Abstract
Upper limb impairments are common consequences of stroke. Noninvasive brain stimulation (NIBS) and virtual reality (VR) play crucial roles in improving upper limb function poststroke. This review aims to evaluate the effects of combined NIBS and VR interventions on upper limb function post-stroke and to provide recommendations for future studies in the rehabilitation field. PubMed, MEDLINE, PEDro, SCOPUS, REHABDATA, EMBASE, and Web of Science were searched from inception to November 2023. Randomized controlled trials (RCTs) encompassed patients with a confirmed stroke diagnosis, administrated combined NIBS and VR compared with passive (i.e., rest) or active (conventional therapy), and included at least one outcome assessing upper limb function (i.e., strength, spasticity, function) were selected. The quality of the included studies was assessed using the Cochrane Collaboration tool. Seven studies met the eligibility criteria. In total, 303 stroke survivors (Mean age: 61.74 years) were included in this review. According to the Cochrane Collaboration tool, five studies were classified as “high quality,” while two were categorized as “moderate quality”. There are mixed findings for the effects of combined NIBS and VR on upper limb function in stroke survivors. The evidence for the effects of combined transcranial direct current stimulation and VR on upper limb function post-stroke is promising. However, the evidence regarding the effects of combined repetitive transcranial magnetic stimulation and VR on upper limb function is limited. Further randomized controlled trials with long-term follow-up are strongly warranted.

Similar content being viewed by others
Data Availability
NA.
References
Mortality and global health estimates (2019) Who.int. https://www.who.int/data/gho/data/themes/topics/topicdetails/GHO/gho-ghe-mortality-and-global-health-estimates
Buma FE, Kwakkel G, Ramsey NF (2013) Understanding upper limb recovery after stroke. Restor Neurol Neurosci 31(6):707–722. https://doi.org/10.3233/rnn-130332
Miller EL, Murray L, Richards L, Zorowitz RD, Bakas T, Clark PC, Billinger SA (2010) Comprehensive Overview of Nursing and interdisciplinary Rehabilitation care of the stroke patient. Stroke 41(10):2402–2448. https://doi.org/10.1161/str.0b013e3181e7512b
Kwakkel G, Kollen BJ (2012) Predicting Activities after Stroke: What is Clinically Relevant? Int J Stroke 8(1):25–32. https://doi.org/10.1111/j.1747-4949.2012.00967.x
Pollock A, Farmer SE, Brady M, Langhorne P, Mead G, Mehrholz J, Van Wijck F (2014) Interventions for improving upper limb function after stroke. Cochrane Libr. https://doi.org/10.1002/14651858.cd010820.pub2
Cassidy JM, Cramer SC (2016) Spontaneous and Therapeutic-Induced Mechanisms of functional recovery after Stroke. Transl Stroke Res 8(1):33–46. https://doi.org/10.1007/s12975-016-0467-5
Warraich Z, Kleim JA (2010) Neural plasticity: the biological substrate for neurorehabilitation. PM&R 2(12S). https://doi.org/10.1016/j.pmrj.2010.10.016
Kleim JA, Jones TA (2008) Principles of Experience-Dependent Neural Plasticity: Implications for rehabilitation after Brain damage. Journal of Speech Language and Hearing Research 51(1). https://doi.org/10.1044/1092-4388(2008/018
Subramanian S, Lourenço CB, Chilingaryan G, Sveistrup H, Levin MF (2012) Arm motor recovery using a virtual reality intervention in chronic stroke. Neurorehabil Neural Repair 27(1):13–23. https://doi.org/10.1177/1545968312449695
Alashram AR, Padua E, Aburub A, Raju M, Annino G (2022) Transcranial direct current stimulation for upper extremity spasticity rehabilitation in stroke survivors: A systematic review of randomized controlled trials. PM&R 15(2):222–234. https://doi.org/10.1002/pmrj.12804
Sherman WR, Craig AB (2003) Understanding Virtual Reality—Interface, application, and design. Presence: Teleoperators Virtual Environ 12(4):441–442
Sveistrup H (2004) Motor rehabilitation using virtual reality. J Neuroeng Rehabil 1(1):1–10. https://doi.org/10.1186/1743-0003-1-10
Saleh S, Fluet GG, Qiu Q, Merians AS, Adamovich SV, Tunik E (2017) Neural Patterns of Reorganization after Intensive Robot-Assisted Virtual Reality Therapy and Repetitive Task Practice in Patients with Chronic Stroke. Frontiers in Neurology 8. https://doi.org/10.3389/fneur.2017.00452
Alashram AR, Annino G, Padua E, Romagnoli C, Mercuri NB (2019) Cognitive rehabilitation post traumatic brain injury: A systematic review for emerging use of virtual reality technology. J Clin Neurosci 66:209–219. https://doi.org/10.1016/j.jocn.2019.04.026
Chi B, Chau B, Yeo E, Ta P (2019) Virtual reality for spinal cord injury-associated neuropathic pain: Systematic review. Ann Phys Rehabil Med 62(1):49–57. https://doi.org/10.1016/j.rehab.2018.09.006
Alashram AR, Padua E, Annino G (2022) Virtual reality for balance and mobility rehabilitation following traumatic brain injury: A systematic review of randomized controlled trials. J Clin Neurosci 105:115–121. https://doi.org/10.1016/j.jocn.2022.09.012
Alashram AR, Padua E, Hammash AK, Lombardo M, Annino G (2020) Effectiveness of virtual reality on balance ability in individuals with incomplete spinal cord injury: A systematic review. J Clin Neurosci 72:322–327. https://doi.org/10.1016/j.jocn.2020.01.037
Teasell R, Mehta S, Pereira S, McIntyre A, Janzen S, Allen L, Lobo L, Viana R (2012) Time to rethink Long-Term rehabilitation management of stroke patients. Top Stroke Rehabil 19(6):457–462. https://doi.org/10.1310/tsr1906-457
Alashram AR, Padua E, Annino G (2022) Noninvasive brain stimulation for cognitive rehabilitation following traumatic brain injury: a systematic review. Appl Neuropsychol Adult 30(6):814–829. https://doi.org/10.1080/23279095.2022.2091440
Alashram AR, Padua E, Romagnoli C, Raju M, Annino G (2021) Effects of Repetitive transcranial magnetic stimulation on Upper extremity spasticity Post-Stroke: A Systematic review. Physikalische Medizin Rehabilitationsmedizin Kurortmedizin. https://doi.org/10.1055/a-1691-9641
Schlemm E, Schulz R, Bönstrup M, Krawinkel L, Fiehler J, Gerloff C, Thomalla G, Cheng B (2020) Structural brain networks and functional motor outcome after stroke—a prospective cohort study. Brain Communications 2(1). https://doi.org/10.1093/braincomms/fcaa001
Hara T, Shanmugalingam A, McIntyre A, Burhan AM (2021) The Effect of Non-Invasive Brain Stimulation (NIBS) on attention and Memory Function in Stroke Rehabilitation Patients: A Systematic Review and Meta-Analysis. Diagnostics 11(2):227. https://doi.org/10.3390/diagnostics11020227
Dhaliwal SK, Meek BP, Modirrousta M (2015) Non-Invasive brain stimulation for the treatment of symptoms following traumatic brain injury. Frontiers in Psychiatry 6. https://doi.org/10.3389/fpsyt.2015.00119
Rossi S, Hallett M, Rossini PM, Pascual-Leone Á (2009) Safety, ethical considerations, and application guidelines for the use of transcranial magnetic stimulation in clinical practice and research. Clin Neurophysiol 120(12):2008–2039. https://doi.org/10.1016/j.clinph.2009.08.016
Tassinari CA, Cincotta M, Zaccara G, Michelucci R (2003) Transcranial magnetic stimulation and epilepsy. Clin Neurophysiol 114(5):777–798. https://doi.org/10.1016/s1388-2457(03)00004-x
Sandrini M, Umiltà C, Rusconi E (2011) The use of transcranial magnetic stimulation in cognitive neuroscience: A new synthesis of methodological issues. Neurosci Biobehav Rev 35(3):516–536. https://doi.org/10.1016/j.neubiorev.2010.06.005
Peinemann A, Reimer B, Löer C, Quartarone A, Münchau A, Conrad B, Siebner HR (2004) Long-lasting increase in corticospinal excitability after 1800 pulses of subthreshold 5 Hz repetitive TMS to the primary motor cortex. Clin Neurophysiol 115(7):1519–1526. https://doi.org/10.1016/j.clinph.2004.02.005
Mansur CG, Fregni F, Boggio PS, Riberto M, Neto JG, Santos CMD, Wagner T, Rigonatti SP, Marcolin MA, Pascual-Leone A (2005) A sham stimulation-controlled trial of rTMS of the unaffected hemisphere in stroke patients. Neurology 64(10):1802–1804. https://doi.org/10.1212/01.wnl.0000161839.38079.92
Huang Y, Edwards MJ, Rounis E, Rothwell JC (2007) Theta burst stimulation on human motor cortex. Clin Neurophysiol 118(5):e151. https://doi.org/10.1016/j.clinph.2006.07.224
Schicktanz N, Fastenrath M, Milnik A, Spalek K, Auschra B, Nyffeler T, Papassotiropoulos A, De Quervain DJ, Schwegler K (2015) Continuous Theta Burst Stimulation over the Left Dorsolateral Prefrontal Cortex Decreases Medium Load Working Memory Performance in Healthy Humans. PLOS ONE 10(3):e0120640. https://doi.org/10.1371/journal.pone.0120640
Oberman LM, Edwards D, Eldaief MC, Pascual-Leone Á (2011) Safety of theta burst Transcranial Magnetic Stimulation: A Systematic Review of the literature. J Clin Neurophysiol 28(1):67–74. https://doi.org/10.1097/wnp.0b013e318205135f
George MS, Nahas Z, Borckardt JJ, Anderson B, Foust MJ, Burns C, Köse S, Short EB (2007) Brain stimulation for the treatment of psychiatric disorders. Curr Opin Psychiatry 20(3):250–254. https://doi.org/10.1097/yco.0b013e3280ad4698
Wassermann EM, Lisanby SH (2001) Therapeutic application of repetitive transcranial magnetic stimulation: a review. Clin Neurophysiol 112(8):1367–1377. https://doi.org/10.1016/s1388-2457(01)00585-5
Zaghi S, Acar M, Hultgren BA, Boggio PS, Fregni F (2009) Noninvasive Brain Stimulation with Low-Intensity Electrical Currents: Putative Mechanisms of Action for Direct and Alternating Current Stimulation. Neuroscientist 16(3):285–307. https://doi.org/10.1177/1073858409336227
Williams J, Imamura M, Fregni F (2009) Updates on the use of non-invasive brain stimulation in physical and rehabilitation medicine. J Rehabil Med 41(5):305–311. https://doi.org/10.2340/16501977-0356
Cassani R, Novak GS, Falk TH, De Oliveira AA (2020) Virtual reality and non-invasive brain stimulation for rehabilitation applications: a systematic review. Journal of Neuroengineering and Rehabilitation 17(1). https://doi.org/10.1186/s12984-020-00780-5
Massetti T, Crocetta TB, Da Silva TD, Trevizan IL, Arab C, Caromano FA, De Mello Monteiro CB (2016) Application and outcomes of therapy combining transcranial direct current stimulation and virtual reality: a systematic review. Disabil Rehabil Assist Technol 12(6):551–559. https://doi.org/10.1080/17483107.2016.1230152
Subramanian S, Prasanna SS (2018) Virtual reality and noninvasive brain stimulation in stroke: How effective is their combination for Upper limb motor Improvement?—A Meta-Analysis. PM&R 10(11):1261–1270. https://doi.org/10.1016/j.pmrj.2018.10.001
Meng J, Yan Z, Gu F, Tao X, Xue T, Liŭ D, Wang Z (2023) Transcranial direct current stimulation with virtual reality versus virtual reality alone for upper extremity rehabilitation in stroke: A meta-analysis. Heliyon 9(1):e12695. https://doi.org/10.1016/j.heliyon.2022.e12695
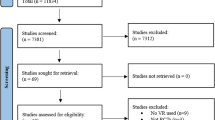
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann T, Mulrow CD, Shamseer L, Tetzlaff J, Akl EA, Brennan S, Chou R, Glanville J, Grimshaw J, Hróbjartsson A, Lalu MM, Li T, Loder E, Mayo‐Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch V, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ :n71. https://doi.org/10.1136/bmj.n71
Liberati A, Altman DG, Tetzlaff J, Mulrow CD, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA Statement for Reporting Systematic Reviews and Meta-Analyses of Studies that Evaluate Health Care Interventions: Explanation and Elaboration. PLoS Med 6(7):e1000100. https://doi.org/10.1371/journal.pmed.1000100
Higgins JPT, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, Savović J, Schulz KF, Weeks L, Sterne JA (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343(oct18 2):d5928. https://doi.org/10.1136/bmj.d5928
Jørgensen L, Paludan-Müller AS, Laursen DRT, Savović J, Boutron I, Sterne J a C, Higgins JPT, Hróbjartsson A (2016) Evaluation of the Cochrane tool for assessing risk of bias in randomized clinical trials: overview of published comments and analysis of user practice in Cochrane and non-Cochrane reviews. Systematic Reviews 5(1). https://doi.org/10.1186/s13643-016-0259-8
Yao X, Cui L, Wang J, Feng W, Bao Y, Xie Q (2020) Effects of transcranial direct current stimulation with virtual reality on upper limb function in patients with ischemic stroke: a randomized controlled trial. Journal of Neuroengineering and Rehabilitation 17(1). https://doi.org/10.1186/s12984-020-00699-x
Lee SJ, Chun MH (2014) Combination transcranial direct current stimulation and virtual reality therapy for upper extremity training in patients with subacute stroke. Arch Phys Med Rehabil 95(3):431–438. https://doi.org/10.1016/j.apmr.2013.10.027
Lee S, Cha H-G (2021) The effect of clinical application of transcranial direct current stimulation combined with non-immersive virtual reality rehabilitation in stroke patients. Technol Health Care 30(1):117–127. https://doi.org/10.3233/thc-212991
Llorens RC, Fuentes MA, Llorens RC, Latorre J, Alcañíz M, Colomer C, Noé E (2021) Effectiveness of a combined transcranial direct current stimulation and virtual reality-based intervention on upper limb function in chronic individuals post-stroke with persistent severe hemiparesis: a randomized controlled trial. Journal of Neuroengineering and Rehabilitation 18(1). https://doi.org/10.1186/s12984-021-00896-2
Viana R, Laurentino GEC, De Souza RMCR, Fonseca JB, Filho EM, Dias S, Teixeira-Salmela LF, Monte-Silva K (2014) Effects of the addition of transcranial direct current stimulation to virtual reality therapy after stroke: A pilot randomized controlled trial. NeuroRehabilitation 34(3):437–446. https://doi.org/10.3233/nre-141065
Cheng Z, Liao W, Xia W (2015) Effect of combined low-frequency repetitive transcranial magnetic stimulation and virtual reality training on upper limb function in subacute stroke: a double-blind randomized controlled trail. J Huazhong Univ Sci Technol 35(2):248–254. https://doi.org/10.1007/s11596-015-1419-0
Chen Y, Chen C-L, Huang Y, Chen H-C, Chen C-Y, Wu C, Lin K (2021) Augmented efficacy of intermittent theta burst stimulation on the virtual reality-based cycling training for upper limb function in patients with stroke: a double-blinded, randomized controlled trial. Journal of Neuroengineering and Rehabilitation 18(1). https://doi.org/10.1186/s12984-021-00885-5
Oosterveer DM, Wermer MJH, Volker G, Vlieland TPMV (2022) Are there differences in Long-Term functioning and recovery between hemorrhagic and ischemic stroke patients receiving rehabilitation? J Stroke Cerebrovasc Dis 31(3):106294. https://doi.org/10.1016/j.jstrokecerebrovasdis.2021.106294
Perna R, Temple J (2015) Rehabilitation Outcomes: Ischemic versus Hemorrhagic Strokes. Behav Neurol 2015:1–6. https://doi.org/10.1155/2015/891651
Winstein CJ, Stein J, Arena R, Bates B, Cherney LR, Cramer SC,...Zorowitz RD (2016) Guidelines for Adult Stroke Rehabilitation and Recovery. Stroke, 47(6). https://doi.org/10.1161/str.0000000000000098
Bernhardt J, Godecke E, Johnson L, Langhorne P (2017) Early rehabilitation after stroke. Curr Opin Neurol 30(1):48–54. https://doi.org/10.1097/wco.0000000000000404
Kwakkel G, Kollen BJ, Van Der Grond JV, Prevo AJH (2003) Probability of regaining dexterity in the flaccid upper limb. Stroke 34(9):2181–2186. https://doi.org/10.1161/01.str.0000087172.16305.cd
Nishimura Y, Onoe H, Morichika Y, Perfiliev S, Tsukada H, Isa T (2007) Time-Dependent central compensatory mechanisms of finger dexterity after spinal cord injury. Science 318(5853):1150–1155. https://doi.org/10.1126/science.1147243
Dhamoon MS, Moon Y, Paik MC, Boden-Albala B, Rundek T, Sacco RL, Elkind MSV (2009) Long-Term functional recovery after first ischemic stroke. Stroke 40(8):2805–2811. https://doi.org/10.1161/strokeaha.109.549576
Kolmos M, Christoffersen LC, Kruuse C (2021) Recurrent Ischemic Stroke – A Systematic Review and Meta-Analysis. J Stroke Cerebrovasc Dis 30(8):105935. https://doi.org/10.1016/j.jstrokecerebrovasdis.2021.105935
D’Souza CE, Greenway MRF, Graff-Radford J, Meschia JF (2021) Cognitive Impairment in Patients with Stroke. Semin Neurol 41(01):075–084. https://doi.org/10.1055/s-0040-1722217
De Luca R, Russo M, Naro A, Tomasello P, Leonardi S, Santamaria F, Desireè L, Bramanti A, Silvestri G, Bramanti P, Calabrò RS (2018) Effects of virtual reality-based training with BTs-Nirvana on functional recovery in stroke patients: preliminary considerations. Int J Neurosci 128(9):791–796. https://doi.org/10.1080/00207454.2017.1403915
Zhang Q, Fu Y, Lu Y, Zhang Y, Huang Q, Yang Y, Zhang K, Li M (2021) Impact of Virtual Reality-Based Therapies on Cognition and Mental Health of Stroke Patients: Systematic Review and Meta-analysis. J Med Internet Res 23(11):e31007. https://doi.org/10.2196/31007
Wu J, Zeng A, Chen Z, Wei Y, Huang K, Chen J, Ren Z (2021) Effects of Virtual Reality Training on Upper Limb Function and Balance in Stroke Patients: Systematic Review and Meta-Meta-Analysis. J Med Internet Res 23(10):e31051. https://doi.org/10.2196/31051
Tedla JS, Sangadala DR, Reddy RS, Gular K, Kakaraparthi VN, Asiri F (2023) Transcranial direct current stimulation (tDCS) effects on upper limb motor function in stroke: an overview review of the systematic reviews. Brain Inj 37(2):122–133. https://doi.org/10.1080/02699052.2022.2163289
Alashram AR, Padua E, Romagnoli C, Annino G (2019) Effectiveness of focal muscle vibration on hemiplegic upper extremity spasticity in individuals with stroke: A systematic review. NeuroRehabilitation 45(4):471–481. https://doi.org/10.3233/nre-192863
Annino G, Alashram AR, Alghwiri AA, Romagnoli C, Messina G, Tancredi V, Padua E, Mercuri NB (2019) Effect of segmental muscle vibration on upper extremity functional ability poststroke. Medicine 98(7):e14444. https://doi.org/10.1097/md.0000000000014444
Alashram AR, Annino G, Al-Qtaishat M, Padua E (2020) Mental practice combined with physical practice to enhance upper extremity functional ability poststroke: A Systematic review. J Stroke Med 3(2):51–61. https://doi.org/10.1177/2516608520943793
Alashram AR, Annino G, Mercuri NB (2019) Task-oriented motor learning in upper extremity rehabilitation post stroke. J Stroke Med 2(2):95–104. https://doi.org/10.1177/2516608519864760
Martin S, Cordeiro L, Richardson P, Davis S, Tartaglia N (2018) The association of motor skills and adaptive functioning in XXY/Klinefelter and XXYY syndromes. Phys Occup Ther Pediatr 39(4):446–459. https://doi.org/10.1080/01942638.2018.1541040
Johnson D, Harris JE, Stratford PW, Richardson J (2018) Interrater reliability of three versions of the Chedoke arm and hand activity inventory. Physiother Can 70(2):133–140. https://doi.org/10.3138/ptc.2016-70
Uswatte G, Taub E, Morris D, Vignolo MJ, McCulloch K (2005) Reliability and validity of the Upper-Extremity Motor Activity Log-14 for measuring Real-World arm use. Stroke 36(11):2493–2496. https://doi.org/10.1161/01.str.0000185928.90848.2e
Egger M, Smith GD (1998) meta-analysis bias in location and selection of studies. BMJ 316(7124):61–66. https://doi.org/10.1136/bmj.316.7124.61
Higgins JPT, Green S (2008) Cochrane Handbook for Systematic Reviews of Interventions. In: Wiley eBooks
Acknowledgements
I would like to thank Dr. Qusai Janada and Tareq Youssef, assistant professors in the physiotherapy department at Middle East University, for their general supervision in search strategy, data extraction, and methodological quality assessment.
Funding
The authors have no source of funding or any potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article is based on previously conducted studies and contains no new studies with human participants or animals performed by any of the authors.
Conflict of interest
None.
Details of any previous presentation of the research, manuscript, or abstract in any form:
None.
Permission
Permissions were approved by Dr. Qusai Janada and Tareq Youssef to include their names in acknowledgments.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix 1: Search strategy in PubMed (November 2023)
-
(1)
Stroke [MeSH]
-
(2)
Cerebrovascular accident
-
(3)
CVA
-
(4)
Hemiplegia
-
(5)
1 or 2 or 3 or 4
-
(6)
Virtual reality [MeSH]
-
(7)
Exergaming [MeSH]
-
(8)
Games
-
(9)
transcranial direct current stimulation
-
(10)
transcranial magnetic stimulation
-
(11)
noninvasive brain stimulation
-
(12)
intermittent theta burst stimulation
-
(13)
tDCS
-
(14)
TMS
-
(15)
NIBS
-
(16)
VR
-
(17)
6 or 7 or 8 or 9 or 10 or 11 or 12 or 13 or 14 or 15 or 16
-
(18)
Upper extremity [MeSH]
-
(19)
Upper limb
-
(20)
Hand [MeSH]
-
(21)
Arm [MeSH]
-
(22)
18 or 19 or 20 or 21
-
(23)
Muscle stiffness
-
(24)
Muscle hypertonia
-
(25)
Muscle spasticity [MeSH]
-
(26)
Function
-
(27)
Impairment
-
(28)
Deficit
-
(29)
Muscle strength [MeSH]
-
(30)
Muscle weakness [MeSH]
-
(31)
Functional ability
-
(32)
23 or 24 or 25 or 26 or 27 or 28 or 29 or 30 or 31
-
(33)
5 and 17 and 22 and 32
AND (“muscle stiffness” OR “muscle hypertonia” OR “muscle spasticity [MeSH]” OR “function” OR “impairment” OR “deficit” OR “muscle strength [MeSH]” OR “functional ability” OR “muscle weakness [MeSH]” (see Appendix 1).
Appendix 2
Table 4
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alashram, A.R. Combined noninvasive brain stimulation virtual reality for upper limb rehabilitation poststroke: A systematic review of randomized controlled trials. Neurol Sci 45, 2523–2537 (2024). https://doi.org/10.1007/s10072-024-07360-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-024-07360-8