Abstract
Background
The prompt recognition of an acute neurovascular syndrome by the patient or a bystander witnessing the event can directly influence outcome. We aimed to study the predictive value of the medical history and clinical features recognized by the patients’ bystanders to preclassify acute stroke syndromes in prehospital settings.
Methods
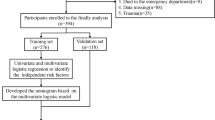
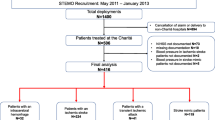
We analyzed 369 patients: 209 (56.6%) with acute ischemic stroke (AIS), 107 (29.0%) with intracerebral hemorrhage (ICH), and 53 (14.4%) with subarachnoid hemorrhage (SAH). All patients had neuroimaging as diagnostic gold standard. We constructed clinical prediction rules (CPRs) with features recognized by the bystanders witnessing the stroke onset to classify the acute neurovascular syndromes before final arrival to the emergency room (ER).
Results
In all, 83.2% cases were referred from other centers, and only 16.8% (17.2% in AIS, 15% in ICH, and 18.9% in SAH) had direct ER arrival. The time to first assessment in ≤ 3 h occurred in 72.4% (73.7%, 73.8%, and 64.2%, respectively), and final ER arrival in ≤ 3 h occurred in 26.8% (32.1%, 15.9%, and 28.3%, respectively). Clinical features referred by witnesses had low positive predictive values (PPVs) for stroke type prediction. Language or speech disorder + focal motor deficit showed 63.3% PPV, and 77.0% negative predictive value (NPV) for predicting AIS. Focal motor deficit + history of hypertension had 35.9% PPV and 78.8% NPV for ICH. Headache alone had 27.9% PPV and 95.3% NPV for SAH. In multivariate analyses, seizures, focal motor deficit, and hypertension increased the probability of a time to first assessment in ≤ 3 h, while obesity was inversely associated. Final ER arrival was determined by age and a direct ER arrival without previous referrals.
Conclusion
CPRs constructed with the witnesses’ narrative had only adequate NPVs in the prehospital classification of acute neurovascular syndromes, before neuroimaging confirmation.
Similar content being viewed by others
References
Ying A, Cheng Y, Lin Y, Yu J, Wu X, Lin Y (2020) Dynamic increase in neutrophil levels predicts parenchymal hemorrhage and function outcome of ischemic stroke with r-tPA thrombolysis. Neurol Sci 41(8):2215–2223. https://doi.org/10.1007/s10072-020-04324-6
Nor AM, McAllister C, Louw SJ, Dyker AG, Davis M, Jenkinson D, Ford GA (2004) Agreement between ambulance paramedic- and physician-recorded neurological signs with face arm speech test (FAST) in acute stroke patients. Stroke 35:1355–1359. https://doi.org/10.1161/01.STR.0000128529.63156.c5
Gonzalez-Aquines A, Cordero-Pérez AC, Cristobal-Niño M, Pérez-Vázquez G, Góngora-Rivera F, GECEN Investigators (2019) Contribution of onset-to-alarm time to prehospital delay in patients with ischemic stroke. J Stroke Cerebrovasc Dis 28(11):104331. https://doi.org/10.1016/j.jstrokecerebrovasdis.2019.104331
León-Jiménez C, Ruiz-Sandoval JL, Chiquete E, Vega-Arroyo M, Arauz A, Murillo-Bonilla LM, Ochoa-Guzmán A, Carrillo-Loza K, Ramos-Moreno A, Barinagarrementeria F, Cantú-Brito C, Investigadores PREMIER (2014) Hospital arrival time and functional outcome after acute ischaemic stroke: results from the PREMIER study. Neurologia 29:200–209
Chiquete E, Sandoval-Rodríguez V, García-Grimshaw M et al (2020) Reliability of bystander recognition of clinical features in pre-hospital classification of acute cerebrovascular syndromes: preliminary findings. Rev Invest Clin 73(5). https://doi.org/10.24875/RIC.20000238
Magnusson C, Lövgren E, Alfredsson J, Axelsson C, Andersson Hagiwara M, Rosengren L, Herlitz J, Jood K (2020) Difficulties in the prehospital assessment of patients with TIA/stroke. Acta Neurol Scand. https://doi.org/10.1111/ane.13369
Knoery CR, Heaton J, Polson R, Bond R, Iftikhar A, Rjoob K, McGilligan V, Peace A, Leslie SJ (2020) Systematic review of clinical decision support systems for prehospital acute coronary syndrome identification. Crit Pathw Cardiol 19(3):119–125. https://doi.org/10.1097/HPC.0000000000000217
Hoschar S, Albarqouni L, Ladwig KH (2020) A systematic review of educational interventions aiming to reduce prehospital delay in patients with acute coronary syndrome. Open Heart 7(1):e001175. https://doi.org/10.1136/openhrt-2019-001175
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL, on behalf of the American Heart Association Stroke Council (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 50(12):e344–e418. https://doi.org/10.1161/STR.0000000000000211
Huang SJ, Diao SS, Lu Y et al (2020) Value of thrombus imaging in predicting the outcomes of patients with large-vessel occlusive strokes after endovascular therapy. Neurol Sci 41(6):1451–1458. https://doi.org/10.1161/STR.0000000000000211
Wahlgren N, Ahmed N, Dávalos A, Hacke W, Millán M, Muir K, Roine RO, Toni D, Lees KR (2008) Thrombolysis with alteplase 3–4·5 h after acute ischaemic stroke (SITS-ISTR): an observational study. Lancet 372:1303–1309. https://doi.org/10.1016/S0140-6736(08)61339-2
Khalil HM, Lahoud N (2020) Knowledge of stroke warning signs, risk factors, and response to stroke among Lebanese older adults in Beirut. J Stroke Cerebrovasc Dis 29(5):104716. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104716
Gomes ABAGR, Henrique M Jr, Schoeps VA (2016) Popular stroke knowledge in Brazil: a multicenter survey during “world stroke day”. eNeurologicalSci 6:63–67. https://doi.org/10.1016/j.ensci.2016.12.002
Vandenbroucke JP, von Elm E, Altman DG et al (2007) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. PLoS Med 4(10):e297. https://doi.org/10.1371/journal.pmed.0040297
Uchida K, Yoshimura S, Hiyama N, Oki Y, Matsumoto T, Tokuda R, Yamaura I, Saito S, Takeuchi M, Shigeta K, Araki H, Morimoto T (2018) Clinical prediction rules to classify types of stroke at prehospital stage: Japan urgent stroke triage (JUST) score. Stroke 49:1820–1827. https://doi.org/10.1161/STROKEAHA.118.021794
Uchida K, Yoshimura S, Sakakibara F et al (2020) Simplified prehospital prediction rule to estimate the likelihood of 4 types of stroke: the 7-item Japan urgent stroke triage (JUST-7) score. Prehosp Emerg Care:1–10. https://doi.org/10.1080/10903127.2020.1800877
Wilhelm LO, Gellert P, White M, Araujo-Soares V, Ford GA, Mackintosh JE, Rodgers H, Sniehotta FF, Thomson RG, Dombrowski SU (2019) The recognition-response gap in acute stroke: examining the relationship between stroke recognition and response in a general population survey. J Stroke Cerebrovasc Dis 29:104499. https://doi.org/10.1016/j.jstrokecerebrovasdis.2019.104499
Goldstein LB, Silberberg M, McMiller Y, Yaggy SD (2009) Stroke-related knowledge among uninsured Latino immigrants in Durham County, North Carolina. J Stroke Cerebrovasc Dis 18:229–231. https://doi.org/10.1016/j.jstrokecerebrovasdis.2008.10.009
Góngora-Rivera F, González-Aquines A, Muruet W, Barrera-Barrera S, Leal-Bailey H, Espinosa-Ortega MA, Patrón-de Treviño A, Jacobo-Saucedo LA, Villarreal-Velazquez HJ, Garcia-Ortiz W, Saucedo-Ostos YY, Cordero-Perez AC, Chavez-Luevanos BE, on Behalf of Secretaria de Salud del Estado de Nuevo León and GECEN Investigators (2018) Difference in stroke knowledge between rural and urban communities in a developing country after community-based stroke educational campaigns: results from a cross-sectional study. Neuroepidemiology 51:224–229. https://doi.org/10.1159/000490724
Morone G, Martino Cinnera A, Paolucci T, Beatriz HDR, Paolucci S, Iosa M (2020) Clinical features of fallers among inpatient subacute stroke: an observational cohort. Neurol Sci 41(9):2599–2604. https://doi.org/10.1007/s10072-020-04352-2
Kidwell CS, Saver JL, Schubert GB, Eckstein M, Starkman S (1988) Design and retrospective analysis of the Los Angeles Prehospital Stroke Screen (LAPSS). Prehosp Emerg Care 2:267–273. https://doi.org/10.1080/10903129808958878
Vidale S, Agostoni E (2018) Prehospital stroke scales and large vessel occlusion: a systematic review. Acta Neurol Scand 138:24–31. https://doi.org/10.1111/ane.12908
Kothari RU, Pancioli A, Liu T et al (1999) Cincinnati prehospital stroke scale: reproducibility and validity. Ann Emerg Med 33:373–378. https://doi.org/10.1016/s0196-0644(99)70299-4
Bibok MB, Votova K, Balshaw RF, Lesperance ML, Croteau NS, Trivedi A, Morrison J, Sedgwick C, Penn AM (2018) Reducing time-to-unit among patients referred to an outpatient stroke assessment unit with a novel triage process: a prospective cohort study. BMC Health Serv Res 18(1):142. https://doi.org/10.1186/s12913-018-2952-x
Leibinger F, Allou T, Van Damme L et al (2020) Usefulness of a single-parameter tool for the prediction of large vessel occlusion in acute stroke. J Neurol 2020. https://doi.org/10.1007/s00415-020-10286-8
Ruiz-Sandoval JL, Briseño-Godínez ME, Chiquete-Anaya E, Arauz-Góngora A, Troyo-Sanromán R, Parada-Garza JD, Ramos-Moreno A, Barinagarrementería F, Murillo-Bonilla LM, Cantú-Brito C, PREMIER Investigators (2018) Public and private hospital care disparities of ischemic stroke in Mexico: results from the Primer Registro Mexicano de Isquemia Cerebral (PREMIER) study. J Stroke Cerebrovasc Dis 27(2):445–453
Griñán K, Arboix A, Massons J et al (2020) Cardioembolic stroke: risk factors, clinical features, and early outcome in 956 consecutive patients. Rev Invest Clin 73(5). https://doi.org/10.24875/RIC.20000227
Nor AM, Davis J, Sen B, Shipsey D, Louw SJ, Dyker AG, Davis M, Ford GA (2004) The Recognition of Stroke in the Emergency Room (ROSIER) scale: development and validation of a stroke recognition instrument. Lancet Neurol 4:727–734. https://doi.org/10.1016/S1474-4422(05)70201-5
Langhorne P, Ramachandra S, Stroke Unit Trialists’ Collaboration (2020) Organised inpatient (stroke unit) care for stroke: network meta-analysis. Cochrane Database Syst Rev 4(4):CD000197. https://doi.org/10.1002/14651858.CD000197.pub4
Chiquete E, Gómez-Piña JJ, Ramírez-García G et al (2020) Enfermedad carotídea aterosclerosa y enfermedad de sustancia blanca en sujetos sin historia de infarto cerebral o isquemia cerebral transitoria. Gac Med Mex 155(4):350–356. https://doi.org/10.24875/GMM.19004494
Ruiz-Sandoval JL, Chiquete E, Gárate-Carrillo A, Ochoa-Guzmán A, Arauz A, León-Jiménez C, Carrillo-Loza K, Murillo-Bonilla LM, Villarreal-Careaga J, Barinagarrementería F, Cantú-Brito C, RENAMEVASC investigators (2011) Spontaneous intracerebral hemorrhage in Mexico: results from a multicenter nationwide hospital-based registry on cerebrovascular disease (RENAMEVASC). Rev Neurol 53(12):705–712
Tanaka K, Uehara T, Ohara T, Sato S, Hayakawa M, Kimura K, Okada Y, Hasegawa Y, Tanahashi N, Suzuki A, Nakagawara J, Arii K, Nagahiro S, Ogasawara K, Uchiyama S, Matsumoto M, Iihara K, Toyoda K, Minematsu K, the PROMISE‐TIA study Investigators (2020) Transient ischemic attack without self-awareness of symptoms witnessed by bystanders: analysis of the PROMISE-TIA registry. Eur J Neurol. https://doi.org/10.1111/ene.14550
Lattanzi S, Rinaldi C, Pulcini A, Corradetti T, Angelocola S, Zedde ML, Ciliberti G, Silvestrini M (2020) Clinical phenotypes of embolic strokes of undetermined source. Neurol Sci. https://doi.org/10.1007/s10072-020-04700-2
Rodríguez-Reyes H, Lara-Vaca S, Ochoa-Guzmán A, Chiquete E, ReMeFa Study Group (2020) Obesity paradox and 12 month outcome in patients with atrial fibrillation. Arch Med Res S0188-4409(20):31075–31074. https://doi.org/10.1016/j.arcmed.2020.10.015
Cantú-Brito C, Chiquete E, Antezana-Castro JF, Toapanta-Yanchapaxi L, Ochoa-Guzmán A, Ruiz-Sandoval JL, INDAGA Cardiologists Investigators (2020) Peripheral artery disease in outpatients with a recent history of acute coronary syndrome or at high atherothrombotic risk. Vascular 8:1708538120938921. https://doi.org/10.1177/1708538120938921
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
NER-1230-14/15-1, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán.
Informed consent
Informed consent was signed by the patients or their legal proxies at hospital admission.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chiquete, E., Jiménez-Ruiz, A., García-Grimshaw, M. et al. Prediction of acute neurovascular syndromes with prehospital clinical features witnessed by bystanders. Neurol Sci 42, 3217–3224 (2021). https://doi.org/10.1007/s10072-020-04929-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04929-x