Abstract
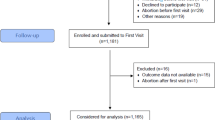
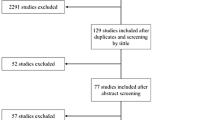
Intracranial haemorrhage (ICH) is an uncommon but one of the most devastating and potentially fatal complications of preeclampsia. Most ICHs in pregnancy are reported in the absence of a vascular lesion, and severe systolic hypertension is thought to be an important risk factor even though many reports suggest that ICH can complicate preeclampsia even at lower blood pressure levels. In this case–control study of preeclamptic women, risk factors associated with ICH were compared in women who did and did not develop ICH. During the study period, ICH occurred in 1.8% (42/2167) pregnancies with preeclampsia, with 45.2% (n = 19/42) resulting in maternal mortality. HELLP syndrome (OR = 11.5; 95% CI 3.8–34.8), multiparity (OR 3.2; 95% CI 1.4–7.7), nausea/vomiting (OR = 3.6; 95% CI 1.4–9.3), and lower educational attainment (OR = 38.2; 95% CI 3.5–423.6) were associated with the increased probability of ICH. The incidence of caesarean birth (n = 29, 74.4% vs. n = 161, 34.5%) and neonatal mortality (n = 4, 13.3% vs. n = 17, 4.0%) were higher among preeclamptic who have ICH compared to those who did not have it. Improving awareness as well as early identification of those at risk of preeclampsia and complications can limit the impact of ICH among pregnant women with preeclampsia, especially in low- to middle-income countries.


Similar content being viewed by others
Data availability
Anonymised data not published within this article will be shared on reasonable request to the corresponding author.
References
Brown MA, Magee LA, Kenny LC, Karumanchi SA, McCarthy FP, Saito S et al (2018) The hypertensive disorders of pregnancy: ISSHP classification, diagnosis & management recommendations for international practice. Pregnancy Hypertens 13(291–310):20180524. https://doi.org/10.1016/j.preghy.2018.05.004
Miller EC (2019) Preeclampsia and cerebrovascular disease. Hypertension 74(1):5–13. https://doi.org/10.1161/HYPERTENSIONAHA.118.11513
Miller EC, Vollbracht S (2021) Neurology of preeclampsia and related disorders: an update in neuro-obstetrics. Curr Pain Headache Rep 25(6):40. https://doi.org/10.1007/s11916-021-00958-z
Kane SC, Dennis A, da Silva CF, Kornman L, Brennecke S (2013) Contemporary clinical management of the cerebral complications of preeclampsia. Obstet Gynecol Int 2013(985606):20131229. https://doi.org/10.1155/2013/985606
Martin JN Jr, Thigpen BD, Moore RC, Rose CH, Cushman J, May W (2005) Stroke and severe preeclampsia and eclampsia: a paradigm shift focusing on systolic blood pressure. Obstet Gynecol 105(2):246–254. https://doi.org/10.1097/01.AOG.0000151116.84113.56
Bateman BT, Schumacher HC, Bushnell CD, Pile-Spellman J, Simpson LL, Sacco RL et al (2006) Intracerebral hemorrhage in pregnancy: frequency, risk factors, and outcome. Neurology 67(3):424–429. https://doi.org/10.1212/01.wnl.0000228277.84760.a2
Lin LT, Tsui KH, Cheng JT, Cheng JS, Huang WC, Liou WS et al (2016) Increased risk of intracranial hemorrhage in patients with pregnancy-induced hypertension: a nationwide population-based retrospective cohort study. Medicine (Baltimore) 95(20):e3732. https://doi.org/10.1097/MD.0000000000003732
Miller EC, Gatollari HJ, Too G, Boehme AK, Leffert L, Marshall RS et al (2017) Risk factors for pregnancy-associated stroke in women with preeclampsia. Stroke 48(7):1752–59. https://doi.org/10.1161/STROKEAHA.117.017374
Hasegawa J, Ikeda T, Sekizawa A, Tanaka H, Nakata M, Murakoshi T et al (2015) Maternal death due to stroke associated with pregnancy-induced hypertension. Circ J 79(8):1835–40. https://doi.org/10.1253/circj.CJ-15-0297
Bojja V, Keepanasseril A, Nair PP, Sunitha VC (2018) Clinical and imaging profile of patients with new-onset seizures & a presumptive diagnosis of eclampsia—a prospective observational study. Pregnancy Hypertens 12:35–39. https://doi.org/10.1016/j.preghy.2018.02.008
Hypertension in pregnancy (2013) Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet Gynecol 122(5):1122–31. https://doi.org/10.1097/01.AOG.0000437382.03963.88
Gestational hypertension and preeclampsia (2020) ACOG Practice Bulletin, Number 222. Obstet Gynecol 135(6):e237–e60. https://doi.org/10.1097/AOG.0000000000003891
Swartz RH, Cayley ML, Foley N, Ladhani NNN, Leffert L, Bushnell C et al (2017) The incidence of pregnancy-related stroke: a systematic review and meta-analysis. Int J Stroke 12(7):687–697. https://doi.org/10.1177/1747493017723271
Fairhall JM, Stoodley MA (2009) Intracranial haemorrhage in pregnancy. Obstet Med 2(4):142–8. https://doi.org/10.1258/om.2009.090030
Liang ZW, Lin L, Gao WL, Feng LM (2015) A clinical characteristic analysis of pregnancy-associated intracranial haemorrhage in China. Sci Rep 5(9509):20150330. https://doi.org/10.1038/srep09509
Meeks JR, Bambhroliya AB, Alex KM, Sheth SA, Savitz SI, Miller EC et al (2020) Association of primary intracerebral hemorrhage with pregnancy and the postpartum period. JAMA Netw Open 3(4):e202769. https://doi.org/10.1001/jamanetworkopen.2020.2769
Khan M, Wasay M (2013) Haemorrhagic strokes in pregnancy and puerperium. Int J Stroke 8(4):265–72. https://doi.org/10.1111/j.1747-4949.2012.00853.x
Camargo EC, Singhal AB (2021) Stroke in pregnancy: a multidisciplinary approach. Obstet Gynecol Clin North Am 48(1):75–96. https://doi.org/10.1016/j.ogc.2020.11.004
Author information
Authors and Affiliations
Contributions
AK, SPS, DN, VB, SVC, and PPN conceived the study. All authors contributed to the design. SPS, DN, VB, and SVC carried out the data collection and guarantee data integrity. AK performed statistical analyses. SPS and PPN reviewed the analysis, and AK and SPS wrote the first draft. All authors contributed to revising and finalisation of the manuscript. AK (corresponding author) guarantees all aspects of the reliability and freedom from bias of the data presented and their discussed interpretation.
Corresponding author
Ethics declarations
Ethical approval and informed consent waiver
This study was done as per the Institute Scientific Advisory and Ethical Committee (Human Studies), following the 1964 Helsinki declaration and its later amendments. Since this was a review based on records of the patients identified from the registers, a waiver of consent was approved by the Institute Ethics Committee for human studies (Certificate number: JIP/IEC/2018/308; dated 25.08.2018).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Keepanasseril, A., Subburaj, S.P., Nayak, D. et al. Risk factors of intracranial haemorrhage in preeclampsia: a case–control study. Neurol Sci 43, 6003–6010 (2022). https://doi.org/10.1007/s10072-022-06286-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06286-3