Abstract
Purpose
Gangrenous cholecystitis (GC) is a severe type of acute cholecystitis that implies higher mortality and morbidity rates than uncomplicated cholecystitis. The characteristics of GC are various for each case. However, preoperative predictors of GC with extensive necrotic change have not been investigated well.
Methods
A total of 239 patients who were pathologically diagnosed with GC underwent laparoscopic cholecystectomy at our hospital between January 2013 and December 2021. Of these, 135 patients were included in this study and were subdivided into the extensive necrosis group (patients with necrotic change extending to the neck of the gallbladder, n = 18) and the control group (patients with necrotic change limited to the fundus or body, not extending to the neck, n = 117) according to each operation video. Patient characteristics and perioperative factors predicting extensive necrotic change were investigated.
Results
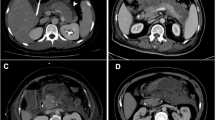
Pericholecystic fat stranding (83.3 vs. 53.8%, p = 0.018) and absence of wall enhancement on preoperative CT images (50.0 vs. 24.7%, p = 0.026) were significantly associated with extensive necrosis. Seven of 18 patients in the extensive necrosis group showed necrotic changes beyond the infundibulum. The absence of wall enhancement on preoperative CT images (71.4 vs. 28.8%, p = 0.018) was significantly associated with necrotic changes beyond the infundibulum.
Conclusions
Pericholecystic fat stranding and absence of wall enhancement on preoperative enhanced CT are predictors of extensive necrotic change in patients with GC. In addition, the absence of wall enhancement also predicts the presence of necrotic changes beyond the infundibulum.



Similar content being viewed by others
Data availability
Not applicable
Code availability
Not applicable
References
Önder A, Kapan M, Ülger BV, Oğuz A, Türkoğlu A, Uslukaya Ö (2015) Gangrenous cholecystitis: mortality and risk factors. Int Surg 100:254–260. https://doi.org/10.9738/INTSURG-D-13-00222.1
Ganapathi AM, Speicher PJ, Englum BR, Perez A, Tyler DS, Zani S (2015) Gangrenous cholecystitis: a contemporary review. J Surg Res. 197:18–24. https://doi.org/10.1016/j.jss.2015.02.058
Kirkwood R, Damon L, Wang J, Hong E, Kirkwood K (2017) Gangrenous cholecystitis: innovative laparoscopic techniques to facilitate subtotal fenestrating cholecystectomy when a critical view of safety cannot be achieved. Surg Endosc. 31:5258–5266. https://doi.org/10.1007/s00464-017-5599-5
Bennett GL, Rusinek H, Lisi V, Israel GM, Krinsky GA, Slywotzky CM, Megibow A (2002) CT findings in acute gangrenous cholecystitis. AJR Am J Roentgenol. 178:275–281. https://doi.org/10.2214/ajr.178.2.1780275
Singh AK, Sagar P (2005) Gangrenous cholecystitis: prediction with CT imaging. Abdom Imaging. 30:218–221. https://doi.org/10.1007/s00261-004-0217-0
Wu CH, Chen CC, Wang CJ, Wong YC, Wang LJ, Huang CC, Lo WC, Chen HW (2011) Discrimination of gangrenous from uncomplicated acute cholecystitis: accuracy of CT findings. Abdom Imaging. 36:174–178. https://doi.org/10.1007/s00261-010-9612-x
Chang WC, Sun Y, Wu EH, Kim SY, Wang ZJ, Huang GS, Yeh BM (2016) CT findings for detecting the presence of gangrenous ischemia in cholecystitis. AJR Am J Roentgenol. 207:302–309. https://doi.org/10.2214/AJR.15.15658
Maehira H, Itoh A, Kawasaki M, Ogawa M, Imagawa A, Mizumura N, Okumura S, Kameyama M (2016) Use of dynamic CT attenuation value for diagnosis of acute gangrenous cholecystitis. Am J Emerg Med. 34:2306–2309. https://doi.org/10.1016/j.ajem.2016.08.033
Uemura S, Higuchi R, Yazawa T, Izumo W, Sugishita T, Morita S, Yamamoto M (2019) Impact of transient hepatic attenuation differences on computed tomography scans in the diagnosis of acute gangrenous cholecystitis. J Hepatobiliary Pancreat Sci. 26:348–353. https://doi.org/10.1002/jhbp.637
Erlichman DB, Lipman JN, In H, Ye K, Lin J, Goldman I (2021) Diagnostic significance of the CT rim sign in cases of gangrenous cholecystitis. Clin Imaging. 73:53–56. https://doi.org/10.1016/j.clinimag.2020.11.052
Wu B, Buddensick TJ, Ferdosi H, Narducci DM, Sautter A, Setiawan L, Shaukat H, Siddique M, Sulkowski GN, Kamangar F, Kowdley GC, Cunningham SC (2014) Predicting gangrenous cholecystitis. HPB (Oxford). 16:801–806. https://doi.org/10.1111/hpb.12226
Mok KW, Reddy R, Wood F, Turner P, Ward JB, Pursnani KG, Date RS (2014) Is C-reactive protein a useful adjunct in selecting patients for emergency cholecystectomy by predicting severe/gangrenous cholecystitis? Int J Surg. 12:649–653. https://doi.org/10.1016/j.ijsu.2014.05.040
Bouassida M, Madhioub M, Kallel Y, Zribi S, Slama H, Mighri MM, Touinsi H (2021) Acute gangrenous cholecystitis: proposal of a score and comparison with previous published scores. J Gastrointest Surg. 25:1479–1486. https://doi.org/10.1007/s11605-020-04707-2
Khan SM, Emile SH, Barsom SH, Naqvi SAA, Khan MS (2021) Accuracy of pre-operative parameters in predicting severe cholecystitis-a systematic review. Surgeon. 19:219–225. https://doi.org/10.1016/j.surge.2020.06.010
Elshaer M, Gravante G, Thomas K, Sorge R, Al-Hamali S, Ebdewi H (2015) Subtotal cholecystectomy for “difficult gallbladders”: systematic review and meta-analysis. JAMA Surg. 150:159–168. https://doi.org/10.1001/jamasurg.2014.1219
Koo JGA, Chan YH, Shelat VG (2021) Laparoscopic subtotal cholecystectomy: comparison of reconstituting and fenestrating techniques. Surg Endosc. 35(3):1014–1024. https://doi.org/10.1007/s00464-020-08096-0
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 240:205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Kimura Y, Takada T, Kawarada Y, Nimura Y, Hirata K, Sekimoto M, Yoshida M, Mayumi T, Wada K, Miura F, Yasuda H, Yamashita Y, Nagino M, Hirota M, Tanaka A, Tsuyuguchi T, Strasberg SM, Gadacz TR (2007) Definitions, pathophysiology, and epidemiology of acute cholangitis and cholecystitis: Tokyo Guidelines. J Hepatobiliary Pancreat Surg. 14:15–26. https://doi.org/10.1007/s00534-006-1152-y
Adachi T, Eguchi S, Muto Y (2022) Pathophysiology and pathology of acute cholecystitis: a secondary publication of the Japanese version from 1992. J Hepatobiliary Pancreat Sci. 29:212–216. https://doi.org/10.1002/jhbp.912
Fagan SP, Awad SS, Rahwan K, Hira K, Aoki N, Itani KM, Berger DH (2003) Prognostic factors for the development of gangrenous cholecystitis. Am J Surg. 186:481–485. https://doi.org/10.1016/j.amjsurg.2003.08.001
Nikfarjam M, Niumsawatt V, Sethu A, Fink MA, Muralidharan V, Starkey G, Jones RM, Christophi C (2011) Outcomes of contemporary management of gangrenous and non-gangrenous acute cholecystitis. HPB (Oxford). 13:551–558. https://doi.org/10.1111/j.1477-2574.2011.00327.x
Altun E, Semelka RC, Elias J Jr, Braga L, Voultsinos V, Patel J, Balci NC, Woosley JT (2007) Acute cholecystitis: MR findings and differentiation from chronic cholecystitis. Radiology. 244:174–183. https://doi.org/10.1148/radiol.2441060920
Hwang H, Marsh I, Doyle J (2014) Does ultrasonography accurately diagnose acute cholecystitis? Improving diagnostic accuracy based on a review at a regional hospital. Can J Surg. 57(3):162–168. https://doi.org/10.1503/cjs.027312
Author information
Authors and Affiliations
Contributions
A.K. wrote the manuscript and performed data analysis. All authors contributed to acquire data and revise the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
This work was supported by departmental resources only, and the corresponding author is not a recipient of a research scholarship.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kohga, A., Suzuki, K., Okumura, T. et al. Prediction of extensive necrotic change in acute gangrenous cholecystitis. Emerg Radiol 29, 723–728 (2022). https://doi.org/10.1007/s10140-022-02055-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-022-02055-z