Abstract
Enterococcus faecalis is among the most resistant bacteria found in infected root canals. The demand for cutting-edge disinfection methods has rekindled research on photoinactivation with visible light. This study investigated the bactericidal activity of femtosecond laser irradiation against vancomycin-resistant Enterococcus faecalis V583 (VRE). The effect of parameters such as wavelength and energy density on the viability and growth kinetics of VRE was studied to design an optimized laser-based antimicrobial photoinactivation approach without any prior addition of exogenous photosensitizers. The most effective wavelengths were 430 nm and 435 nm at a fluence of 1000 J/cm2, causing a nearly 2-log reduction (98.6% and 98.3% inhibition, respectively) in viable bacterial counts. The colony-forming units and growth rate of the laser-treated cultures were progressively decreased as energy density or light dose increased at 445 nm but reached a limit at 1250 J/cm2. At a higher fluence of 2000 J/cm2, the efficacy was reduced due to a photobleaching phenomenon. Our results highlight the importance of optimizing laser exposure parameters, such as wavelength and fluence, in bacterial photoinactivation experiments. To our knowledge, this is the first study to report an optimized wavelength for the inactivation of VRE using visible femtosecond laser light.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The bacterium Enterococcus faecalis is widespread throughout the gastrointestinal tract, including the oral cavity [1]. It has been reported that E. faecalis is the most common microorganism found in infected root canals and in recurrent cases of apical periodontitis, with a prevalence ranging from 24–77% [2]. This is because E. faecalis can invade deeply into dentinal tubules and can resist intracanal disinfection procedures during routine endodontic treatment [3]. E. faecalis can survive in filled root canals without the support of any other bacteria [4]. Furthermore, E. faecalis is well-known for its resilience in the environment and can occur naturally in water sources such as rivers, lakes, and groundwater [5].
To prevent E. faecalis survival in dental settings and drinking water systems, proper disinfection control measures should be followed. In dentistry, irrigation with sodium hypochlorite, sterilization of dental instruments, using disposables when necessary, and adhering to stringent hand hygiene guidelines should all be standard practice. Sodium hypochlorite is used as the main irrigant during root canal therapy. However, it can be hazardous to the host cells of the periapical region if they come into contact [6, 7].
Vancomycin-resistant Enterococci (VRE) such as E. faecalis V583 are challenging to treat and can cause life-threatening infections, especially in immunocompromised individuals. Recently the spread of multidrug-resistant microorganisms in healthcare settings has become a serious threat to public health, so it is now urgent that new anti-infective strategies be discovered. Moreover, new methods of treating endodontic infections in periapical tissues are also needed [8].
In the search for new antibacterial technologies, light-based techniques have been the subject of much study [9]. Optical irradiation using visible-light wavelengths has been widely proposed as an antibacterial technique [10, 11]. Endoscopically administered light therapy has previously been used to treat gastric Helicobacter pylori infection [12], in the treatment of urinary tract infection in a rat model [13], and in controlling bacterial biofilm growth on catheter material [14].
One promising light candidate is femtosecond laser-based antimicrobial photoinactivation (aPI) [15,16,17,18,19], which is actively being investigated for the treatment of resistant microbes [20,21,22]. aPI is a widely accepted, simple, non-invasive, and inexpensive treatment method that causes minimal to no harm to host tissue [23]. Additionally, microbes are unlikely to develop resistance to aPI [24,25,26]. The term "laser-based aPI" refers to a process whereby reactive oxygen species (ROS) are produced without the addition of any exogenous photosensitizers (PS), but instead relies on naturally occurring PS within the bacteria. Mechanistically it is similar to antimicrobial photodynamic therapy (aPDT), which does require the addition of PS. Both approaches can be used to kill specific pathogens, using ROS produced through two simultaneously competing photochemical processes [27]. Type I involves electron transfer reactions producing reactive free radicals, while Type II involves an energy transfer reaction producing singlet oxygen (1O2) [28]. In both these procedures, light energy is transformed into chemical energy via the interaction of laser radiation with absorbing compounds [15]. The release of ROS inside the bacterial cells causes oxidative stress, which ultimately results in cell death [29].
These photochemical processes require an energy-absorbing platform known as a photosensitizer (PS). The correct wavelength and intensity of light can trigger photochemical and photophysical events inside the microbial cell by activating these PS molecules [30, 31]. As the technology behind pulsed laser systems evolves, it is possible to control more and more laser characteristics, including wavelength, power density, pulse duration, exposure time, energy density, and laser polarization, for specific applications. The major goal of all researchers in this field is to identify the optimal light wavelength, dose and fluence, for preventing bacterial growth and multiplication while minimizing adverse effects to host tissue.
It was previously believed that radiation in the 405–410 nm range was the most effective visible spectral region for the photoinactivation of microbes [32,33,34,35,36,37,38,39]. However, recent research has suggested that the 420–470 nm spectral range can also kill bacteria without the use of exogenous PS [40,41,42]. Nevertheless, the visible spectrum from 420 to 465 nm has not been thoroughly investigated.
Moreover, it's essential to highlight the unique advantages of femtosecond laser technology over LED light. Femtosecond lasers offer precise control over pulse duration, enabling targeted and efficient delivery of light energy to bacterial cells. This precise control is crucial for maximizing ROS generation while minimizing damage to surrounding host tissue. Furthermore, femtosecond lasers provide superior spatial and temporal resolution compared to LEDs, allowing for highly localized and rapid bacterial photoinactivation. This capability is particularly advantageous in clinical settings where precise targeting of microbial pathogens is essential for successful treatment outcomes. While LEDs may offer affordability and versatility, their broader emission spectra and less precise pulse control may limit their effectiveness for certain aPI applications. In contrast, femtosecond lasers provide a sophisticated platform for fine-tuning treatment parameters and optimizing bacterial photoinactivation [17, 18, 22].
To date, very few reports have identified the optimum femtosecond laser parameters that could kill bacterial pathogens, particularly VRE. Most reports have focused on targeting bacterial porphyrins with light in the range of 390–420 nm, which is not the case when dealing with E. faecalis which does not contain any free porphyrins, but where flavins are the main absorbing molecules that could be targeted [43].
Therefore, this work set out to examine to what extent femtosecond laser irradiation could eradicate VRE. To determine the optimal laser-based bactericidal parameters, the effect of varying wavelength and energy density on the growth kinetics and viability of VRE was examined in bacterial suspensions in vitro.
Materials and Methods
Microorganisms and culture conditions
In the present study, the infectious bacterial species, vancomycin-resistant Enterococcus faecalis V583 (ATCC 700802), was cultured in Brain Heart Infusion broth and incubated at 37° C for 18 h. 100 µL of the overnight bacterial suspension was diluted in 10 mL 0.9% NaCl to bring the turbidity down to 0.5 McFarland units. Laser irradiation was performed by transferring 200 µL aliquots of the diluted suspension, using sterile pipette tips, into individual wells of a 96 microtiter plate.
Preparation and installation of a laser system
Laser pulses were generated using a Spectra-Physics INSPIRE HF100 laser system, which was pumped by a mode-locked femtosecond Ti: sapphire MAI TAI HP laser, with 1.5–2.9 W average power, 80 MHz repetition rate, and wavelength range 690 to 1040 nm.
To achieve uniform interaction with the laser light, the bacterial suspensions were irradiated by positioning the laser beam about 10 cm above each well of a 96 well plate, as illustrated in Fig. 1.
A beam expander composed of two convergent lenses was used to increase the diameter of the original laser beam from 2 to 20 mm. An adjustable iris I was used to set the laser beam diameter at 6 mm, to match the diameter of each well of the microtiter plate, and a laser beam attenuator A was used to regulate the laser intensity delivered to the samples. As shown in Fig. 1, the laser beam was directed at the samples with the help of highly reflective mirrors M1 and M2. A Newport 843R power meter was used to determine the precise output of the laser.
The effect of varying laser irradiation parameters on E. faecalis
Horizontally polarised Gaussian laser pulses of 100 fs pulse duration and 80 MHz repetition rate were used to irradiate E. faecalis inoculated 96 well plates at a variety of wavelengths. A comprehensive analysis was conducted, comparing the viable bacterial counts, growth curves, and growth rate analysis of E. faecalis irradiated with 420, 425, 430, 440, 445, 452, 455, 460 and 465 nm, each at a constant energy density of 1000 J/cm2, to determine the most effective wavelengths. For the wavelengths of 420, 425, 430, 435, 440, and 445 nm, a higher energy density of 2000 J/cm2 was also explored. The effect of increasing energy density to potentiate the efficacy of the wavelength 445 nm was investigated using energy densities of 100, 250, 750, 1000, 1250, and 2000 J/ cm2.
Determining and analyzing growth kinetics
The plates were incubated at 37° C for 16 h after each treatment. Every 30 min during this incubation, the optical density of all the samples was measured at 620 nm using an FC Microplate reader (Thermo Fisher Scientific SN: 357–906,489). To track the development and proliferation of the bacteria over time, growth curves and maximum growth kinetics at specific time points (μmax) were plotted. Each experiment was conducted in triplicate under a laminar flow hood (Class II biological safety cabinet, MSC-Advantage). The following equation was used to obtain μmax:
(Xt is the growth absorbance at a specified time point; X0 is the initial growth absorbance; t is the time at which μmax obtained).
Viable bacterial counts and assessment of photoinactivation effect
To measure the number of viable bacteria, 100 μL of each control and femtosecond laser irradiated sample were serial tenfold diluted using tubes containing 900 μL of sterile 0.9% NaCl (up to 1:10,000,000 dilutions). Then, 0.1 mL of each dilution was immediately plated on nutrient agar. After incubating the plates at 37 °C in an aerobic environment for 24 h, the total number of bacteria was counted. Colony-forming unit (CFU) counts were used to determine bacterial viability in test and control samples, with results given as log CFU/mL or % CFU/mL compared to the control. All experiments were carried out in triplicate.
Statistical analysis and graphical representation
GraphPad Prism 7 was used for a one-way analysis of variance (ANOVA) test, followed by a Tukey test (P < 0.05 were considered significant), to compare the means of the treatment groups to those of the control group. Three independent runs of each experiment were conducted. Data visualization was plotted using GraphPad Prism 7 software.
Results and Discussion
E. faecalis, a type of Gram-positive bacteria commonly found in dentistry, is highly resilient, and is blamed for the failure of 67% of cases of root canal treatment, because these bacteria can withstand endodontic procedures and infiltrate the tiny channels within the tooth's structure known as dentinal tubules [44, 45]. To treat or prevent endodontic lesions, standard endodontic therapy focuses on lowering the microbial load within the root canal system. To better debride and cleanse the root canal system, various endodontic procedures employ chemo-mechanical treatment plus irrigation with disinfectants [46]. The most common solution used in endodontic treatment is sodium hypochlorite (NaOCl) because of its well-established efficacy against bacteria and other pathogens [47]. However, ecchymosis, tissue necrosis, and paresthesia are some of the unintended consequences of NaOCl use [48]. It has therefore been proposed that, rather than resorting to systemic antibiotics, it would be desirable to design a locally administered therapeutic agent with antibacterial activity that can reach into the dentinal tubules. Root canal bacteria could in theory be reduced or eliminated using laser technology in a way that is both noninvasive and effective [49, 50].
Visible light irradiation can be used to inactivate bacteria without the use of any chemical compounds, solvents, or other additives. Several different types of bacteria and fungi have been disclosed to be sensitive to this visible light disinfection technique. The use of light alone to kill microorganisms is known as antimicrobial photoinactivation (aPI) [51]. On the other hand, in antimicrobial photodynamic therapy (aPDT) a photosensitizer must be added from outside to allow the chemical reaction between light and oxygen to take place. Oxidative damage to the bacteria is caused by the ROS produced during this process [52]. aPI is advantageous since it kills bacteria without harming the host [51]. It has been observed that the usage of aPI within the visible light range results in rapid, effective, and locally targeted antibacterial action [23, 53], with little or no collateral impairment to the surrounding host tissue [23]. Consequently, the use of laser-based aPI for a variety of medicinal purposes is now being considered. Additionally, given the multi-target properties inherent in ROS, the probability of inducing bacterial resistance through aPI is lessened in comparison to antibiotics [54,55,56]. Compared to high-powered lasers, the cost of aPI is far lower, and the procedure itself is rapid and painless [57].
Few studies have shown that lasers were capable of eliminating E. faecalis completely [58, 59]. The efficacy of aPI is reliant on many aspects, comprising the spectral range of the light source and the ability of the PS inside the bacteria to absorb the radiation [60]. To maximize the effectiveness of aPI, optimizing the laser wavelength is critical.
In this study, vancomycin-resistant E. faecalis V583 was irradiated with femtosecond laser light tuned to different wavelengths between 420 and 465 nm initially at a fixed fluence of 1000 J/cm2 to determine the most effective wavelength to inactivate the bacteria. We employed VRE in this study, as a worst-case scenario, because the American Society for Microbiology (ASM) recommends using a strain that is exceptionally resistant compared to most bacteria when testing disinfection strategies such as femtosecond laser therapy [61]. To our knowledge, there are no studies available reporting the inactivation of VRE with visible light in the range of 420 – 465 nm. The irradiated bacteria were harvested from a stationary growth phase of an overnight culture because endogenous bacterial PS such as porphyrins or flavins are only produced at certain stages of the growth cycle (lag, exponential, or stationary), making the value of the aPI effect conditional on the stage of bacterial growth [10, 62].
Colony-forming units (CFU) were utilized to enumerate viable bacterial abundance in each sample, and the results were statistically compared. The viable bacterial count (CFU/mL) and the percentage of viable bacterial cells before and after laser irradiation at different wavelengths were plotted in (Figs. 2A and 2B). The highest effective wavelengths were 430 nm and 435 nm, causing nearly 2 log reduction (98.6% and 98.3% inhibition, respectively) of viable bacteria counts, and this is close to the ASM recommendation that a 99% reduction is needed in bactericidal testing [63]. Other researchers have adopted a 90% reduction in CFUs as a target value to be achieved using bactericidal radiation [33, 64,65,66].
The bar graph compares the control culture to bacterial cultures that were irradiated with different Laser parameters at ten specific wavelengths: 420, 425, 430, 435, 440, 445, 452, 455, 460, and 465 nm at a fixed fluence of 1000 J/cm2 in terms of (a) percentage CFU/mL, (b) log CFU/mL, and (c) the growth rate (μmax) during the logarithmic phase of growth. Statistical significance was determined through ANOVA followed by the Tukey test, with the level of significance indicated by asterisks: *** denotes highly significant (P < 0.001), ** denotes moderately significant (P < 0.01), * denotes low significance (P < 0.05), and "ns" represents not statistically significant
440 nm caused 85.6% decrease in viable bacteria counts. Other wavelengths caused a decrease in the viable bacterial counts, but these were not statistically significant. The percentage of killed bacteria treated with 445, 452, 455, 460 and 465 nm were 54.2%, 63.67%, 20.5%, 25.5% and 42%, respectively. Both 420 nm and 425 nm showed no bactericidal effects against E. faecalis.
Our findings are consistent with those of other groups who showed enhanced disinfection but did not observe complete eradication of bacteria (100%). Therefore, femtosecond lasers could be employed in conjunction with other disinfectant agents [67]. In addition to irrigation solutions, the use of femtosecond lasers may accelerate the rate at which bacteria are eliminated [68, 69]. Previously, it was reported that a high-power laser eliminated only 97% of E. faecalis [6, 70]. Castelo et al. [71] employed a 940 nm diode-laser to kill E. faecalis, and found that 70% of the bacteria were eradicated. With an 810 nm diode laser, Gutknecht et al. [59] found that 74% of bacterial colonies were destroyed. Some diode lasers have been displayed to be > 95% effective towards bacteria, according to other studies [58, 70].
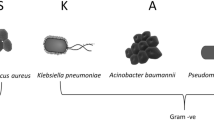
In this study, a higher energy density of 1000 J/cm2 was required to achieve 98.6% killing of E. faecalis. This is consistent with other reports which showed that visible light was more effective against S. aureus, A. baumannii, and P. aeruginosa than it was against Enterococci, E. coli, or K. pneumoniae, which required higher doses to achieve just a 1 log reduction [72]. Using E. faecium isolated from clinical sample, Halstead et al. [33] reported that 393 J/cm2 of 400 nm irradiation was required for a 1 log reduction, while Hones et al. [72] reported that 525 J/cm2 was needed for the same result. To disinfect drinking water against E. faecalis, Lui et al. [66] reviewed the effects of 455 nm irradiation and reported that an exposure level of 410 J/cm2 was necessary for a 1 log reduction.
Moreover, growth curves (Fig. S1) and maximum growth kinetics (μmax) of the bacteria at specific time points (Fig. 2C) were plotted before and after laser irradiation to monitor the differences in growth rates. The growth rate kinetics were significantly different after femtosecond laser treatment with wavelengths from 430 to 465 nm compared to the control untreated bacteria. It is worth mentioning that by slowing the growth rate kinetics, treatment with other antibacterial agents would be made more effective and synergistic effects could be observed. In the growth curves of the femtosecond laser treated bacteria with wavelengths between 430 and 465 nm, there was an increase in the lag phase, and the maximum growth was obtained after a longer time compared to 6 h in the case of control bacteria.
According to the findings of this study, the wavelengths that exhibited the greatest effectiveness were 430 and 435 nm. Bacterial cells contain endogenous photosensitizers that are responsible for their inactivation when exposed to visible light. These photosensitizers are excited when they absorb photons of the correct wavelength. ROS can be generated when the excited state PS undergoes a reaction with atmospheric oxygen in its ground state [11], which can then oxidize multiple intracellular targets at a molecular level [73,74,75,76,77,78].
Evidence supporting the importance of ROS comes from studies in which the cellular photodamage effect was partially blocked by pre-treating a suspension of microorganism cells with a recognized ROS scavenger before irradiation with a laser [36, 42, 79]. Indeed, blue light can cause damage to microorganisms in a number of ways, including the disruption of membrane integrity [34], the oxidation and release of DNA [75, 80], low levels of ATP inside the cell as a result of ATPase inhibition [75], harmful effects on vital metabolic enzymes [75], and disturbances to a number of metabolites such as coformycin, actinonin, 11-deoxycortisol, chitobiose, and tyramine [81]. Exposure to blue light has a photochemical effect rather than a photothermal effect. In fact, when microorganisms in a suspension had their temperature rise tracked using a thermocouple during irradiation, it did not surpass 0.5–4.0 °C, and the median temperature was below the point at which microorganisms are thought to die [39, 64].
Endogenous photosensitizer composition and concentration are the main factors governing bacterial damage after light irradiation. The role of porphyrin or flavin photosensitizers in the growth inhibition of microorganisms produced by blue light radiation is pathogen-specific [43]. The contribution of porphyrin photosensitizers is maximized by radiation with a wavelength of 405 nm (the Soret band absorption maximum), while the contribution of flavins is greatest when exposed to radiation at 430—450 nm, particularly 445 nm, which is the flavin absorption maxima and is barely noticeable in porphyrin absorption spectra [82]. For clinical applications, the blue wavelength of 450 nm may be preferable to 405 nm because of its deeper tissue penetration and reduced absorption by blood [25, 32, 43]. Flavin fluorescence is easily detected in extracts of S. aureus and Enterococcus spp., while porphyrin fluorescence is barely detectable [43].
Most reports have focused on targeting porphyrins in the range of 390–420 nm. But E. faecalis is an exception to this rule due to no endogenous porphyrin content but does have flavins as the main photosensitizers. E. faecalis cannot synthesize its own porphyrins, but instead must rely on taking up heme from its environment as a source of the porphyrins needed for enzyme co-factors [83]. Maximum fluorescence emission from flavin compounds occurs between 520 and 525 nm, while the excitation spectrum for fluorescence has two peaks, at 370 and 435 nm [43]. This is consistent with the results of our study, at which the maximum antimicrobial activity was noticed between 430 and 435 nm, indicating that the efficacy was due to absorption by flavins rather than porphyrins. Experimental evidence has shown that compounds of the flavin class could act as absorbers of blue spectrum light, followed by sensitizing the generation of reactive oxygen species [43, 72].
Although our preliminary results showed that the maximum antibacterial activity was at 430 and 435 nm, we also investigated the wavelength of 445 nm, which was previously reported to be a maximum in the flavin absorption spectrum. Our investigation evaluated the antibacterial activity of femtosecond laser at 445 nm with different fluences of 100, 250, 500, 750, 1000, 1250, and 2000 J/cm2. Then the viable bacterial count (CFU/mL) and the percentage of viable bacterial cells before and after laser irradiation were plotted in (Fig. 3A and Fig. 3B). Moreover, growth curves (Fig. S2) and maximum growth kinetics (μmax) of the bacteria at specific time points (Fig. 3C) were graphed before and after laser irradiation to monitor the growth rate differences at each tested fluence. Physically, the term fluence or energy density refers to the amount of energy imparted by electromagnetic radiation per unit area. Fluence equals (Pave / \(\pi\) r2) \(\times T\), where the average laser power is denoted by Pave, the laser beam radius is denoted by r, and the exposure duration is denoted by T. This means that an increase in either the average power or the exposure time will result in an increase in energy density.
The bar graph compares the control culture to bacterial cultures that were irradiated fixed laser wavelength of 445 nm at different fluences of 100, 250, 500, 750, 1000, 1250 and 2000 J/cm2 in terms of (a) percentage CFU/mL, (b) log CFU/mL, and (c) the growth rate (μmax) during the logarithmic phase of growth. Statistical significance was determined through ANOVA followed by the Tukey test, with the level of significance indicated by asterisks: **** denotes the highest significance (P < 0.001), *** denotes highly significant (P < 0.001), * denotes low significance (P < 0.05), and "ns" represents not statistically significant
A progressive decrease in colony-forming units was observed after a corresponding increase in energy density at a fixed wavelength of 445 nm, and the most effective fluence was 1250 J/cm2 causing 92.5% inhibition (more than 1 log) of viable bacteria counts. Also, the growth rate kinetics were progressively altered after femtosecond-laser treatment at 445 nm using a gradual increase in energy density. In particular, at an energy density of 1250 J/cm2, laser-exposed cultures grew substantially more slowly than control cultures.
Our results are consistent with those of previous studies indicating that the inactivation rate of many bacteria increases with increasing doses of irradiation at different wavelengths: 400 nm [33], 405 nm [34, 36, 42, 80], 460 nm [65] for E. coli; 405 nm [36] and 415 nm [84] for C. albicans; 400 nm [33], 405 nm [64, 80], 520 nm [64] and 400–550 nm [40] for S. aureus. This behavior may have a rational explanation: a higher number of photons will increase the probability of them interacting with photosensitizers and inducing more ROS production; hence, increasing the antibacterial photoinactivation effect [15, 85].
Previously, it was reported that Enterococci required higher irradiation doses for effective photoinactivation compared to other species, and microbial cell photodestruction increases with the energy dose up to a relatively high-level [42]. For this reason, we doubled the irradiation dose to 2000 J/cm2 using wavelengths from 420 to 445 nm in order to investigate the antimicrobial efficacy. The percentage of viable bacterial cells before and after laser irradiation were plotted in Fig. 4A. Moreover, growth curves (Fig. S3) and maximum growth kinetics (μmax) of the bacteria at specific time points (Fig. 4B) were plotted before and after laser irradiation.
The bar graph compares the control culture to bacterial cultures that were irradiated with different Laser parameters at ten specific wavelengths: 420, 425, 430, 435, 440, 445, 452, 455, 460, and 465 nm at a fixed fluence of 2000 J/cm.2 in terms of a) percentage CFU/mL, and c) the growth rate (μmax) during the logarithmic phase of growth. (ns; not-significant)
Surprisingly, after applying a fluence of 2000 J/cm2, the efficacy was reduced and we got less inhibitory effects in terms of viable bacterial counts. This observation could be attributed to a photobleaching phenomenon of the flavin molecules arising at a high energy density of 2000 J/cm2. Also, the growth rate kinetics were not altered compared to the control bacteria for all laser treatment wavelengths. The findings here are in line with those of other studies that reported higher energy doses of radiation were required to detect a pronounced bactericidal effect [32, 39], but photobleaching phenomena could be considered at certain high energy levels. Contrary to the findings of some earlier studies [86,87,88], we found that raising the energy density beyond a specific value had no additional effect on reducing the bacterial viability. A reasonable explanation as mentioned, could be the occurrence of the phenomenon known as photobleaching, an irreversible process in which the excitation light triggers chemical reactions that could destroy the molecular structure of a particular photosensitizer [89]. The temperature rise produced, and the excitation light power both influence the photobleaching process. Therefore, the photosensitizer molecule is damaged when the energy density is increased beyond a specific threshold, which then affects ROS production and, in turn, reduces the bactericidal action [86, 90, 91]. This phenomenon highlights the need to optimize not only the wavelength, but also the energy density for most effective aPI implementation.
Conclusions
Antibacterial photoinactivation treatment might be a revolutionary, non-invasive therapy for Vancomycin-resistant Enterococcus faecalis. As far as we are aware, this is the first study to report the deactivation of VRE with visible light. The most effective wavelengths were 430 and 435 nm at a fluence of 1000 J/cm2, causing nearly 2 log reduction (98.6% and 98.3% inhibition, respectively) of viable bacteria counts, suggesting the participation of intracellular flavins rather than intracellular porphyrins in the photodynamic bactericidal effect. Bacterial survival and growth kinetics are clearly affected by an increase in energy density, but only up to a certain point. The colony-forming units and growth rate of the laser-treated cultures were progressively decreased as energy density or light dose increased at a fixed wavelength of 445 nm, at which the most effective fluence was 1250 J/cm2 causing 92.5% inhibition (more than 1 log inhibition) of viable bacteria counts. Surprisingly, after applying a fluence of 2000 J/cm2, the efficacy was reversed and less inhibitory effects in terms of viable bacterial counts were recorded. This could be attributed to photobleaching of the flavins. Our results highlight the importance of optimising laser exposure parameters such as wavelength and energy density and their effect on improving the efficacy of aPI.
Data availability
Data will be made available on request.
References
Eldeniz AU et al (2006) Assessment of antibacterial activity of EndoREZ. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102(1):119–126
Stuart CH et al (2006) Enterococcus faecalis: its role in root canal treatment failure and current concepts in retreatment. J Endod 32(2):93–98
AlShwaimi E et al (2016) In Vitro Antimicrobial Effectiveness of Root Canal Sealers against Enterococcus faecalis: A Systematic Review. J Endod 42(11):1588–1597
Siqueira JF Jr et al (2000) Antimicrobial activity and flow rate of newer and established root canal sealers. J Endod 26(5):274–277
Behere MJ, Shinde AH, Haldar S (2023) Determination of antibiotic resistance profile of bacterial community from environmental water using antibiotic-resistant bacterial contamination detection (ABCD) kit. Biosens Bioelectron 221:114943
Afkhami F, Akbari S, Chiniforush N (2017) Entrococcus faecalis Elimination in Root Canals Using Silver Nanoparticles, Photodynamic Therapy, Diode Laser, or Laser-activated Nanoparticles: An In Vitro Study. J Endod 43(2):279–282
Verma N et al (2019) Effect of Different Concentrations of Sodium Hypochlorite on Outcome of Primary Root Canal Treatment: A Randomized Controlled Trial. J Endod 45(4):357–363
Mulani MS et al (2019) Emerging Strategies to Combat ESKAPE Pathogens in the Era of Antimicrobial Resistance: A Review. Front Microbiol 10:539
Wang Y et al (2017) Antimicrobial blue light inactivation of pathogenic microbes: State of the art. Drug Resist Updat 33–35:1–22
Hamblin MR, Abrahamse H (2020) Oxygen-independent antimicrobial photoinactivation: type III photochemical mechanism? Antibiotics (Basel) 9(2):53
Ganz RA et al (2005) Helicobacter pylori in patients can be killed by visible light. Lasers Surg Med 36(4):260–265
Huang YY et al (2018) Antimicrobial photodynamic therapy mediated by methylene blue and potassium iodide to treat urinary tract infection in a female rat model. Sci Rep 8(1):7257
Vollmerhausen TL et al (2017) Visible and UVA light as a potential means of preventing Escherichia coli biofilm formation in urine and on materials used in urethral catheters. J Photochem Photobiol B 170:295–303
Gois MM et al (2010) Susceptibility of Staphylococcus aureus to porphyrin-mediated photodynamic antimicrobial chemotherapy: an in vitro study. Lasers Med Sci 25(3):391–395
Yoneyama H, Katsumata R (2006) Antibiotic resistance in bacteria and its future for novel antibiotic development. Biosci Biotechnol Biochem 70(5):1060–1075
Wainwright M (2009) Photoantimicrobials–so what’s stopping us? Photodiagnosis Photodyn Ther 6(3–4):167–169
Ahmed E, El-Gendy AO, Hamblin MR, Mohamed T (2021) The effect of femtosecond laser irradiation on the growth kinetics of Staphylococcus aureus: An in vitro study. J Photochem Photobiol, B 221:112240
Ahmed E, El-Gendy AO, Moniem Radi NA, Mohamed T (2021) The bactericidal efficacy of femtosecond laser-based therapy on the most common infectious bacterial pathogens in chronic wounds: An in vitro study. Lasers Med Sci 36:641–647
El-Gendy AO, Obaid Y, Ahmed E, Enwemeka CS, Hassan M, Mohamed T (2022) The antimicrobial effect of gold quantum dots and femtosecond laser irradiation on the growth kinetics of common infectious eye pathogens: an in vitro study. Nanomaterials 12(21):3757
Dai T, Huang YY, Hamblin MR (2009) Photodynamic therapy for localized infections–state of the art. Photodiagnosis Photodyn Ther 6(3–4):170–188
Ghorbani J et al (2018) Photosensitizers in antibacterial photodynamic therapy: an overview. Laser Ther 27(4):293–302
El-Gendy AO, Nawaf KT, Ahmed E, Samir A, Hamblin MR, Hassan M, Mohamed T (2022) Preparation of zinc oxide nanoparticles using laser-ablation technique: Retinal epithelial cell (ARPE-19) biocompatibility and antimicrobial activity when activated with femtosecond laser. J Photochem Photobiol, B 234:112540
Schastak S et al (2010) Efficient photodynamic therapy against gram-positive and gram-negative bacteria using THPTS, a cationic photosensitizer excited by infrared wavelength. PLoS One 5(7):e11674
Tomb RM et al (2017) Assessment of the potential for resistance to antimicrobial violet-blue light in Staphylococcus aureus. Antimicrob Resist Infect Control 6:100
Leanse LG et al (2018) Evaluating the Potential for Resistance Development to Antimicrobial Blue Light (at 405 nm) in Gram-Negative Bacteria: In vitro and in vivo Studies. Front Microbiol 9:2403
Hamblin MR, Hasan T (2004) Photodynamic therapy: a new antimicrobial approach to infectious disease? Photochem Photobiol Sci 3(5):436–450
Dolmans DE, Fukumura D, Jain RK (2003) Photodynamic therapy for cancer. Nat Rev Cancer 3(5):380–387
Stark G (2005) Functional consequences of oxidative membrane damage. J Membr Biol 205(1):1–16
Henderson BW et al (2000) Photofrin photodynamic therapy can significantly deplete or preserve oxygenation in human basal cell carcinomas during treatment, depending on fluence rate. Can Res 60(3):525–529
Kwiatkowski S et al (2018) Photodynamic therapy - mechanisms, photosensitizers and combinations. Biomed Pharmacother 106:1098–1107
Hessling M, Spellerberg B, Hoenes K (2017) Photoinactivation of bacteria by endogenous photosensitizers and exposure to visible light of different wavelengths - a review on existing data. FEMS Microbiol Lett 364(2):1–12
Halstead FD et al (2016) Antibacterial Activity of Blue Light against Nosocomial Wound Pathogens Growing Planktonically and as Mature Biofilms. Appl Environ Microbiol 82(13):4006–4016
Kim MJ et al (2015) Antibacterial effect and mechanism of high-intensity 405 ± 5 nm light emitting diode on Bacillus cereus, Listeria monocytogenes, and Staphylococcus aureus under refrigerated condition. J Photochem Photobiol B 153:33–39
de Sousa NT et al (2015) Blue Laser Inhibits Bacterial Growth of Staphylococcus aureus, Escherichia coli, and Pseudomonas aeruginosa. Photomed Laser Surg 33(5):278–282
Murdoch LE et al (2013) Lethal effects of high-intensity violet 405-nm light on Saccharomyces cerevisiae, Candida albicans, and on dormant and germinating spores of Aspergillus niger. Fungal Biol 117(7–8):519–527
Dai T et al (2012) Blue light for infectious diseases: Propionibacterium acnes, Helicobacter pylori, and beyond? Drug Resist Updat 15(4):223–236
Murdoch Lynne E et al (2012) Bactericidal effects of 405 nm light exposure demonstrated by inactivation of Escherichia, Salmonella, Shigella, Listeria, and Mycobacterium species in liquid suspensions and on exposed surfaces. Sci World J 2012:1
Lipovsky A et al (2010) Visible light-induced killing of bacteria as a function of wavelength: implication for wound healing. Lasers Surg Med 42(6):467–472
Maclean M et al (2008) High-intensity narrow-spectrum light inactivation and wavelength sensitivity of Staphylococcus aureus. FEMS Microbiol Lett 285(2):227–232
Fukui M et al (2008) Specific-wavelength visible light irradiation inhibits bacterial growth of Porphyromonas gingivalis. J Periodontal Res 43(2):174–178
Endarko E et al (2012) High-intensity 405 nm light inactivation of Listeria monocytogenes. Photochem Photobiol 88(5):1280–1286
Plavskii VY et al (2018) Porphyrins and flavins as endogenous acceptors of optical radiation of blue spectral region determining photoinactivation of microbial cells. J Photochem Photobiol B 183:172–183
Distel JW, Hatton JF, Gillespie MJ (2002) Biofilm formation in medicated root canals. J Endod 28(10):689–693
Neelakantan P et al (2015) Antibiofilm activity of three irrigation protocols activated by ultrasonic, diode laser or Er:YAG laser in vitro. Int Endod J 48(6):602–610
Sebbane N et al (2022) Antibacterial Effect of Er: YAG Laser Irradiation Applied by a New Side-Firing Spiral Tip on Enterococcus faecalis Biofilm in the Tooth Root Canal—An Ex Vivo Study. Appl Sci 12(24):12656
Siqueira JF Jr et al (1997) Evaluation of the effectiveness of sodium hypochlorite used with three irrigation methods in the elimination of Enterococcus faecalis from the root canal, in vitro. Int Endod J 30(4):279–282
Zhu WC et al (2013) Anatomy of sodium hypochlorite accidents involving facial ecchymosis - a review. J Dent 41(11):935–948
Gordon W et al (2007) The antimicrobial efficacy of the erbium, chromium:yttrium-scandium-gallium-garnet laser with radial emitting tips on root canal dentin walls infected with Enterococcus faecalis. J Am Dent Assoc 138(7):992–1002
Stabholz A, Sahar-Helft S, Moshonov J (2004) Lasers in endodontics. Dent Clin North Am 48(4):809–32
Shrestha A et al (2010) Nanoparticulates for antibiofilm treatment and effect of aging on its antibacterial activity. J Endod 36(6):1030–1035
Siddiqui SH, Awan KH, Javed F (2013) Bactericidal efficacy of photodynamic therapy against Enterococcus faecalis in infected root canals: a systematic literature review. Photodiagnosis Photodyn Ther 10(4):632–643
Cassidy CM et al (2009) Drug delivery strategies for photodynamic antimicrobial chemotherapy: from benchtop to clinical practice. J Photochem Photobiol B 95(2):71–80
Jori G et al (2006) Photodynamic therapy in the treatment of microbial infections: basic principles and perspective applications. Lasers Surg Med 38(5):468–481
Frei A et al (2014) Synthesis, characterization, and biological evaluation of new Ru(II) polypyridyl photosensitizers for photodynamic therapy. J Med Chem 57(17):7280–7292
Maisch T et al (2011) Photodynamic inactivation of multi-resistant bacteria (PIB) - a new approach to treat superficial infections in the 21st century. J Dtsch Dermatol Ges 9(5):360–366
Gursoy H et al (2013) Photodynamic therapy in dentistry: a literature review. Clin Oral Investig 17(4):1113–1125
Schoop U et al (2004) Bactericidal effect of different laser systems in the deep layers of dentin. Lasers Surg Med 35(2):111–116
Gutknecht N et al (2004) Bactericidal effect of a 980-nm diode laser in the root canal wall dentin of bovine teeth. J Clin Laser Med Surg 22(1):9–13
Dougherty T, MacDonald I (2001) Basic principles of photodynamic therapy. J Porphyrins Phthalocyanines 5:105–129
Sinclair RG et al (2012) Criteria for selection of surrogates used to study the fate and control of pathogens in the environment. Appl Environ Microbiol 78(6):1969–1977
Biener G et al (2017) Blue/violet laser inactivates methicillin-resistant Staphylococcus aureus by altering its transmembrane potential. J Photochem Photobiol B 170:118–124
Instructions to authors (2019) Microbiology, A.S.f. Antimicrob Agents Chemoth 45(1):1–23
Kumar A et al (2015) Kinetics of bacterial inactivation by 405nm and 520nm light emitting diodes and the role of endogenous coproporphyrin on bacterial susceptibility. J Photochem Photobiol B 149:37–44
Kumar A et al (2017) Inactivation and changes in metabolic profile of selected foodborne bacteria by 460 nm LED illumination. Food Microbiol 63:12–21
Lui GY et al (2016) Point-of-use water disinfection using ultraviolet and visible light-emitting diodes. Sci Total Environ 553:626–635
Naghavi N et al (2014) Diode laser and calcium hydroxide for elimination of enterococcus faecalis in root canal. J Dent Mater Tech 3(2):55–60
Hegde MN, Bhat R, Shetty P (2015) Efficiency of a semiconductor diode laser in disinfection of the root canal system in endodontics: An in vitro study. J Int Clin Dent Res Organ 7(1):35
Fonseca MB et al (2008) Photodynamic therapy for root canals infected with Enterococcus faecalis. Photomed Laser Surg 26(3):209–213
Gutknecht N et al (2000) Diode laser radiation and its bactericidal effect in root canal wall dentin. J Clin Laser Med Surg 18(2):57–60
Castelo BP et al (2012) Combined sodium hypochlorite and 940 nm diode laser treatment against mature E. faecalis biofilms in-vitro. J Lasers Med Sci 3(3):116–121
Hoenes K et al (2020) Inactivation Effect of Violet and Blue Light on ESKAPE Pathogens and Closely Related Non-pathogenic Bacterial Species - A Promising Tool Against Antibiotic-Sensitive and Antibiotic-Resistant Microorganisms. Front Microbiol 11:612367
Dai T et al (2013) Blue light rescues mice from potentially fatal Pseudomonas aeruginosa burn infection: efficacy, safety, and mechanism of action. Antimicrob Agents Chemother 57(3):1238–1245
Adair TL, Drum BE (2016) RNA-Seq reveals changes in the Staphylococcus aureus transcriptome following blue light illumination. Genom Data 9:4–6
Kim MJ, Yuk HG (2017) Antibacterial mechanism of 405-nanometer light-emitting diode against salmonella at refrigeration temperature. Appl Environ Microbiol 83(5):1–14
Djouiai B et al (2018) Role of DNA repair and protective components in bacillus subtilis spore resistance to inactivation by 400-nm-wavelength blue light. Appl Environ Microbiol 84(19):1–11
Chu Z et al (2019) Inactivation of Cronobacter sakazakii by blue light illumination and the resulting oxidative damage to fatty acids. Can J Microbiol 65(12):922–929
Hyun JE, Lee SY (2020) Antibacterial effect and mechanisms of action of 460–470 nm light-emitting diode against Listeria monocytogenes and Pseudomonas fluorescens on the surface of packaged sliced cheese. Food Microbiol 86:103314
Ramakrishnan P et al (2016) Cytotoxic responses to 405nm light exposure in mammalian and bacterial cells: Involvement of reactive oxygen species. Toxicol In Vitro 33:54–62
McKenzie K et al (2016) The effects of 405 nm light on bacterial membrane integrity determined by salt and bile tolerance assays, leakage of UV-absorbing material and SYTOX green labelling. Microbiology (Reading) 162(9):1680–1688
Fontana CR et al (2015) The effect of blue light on periodontal biofilm growth in vitro. Lasers Med Sci 30(8):2077–2086
Hessling M et al (2020) Photoinactivation results of Enterococcus moraviensis with blue and violet light suggest the involvement of an unconsidered photosensitizer. Biochem Biophys Res Commun 533(4):813–817
Frankenberg L, Brugna M, Hederstedt L (2002) Enterococcus faecalis heme-dependent catalase. J Bacteriol 184(22):6351–6356
Zhang Y et al (2016) Antimicrobial blue light inactivation of Candida albicans: In vitro and in vivo studies. Virulence 7(5):536–545
Fu XJ, Fang Y, Yao M (2013) Antimicrobial photodynamic therapy for methicillin-resistant Staphylococcus aureus infection. Biomed Res Int 2013:159157
Wu J et al (2018) Changes of Intracellular Porphyrin, Reactive Oxygen Species, and Fatty Acids Profiles During Inactivation of Methicillin-Resistant Staphylococcus aureus by Antimicrobial Blue Light. Front Physiol 9:1658
Walter AB et al (2020) Optimization of optical parameters for improved photodynamic therapy of Staphylococcus aureus using endogenous coproporphyrin III. Photodiagnosis Photodyn Ther 29:101624
Rapacka-Zdonczyk A et al (2019) Development of Staphylococcus aureus tolerance to antimicrobial photodynamic inactivation and antimicrobial blue light upon sub-lethal treatment. Sci Rep 9(1):9423
Song L et al (1995) Photobleaching kinetics of fluorescein in quantitative fluorescence microscopy. Biophys J 68(6):2588–2600
Strassert CA et al (2009) Photoactive hybrid nanomaterial for targeting, labeling, and killing antibiotic-resistant bacteria. Angew Chem Int Ed Engl 48(42):7928–7931
El-Gendy AO, Samir A, Ahmed E, Enwemeka CS, Mohamed T (2021) The antimicrobial effect of 400 nm femtosecond laser and silver nanoparticles on gram-positive and gram-negative bacteria. J Photochem Photobiol, B 223:112300
Boucher HW et al (2009) Bad bugs, no drugs: no ESKAPE! An update from the Infectious Diseases Society of America. Clin Infect Dis 48(1):1–12
Acknowledgements
I affirm that We have no financial affiliation (e.g., employment, direct payment, stock holdings, retainers, consultantships, patent licensing arrangements or honoraria), or involvement with any commercial organization with direct financial interest in the subject or materials discussed in this manuscript, nor have any such arrangements existed in the past three years.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB).
Author information
Authors and Affiliations
Contributions
Conceptualization, Jonathan S. Dahm; methodology, Tarek Mohamed, Jonathan S. Dahm, Ahmed O. El-Gendy, Sarah Ezzat, Fatma Abdel Samad, Ola Ali Dabbous; validation, Ahmed O. El-Gendy, Sarah Ezzat, Fatma Abdel Samad, Ola Ali Dabbous; formal analysis, Tarek Mohamed, Jonathan S. Dahm, Ahmed O. El-Gendy; investigation, Tarek Mohamed, Jonathan S. Dahm, Ahmed O. El-Gendy, Michael R. Hamblin; writing original draft preparation, Tarek Mohamed, Ahmed O. El-Gendy; writing review and editing, Tarek Mohamed, Jonathan S. Dahm, Ahmed O. El-Gendy, Michael R. Hamblin; visualization, Sarah Ezzat, Fatma Abdel Samad, Ola Ali Dabbous; supervision: Tarek Mohamed, Ahmed O. El-Gendy; project administration, Tarek Mohamed, Ahmed O. El-Gendy. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Informed Consent
Not Applicable.
Competing Interest
The authors declare that there are no conflicts of interest related to this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
El-Gendy, A.O., Ezzat, S., Samad, F.A. et al. Studying the viability and growth kinetics of vancomycin-resistant Enterococcus faecalis V583 following femtosecond laser irradiation (420–465 nm). Lasers Med Sci 39, 144 (2024). https://doi.org/10.1007/s10103-024-04080-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-024-04080-5