Abstract
Background
Enthesitis-related arthritis (ERA) could be considered the pediatric equivalent of ankylosing spondylitis in adults albeit with certain significant differences. We aim to evaluate the sensitivity and specificity of the International League of Associations for Rheumatology (ILAR), the Assessment of Spondyloarthritis International Society (ASAS), and the preliminary Pediatric Rheumatology International Trials Organization (PRINTO) classification criteria in ERA patients.
Method
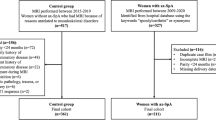
The medical records of ERA patients who were followed up between January 2005 and September 2020 have been analyzed. The control group consisted of patients with oligoarticular JIA (n = 146), polyarticular JIA (n = 55), and psoriatic arthritis (n = 20).
Results
This retrospective study included 108 ERA (73.1% male) and 221 control patients (25.8% male). The median age at diagnosis for ERA and control patients were 12.5 and 4.0 years, respectively (p < 0.001). Arthritis was observed more frequently in the control group at diagnosis and in the follow-up (p < 0.001 for both), while enthesitis, sacroiliac joint tenderness, and inflammatory back pain were more common in the ERA group both at diagnosis and in the follow-up (p < 0.001 for all). In sacroiliac imaging, 70.1% of ERA patients had positive findings suggestive of sacroiliitis at diagnosis and 78% in the follow-up. The sensitivities of ILAR, PRINTO, ASAS criteria for axial SpA, and peripheral SpA at diagnosis were 74.0%, 57.4%, 21.3%, and 85.1%, respectively which increased to 82.4%, 78.7%, 35.1%, and 92.5%, respectively at follow-up. The specificities were 100%, 100%, 99.1%, and 90.9%, respectively at both diagnosis and follow-up.
Conclusion
The ASAS criteria for peripheral SpA were the most sensitive while ILAR and the preliminary PRINTO criteria were the most specific criteria for classifying ERA patients.
Key Points.
-
The ASAS criteria for peripheral SpA were the most sensitive criteria for classifying ERA patients.
-
The use of ASAS axial SpA criteria may provide early detection of axial involvement.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
References
Solau-Gervais E, Robin C, Gambert C et al (2010) Prevalence and distribution of juvenile idiopathic arthritis in a region of Western France. Joint Bone Spine 77:47–49. https://doi.org/10.1016/j.jbspin.2009.11.002
Oen K, Tucker L, Huber AM et al (2009) Predictors of early inactive disease in a juvenile idiopathic arthritis cohort: results of a Canadian multicenter, prospective inception cohort study. Arthritis Rheum 61:1077–1086. https://doi.org/10.1002/art.24539
Demirkaya E, Ozen S, Bilginer Y et al (2011) Paediatric rheumatology. Clin Exp Rheumatol 29:111–116
Weiss PF, Klink AJ, Behrens EM et al (2011) Enthesitis in an inception cohort of enthesitis-related arthritis. Arthritis Care Res 63:1307–1312. https://doi.org/10.1002/acr.20508
Saurenmann R, Rose J, Tyrrell P et al (2007) Epidemiology of juvenile idiopathic arthritis in a multiethnic cohort: ethnicity as a risk factor. Arthritis Rheum 56:1974–1984. https://doi.org/10.1002/art.22709
Weiss PF (2012) Diagnosis and treatment of enthesitis-related arthritis. Adolesc Health Med Ther 3:67. https://doi.org/10.2147/AHMT.S25872
Tse SM, Petty RE (2015) Enthesitis related arthritis. Textbook of pediatric rheumatology 7:238–255
Gmuca S, Xiao R, Brandon TG et al (2017) Multicenter inception cohort of enthesitis-related arthritis: variation in disease characteristics and treatment approaches. Arthritis Res Ther 19:1–10. https://doi.org/10.1186/s13075-017-1297-x
Petty RE, Southwood TR, Manners P et al (2004) International League of Associations for Rheumatology classification of juvenile idiopathic arthritis: second revision, Edmonton, 2001. J Rheumatol 31:390–392
Martini A, Ravelli A, Avcin T et al (2019) Toward new classification criteria for juvenile idiopathic arthritis: first steps, pediatric rheumatology international trials organization international consensus. J Rheumatol 46:190–197
Rudwaleit M, Van Der Heijde D, Landewé R et al (2009) The development of Assessment of SpondyloArthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis 68:777–783. https://doi.org/10.1136/ard.2009.108233
Goirand M, Breton S, Chevallier F et al (2018) Clinical features of children with enthesitis-related juvenile idiopathic arthritis/juvenile spondyloarthritis followed in a French tertiary care pediatric rheumatology centre. Pediatr Rheumatol 16:1–9. https://doi.org/10.1186/s12969-018-0238-9
Adrovic A, Sezen M, Barut K et al (2017) The performance of classification criteria for juvenile spondyloarthropathies. Rheumatol Int 37:2013–2018. https://doi.org/10.1007/s00296-017-3837-8
Debrach A-C, Rougelot A, Beaumel A et al (2021) Comparison of paediatric and adult classification criteria in juvenile idiopathic arthritis during the transition from paediatric to adult care. Joint Bone Spine 88:105047. https://doi.org/10.1016/j.jbspin.2020.06.020
Naveen R, Mohindra N, Jain N et al (2021) Hip involvement in children with enthesitis related arthritis (ERA) is associated with poor outcomes in adulthood. Clin Rheumatol 40:4619–4627. https://doi.org/10.1007/s10067-021-05807-3
Flatø B, Hoffmann-Vold AM, Reiff A et al (2006) Long-term outcome and prognostic factors in enthesitis-related arthritis: a case–control study. Arthritis Rheum 54:3573–3582. https://doi.org/10.1002/art.22181
Burgos-Vargas R, Zquez-Mellado JV (1995) The early clinical recognition of juvenile-onset ankylosing spondylitis and its differentiation from juvenile rheumatoid arthritis. Arthritis Rheum 38:835–844. https://doi.org/10.1002/art.1780380618
Weiss PF, Xiao R, Biko DM et al (2016) Assessment of sacroiliitis at diagnosis of juvenile spondyloarthritis by radiography, magnetic resonance imaging, and clinical examination. Arthritis Care Res 68:187–194. https://doi.org/10.1002/acr.22665
Zisman D, Stoll ML, Aviel YB et al (2018) Juvenile psoriatic arthritis: a report from the GRAPPA 2017 annual meeting. J Rheumatol 94:11–16. https://doi.org/10.3899/jrheum.180131
Stoll ML, Nigrovic PA, Gotte AC et al (2011) Clinical comparison of early-onset psoriatic and non-psoriatic oligoarticular juvenile idiopathic arthritis. Clin Exp Rheumatol 29:582
Stoll ML, Zurakowski D, Nigrovic LE et al (2006) Patients with juvenile psoriatic arthritis comprise two distinct populations. Arthritis Rheum 54:3564–3572. https://doi.org/10.1002/art.22173
Stoll ML, Punaro M (2011) Psoriatic juvenile idiopathic arthritis: a tale of two subgroups. Curr Opin Rheumatol 23:437–443. https://doi.org/10.1097/BOR.0b013e328348b278
Nigrovic PA, Colbert RA, Holers VM et al (2021) Biological classification of childhood arthritis: roadmap to a molecular nomenclature. Nat Rev Rheumatol 17:257–269. https://doi.org/10.1038/s41584-021-00590-6
Oen K, Duffy CM, Tse SM et al (2010) Early outcomes and improvement of patients with juvenile idiopathic arthritis enrolled in a Canadian multicenter inception cohort. Arthritis Care Res 62:527–536. https://doi.org/10.1002/acr.20044
Weiss PF (2013) Evaluation and treatment of enthesitis-related arthritis. Curr Med Lit Rheumatol 32:33–41
Sarma PK, Misra R, Aggarwal A (2008) Outcome in patients with enthesitis related arthritis (ERA): juvenile arthritis damage index (JADI) and functional status. Pediatr Rheumatol 6:1–7. https://doi.org/10.1186/1546-0096-6-18
Sönmez HE, Batu ED, Demir S et al (2017) Comparison of patients with familial Mediterranean fever accompanied with sacroiliitis and patients with juvenile spondyloarthropathy. Clin Exp Rheumatol 35:124–127
Author information
Authors and Affiliations
Contributions
Study design: SO, YB, EDB, OB, and UKA. Data collection: UKA, EA, MKC, ZB, and SS. Interpretation and analysis of the data: UKA, OB, EDB, YB, and SO. All authors were involved in drafting and revising the manuscript, and approved the final version.
Each author has agreed to be accountable for the author’s own contributions and to ensure that questions related to the accuracy or integrity of any part of the work.
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kaya Akca, U., Batu, E.D., Sener, S. et al. The performances of the ILAR, ASAS, and PRINTO classification criteria in ERA patients: a comparison study. Clin Rheumatol 41, 1785–1792 (2022). https://doi.org/10.1007/s10067-022-06080-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-022-06080-8