Abstract
Purpose
Intracerebral hemorrhage (ICH) can be a fatal complication of intravenous thrombolysis (IVT) for acute ischemic stroke. An early coagulopathy can develop after IVT, in relation to a significant fibrinogen depletion, increasing the risk of ICH. This systematic review and meta-analysis aimed at defining the role of fibrinogen depletion after IVT on the risk of ICH after IVT.
Methods
Protocol was registered with PROSPERO (CRD42020124241) and followed PRISMA and MOOSE guidelines. We systematically searched English studies reporting rates of post-IVT ICH depending on fibrinogen depletion until 7/1/2021. Primary outcome was symptomatic ICH (sICH). Meta-analysis followed random-effects model to account for heterogeneity in design and timing of ascertainments. Biases were assessed via the Newcastle–Ottawa Scale.
Results
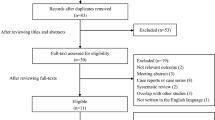
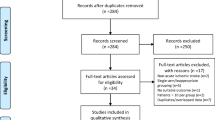
Overall, among 352 records identified, 5 observational studies were eligible for quantitative synthesis (n = 2142), all of fair quality. Considering sICH within 24–36 h post-IVT, pooling data from 4 studies (n = 1753), fibrinogen depletion consistently increased the risk of sICH (OR 3.67, 95%CI 2.28–5.90, pheterogeneity = 0.55). Pooling adjusted estimated for age, gender, and NIHSS from 3 studies (n = 723), fibrinogen depletion was confirmed to significantly increase the risk of ICH after IVT (OR 5.41, 95%CI 2.96–9.89).
Conclusions
Fibrinogen depletion significantly increases the risk of ICH after IVT for acute ischemic stroke. Routine fibrinogen assessment might be considered to identify people at higher risk of ICH. As fibrinogen repletion is feasible, trials should investigate its efficacy in preventing ICH, potentially increasing the net benefit profile of IVT in acute ischemic stroke.



Similar content being viewed by others
Data availability
Data will be shared upon reasonable request from the corresponding author.
Code availability
Data will be shared upon reasonable request from the corresponding author.
References
NINDS rtPA Study Group (1997) Intracerebral hemorrhage after intravenous t-PA therapy for ischemic stroke. Stroke 28:2109–2118
Hacke W, Kaste M, Fieschi C, Von Kummer R, Davalos A, Meier D, Larrue V, Bluhmki E, Davis S, Donnan G, Schneider D, Diez-Tejedor E, Trouillas P (1998) Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Lancet 352:1245–1251
Vandelli L, Marietta M, Trenti T, Varani M, Bigliardi G, Rosafio F, Dell’Acqua ML, Picchetto L, Nichelli P, Zini A (2019) Fibrinogen concentrate replacement in ischemic stroke patients after recombinant tissue plasminogen activator treatment. Adv Clin Exp Med 28:219–222
Schlemm L, Endres M, Werring DJ, Nolte CH (2020) Benefit of intravenous thrombolysis in acute ischemic stroke patients with high cerebral microbleed burden. Stroke 51:232–239
Bagoly Z, Szegedi I, Kálmándi R, Tóth NK, Csiba L. Markers of coagulation and fibrinolysis predicting the outcome of acute ischemic stroke thrombolysis treatment: a review of the literature. Front Neurol 2019; 10.
Trouillas P, Derex L, Philippeau F, Nighoghossian N, Honnorat J, Hanss M, Ffrench P, Adeleine P, Dechavanne M (2004) Early fibrinogen degradation coagulopathy is predictive of parenchymal hematomas in cerebral rt-PA thrombolysis: a study of 157 cases. Stroke 35:1323–1328
Sun X, Berthiller J, Trouillas P, Derex L, Diallo L, Hanss M (2015) Early fibrinogen degradation coagulopathy: a predictive factor of parenchymal hematomas in cerebral rt-PA thrombolysis. J Neurol Sci 351:109–14
Matosevic B, Knoflach M, Werner P, Pechlaner R, Zangerle A, Ruecker M, Kirchmayr M, Willeit J, Kiechl S (2013) Fibrinogen degradation coagulopathy and bleeding complications after stroke thrombolysis. Neurology 80:1216–1224
Vandelli L, Marietta M, Gambini M, Cavazzuti M, Trenti T, Cenci MA, Casoni F, Bigliardi G, Pentore R, Nichelli P, Zini A (2015) Fibrinogen decrease after intravenous thrombolysis in ischemic stroke patients is a risk factor for intracerebral hemorrhage. J Stroke Cerebrovasc Dis 24:394–400
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Phys Ther 89:873–80
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008–12
Romoli M, Paciaroni M, Tsivgoulis G, Agostoni EC, Vidale S. Mothership versus drip-and-ship model for mechanical thrombectomy in acute stroke: a systematic review and meta-analysis for clinical and radiological outcomes. J Stroke 2020; 22.
Romoli M, Mosconi MG, Pierini P, Alberti A, Venti M, Caso V, Vidale S, Lotti EM, Longoni M, Calabresi P, Tsivgoulis G, Paciaroni M. Reperfusion strategies in stroke due to isolated cervical internal carotid artery occlusion: systematic review and treatment comparison. Neurol Sci 2020; .
Viechtbauer W (2010) Conducting meta-analyses in R with the metafor. J Stat Softw 36:1–48
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Higgins JPT (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Yan S, Zhang X, Zhang R, Xu J, Lou M (2019) Early fibrinogen depletion and symptomatic intracranial hemorrhage after reperfusion therapy. Stroke 50:2716–2721
Lee VH, Conners JJ, Cutting S, Song SY, Bernstein RA, Prabhakaran S (2014) Elevated international normalized ratio as a manifestation of post-thrombolytic coagulopathy in acute ischemic stroke. J Stroke Cerebrovasc Dis 23:2139–2144
Barra ME, Feske SK, Sylvester KW, Ong C, Culbreth SE, Krause P, Henderson G V., Rybak E. Fibrinogen concentrate for the treatment of thrombolysis-associated hemorrhage in adult ischemic stroke patients. Clin Appl Thromb 2020; 26.
Szabo S, Letsch R, Ehlers R, Walter T, Kazmaier S, Helber U, Hoffmeister HM (2002) Absence of paradoxical thrombin activation by fibrin-specific thrombolytics in acute myocardial infarction: comparison of single-bolus tenecteplase and front-loaded alteplase. Thromb Res 106:113–119
Author information
Authors and Affiliations
Contributions
MR and DG performed systematic review and drafted the manuscript. MR completed statistical analysis. AZ critically reviewed the manuscript for scientific content.
Corresponding author
Ethics declarations
Ethical approval
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Romoli, M., Giannandrea, D. & Zini, A. Fibrinogen depletion and intracerebral hemorrhage after thrombolysis for ischemic stroke: a meta-analysis. Neurol Sci 43, 1127–1134 (2022). https://doi.org/10.1007/s10072-021-05441-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05441-6