Abstract
Background
Although peritoneal dialysis (PD) is becoming more widespread, PD among diabetic patients carries some concerns, such as worsened glycemic control due to constant exposure to glucose and operational errors due to diabetic complications. However, several technical advances could overcome these disadvantages. We, therefore, aimed to compare technical and patient survival between diabetic and non-diabetic PD patients.
Methods
We conducted a historical cohort study of 103 patients (mean age, 57 ± 16 years; 75 males, 32 diabetic patients) who started PD between January 2011 and January 2016. Kaplan–Meier survival analysis was used to compare technical and patient survivals between diabetic and non-diabetic patients. Multivariate Cox regression analysis was used to estimate the effects of the presence of diabetes on these outcomes.
Results
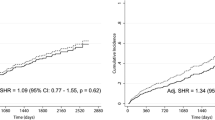
Technical and patient survivals did not differ significantly between groups (P = 0.62, P = 0.34, respectively). In addition, presence of diabetes affected neither technical nor patient survival in multivariate analysis (hazard ratio [HR], 1.31; 95% confidence interval [CI], 0.58–2.82 and HR 0.80; 95% CI 0.22–2.68, respectively).
Conclusions
Technical and patient survivals of diabetic PD patients were not inferior to those of non-diabetic PD patients. These results suggest that no hesitation is warranted in initiating PD for diabetic patients with end-stage renal disease.

Similar content being viewed by others
References
Nakai S, Hanafusa N, Masakane I, Taniguchi M, Hamano T, Shoji T, et al. An overview of regular dialysis treatment in Japan (as of 31 December 2012). Ther Apher Dial. 2014;18(6):535–602. https://doi.org/10.1111/1744-9987.12281.
Lei Y, Xiong Y, Zhang L, Yan H, Li Z, Cao L, et al. Comparison of long-term outcomes between peritoneal dialysis patients with diabetes as a primary renal disease or as a comorbid condition. PLoS One. 2015;10(5):e0126549. https://doi.org/10.1371/journal.pone.0126549.
Ozener C, Arikan H, Karayaylali I, Utas C, Bozfakioglu S, Akpolat T, et al. The impact of diabetes mellitus on peritoneal dialysis: the Turkey Multicenter Clinic Study. Renal failure. 2014;36(2):149–53. https://doi.org/10.3109/0886022X.2013.843275.
Fang W, Yang X, Kothari J, Khandelwal M, Naimark D, Jassal SV, et al. Patient and technique survival of diabetics on peritoneal dialysis: one-center’s experience and review of the literature. Clin Nephrol. 2008;69(3):193–200.
Wu B, Wang M, Zhao H. Survival rates in patients with diabetes on peritoneal dialysis in China. Ren Fail. 2013;35(2):231–4. https://doi.org/10.3109/0886022X.2012.747132.
Chow KM, Szeto CC, Leung CB, Kwan BC, Law MC, Li PK. A risk analysis of continuous ambulatory peritoneal dialysis-related peritonitis. Perit Dial Int. 2005;25(4):374–9.
Oo TN, Roberts TL, Collins AJ. A comparison of peritonitis rates from the United States renal data system database: CAPD versus continuous cycling peritoneal dialysis patients. Am J Kidney Dis. 2005;45(2):372–80.
Han SH, Lee SC, Ahn SV, Lee JE, Kim DK, Lee TH, et al. Reduced residual renal function is a risk of peritonitis in continuous ambulatory peritoneal dialysis patients. Nephrol Dial Transplant. 2007;22(9):2653–8. https://doi.org/10.1093/ndt/gfm242.
Couchoud C, Bolignano D, Nistor I, Jager KJ, Heaf J, Heimburger O, et al. Dialysis modality choice in diabetic patients with end-stage kidney disease: a systematic review of the available evidence. Nephrol Dial Transplant. 2015;30(2):310–20. https://doi.org/10.1093/ndt/gfu293.
See EJ, Johnson DW, Hawley CM, Pascoe EM, Badve SV, Boudville N, et al. Risk predictors and causes of technique failure within the first year of peritoneal dialysis: an Australia and New Zealand dialysis and transplant registry (ANZDATA) study. Am J Kidney Dis. 2017. https://doi.org/10.1053/j.ajkd.2017.10.019.
Li PK, Szeto CC, Piraino B, de Arteaga J, Fan S, Figueiredo AE, et al. ISPD peritonitis recommendations: 2016 update on prevention and treatment. Perit Dial Int. 2016;36(5):481–508. https://doi.org/10.3747/pdi.2016.00078.
Mehrotra R, Kermah D, Fried L, Kalantar-Zadeh K, Khawar O, Norris K, et al. Chronic peritoneal dialysis in the United States: declining utilization despite improving outcomes. J Am Soc Nephrol. 2007;18(10):2781–8. https://doi.org/10.1681/ASN.2006101130.
Frampton JE, Plosker GL. Icodextrin: a review of its use in peritoneal dialysis. Drugs. 2003;63(19):2079–105.
Posthuma N, ter Wee PM, Donker AJ, Oe PL, Peers EM, Verbrugh HA. Assessment of the effectiveness, safety, and biocompatibility of icodextrin in automated peritoneal dialysis. The Dextrin in APD in Amsterdam (DIANA) Group. Perit Dial Int. 2000;20(Suppl 2):106-13.
Paniagua R, Ventura MD, Avila-Diaz M, Cisneros A, Vicente-Martinez M, Furlong MD, et al. Icodextrin improves metabolic and fluid management in high and high-average transport diabetic patients. Perit Dial Int. 2009;29(4):422–32.
Takatori Y, Akagi S, Sugiyama H, Inoue J, Kojo S, Morinaga H, et al. Icodextrin increases technique survival rate in peritoneal dialysis patients with diabetic nephropathy by improving body fluid management: a randomized controlled trial. Clin J Am Soc Nephrol. 2011;6(6):1337–44. https://doi.org/10.2215/CJN.10041110.
Bredie SJ, Bosch FH, Demacker PN, Stalenhoef AF, van Leusen R. Effects of peritoneal dialysis with an overnight icodextrin dwell on parameters of glucose and lipid metabolism. Perit Dial Int. 2001;21(3):275–81.
Lin A, Qian J, Li X, Yu X, Liu W, Sun Y, et al. Randomized controlled trial of icodextrin versus glucose containing peritoneal dialysis fluid. Clin J Am Soc Nephrol. 2009;4(11):1799–804. https://doi.org/10.2215/CJN.02950509.
Li PK, Culleton BF, Ariza A, Do JY, Johnson DW, Sanabria M, et al. Randomized, controlled trial of glucose-sparing peritoneal dialysis in diabetic patients. J Am Soc Nephrol. 2013;24(11):1889–900. https://doi.org/10.1681/ASN.2012100987.
Nessim SJ, Perl J, Bargman JM. The renin-angiotensin-aldosterone system in peritoneal dialysis: is what is good for the kidney also good for the peritoneum? Kidney Int. 2010;78(1):23–8. https://doi.org/10.1038/ki.2010.90.
Shen JI, Saxena AB, Montez-Rath ME, Chang TI, Winkelmayer WC. Angiotensin-converting enzyme inhibitor/angiotensin receptor blocker use and cardiovascular outcomes in patients initiating peritoneal dialysis. Nephrol Dial Transplant. 2017;32(5):862–9. https://doi.org/10.1093/ndt/gfw053.
Fang W, Oreopoulos DG, Bargman JM. Use of ACE inhibitors or angiotensin receptor blockers and survival in patients on peritoneal dialysis. Nephrol Dial Transplant. 2008;23(11):3704–10. https://doi.org/10.1093/ndt/gfn321.
Kolesnyk I, Noordzij M, Dekker FW, Boeschoten EW, Krediet RT. A positive effect of AII inhibitors on peritoneal membrane function in long-term PD patients. Nephrol Dial Transplant. 2009;24(1):272–7. https://doi.org/10.1093/ndt/gfn421.
Suzuki H, Kanno Y, Sugahara S, Okada H, Nakamoto H. Effects of an angiotensin II receptor blocker, valsartan, on residual renal function in patients on CAPD. Am J Kidney Dis. 2004;43(6):1056–64.
Nakao M, Yamamoto I, Maruyama Y, Nakashima A, Matsuo N, Tanno Y, et al. 33 Years of peritoneal dialysis-associated peritonitis: a single-Center Study in Japan. Ther Apher Dial. 2016;20(1):60–5. https://doi.org/10.1111/1744-9987.12372.
Yamagata K, Nakai S, Iseki K, Tsubakihara Y, Committee of Renal Data Registry of the Japanese Society for Dialysis T. Late dialysis start did not affect long-term outcome in Japanese dialysis patients: long-term prognosis from Japanese Society for [corrected] Dialysis Therapy Registry. Ther Apher Dial. 2012;16(2):111–20. https://doi.org/10.1111/j.1744-9987.2011.01052.x.
Lee MJ, Kwon YE, Park KS, Kee YK, Yoon CY, Han IM, et al. Glycemic control modifies difference in mortality risk between hemodialysis and peritoneal dialysis in incident dialysis patients with diabetes: results from a nationwide prospective cohort in Korea. Medicine. 2016;95(11):e3118. https://doi.org/10.1097/MD.0000000000003118.
Acknowledgements
We gratefully acknowledge the support and participation of the patients in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Y.M. and M.I. have received scholarship funds from Baxter International, Inc. and Terumo Corporation. Y.T. has received research grants from Baxter International, Inc. No sources of funding had any direct involvement in the design or conduct of the study; the collection, management, analysis, or interpretation of data; or the preparation, review, or approval of the manuscript. No other authors have any conflicts of interest to declare.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee at which the studies were conducted (IRB approval number 29–286 (8902)) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Written informed consent was not required because of the non-intervention and retrospective chart review design. We provided all individual participants a means to opt out in this study.
About this article
Cite this article
Kishida, K., Maruyama, Y., Asari, K. et al. Clinical outcome of incident peritoneal dialysis patients with diabetic kidney disease. Clin Exp Nephrol 23, 409–414 (2019). https://doi.org/10.1007/s10157-018-1646-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-018-1646-3