Abstract
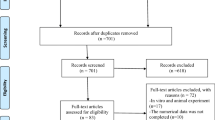
Conventional therapies have aimed to try to help individuals suffering with dentine hypersensitivity (DH/DHS). A relatively new approach, laser therapy claims to be beneficial while having immediate and long-lasting effect. Therefore, our analysis aims to explore the immediate and 1-month efficacy of near-infrared laser (NIR) therapy in treating dentinal hypersensitivity. A systematic literature search conducted in databases, and analysis was undertaken utilizing a meta-analysis approach. Randomized controlled clinical trials comparing near-infrared lasers and placebo/no treatment in patients (> 18 years) were included. The risk of bias for included studies was assessed using Cochrane RoB tool (for randomized studies). Random effects meta-analyses model of standardized mean differences and 95% confidence intervals were performed using RevMan 5.4 software. A comprehensive electronic and manual search yielded a total of 1081 potential articles. Following the implementation of the inclusion and exclusion criteria, a total of 6 studies were included in the analysis. Near-infrared laser therapy led to statistical significant reduction in immediate and 1-month follow-up VAS (visual analog scale) scores compared to placebo/no treatment (p < 0.05). Statistical heterogeneity across the studies was high (I2-96%). The findings suggest that near-infrared laser therapy does have a significant immediate effect in reducing dentine hypersensitivity compared to placebo/no treatment. Furthermore, this effect is not diminished and endured at 1-month follow-up.






Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Curro FA (1990) Tooth hypersensitivity in the spectrum of pain. Dent Clin North Am 34:429–437
Canadian Advisory Board on Dentin Hypersensitivity (2003) Consensus-based recommendations for the diagnosis and management of dentin hypersensitivity. J Can Dent Assoc 69:221–226
Rees JS, Addy M (2004) A cross-sectional study of buccal cervical sensitivity in UK general dental practice and a summary review of prevalence studies. Int J Dent Hyg 2:64–69. https://doi.org/10.1111/j.1601-5029.2004.00068.x
Pashley DH, Tay F, Haywood VB, Collins MA, Drisko CL (2008) Dentin hypersensitivity: consensus - based recommendations for the diagnosis and management of dentin hypersensitivity. Compend Contin Educ Dent 8:1–37
West NX, Lussi A, Seong J, Hellwig E (2013) Dentin hypersensitivity: pain mechanisms and aetiology of exposed cervical dentin. Clin Oral Investig 17:S9–S19. https://doi.org/10.1007/s00784-012-0887-x
Magloire H, Maurin JC, Couble ML, Shibukawa Y, Tsumura M, Thivichon-Prince B, Bleicher F (2010) Topical review. Dental pain and odontoblasts: facts and hypotheses. J Orofac Pain 24:335–349
Panagakos F, Schiff T, Guignon A (2009) Dentin hypersensitivity: effective treatment with an in-office desensitizing paste containing 8% arginine and calcium carbonate. Am J Dent 22:3A-7A
Schmalz G, Hellwig F, Mausberg RF, Schneider H, Krause F, Haak R, Ziebolz D (2017) Dentin protection of different desensitizing varnishes during stress simulation: an in vitro study. Oper Dent 42:E35–E43. https://doi.org/10.2341/16-068-l
Lin PY, Cheng YW, Chu CY, Chien KL, Lin CP, Tu YK (2013) In-office treatment for dentin hypersensitivity: a systematic review and network meta-analysis. J Clin Periodontol 40:53–64. https://doi.org/10.1111/jcpe.12011
Asnaashari M, Moeini M (2013) Effectiveness of lasers in the treatment of dentin hypersensitivity. J Lasers Med Sci 4:1–7
Sgolastra F, Petrucci A, Severino M, Gatto R, Monaco A (2013) Lasers for the treatment of dentin hypersensitivity: a meta-analysis. J Dent Res 92:492–499. https://doi.org/10.1177/0022034513487212
Kong Y, Lei Y, Li S, Zhang Y, Han J, Hu M (2020) Network meta-analysis of the desensitizing effects of lasers in patients with dentine hypersensitivity. Clin Oral Investig 24:1917–1928. https://doi.org/10.1007/s00784-019-03051-3
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al (2011) The cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928. https://doi.org/10.1136/bmj.d5928
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558. https://doi.org/10.1002/sim.1186
Hunter J, Schmidt F (2000) Fixed effects vs. random effects meta-analysis models: implications for cumulative research knowledge. Int JSelAssess 8:275–292. https://doi.org/10.1111/1468-2389.00156
Petrie A, Bulman J, Osborn J (2003) Further statistics in dentistry Part 8: systematic reviews and meta-analyses. Br Dent J 194:73–78. https://doi.org/10.1038/sj.bdj.4809877
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56:455–463. https://doi.org/10.1111/j.0006-341x.2000.00455.x
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed1000097
Lier BB, Rösing CK, Aass AM, Gjermo P (2002) Treatment of dentin hypersensitivity by Nd:YAG laser. J Clin Periodontol 29:501–506. https://doi.org/10.1034/j.1600-051x.2002.290605.x
Birang R, Poursamimi J, Gutknecht N, Lampert F, Mir M (2007) Comparative evaluation of the effects of Nd:YAG and Er:YAG laser in dentin hypersensitivity treatment. Lasers Med Sci 22:21–24. https://doi.org/10.1007/s10103-006-0412-z
Maximiano V, Machado AC, Yoshida ML, Pannuti CM, Scaramucci T, Aranha AC (2018) Nd:YAG laser and calcium sodium phosphosilicate prophylaxis paste in the treatment of dentin hypersensitivity: a double-blind randomized clinical study. Clin Oral Investig 23:3331–3338. https://doi.org/10.1007/s00784-018-2759-5
Bal MV, Keskiner I, Sezer U, Acikel C, Saygun I (2015) Comparison of low level laser and arginine-calcium carbonate alone or combination in the treatment of dentin hypersensitivity: a randomized split-mouth clinical study. Photomed Laser Surg 33:200–205. https://doi.org/10.1089/pho.2014.3873
Yilmaz H, Kurtulmus-Yilmaz S, Cengiz E, Bayindir H, Aykac Y (2011) Clinical evaluation of Er, Cr: YSGG and GaAlAs laser therapy for treating dentine hypersensitivity: a randomized controlled clinical trial. J Dentistry 39:249–254. https://doi.org/10.1016/j.jdent.2011.01.003
Yilmaz HG, Kurtulmus-Yilmaz S, Cengiz E (2011) Long-term effect of diode laser irradiation compared to sodium fluoride varnish in the treatment of dentine hypersensitivity in periodontal main- tenance patients: a randomized controlled clinical study. Photomed Laser Surg 29:721–725. https://doi.org/10.1089/pho.2010.2974
Marto CM, Baptista Paula A, Nunes T, Pimenta M, Abrantes AM, Pires AS et al (2019) Evaluation of the efficacy of dentin hypersensitivity treatments-a systematic review and follow-up analysis. J Oral Rehabil 46(10):952–990. https://doi.org/10.1111/joor.12842
Gillam DG (2015) Management of dentin hypersensitivity. Curr Oral Health Rep 2:87–94. https://doi.org/10.1007/s40496-015-0047-x
Karcioglu O, Topacoglu H, Dikme O, Dikme O (2018) A systematic review of the pain scales in adults: which to use? Am J Emerg Med 36(4):707–714. https://doi.org/10.1016/j.ajem.2018.01.008
Idon PI, Sotunde OA, Ogundare TO (2009) Beyond the relief of pain: dentin hypersensitivity and oral health-related quality of life. Front Dent 16(5):325–334. https://doi.org/10.18502/fid.v16i5.2272
Hu ML, Zheng G, Han JM, Yang M, Zhang YD, Lin H (2019) Effect of lasers on dentine hypersensitivity: evidence from a meta-analysis. J Evid Based Dent Pract 19:115–130. https://doi.org/10.1016/j.jebdp.2018.12.004
Davari A, Ataei E, Assarzadeh H (2013) Dentin hypersensitivity: etiology, diagnosis and treatment; a literature review. J Dent (Shiraz) 149(3):136–145
Lan WH, Lee BS, Liu HC, Lin CP (2004) Morphologic study of Nd:YAG laser usage in treatment of dentinal hypersensitivity. J Endod 30:131–134. https://doi.org/10.1097/00004770-200403000-00001
Aranha AC, Pimenta LA, Marchi GM (2009) Clinical evaluation of desensitizing treatments for cervical dentin hypersensitivity. Braz Oral Res 23:333–339. https://doi.org/10.1590/s1806-83242009000300018
Yilmaz HG, Cengiz E, Kurtulmus-Yilmaz S, Leblebicioglu B (2011) Effectiveness of Er, Cr:YSGG laser on dentine hypersensitivity: a controlled clinical trial. J Clin Periodontol 38:341–346. https://doi.org/10.1111/j.1600-051x.2010.01694.x
Parker S, Cronshaw M, Anagnostaki E, Mylona V, Lynch E, Grootveld M (2020) Current concepts of laser tissue interaction. Dent J (Basel) 8(3):61. https://doi.org/10.3390/dj8030061
Kreisler M, Al-Haj H, D’Hoedt B (2002) Intrapulpal temperature changes during root surface irradiation with an 809-nm GaAlAs laser. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 93(6):730–735. https://doi.org/10.1067/moe.2002.124766
Turner RM, Bird SM, Higgins JP (2013) The impact of study size on meta - analyses: examination of underpowered studies in cochrane reviews. PLoS ONE 8:e59202. https://doi.org/10.1371/journal.pone.0059202
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bellal, S., Feghali, R.E., Mehta, A. et al. Efficacy of near infrared dental lasers on dentinal hypersensitivity: a meta-analysis of randomized controlled clinical trials . Lasers Med Sci 37, 733–744 (2022). https://doi.org/10.1007/s10103-021-03391-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-021-03391-1