Abstract
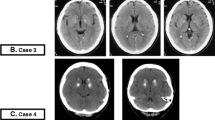
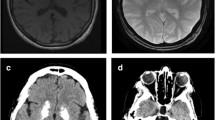
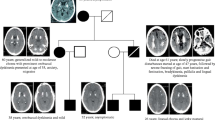
Familial idiopathic bilateral strio-pallido-dentate calcinosis is a rare autosomal dominant disorder characterized by massive symmetric calcification, detectable by CT, into the globus pallidus and striatum, with or without the involvement of the dentate nucleus, thalamus and white matter in the absence of alterations of calcium metabolism. Clinically, it has been associated with movement and/or neuropsychiatric disorders with age at onset typically in the fourth or fifth decade. Other sporadic or familial diseases can be responsible for brain calcifications with a similar anatomic strio-pallidal or strio-pallido-dentate pattern and, a restricted number of them, for neurological symptoms with onset in adulthood. Moreover, physiological age-related basal ganglia calcifications are often incidentally found, although with a far different CT aspect, in elderly patients with movement disorders. Indentifying familial and idiopathic cases may offer the opportunity to study the molecular mechanisms underlying this minerals deposition.





Similar content being viewed by others
References
Klein C, Vieregge P (1998) Fahr’s disease—far from a disease. Mov Disord 13(3):620–621. doi:10.1002/mds.870130350
Manyam BV (2005) What is and what is not ‘Fahr’s disease’. Parkinsonism Relat Disord 11(2):73–80. doi:10.1016/j.parkreldis.2004.12.001
Sobrido MJ, Hopfer S, Geschwind DH (2007) Familial idiopathic basal ganglia calcification In: Pagon RA, Bird TC, Dolan CR, Stephens K (eds) GeneReviews. http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=gene&part=bgc
Baba Y, Broderick DF, Uitti RJ, Hutton ML, Wszolek ZK (2005) Heredofamilial brain calcinosis syndrome. Mayo Clin Proc 80(5):641–651. doi:10.4065/80.5.641
Lhatoo SD, Perunovic B, Love S, Houlden H, Campbell MJ (2003) Familial idiopathic brain calcification—a new and familial alpha-synucleinopathy? Eur Neurol 49(4):223–226. doi:10.1159/000070189
Manyam BV, Walters AS, Narla KR (2001) Bilateral striopallidodentate calcinosis: clinical characteristics of patients seen in a registry. Mov Disord 16(2):258–264
Casanova MF, Araque JM (2003) Mineralization of the basal ganglia: implications for neuropsychiatry, pathology and neuroimaging. Psychiatry Res 1 121(1):59–87. doi:10.1016/S0165-1781(03)00202-6
Geschwind DH, Loginov M, Stern JM (1999) Identification of a locus on chromosome 14q for idiopathic basal ganglia calcification (Fahr disease). Am J Hum Genet 65(3):764–772. doi:10.1086/302558
Oliveira JR, Spiteri E, Sobrido MJ, Hopfer S, Klepper J, Voit T, Gilbert J, Wszolek ZK, Calne DB, Stoessl AJ, Hutton M, Manyam BV, Boller F, Baquero M, Geschwind DH (2004) Genetic heterogeneity in familial idiopathic basal ganglia calcification (Fahr disease). Neurology 63(11):2165–2167
Brodaty H, Mitchell P, Luscombe G, Kwok JJ, Badenhop RF, McKenzie R, Schofield PR (2002) Familial idiopathic basal ganglia calcification (Fahr’s disease) without neurological, cognitive and psychiatric symptoms is not linked to the IBGC1 locus on chromosome 14q. Hum Genet 110(1):8–14. doi:10.1007/s00439-001-0650-x
Sobrido MJ, Geschwind DH (2002) Genetics of familial idiopathic basal ganglia calcification (FIBGC). In: Pulst SM (ed) Genetics of movement disorders. Academic Press, San Diego, pp 443–448
Oliveira JR, Sobrido MJ, Spiteri E, Hopfer S, Meroni G, Petek E, Baquero M, Geschwind DH (2007) Analysis of candidate genes at the IBGC1 locus associated with idiopathic basal ganglia calcification (“Fahr’s disease”). J Mol Neurosci 33(2):151–154
Volpato CB, De Grandi A, Buffone E, Facheris M, Gebert U, Schifferle G, Schönhuber R, Hicks A, Pramstaller PP (2009) 2q37 as a susceptibility locus for idiopathic basal ganglia calcification (IBGC) in a large South Tyrolean family. J Mol Neurosci 39(3):346–353. doi:10.1007/s12031-009-9287-3
Dai X, Gao Y, Xu Z, Cui X, Liu J, Li Y, Xu H, Liu M, Wang QK, Liu JY (2010) Identification of a novel genetic locus on chromosome 8p21.1–q11.23 for idiopathic basal ganglia calcification. Am J Med Genet B Neuropsychiatr Genet 153B(7):1305–1310
Kiroglu Y, Calli C, Karabulut N, Cagatay O (2009) Intracranial calcifications on CT. Diagn Interv Radiol. doi:10.4261/1305-3825.DIR.2626-09.1
Deepak S, Jayakumar B, Shanavas (2005) Extensive intracranial calcification. J Assoc Physicians India 53:948
Kieffer SA, Gold LH (1974) Intracranial physiologic calcifications. Semin Roentgenol 9(2):151–162
Daghighi MH, Rezaei V, Zarrintan S, Pourfathi H (2007) Intracranial physiological calcifications in adults on computed tomography in Tabriz, Iran. Folia Morphol (Warsz) 66(2):115–9
Bosworth M, Mouw D, Skolnik DC, Hoekzema G (2008) Clinical inquiries: what is the best workup for hypocalcemia? J Fam Pract 57(10):677–679
Maeda SS, Fortes EM, Oliveira UM, Borba VC, Lazaretti-Castro M (2006) Hypoparathyroidism and pseudohypoparathyroidism. Arq Bras Endocrinol Metabol 50(4):664–673. doi:10.1590/S0004-27302006000400012
Manabe Y, Araki M, Takeda K, Yokota S, Kimura T (1989) Pseudohypoparathyroidism with striopallidodentate calcification—a case report and review of the literature. Jpn J Med 28(3):391–395
Shoback D (2008) Clinical practice. Hypoparathyroidism. N Engl J Med 359(4):391–403
Sieberer M, Haltenhof H, Haubitz B, Pabst B, Miller K, Garlipp P (2005) Basal ganglia calcification and psychosis in 22q11.2 deletion syndrome. Eur Psychiatry 20(8):567–9
Nordstrom DM, West SG, Andersen PA (1985) Basal ganglia calcifications in central nervous system lupus erythematosus. Arthritis Rheum 28(12):1412–1416
García Raya P, Gil Aguado A, Simón Merlo MJ, Lavilla Uriol P, Vega Astudillo A, García Puig J (1994) Massive cerebral calcification in systemic lupus erythematosus: report of an unusual case. Lupus 3(2):133–135
Raymond AA, Zariah AA, Samad SA, Chin CN, Kong NC (1996) Brain calcification in patients with cerebral lupus. Lupus 5(2):123–128
Filloux V, Marotte H, Miossec P (2003) Cerebral calcifications in an elderly lupus patient. Ann Rheum Dis 62(3):283–284. doi:10.1136/ard.62.3.283
Cañas CA, Tobón GJ (2008) Multiple brain calcifications in a patient with systemic lupus erythematosus. Clin Rheumatol 27(Suppl 2):S63–S65. doi:10.1007/s10067-008-0933-x
Andres RH, Schroth G, Remonda L (2008) Neurological picture. Extensive cerebral calcification in a patient with systemic lupus erythematosus. J Neurol Neurosurg Psychiatry 79(4):365. doi:10.1136/jnnp.2007.12539
Masuda Y, Uchiyama Y, Hashimoto S, Uchiyama S, Iwata M (2010) Symmetrical progressive intracranial calcification in a patient with SLE. Intern Med 49(4):351. doi:10.2169/internalmedicine.49.2693
Preusser M, Kitzwoegerer M, Budka H, Brugger S (2007) Bilateral striopallidodentate calcification (Fahr’s syndrome) and multiple system atrophy in a patient with longstanding hypoparathyroidism. Neuropathology 27(5):453–456. doi:10.1111/j.1440-1789.2007.00790
Kuroda S, Shomori A, Tateishi J (1976) Atypical Alzheimer’s disease—an autopsy case. No To Shinkei 28(4):389–395 Japanese
Shibayama H, Kobayashi H, Nakagawa M, Yamada K, Iwata H, Iwai K, Takeuchi T, Mu-Qune X, Ishihara R, Iwase S et al (1992) Non-Alzheimer non-Pick dementia with Fahr’s syndrome. Clin Neuropathol 11(5):237–250
Kosaka K (1994) Diffuse neurofibrillary tangles with calcification: a new presenile dementia. J Neurol Neurosurg Psychiatry 57(5):594–596. doi:10.1136/jnnp.57.5.594
Jellinger KA, Bancher C (1998) Senile dementia with tangles (tangle predominant form of senile dementia). Brain Pathol 8(2):367–376
Tanabe Y, Ishizu H, Ishiguro K, Itoh N, Terada S, Haraguchi T, Kawai K, Kuroda S (2000) Tau pathology in diffuse neurofibrillary tangles with calcification (DNTC): biochemical and immunohistochemical investigation. Neuroreport 11(11):2473–2477
Terada S, Ishizu H, Tanabe Y, Takehisa Y, Haraguchi T, Hamaya K, Nose S, Sudo K, Kuroda S (2001) Plaque-like structures and arteriosclerotic changes in “diffuse neurofibrillary tangles with calcification” (DNTC). Acta Neuropathol 102(6):597–603
Modrego PJ, Mojonero J, Serrano M, Fayed N (2005) Fahr’s syndrome presenting with pure and progressive presenile dementia. Neurol Sci 26(5):367–369. doi:10.1007/s10072-005-0493-7
Haraguchi T, Ishizu H, Takehisa Y, Kawai K, Yokota O, Terada S, Tsuchiya K, Ikeda K, Morita K, Horike T, Kira S, Kuroda S (2001) Lead content of brain tissue in diffuse neurofibrillary tangles with calcification (DNTC): the possibility of lead neurotoxicity. Neuroreport 12(18):3887–90. Erratum in: Neuroreport 2002 13(1):inside back cover
Tonge JI, Burry AF, Saal JR (1977) Cerebellar calcification: a possible marker of lead poisoning. Pathology 9:289–300
Benson MD, Price J (1985) Cerebellar calcification and lead. J Neurol Neurosurg Psychiatry 48:814–818
Reyes PF, Gonzalez CF, Zalewska MK, Besarab A (1986) Intracranial calcification in adults with chronic lead exposure. Am J Roentgenol 146:267–270
Thomas KP, Muthugovindan D, Singer HS (2010) Paroxysmal kinesigenic dyskinesias and pseudohypo-parathyroidism type Ib. Pediatr Neurol 43(1):61–64
Diaz GE, Wirrell EC, Matsumoto JY, Krecke KN (2010) Bilateral striopallidodentate calcinosis with paroxysmal kinesigenic dyskinesia. Pediatr Neurol 43(1):46–48
Alemdar M, Iseri P, Selekler M, Komsuoğlu SS (2007) Levetiracetam-responding paroxysmal nonkinesigenic dyskinesia. Clin Neuropharmacol 30(4):241–244 PubMed PMID: 17762321
Harwood-Nash DC, Reilly BJ (1970) Calcification of the basal ganglia following radiation therapy. Am J Roentgenol Radium Ther Nucl Med 108(2):392–395
Williams JP, Dixon G, Fowler GW, Pribram HF, Sargent EN, Turner AF (1973) Calcification of the auricular cartilage and basal ganglia secondary to radiation therapy. Bull Los Angeles Neurol Soc 38(1):33–36
Numaguchi Y, Hoffman JC, Sones PJ (1975) Basal ganglia calcification as a late radiation effect. Am J RoentgenolRadium Ther Nucl Med 123(1):27–30
Illum F (1980) Calcification of the basal ganglia following carbon monoxide poisoning. Neuroradiology 19:213–214
Smith D, Bloch S, Al-Rashid RA (1980) Basal ganglia calcification on CT scanning in children with acute lymphocytic leukemia. Neuroradiology 20(2):91–93
Almubarak S, Gan YC, Steinbok P, Hendson G, Poskitt K, Nadel H, Goddard K, Hukin J (2009) Occurrence of basal ganglia germ cell tumors without a mass. Arch Neurol 66(6):789–787 doi:10.1001/archneurol.2009.74
Hakola HP (1972) Neuropsychiatric and genetic aspects of a new hereditary disease characterized by progressive dementia and lipomembranous polycystic osteodysplasia. Acta Psychiatr Scand Suppl 232:1–173
Nasu T, Tsukahara Y, Terayama K (1973) A lipid metabolic disease-”membranouslipodystrophy”—an autopsy case demonstrating numerous peculiar membrane-structures composed of compound lipid in bone and bone marrow and various adipose tissues. Acta Pathol Jpn 23(3):539–558
Adolfsson R, Forsell A, Johansson G (1978) Hereditary polycystic osteodysplasia with progressive dementia in Sweden. Lancet 1(8075):1209–1210. doi:10.1016/S0140-6736(78)91000-0
Matsuo T, Suetsugu M, Eguchi M, Sasaki M, Tsuneyoshi M (1982) Membranous lipodystrophy. A case report. Arch Psychiatr Nervenkr 231(2):123–130
Hakola HP, Puranen M (1993) Neuropsychiatric and brain CT findings in polycystic lipomembranous osteodysplasia with sclerosing leukoencephalopathy. Acta Neurol Scand 88(5):370–375
Iivanainen M, Hakola P, Erkinjuntti T, Sipponen JT, Ketonen L, Sulkava R, Sepponen RE (1984) Cerebral MR and CT imaging in polycystic lipomembranous osteodysplasia with sclerosing leukoencephalopathy. J Comput Assist Tomogr 8(5):940–943
Markesbery WR (1979) Lactic acidemia, mitochondrial myopathy, and basal ganglia calcification. Neurology 29(7):1057–1060
Hirano M, Pavlakis SG (1994) Mitochondrial myopathy, encephalopathy, lactic acidosis, and strokelike episodes (MELAS): current concepts. J Child Neurol 9(1):4–13
Younes-Mhenni S, Thobois S, Streichenberger N, Giraud P, Mousson-de-Camaret B, Montelescaut ME et al (2002) Mitochondrial encephalomyopathy, lactic acidosis and stroke-like episodes (MELAS) associated with a Fahr disease and cerebellar calcifications. Rev Med Interne 23:1027–1029
Finsterer J (2006) Central nervous system manifestations of mitochondrial disorders. Acta Neurol Scand 114:217–238. doi:10.1111/j.1600-0404.2006.00671.x
Nakamura M, Nakano S, Goto Y, Ozawa M, Nagahama Y, Fukuyama H, Akiguchi I, Kaji R, Kimura J (1995) A novel point mutation in the mitochondrial tRNA (Ser(UCN)) gene detected in a family with MERRF/MELAS overlap syndrome. Biochem Biophys Res Commun 214(1):86–93. doi:10.1006/bbrc.1995.2260
Sue CM, Quigley A, Katsabanis S, Kapsa R, Crimmins DS, Byrne E, Morris JG (1998) Detection of MELAS A3243G point mutation in muscle, blood and hair follicles. J Neurol Sci 161(1):36–39. doi:10.1016/S0022-510X(98)00179-8
Bataillard M, Chatzoglou E, Rumbach L, Sternberg D, Tournade A, Laforêt P, Jardel C, Maisonobe T, Lombès A (2001) Atypical MELAS syndrome associated with a new mitochondrial tRNA glutamine point mutation. Neurology 56(3):405–407
Mariotti C, Savarese N, Suomalainen A, Rimoldi M, Comi G, Prelle A, Antozzi C, Servidei S, Jarre L, DiDonato S, Zeviani M (1995) Genotype to phenotype correlations in mitochondrial encephalomyopathies associated with the A3243G mutation of mitochondrial DNA. J Neurol 242(5):304–312
Martinelli P, Giuliani S, Ippoliti M, Martinelli A, Sforza A, Ferrari S (1993) Familial idiopathic strio-pallidodentate calcifications with late onset extrapyramidal syndrome. Mov Disord 8(2):220–2. doi:10.1002/mds.870080221
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bonazza, S., La Morgia, C., Martinelli, P. et al. Strio-pallido-dentate calcinosis: a diagnostic approach in adult patients. Neurol Sci 32, 537–545 (2011). https://doi.org/10.1007/s10072-011-0514-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-011-0514-7