Abstract
Background
Both frailty and chronic kidney disease (CKD) increase with age and share many similarities. Many studies have demonstrated an association between frailty and chronic kidney disease (CKD), but an association with dipstick proteinuria is limited.
Methods
This is the cross-sectional analysis of the Nambu Cohort Study at the beginning of observation. Frailty was diagnosed using Kihon Checklist. Logistic analysis was used to evaluate the association between frailty and CKD or dipstick proteinuria.
Results
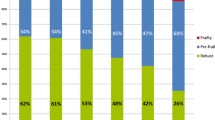
Among a total of 630 outpatients [age, 78 (70–84) years, men, 50%], the prevalence of patients with pre-frailty and frailty was 32% and 40%, respectively. The proportion of patients with pre-frailty and frailty increased with decreasing estimated glomerular filtration rate (eGFR) and increasing dipstick proteinuria levels. The odds ratios (95% confidence intervals) for CKD stage of 60 < eGFR ≤ 45 ml/min/1.73 m2, and 45 ml/min/1.73 m2 < eGFR for frailty was 0.87 (0.56–1.35) and 2.54 (1.46–4.53), respectively, compared with non-CKD as a reference. Furthermore, the odds ratios for the frailty of dipstick proteinuria with ± and + or over were 1.36 (0.88–2.09) and 1.78 (1.00–3.17), respectively, when dipstick proteinuria—was used as a reference. Moreover, the combination of eGFR and dipstick proteinuria levels increased the odds ratio for pre-frailty and frailty.
Conclusion
Elderly patients with CKD had a higher prevalence of pre-frailty and frailty. By adding urinary protein information to eGFR, the link between CKD and frailty becomes even more robust.




Similar content being viewed by others
References
Xue Q-L. The frailty syndrome: definition and natural history. Clin Geriatr Med. 2011;27:1–15.
Satake S, Shimokata H, Senda K, Kondo I, Toba K. Validity of total kihon checklist score for predicting the incidence of 3-year dependency and mortality in a community-dwelling older population. J Am Med Dir Assoc. 2017;18:552.e1-552.e6.
Yamada Y, Nanri H, Watanabe Y, Yoshida T, Yokoyama K, Itoi A, et al. Prevalence of frailty assessed by fried and kihon checklist indexes in a prospective cohort study: design and demographics of the Kyoto–Kameoka longitudinal study. J Am Med Dir Assoc. 2017;18:733.e7-733.e15.
Gale CR, Cooper C, Sayer AA. Prevalence of frailty and disability: findings from the English longitudinal study of ageing. Age Ageing. 2015;44:162–5.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56:M146–56.
Chowdhury R, Peel NM, Krosch M, Hubbard RE. Frailty and chronic kidney disease: a systematic review. Arch Gerontol Geriatr. 2017;68:135–42.
Roshanravan B, Khatri M, Robinson-Cohen C, Levin G, Patel KV, De Boer IH, et al. A prospective study of frailty in nephrology-referred patients with CKD. Am J Kidney Dis. 2012;60:912–21.
Odden MC, Chertow GM, Fried LF, Newman AB, Connelly S, Angleman S, et al. Cystatin C and measures of physical function in elderly adults: the health, aging, and body composition (HABC) study. Am J Epidemiol. 2006;164:1180–9.
Hiraki K, Yasuda T, Hotta C, Izawa KP, Morio Y, Watanabe S, et al. Decreased physical function in pre-dialysis patients with chronic kidney disease. Clin Exp Nephrol. 2013;17:225–31.
Hart A, Paudel ML, Taylor BC, Ishani A, Orwoll ES, Cawthon PM, et al. Cystatin C and frailty in older men. J Am Geriatr Soc. 2013;61:1530–6.
Ballew SH, Chen Y, Daya NR, Godino JG, Windham BG, McAdams-DeMarco M, et al. Frailty, kidney function, and polypharmacy: the atherosclerosis risk in communities (ARIC) study. Am J Kidney Dis. 2017;69:228–36.
Chang C-C, Hsu C-Y, Chang T-Y, Huang P-H, Liu L-K, Chen L-K, et al. Association between low-grade albuminuria and frailty among community-dwelling middle-aged and older people: a cross-sectional analysis from I-Lan Longitudinal Aging Study. Sci Rep. 2016;6:39434.
Levey AS, de Jong PE, Coresh J, El Nahas M, Astor BC, Matsushita K, et al. The definition, classification, and prognosis of chronic kidney disease: a KDIGO controversies conference report. Kidney Int. 2011;80:17–28.
Iseki K, Ikemiya Y, Iseki C, Takishita S. Proteinuria and the risk of developing end-stage renal disease. Kidney Int. 2003;63:1468–74.
Iseki K, Konta T, Asahi K, Yamagata K, Fujimoto S, Tsuruya K, et al. Dipstick proteinuria and all-cause mortality among the general population. Clin Exp Nephrol. 2018;22:1331–40.
Matsuoka M, Inoue T, Shinjo T, Miiji A, Tamashiro M, Oba K, et al. Cardiovascular risk profile and frailty in Japanese outpatients: the Nambu Cohort Study. Hypertens Res. 2020;43:817–23.
Satake S, Senda K, Hong Y-J, Miura H, Endo H, Sakurai T, et al. Validity of the Kihon Checklist for assessing frailty status. Geriatr Gerontol Int. 2016;16:709–15.
Dalrymple LS, Katz R, Rifkin DE, Siscovick D, Newman AB, Fried LF, et al. Kidney function and prevalent and incident frailty. Clin J Am Soc Nephrol. 2013;8:2091–9.
Walker SR, Gill K, Macdonald K, Komenda P, Rigatto C, Sood MM, et al. Association of frailty and physical function in patients with non-dialysis CKD: a systematic review. BMC Nephrol. 2013;14:228.
Iseki K, Iseki C, Ikemiya Y, Fukiyama K. Risk of developing end-stage renal disease in a cohort of mass screening. Kidney Int. 1996;49:800–5.
Ferrucci L, Fabbri E. Inflammageing: chronic inflammation in ageing, cardiovascular disease, and frailty. Nat Rev Cardiol. 2018;15:505–22.
Stepanova M, Rodriguez E, Birerdinc A, Baranova A. Age-independent rise of inflammatory scores may contribute to accelerated aging in multi-morbidity. Oncotarget. 2015;6:1414–21.
Avesani CM, Carrero JJ, Axelsson J, Qureshi AR, Lindholm B, Stenvinkel P. Inflammation and wasting in chronic kidney disease: partners in crime. Kidney Int. 2006;70:S8–13.
Fraser SDS, Roderick PJ, May CR, McIntyre N, McIntyre C, Fluck RJ, et al. The burden of comorbidity in people with chronic kidney disease stage 3: a cohort study. BMC Nephrol. 2015;16:193.
Justice JN, Gregory H, Tchkonia T, Lebrasseur NK, Kirkland JL, Kritchevsky SB, et al. Cellular senescence biomarker p16 INK4a + cell burden in thigh adipose is associated with poor physical function in older women. J Gerontol—Ser A Biol Sci Med Sci. 2018;73:939–45.
Andrassy KM. KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease’. Kidney Intern. 2013;84:622–3.
Upadhyay A, Larson MG, Guo CY, Vasan RS, Lipinska I, O’Donnell CJ, et al. Inflammation, kidney function and albuminuria in the Framingham Offspring cohort. Nephrol Dial Transpl. 2011;26:920–6.
Landi F, Marzetti E, Liperoti R, Pahor M, Russo A, Martone AM, et al. Nonsteroidal anti-inflammatory drug (NSAID) use and sarcopenia in older people: Results from the ilsirente study. J Am Med Dir Assoc. 2013;14:626.e9-626.e13.
Wang C-PP, Lorenzo C, Habib SL, Jo B, Espinoza SE. Differential effects of metformin on age related comorbidities in older men with type 2 diabetes HHS Public Access. J Diabetes Complicat. 2017;31:679–86.
Laksmi PW, Setiati S, Tamin TZ, Soewondo P, Rochmah W, Nafrialdi N, et al. Effect of metformin on handgrip strength, gait speed, myostatin serum level, and health-related quality of life: a double blind randomized controlled trial among non-diabetic pre-frail elderly patients. Acta Med Indones. 2017;49:118–27.
Ofori-Asenso R, Chin KL, Mazidi M, Zomer E, Ilomaki J, Zullo AR, et al. Global Incidence of Frailty and Prefrailty Among Community-Dwelling Older Adults: A Systematic Review and Meta-analysis. JAMA Netw open 2019; 2:e198398.
Acknowledgements
The authors are grateful to Ms. Makiko. Chinen, Ms. Masae Toma, Ms. Mitsue Nakajo, Ms. Asuka Kina, Ms. Minako Kikuyama, Ms. Megumi Ishiki, Ms. Mizuki Ohkata, Ms. Miwa Sunagawa, Ms. Minako Yamaniha, Ms. Masami Fukuyama, Ms. Minatsu Yamashiro, Ms. Megumi Kawabata, Ms. Sawako Sakugawa, Ms. Yuka Shimazaki, Ms. Kaori Unten, Ms. Mitsue Kuwae, Ms. Shoko Nagamine, Ms. Aya Henzan, Ms. Sayuri Matsumura, Ms. Yuko Kohno, Ms. Yoko Karakasa, Ms. Rie Kubota and Dr. Asuka Miiji for their dedicated work, and Mr. Makoto Ohmine for retrieving the data. Furthermore, the authors would like to thank Prof. Kunitoshi Iseki, Dr. Kazufumi Nagahama, and Dr. Masako Kochi for their valuable advice on the preparation of this paper. Finally, the authors extend their sincere appreciation to Mr. Kazuhide Nizato and Ms. Kuniko Inoue for their dedicated assistance.
Funding
The author(s) received no financial support for the research, authorship, and / or publication of this article.
Author information
Authors and Affiliations
Contributions
TI, TS, and MM participated in study design. TI drafted the manuscript. TI and HA performed the statistical analysis. MT, KO, TM, and OA participated in study coordination. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All the authors have declared no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Inoue, T., Shinjo, T., Matsuoka, M. et al. The association between frailty and chronic kidney disease; cross-sectional analysis of the Nambu Cohort Study. Clin Exp Nephrol 25, 1311–1318 (2021). https://doi.org/10.1007/s10157-021-02110-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-021-02110-y