Abstract
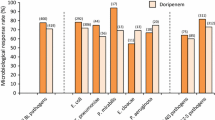
The selection of resistant gram-negative bacilli by broad-spectrum antibiotic use is a major issue in infection control. The aim of this comparative study was to assess the impact of different antimicrobial regimens commonly used to treat intra-abdominal infections on the susceptibility patterns of gram-negative bowel flora after completion of therapy. In two international randomized open-label trials with laboratory blinding, adults with complicated intra-abdominal infection requiring surgery received piperacillin-tazobactam (OASIS 1) or ceftriaxone/metronidazole (OASIS II) versus ertapenem for 4–14 days. Rectal swabs were obtained at baseline, end of therapy, and 2 weeks post-therapy. Escherichia coli and Klebsiella spp. were tested for production of extended-spectrum β-lactamase (ESBL). Enterobacteriaceae resistant to the agent used were recovered from 19 of 156 (12.2%) piperacillin-tazobactam recipients at the end of therapy compared to 1 (0.6%) patient at baseline (p<0.001) in OASIS I, and from 33 of 193 (17.1%) ceftriaxone/metronidazole recipients at the end of therapy compared to 5 (2.6%) patients at baseline (p<0.001) in OASIS II. Ertapenem-resistant Enterobacteriaceae were recovered from 1 of 155 and 1 of 196 ertapenem recipients at the end of therapy versus 0 and 1 ertapenem recipients at baseline in OASIS I and II, respectively. Resistant Enterobacteriaceae emerged significantly less often during treatment with ertapenem than with the comparator in both OASIS I (p<0.001) and OASIS II (p<0.001). The prevalence of ESBL-producers increased significantly during therapy in OASIS II among 193 ceftriaxone/metronidazole recipients (from 4 [2.1%] to 18 [9.3%]) (p<0.001), whereas no ertapenem recipient was colonized with an ESBL-producer at the end of therapy in either study. Selection for imipenem-resistant Pseudomonas aeruginosa was uncommon in all treatment groups. In these studies, the frequency of bowel colonization with resistant Enterobacteriaceae substantially increased in patients treated with either piperacillin-tazobactam or ceftriaxone/metronidazole, but not in patients treated with ertapenem.

Similar content being viewed by others
References
Lautenbach E, Strom BL, Bilker WB et al. (2001) Epidemiological investigation of fluoroquinolone resistance in infections due to extended-spectrum beta-lactamase-producing Escherichia coli and Klebsiella pneumoniae. Clin Infect Dis 33:1288–1294
Pitout JD, Sanders CC, Sanders WE Jr (1997) Antimicrobial resistance with focus on beta-lactam resistance in gram-negative bacilli. Am J Med 103:51–59
Safdar N, Maki DG (2002) The commonality of risk factors for nosocomial colonization and infection with antimicrobial-resistant Staphylococcus aureus, enterococcus, gram-negative bacilli, Clostridium difficile, and Candida. Ann Intern Med 136:834–844
Bodey GP, Fainstein V, Garcia I et al. (1983) Effect of broad-spectrum cephalosporins on the microbial flora of recipients. J Infect Dis 148:892–897
Paterson DL (2004) “Collateral damage” from cephalosporin or quinolone antibiotic therapy. Clin Infect Dis 38[Suppl 4]:341–345
Donskey CJ, Chowdhry TK, Hecker MT et al. (2000) Effect of antibiotic therapy on the density of vancomycin-resistant enterococci in the stool of colonized patients. New Engl J Med 343:1925–1932
Hoyen CK, Pultz NJ, Paterson DL et al. (2003) Effect of parenteral antibiotic administration on establishment of intestinal colonization in mice by Klebsiella pneumoniae strains producing extended-spectrum beta-lactamases. Antimicrob Agents Chemother 47:3610–3612
Donskey CJ (2004) The role of the intestinal tract as a reservoir and source for transmission of nosocomial pathogens. Clin Infect Dis 39:219–226
Flynn DM, Weinstein RA, Nathan C et al. (1987) Patients’ endogenous flora as the source of “nosocomial” Enterobacter in cardiac surgery. J Infect Dis 156:363–368
Shah PM, Isaacs RD (2003) Ertapenem, the first of a new group of carbapenems. J Antimicrob Chemother 52:538–542
Solomkin JS, Yellin AE, Rotstein OD et al. (2003) Ertapenem versus piperacillin/tazobactam in the treatment of complicated intraabdominal infections: results of a double-blind, randomized comparative phase III trial. Ann Surgery 237:235–245
Yellin AE, Hassett JM, Fernandez A et al. (2002) Ertapenem monotherapy versus combination therapy with ceftriaxone plus metronidazole for treatment of complicated intra-abdominal infections in adults. Int J Antimicrob Agents 20:165–173
National Committee for Clinical Laboratory Standards (1999) Performance standards for antimicrobial susceptibility testing. Approved standard M27-A. Ninth informational supplement. NCCLS, Wayne, PA
Piroth L, Aube H, Doise JM et al. (1998) Spread of extended-spectrum beta-lactamase-producing Klebsiella pneumoniae: are beta-lactamase inhibitors of therapeutic value? Clin Infect Dis 27:76–80
Beaber JW, Hochhut B, Waldor MK (2004) SOS response promotes horizontal dissemination of antibiotic resistance genes. Nature 427:72–74
Berkowitz FE, Metchock B (1995) Third-generation cephalosporin-resistant gram-negative bacilli in the feces of hospitalized children. Pediatr Infect Dis J 14:97–100
Cavallaro V, Catania V, Bonaccorso R et al. (1992) Effect of a broad-spectrum cephalosporin on the oral and intestinal microflora in patients undergoing colorectal surgery. J Chemother 4:82–87
Guggenbichler JP, Allerberger FJ, Dierich M (1986) Influence of cephalosporins III generation with varying biliary excretion on fecal flora and emergence of resistant bacteria during and after cessation of therapy. Padiatr Padol 21:335–342
Bhalla A, Pultz NJ, Ray AJ et al. (2003) Antianaerobic antibiotic therapy promotes overgrowth of antibiotic-resistant, gram-negative bacilli and vancomycin-resistant enterococci in the stool of colonized patients. Infect Control Hosp Epidemiol 24:644–649
Mazuski JE, Sawyer RG, Nathens AB et al. (2002) The Surgical Infection Society guidelines on antimicrobial therapy for intra-abdominal infections: an executive summary. Surg Infect (Larchmt) 3:161–173
Solomkin JS, Mazuski JE, Baron EJ et al. (2003) Guidelines for the selection of anti-infective agents for complicated intra-abdominal infections. Clin Infect Dis 37:997–1005
Motohiro T, Tanaka K, Koga T et al. (1985) Influence of ceftriaxone on bacterial flora in human feces. Jpn J Antibiot 38:2770–2796
Paterson DL, Ko WC, Von Gottberg A et al. (2001) Outcome of cephalosporin treatment for serious infections due to apparently susceptible organisms producing extended-spectrum beta-lactamases: implications for the clinical microbiology laboratory. J Clin Microbiol 39:2206–2212
Kollef MH, Sherman G, Ward S et al. (1999) Inadequate antimicrobial treatment of infections: a risk factor for hospital mortality among critically ill patients. Chest 115:462–474
Cosgrove SE, Kaye KS, Eliopoulous GM et al. (2002) Health and economic outcomes of the emergence of third-generation cephalosporin resistance in Enterobacter species. Arch Intern Med 162:185–190
Paterson DL, Ko WC, Von Gottberg A et al. (2004) International prospective study of Klebsiella pneumoniae bacteremia: implications of extended-spectrum beta-lactamase production in nosocomial infections. Ann Intern Med 140:26–32
Trouillet JL, Vuagnat A, Combes A et al. (2002) Pseudomonas aeruginosa ventilator-associated pneumonia: comparison of episodes due to piperacillin-resistant versus piperacillin-susceptible organisms. Clin Infect Dis 34:1047–1054
Martin GS, Mannino DM, Eaton S et al. (2003) The epidemiology of sepsis in the United States from 1979 through 2000. New Engl J Med 348:1546–1554
Neuhauser MM, Weinstein RA, Rydman R et al. (2003) Antibiotic resistance among gram-negative bacilli in U.S. intensive care units: implications for fluoroquinolone use. JAMA 289:885–888
Rahal JJ, Urban C, Horn D et al. (1998) Class restriction of cephalosporin use to control total cephalosporin resistance in nosocomial Klebsiella. JAMA 280:1233–1237
Fridkin SK, Hill HA, Volkova NV et al. (2002) Temporal changes in prevalence of antimicrobial resistance in 23 U.S. hospitals. Emerg Infect Dis 8:697–701
Murray BE (2000) Vancomycin-resistant enterococcal infections. New Engl J Med 342:710–721
Livermore DM (2002) Multiple mechanisms of antimicrobial resistance in Pseudomonas aeruginosa: our worst nightmare? Clin Infect Dis 34:634–640
Conflict of interest:
No information supplied
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
DiNubile, M.J., Friedland, I., Chan, C.Y. et al. Bowel colonization with resistant gram-negative bacilli after antimicrobial therapy of intra-abdominal infections: observations from two randomized comparative clinical trials of ertapenem therapy. Eur J Clin Microbiol Infect Dis 24, 443–449 (2005). https://doi.org/10.1007/s10096-005-1356-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-005-1356-0