Abstract
Objectives
To study the clinical, epidemiological, and microbiological associations between intestinal failure (IF) and central line–associated infections (CLABSI) in patients with central vein catheters (CVCs) during 2005–2016.
Methods
We compared retrospectively CLABSI rates according to background disease, type of line access, pathogen distribution, and antibiotic susceptibilities.
Results
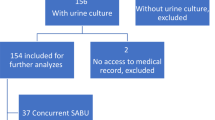
One hundred and fourteen children (64.1% < 4 years) were enrolled. Main diagnoses were persistent diarrhea (20, 17.5%), short bowel syndrome (13, 11.4%), continuous-TPN w/o diarrhea (11, 9.7%), very early–onset inflammatory bowel disease (VEO-IBD, 8, 7%), Hirschsprung’s disease (3, 2.6%), non-oncologic hematologic conditions (13, 11.4%), and other diseases (46, 40.4%). 152.749 catheter days were recorded; 71.1% had Hickman’s catheters. Two hundred and nine CLABSI episodes were recorded in 58 patients (82% with IF, 13.7 and 8.2/1000 catheter days in IF, and non-gastrointestinal conditions, P = 0.09). More CLABSI were recorded in continuous TPN vs. VEO-IBD or persistent diarrhea (38.8 vs.15.8 and 12.8/1000 catheter days, P < 0.004). Among patients with Hickman in jugular vein, highest CLBSI incidence was in continuous TPN, VEO-IBD, and persistent diarrhea (29.9, 15.84, and 12.49 episodes/1000 catheter days, respectively). CVCs were removed in 38.8% CLABSI. Two hundred and thirty-five pathogens were isolated (Enterobacteriaceae spp. in 39% of IF patients, mostly in persistent diarrhea and short bowel syndrome patients, 47.6% and 34.8%, respectively). Coagulase-negative Staphylococcus was the commonest pathogen in continuous TPN, VEO-IBD, and Hirschsprung’s (71.4%, 55.6% and 46.1%, respectively).
Conclusions
CLABSI rates in IF patients were among the highest reported. We reported a “hierarchy” in CLABSI incidence among patients with IF and showed that CLABSI incidence and etiology were different as function of background diseases and CVC insertion site.


Similar content being viewed by others
References
O’Grady NP, Alexander M, Dellinger EP, Gerberding JL, Heard SO, Maki DG et al (2002) Guidelines for the prevention of intravascular catheter-related infections. Pediatrics Nov 110(5):e51
Beekman SE, Henderson DK (2005) Infections caused by percutaneous intravascular devices. In: Mandell GL, Bennett JE, Dolin R (eds) Principles and practice of infectious diseases, sixth edition. Elsevier, Churchill Livingstone, pp 3347–3362
Mermel LA, Allon ML, Bouza E, Craven DE, Flynn P, O’Grady NP et al (2009) Clinical practice guidelines for the diagnosis and management of intravascular catheter-related infection: 2009 update by the infectious diseases society of America. Clin Infect Dis 49(1):1–45
Chesshyre E, Goff Z, Bowen A, Carapetis J (2015) The prevention, diagnosis and management of central venous line infections in children. Journal of Infection 71:S59–S75
Newman CD (2006) Catheter-related bloodstream infections in the pediatric intensive care unit. Semin Pediatr Infect Dis 17:20–24
Carter JH, Langley JM, Kuhle S, Kirkland S (2016) Risk factors for central venous catheter–associated bloodstream infection in pediatric patients: a cohort study. Infection Control & Hospital Epidemiology 37:939–945
Hartman C, Shamir R, Simchowitz V, Lohner S, Cai W, Decsi T, the ESPGHAN/ ESPEN/ESPR/CSPEN working group on pediatric parenteral nutrition. Complications (2018). Clinical Nutrition https://doi.org/10.1016/j.cinu.2018.06.956.
Wagner M, Bonhoeffer J, Erb TO, Glanzmann R, Hacker FM, Aulussen M et al (2011) Prospective study on central venous line associated bloodstream infections. Arch Dis Child 96(9):827–831
Kelly M, Conway M, Wirth K, Potter-Bynoe G, Billett AL, Sandora TJ (2011) Moving CLABSI prevention beyond the ICU: risk factors in pediatric oncology patients. Infect Control Hosp Epidemiol 32(11):1079–1085
Ammann RA, Laws HJ, Schrey D, Ehlert K, Moser O, Dilloo D et al (2015) Bloodstream infection in paediatric cancer centres-leukaemia and relapsed malignancies are independent risk factors. Eur J Pediatr 174:675686
Opilla M (2008) Epidemiology of bloodstream infection associated with parenteral nutrition. Am J Infect Control 36(10):S173–e5-8
Robinson JL, Casey LM, Huynh HQ, Spady DW (2014) Prospective cohort study of the outcome of and risk factors for intravascular catheter-related bloodstream infections in children with IF. J Parenter Enteral Nutr. 38(5):625–630
Diamanti A, Bass MS, Castro M, Calce A, Pietrobattista A, Gambarra M (2007) Prevalence of life-threatening complications in pediatric patients affected by IF. Transplant Proc 39:1632–1633
Newman N, Issa A, Greenberg D, Kapelushnik J, Cohen Z, Leibovitz E (2012) Central venous catheter-associated bloodstream infections. Pediatr Blood & Cancer 59:410–414
Piedra PA, Dryja DM, LaScolea LJ Jr (1989) Incidence of catheter-associated gram-negative bacteremia in children with short bowel syndrome. J Clin Microbiol 27(6):1317–1319
Kurkchubasche AG, Smith SD, Rowe MI (1992) Catheter sepsis in short-bowel syndrome. Arch Surg 127(1):21–24
Advani S, Reich NG, Sengupta A, Gosey L, Milstone AM (2011) Central line-associated bloodstream infection in hospitalized children with peripherally inserted central venous catheters: extending risk analyses outside the intensive care unit. Clin Infect Dis 52(9):1108–1115. https://doi.org/10.1093/cid/cir145
Terra RM, Plopper C, Waitzberg DL, Cukier C, Santoro S, Martins JR, Song RJ, Gama-Rodrigues J (2000) Remaining small bowel length: association with catheter sepsis in patients receiving home total parenteral nutrition: evidence of bacterial translocation. World J Surg 24(12):1537–1541
van Saene HK, Taylor N, Donnell SC, Glynn J, Magnall VL, Okada Y, Klein NJ, Pierro A, Lloyd DA (2003) Gut overgrowth with abnormal flora: the missing link in parenteral nutrition-related sepsis in surgical neonates. Eur J Clin Nutr 57(4):548–553
Pichler J, Horn V, Macdonald S, Hill S (2010) Sepsis and its etiology among hospitalized children less than 1 year of age with IF on parenteral nutrition. Transplant Proc 42(1):24–25
Kawagoe JY, Segre CA, Pereira CR, Cardoso MF, Silva CV, Fukushima JT (2001) Risk factors for nosocomial infections in critically ill newborns: a 5-year prospective cohort study. Am J Infect Control 29(2):109–114
Uchino M, Ikeuchi H, Matsuoka H, Bando T, Ichiki K, Nakajima K et al (2014) Catheter-associated bloodstream infection after bowel surgery in patients with inflammatory bowel disease. Surg Today 44:677–684
Miko BA, Kamath SS, Cohen BA, Jeon C, Jia H, Larson EL (2015) Epidemiologic associations between short-bowel syndrome and bloodstream infection among hospitalized children. J Pediatr Infect Dis Soc 4(3):192–197
Jeng MR, Feusner J, Skibola C, Vichinsky E (2002) Central venous catheter complications in sickle cell disease. Am J Hematol 69(2):103–108
Bartram JL, O’Driscoll S, Kulasekararaj AG, Height SE, Dick M, Patel S, Rees DC (2011) Portacaths are safe for long-term regular blood transfusion in children with sickle cell anaemia. Arch Dis Child 96(11):1082–1084
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research protocol was approved by the Ethics Committee of the Soroka University Medical Center.
Informed consent
Retrospective research, informed consent not needed.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nassar, R., Hazan, G., Leibovitz, E. et al. Central venous catheter-associated bloodstream infections in children diagnosed with intestinal failure in Southern Israel. Eur J Clin Microbiol Infect Dis 39, 517–525 (2020). https://doi.org/10.1007/s10096-019-03753-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-019-03753-2