Abstract
Background
Video-assisted anal fistula treatment (VAAFT) has gained increasing acceptance as a sphincter-sparing procedure for treating complex anorectal fistulas (CAF), but no unequivocal conclusions can yet be drawn regarding its ultimate effectiveness. We reviewed the literature and performed a meta-analysis to evaluate the efficacy and safety of VAAFT in CAF patients.
Methods
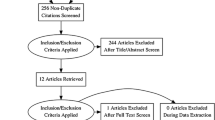
The study protocol was registered with the PROSPERO database (CRD42021279085). A systematic literature search was performed in the PubMed, Embase, and Cochrane Library databases up to June 2021 with no restriction on language based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. We used the keywords video-assisted surgery, video-assisted anal fistula treatment, and complex anorectal fistula to identify relevant studies.
Results
Fourteen trials (7 prospective and 7 retrospective) with a total of 1201 patients (mean age 43.5 years) were included. The median follow-up duration was 16.5(8–48) months. Pooled analysis showed that the rates of success, recurrence and postoperative complication across the studies were 83% (95% CI 81–85%, I2 = 37.9%), 16% (95% CI 14–18%, I2 = 4.8%), 11% (95% CI 7–15%, I2 = 72.1%), respectively. The postoperative Jorge–Wexner score used to assess the level of anal incontinence was 1.09 (95% CI, 0.9–1.27, I2 = 74.6%). The internal opening detection rate was 97.6% (95% CI 96.1–99.6%, I2 = 48.2%). Recurrence rates varied according to the closure method of internal opening from 21.4% after using staplers, 18.7% after suturing, to 23.5% after advancement flap. The hospital stay was 3.15 days (95% CI 2.96–3.35, I2 = 49.7%). Subgroup analysis indicated that the risk of heterogeneity in the urine retention group was higher compared with that of the overall group and that retrospective studies may be the source of heterogeneity for postoperative anal incontinence. r . Sensitivity analysis confirmed the stability of the pooled results. Begg's and Egger’s tests showed no evidence of publication bias.
Conclusions
According to the available evidence, VAAFT may be a valuable alternative to fistulotomy or seton in treating CAF and has the additional long-term benefits of reducing anal incontinence and surgical morbidity, permitting earlier healing and accelerated rehabilitation.








Similar content being viewed by others
References
Chaveli Diaz C, Esquiroz Lizaur I, Marzo Virto J, Oteiza Martinez F, Gonzalez Alvarez G, de Miguel VM et al (2021) Fistulectomy and endorectal advancement flap repair for cryptoglandular anal fistula: recurrence and functional outcome over 10 years of follow-up. Int J Colorectal Dis 36:841–846. https://doi.org/10.1007/s00384-021-03867-0
Jordan J, Roig JV, Garcia-Armengol J, Garcia-Granero E, Solana A, Lledo S (2010) Risk factors for recurrence and incontinence after anal fistula surgery. Colorectal Dis 12:254–260. https://doi.org/10.1111/j.1463-1318.2009.01806.x
Mei Z, Li Y, Wang Q, Shao Z, Du P, Zhu J et al (2021) Risk factors for postoperative recurrence of anal fistula identified by an international, evidence-based Delphi consultation survey of surgical specialists. Int J Surg 92:106038. https://doi.org/10.1016/j.ijsu.2021.106038
Ratto C, Litta F, Donisi L, Parello A (2015) Fistulotomy or fistulectomy and primary sphincteroplasty for anal fistula (FIPS): a systematic review. Tech Coloproctol 19:391–400. https://doi.org/10.1007/s10151-015-1323-4
Limura E, Giordano P (2015) Modern management of anal fistula. World J Gastroenterol 21:12–20. https://doi.org/10.3748/wjg.v21.i1.12
Regusci L, Fasolini F, Meinero P, Caccia G, Ruggeri G, Serati M et al (2020) Video-assisted anal fistula treatment (VAAFT) for complex anorectal fistula: efficacy and risk factors for failure at 3-year follow-up. Tech Coloproctol 24:741–746. https://doi.org/10.1007/s10151-020-02213-w
Dige A, Hougaard HT, Agnholt J, Pedersen BG, Tencerova M, Kassem M et al (2019) Efficacy of injection of freshly collected autologous adipose tissue into perianal fistulas in patients with Crohn’s disease. Gastroenterology 156(2208–16):e1. https://doi.org/10.1053/j.gastro.2019.02.005
Aho Falt U, Zawadzki A, Starck M, Bohe M, Johnson LB (2021) Long-term outcome of the Surgisis((R)) (Biodesign((R)) ) anal fistula plug for complex cryptoglandular and Crohn’s fistulas. Colorectal Dis 23:178–185. https://doi.org/10.1111/codi.15429
Kotze PG, Shen B, Lightner A, Yamamoto T, Spinelli A, Ghosh S et al (2018) Modern management of perianal fistulas in Crohn’s disease: future directions. Gut 67:1181–1194. https://doi.org/10.1136/gutjnl-2017-314918
Tao Y, Zheng Y, Han J, Wang Z, Cui J, Zhao B et al (2020) Long-term clinical results of use of an anal fistula plug for treatment of low trans-sphincteric anal fistulas. Med Sci Monit 26:e928181. https://doi.org/10.12659/msm.928181
Alasari S, Kim N (2014) Overview of anal fistula and systematic review of ligation of the intersphincteric fistula tract (LIFT). Tech Coloproctol 18:13–22. https://doi.org/10.1007/s10151-013-1050-7
Emile S, Khan S, Adejumo A, Koroye O (2020) Ligation of intersphincteric fistula tract (LIFT) in treatment of anal fistula: an updated systematic review, meta-analysis, and meta-regression of the predictors of failure. Surgery 167:484–492. https://doi.org/10.1016/j.surg.2019.09.012
Madbouly K, Emile S, Issa Y, Omar W (2021) Ligation of intersphincteric fistula tract (LIFT) with or without injection of platelet-rich plasma (PRP) in management of high trans-sphincteric fistula-in-ano: Short-term outcomes of a prospective, randomized trial. Surgery 170:61–66. https://doi.org/10.1016/j.surg.2020.12.025
Giamundo P, De Angelis M (2021) Treatment of anal fistula with FiLaC: results of a 10-year experience with 175 patients. Tech Coloproctol 25:941–948. https://doi.org/10.1007/s10151-021-02461-4
Marref I, Spindler L, Aubert M, Lemarchand N, Fathallah N, Pommaret E et al (2019) The optimal indication for FiLaC is high trans-sphincteric fistula-in-ano: a prospective cohort of 69 consecutive patients. Tech Coloproctol 23:893–897. https://doi.org/10.1007/s10151-019-02077-9
Meinero P, Mori L (2011) Video-assisted anal fistula treatment (VAAFT): a novel sphincter-saving procedure for treating complex anal fistulas. Tech Coloproctol 15:417–422. https://doi.org/10.1007/s10151-011-0769-2
Shamseer L, Moher D, Clarke M, Ghersi D, Liberati A, Petticrew M et al (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ (Clinical Research Ed) 350:g7647. https://doi.org/10.1136/bmj.g7647
Parks A, Gordon P, Hardcastle J (1976) A classification of fistula-in-ano. Br J Surg 63:1–12. https://doi.org/10.1002/bjs.1800630102
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605. https://doi.org/10.1007/s10654-010-9491-z
McGrath S, Zhao X, Steele R, Thombs B, Benedetti A (2020) Estimating the sample mean and standard deviation from commonly reported quantiles in meta-analysis. Stat Methods Med Res. https://doi.org/10.1177/0962280219889080
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135. https://doi.org/10.1186/1471-2288-14-135
Giarratano G, Shalaby M, Toscana C, Sileri P (2020) Video-assisted anal fistula treatment for complex anal fistula: a long-term follow-up study. Colorectal Dis 22:939–944. https://doi.org/10.1111/codi.15005
Romaniszyn M, Walega P (2017) Video-assisted anal fistula treatment: pros and cons of this minimally invasive method for treatment of perianal fistulas. Gastroenterol Res Pract 2017:9518310. https://doi.org/10.1155/2017/9518310
Wanitsuwan W, Junmitsakul K, Jearanai S, Lohsiriwat V (2020) Video-assisted ligation of intersphincteric fistula tract for complex anal fistula: technique and preliminary outcomes. Dis Colon Rectum 63:1534–1540. https://doi.org/10.1097/dcr.0000000000001691
Wu Y, Zheng B, Chen Q, Chen X, Ye S, Lin Q et al (2020) Video-assisted modified ligation of the intersphincteric fistula tract, an integration of 2 minimally invasive techniques for the treatment of parks type II anal fistulas. Surg Innov. https://doi.org/10.1177/1553350620978026
Zelić M, Karlović D, Kršul D, Bačić Đ, Warusavitarne J (2020) Video-assisted anal fistula treatment for treatment of complex cryptoglandular anal fistulas with 2 years follow-up period: our experience. J Laparoendosc Adv Surg Tech A 30:1329–1333. https://doi.org/10.1089/lap.2020.0231
Zhang Y, Li F, Zhao T, Cao F, Zheng Y, Li A (2020) Efficacy of video-assisted anal fistula treatment combined with closure of the internal opening using a stapler for Parks II anal fistula. Ann Trans Med. https://doi.org/10.21037/atm-20-7154
Chase T, Quddus A, Selvakumar D, Cunha P, Cuming T (2021) VAAFT for complex anal fistula: a useful tool, however, cure is unlikely. Tech Coloproctol. https://doi.org/10.1007/s10151-021-02492-x
Jiang H, Liu H, Li Z, Xiao Y, Li A, Chang Y et al (2017) Video-assisted anal fistula treatment (VAAFT) for complex anal fistula: a preliminary evaluation in China. Med Sci Monit 23:2065–2071. https://doi.org/10.12659/msm.904055
Liu H, Tang X, Chang Y, Li A, Li Z, Xiao Y et al (2020) Comparison of surgical outcomes between video-assisted anal fistula treatment and fistulotomy plus seton for complex anal fistula: a propensity score matching analysis—retrospective cohort study. Int J Surg 75:99–104. https://doi.org/10.1016/j.ijsu.2020.01.137
Meinero P, Mori L, Gasloli G (2014) Video-assisted anal fistula treatment: a new concept of treating anal fistulas. Dis Colon Rectum 57:354–359. https://doi.org/10.1097/dcr.0000000000000082
Stazi A, Izzo P, D’Angelo F, Radicchi M, Mazzi M, Tomassini F et al (2018) Video-assisted anal fistula treatment in the management of complex anal fistula: a single-center experience. Minerva Chir 73:142–150. https://doi.org/10.23736/s0026-4733.18.07390-x
Zhang Y, Li F, Zhao T, Cao F, Zheng Y, Li A (2021) Treatment of complex anal fistula by video-assisted anal fistula treatment combined with anal fistula plug: a single-center study. Surg Innov. https://doi.org/10.1177/1553350621992924
Zhang Y, Li F, Zhao T, Cao F, Zheng Y, Li A (2021) Video-assisted anal fistula treatment combined with anal fistula plug for treatment of horseshoe anal fistula. J Int Med Res 49:300060520980525. https://doi.org/10.1177/0300060520980525
Adegbola S, Sahnan K, Pellino G, Tozer P, Hart A, Phillips R et al (2017) Short-term efficacy and safety of three novel sphincter-sparing techniques for anal fistulae: a systematic review. Tech Coloproctol 21:775–782. https://doi.org/10.1007/s10151-017-1699-4
Jayne D, Scholefield J, Tolan D, Gray R, Senapati A, Hulme C et al (2021) A multicenter randomized controlled trial comparing safety, efficacy, and cost-effectiveness of the surgisis anal fistula plug versus surgeon’s preference for transsphincteric fistula-in-Ano: the FIAT trial. Ann Surg 273:433–441. https://doi.org/10.1097/sla.0000000000003981
Zarin M, Khan M, Ahmad M, Ibrahim M, Khan M (2015) VAAFT: video assisted anal fistula treatment; bringing revolution in fistula treatment. Pakistan journal of medical sciences 31:1233–1235. https://doi.org/10.12669/pjms.315.6836
Liaqat N, Iqbal A, Dar S, Liaqat F (2016) Video assisted anal fistula treatment in a child with perianal fistula. J Case Rep 7:3
Pini Prato A, Zanaboni C, Mosconi M, Mazzola C, Muller L, Meinero P et al (2016) Preliminary results of video-assisted anal fistula treatment (VAAFT) in children. Tech Coloproctol 20:279–285. https://doi.org/10.1007/s10151-016-1447-1
Emile S, Elfeki H, Thabet W, Sakr A, Magdy A, El-Hamed T et al (2017) Predictive factors for recurrence of high transsphincteric anal fistula after placement of seton. J Surg Res 213:261–268. https://doi.org/10.1016/j.jss.2017.02.053
Kochhar G, Saha S, Andley M, Kumar A, Saurabh G, Pusuluri R et al (2014) Video-assisted anal fistula treatment. J Soc Laparoendosc Surg. https://doi.org/10.4293/jsls.2014.00127
Abcarian H (2011) Anorectal infection: abscess-fistula. Clin Colon Rectal Surg 24:14–21. https://doi.org/10.1055/s-0031-1272819
Ommer A, Herold A, Berg E, Fürst A, Sailer M, Schiedeck T (2011) Cryptoglandular anal fistulas. Deutsch Arztebl Int 108:707–713. https://doi.org/10.3238/arztebl.2011.0707
Chowbey P, Khullar R, Sharma A, Soni V, Najma K, Baijal M (2015) Minimally invasive anal fistula treatment (MAFT)-an appraisal of early results in 416 patients. Indian J Surg 77:716–721. https://doi.org/10.1007/s12262-013-0977-2
Funding
There has been no significant financial support for this work that could have influenced its outcome.
Author information
Authors and Affiliations
Contributions
Conceptualization: ZT, YL, SN, WX, YW. Data curation: ZT, YL. Methodology: ZT, YLi. Statistical analysis: ZT. Quality control of data and algorithms: ZT, YL, SN, WX, YW. Supervision: ZT, YW. Validation: ZT, YL. Manuscript—original draft: ZT. Manuscript—review & editing: ZT, YL, SN, WX, YW.
Corresponding author
Ethics declarations
Conflict of interest
The authors confirm there is no known conflict of interest associated with this publication.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tian, Z., Li, Y., Nan, S. et al. Video-assisted anal fistula treatment for complex anorectal fistulas in adults: a systematic review and meta-analysis. Tech Coloproctol 26, 783–795 (2022). https://doi.org/10.1007/s10151-022-02614-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-022-02614-z