validating and adjusting the classification of medications for chronic conditions to the Dutch situation. Health Policy 68, 113–121 (2004)
Fishman, P.A., Goodman, M.J., Hornbrook, M.C., Meenan, R.T., Bachman, D.J., Rosetti, M.C.K.: Risk adjustment using automated ambulatory pharmacy data. The RxRisk model. Med. Care 41, 84–99 (2003)
Lamers, L.M., Van Vliet, R.C.J.A.: Health-based risk adjustment: improving the pharmacy-based cost group model to reduce gaming possibilities. Eur. J. Health Econ. 4, 107–114 (2003)
Van Kleef, R.C., Van Vliet, R.C.J.A.: Prior use of durable medical equipment as a risk adjuster for health-based capitation. Inquiry 47, 343–358 (2010)
Van Kleef, R.C., Van Vliet, R.C.J.A.: Improving risk equalization using multiple-year high cost as a health indicator. Med. Care 50, 140–144 (2012)
Ash, A., Porell, F., Gruenberg, L., Sawitz, E., Beiser, A.: Adjusting Medicare capitation payments using prior hospitalization data. Health Care Financ. Rev. 10, 17–29 (1989)
Ellis, R.P., Ash, A.S.: Refinements to the diagnostic cost group model. Inquiry 32, 1–12 (1995)
Ellis, R.P., Pope, G.C., Iezzoni, L.I., Ayanian, J.Z., Bates, D.W., Burstin, H., Ash, A.S.: Diagnosis-based risk adjustment for Medicare capitation payments. Health Care Financ. Rev. 17, 101–128 (1996)
Lamers, L.M.: Risk-adjusted capitation payments: developing a diagnostic cost groups classification for the Dutch situation. Health Policy 45, 15–32 (1998)
Kronick, R., Dreyfus, T., Lee, L., Zhou, Z.: Diagnostic risk adjustment for Medicaid: the disability payment system. Health Care Financ. Rev. 17, 7–33 (1996)
Clark, D.O., Von Korff, M., Saunders, K., Baluch, W.M., Simon, G.E.: A chronic disease score with empirically derived weights. Med. Care 33, 783–795 (1995)
Van Kleef R.C., Van Vliet R.C.J.A., Van de Ven W.P.M.M.: Risk equalization 2014: an empirical evaluation. Research report (in Dutch), Erasmus University Rotterdam (2014)
Ware, J.E., Kosinski, M., Keller, S.D.: A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med. Care 50, 140–144 (2012)
Acknowledgments
The authors gratefully acknowledge two anonymous reviewers, Thomas G. McGuire, Suzanne H.C.M. van Veen and the members of the Risk Adjustment Network for their valuable comments on earlier versions of this article. The responsibility for this article fully rests with the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
van Kleef, R.C., van Vliet, R.C.J.A. & van de Ven, W.P.M.M. Overpaying morbidity adjusters in risk equalization models. Eur J Health Econ 17, 885–895 (2016). https://doi.org/10.1007/s10198-015-0729-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-015-0729-2