Abstract
Objective
The aim of this study was to investigate the expression of salivary Toll-like receptors (TRL) 2 and 4 in patients with systemic lupus erythematosus (SLE) and chronic periodontitis (CP).
Methods
A case-control study was conducted with 77 participants (42 SLE and 35 non-SLE) stratified according to CP diagnosis criteria. Periodontal parameters consisted of clinical attachment level (CAL), probing depth (PD), the visible plaque index (VPI), and the gingival bleeding index (GBI). Salivary TRL 2 and 4 expressions were determined by quantitative real-time polymerase chain reaction (RT-PCR). Statistical analysis included Mann-Whitney U test, Kruskal-Wallis test, Spearman’s correlation rank, and multiple linear regression.
Results
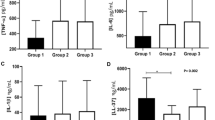
Patients with isolated SLE or CP had higher TLR 2 and TLR 4 expression in their saliva samples (P < 0.05). The group with both SLE and CP had lower TLR 2 and 4 expressions (P < 0.05). TLR 2 and TLR 4 showed significant negative correlations with PD, CAL, and GBI in SLE patients, and a significant positive correlation with periodontal parameters in non-SLE patients. CP was independently associated with reduction of TLR2 and TLR4 expression, even after adjusting for clinical data and current drug use.
Conclusion
Reduced TRL 2 and 4 expression in saliva was associated with the presence of CP in SLE patients.
Key Points • Patients affected by isolated CP or SLE had higher TLR2 and TLR4 expression. • TLR under-expression may be associated with a worse periodontal status in SLE. • Abnormalities in TLRs expression may increase the susceptibility to periodontitis. |



Similar content being viewed by others
References
Brubaker SW, Bonham KS, Zanoni I, Kagan JC (2015) Innate immune pattern recognition: a cell biological perspective. Ann Rev Immunol 33:257–290. https://doi.org/10.1146/annurev-immunol-042617-053309
Tartey S, Takeuchi O (2017) Pathogen recognition and Toll–like receptor targeted therapeutics in innate immune cells. Int Rev Immunol 36(2):57–73. https://doi.org/10.1080/08830185.2016.1261318
Jiménez-Dalmaroni MJ, Gerswhin ME, Adamopoulos IE (2016) The critical role of toll–like receptors—from microbial recognition to autoimmunity: a comprehensive review. Autoimm Rev 15(1):1–8. https://doi.org/10.1016/j.autrev.2015.08.009
Joosten LA, Abdollahi-Roodsaz S, Dinarello CA, O'neill L, Netea MG (2016) Toll–like receptors and chronic inflammation in rheumatic diseases: new developments. Nat Rev Rheumatol 12(6):344–357. https://doi.org/10.1038/nrrheum.2016.61
Schenkein HA, Thomas RR (2018) Anticardiolipin (aCL) in sera from periodontitis subjects activate Toll–like receptor 4 (TLR4). PLoS One 13(9):e0203494. https://doi.org/10.1371/journal.pone.0203494
Prasad SV, Fiedoruk K, Daniluk T, Piktel E, Bucki R (2020) Expression and function of host defense peptides at inflammation sites. Int J Mol Sci 21(1):104. https://doi.org/10.3390/ijms21010104
Hans M, Hans VM (2011) Toll–like receptors and their dual role in periodontitis: a review. J Oral Sci 53(3):263–271. https://doi.org/10.2334/josnusd.53.263
Ding PH, Jin LJ (2014) The role of lipopolysaccharide-binding protein in innate immunity: a revisit and its relevance to oral/periodontal health. J Periodontal Res 49(1):1–9. https://doi.org/10.1111/jre.12081
Cecil JD, O’Brien-Simpson NM, Lenzo JC, Holden JA, Chen YY, Singleton W, Gause KT, Yan Y, Caruso F, Reynolds EC (2016) Differential responses of pattern recognition receptors to outer membrane vesicles of three periodontal pathogens. PLoS One 11(4):e0151967. https://doi.org/10.1371/journal.pone.0151967
Marques CPC, Maor Y, De Andrade MS, Rodrigues VP, Benatti BB (2016) Possible evidence of systemic lupus erythematosus and periodontal disease association mediated by Toll-like receptors 2 and 4. Clin Exp Immunol 183(2):187–192. https://doi.org/10.1111/cei.12708
Lee YH, Choi SJ, Ji JD, Song GG (2016) Association between toll–like receptor polymorphisms and systemic lupus erythematosus: a meta–analysis update. Lupus 25(6):593–601. https://doi.org/10.1177/0961203315622823
Faridi MH, Khan SQ, Zhao W, Lee HW, Altintas MM, Zhang K, Kumar V, Armstrong AR, Carmona-Rivera C, Dorschner JM, Schnaith AM, Li X, Ghodke-Puranik Y, Moore E, Purmalek M, Irizarry-Caro J, Zhang T, Day R, Stoub D, Hoffmann V, Khaliqdina SJ, Bhargava P, Santander AM, Torroella-Kouri M, Issac B, Cimbaluk DJ, Zloza A, Prabhakar R, Deep S, Jolly M, Koh KH, Reichner JS, Bradshaw EM, Chen JF, Moita LF, Yuen PS, Li Tsai W, Singh B, Reiser J, Nath SK, Niewold TB, Vazquez-Padron RI, Kaplan MJ, Gupta V (2017) CD11b activation suppresses TLR–dependent inflammation and autoimmunity in systemic lupus erythematosus. The J Clin Inv 127(4):1271–1283. https://doi.org/10.1172/JCI88442
Tsokos GC, Lo MS, Reis PC, Sullivan KE (2016) New insights into the immunopathogenesis of systemic lupus erythematosus. Nat Rev Rheumatol 12:716–730. https://doi.org/10.1038/nrrheum.2016.186
Liu Y, Yin H, Zhao M, Lu Q (2014) TLR2 and TLR4 in autoimmune diseases: a comprehensive review. Clin Rev All Immunol 47(2):136–147. https://doi.org/10.1007/s12016-013-8402-y
Marques CPC, Victor EC, Franco MM, Fernandes JMC, Maor Y, De Andrade MS, Rodrigues VP, Benatti BB (2016) Salivary levels of inflammatory cytokines and their association to periodontal disease in systemic lupus erythematosus patients. A case–control study. Cytokine 85:165–170. https://doi.org/10.1016/j.cyto.2016.06.025
Corrêa JD, Calderaro DC, Ferreira GA, Mendonça SMS, Fernandes GR, Xiao E, Teixeira AL, Leys EJ, Graves DT, Silva TA (2017) Subgingival microbiota dysbiosis in systemic lupus erythematosus: association with periodontal status. Microbiome 5(1):34. https://doi.org/10.1186/s40168-017-0252-z
Pessoa L, Aleti G, Choudhury S, Nguyen D, Yaskell T, Zhang Y, Li W, Nelson KE, Neto LLS, Sant'Ana ACP, Freire M (2019) Host–microbial interactions in systemic lupus erythematosus and periodontitis. Front Immunol 10:2602. https://doi.org/10.3389/fimmu.2019.02602
Sete MRC, Carlos JC, Lira-Junior R, Boström EA, Sztajnbok FR, Figueredo CM (2019) Clinical, immunological and microbial gingival profile of juvenile systemic lupus erythematosus patients. Lupus 28(2):189–198. https://doi.org/10.1177/0961203318819134
Mendonça SMS, Corrêa JD, Souza AF, Travassos DV, Calderaro DC, Rocha NP, Vieira ELM, Teixeira AL, Ferreira GA, Silva TA (2019) Immunological signatures in saliva of systemic lupus erythematosus patients: influence of periodontal condition. Clin Exp Rheumatol 37:208–214
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40(9):1725. https://doi.org/10.1002/art.1780400928
Ainamo J, Bay I (1975) Problems and proposals for recording gingivitis and plaque. Int Dent J 25(4):229–235
Machtet EE, Christersson LA, Grossi SG, Dunford R, Zambon JJ, Genco RJ (1992) Clinical criteria for the definition of “established periodontitis”. J Periodontol 63(3):206–214. https://doi.org/10.1902/jop.1992.63.3.206
Wu YW, Tang W, Zuo JP (2015) Toll–like receptors: potential targets for lupus treatment. Acta Pharmacol Sin 36(12):1395–1407. https://doi.org/10.1038/aps.2015.91
O'Gorman WE, Hsieh EW, Savig ES, Gherardini PF, Hernandez JD, Hansmann L, Balboni IM, Utz PJ, Bendall SC, Fantl WJ, Lewis DB, Nolan GP, Davis MM (2015) Single–cell systems–level analysis of human Toll–like receptor activation defines a chemokine signature in patients with systemic lupus erythematosus. J All Clin Immunol 136(5):1326–1336. https://doi.org/10.1016/j.jaci.2015.04.008
Urbonaviciute V, Starke C, Pirschel W, Pohle S, Frey S, Daniel C, Amann K, Schett G, Herrmann M, Voll RE (2013) Toll-like receptor 2 is required for autoantibody production and development of renal disease in pristane-induced lupus. Arthritis Rheum 65(6):1612–1623. https://doi.org/10.1002/art.37914
Houssen ME, El-Mahdy RH, Shahin DA (2016) Serum soluble toll-like receptor 2: a novel biomarker for systemic lupus erythematosus disease activity and lupus-related cardiovascular dysfunction. Int J Rheum Dis 19(7):685–692. https://doi.org/10.1111/1756-185X.12452
Perez-Ferro M, Del Castillo CS, Sanchez-Pernaute O (2016) Cell membrane–bound TLR2 and TLR4: potential predictors of active systemic lupus erythematosus and lupus nephritis. J Rheumatol 43(7):1444–1445. https://doi.org/10.3899/jrheum.151386
Tian L, Wen Q, Dang X, You W, Fan L, Wang K (2014) Immune response associated with Toll–like receptor 4 signaling pathway leads to steroid–induced femoral head osteonecrosis. BMC Musculoskelet Disord 15:18. https://doi.org/10.1186/1471-2474-15-18
Broering R, Montag M, Jiang M, Lu M, Sowa JP, Kleinehr K, Gerken G, Schlaak JF (2011) Corticosteroids shift the Toll–like receptor response pattern of primary–isolated murine liver cells from an inflammatory to an anti–inflammatory state. Int Immunol 23(9):537–544. https://doi.org/10.1093/intimm/dxr048
MacRedmond RE, Greene CM, Dorscheid DR, McElvaney NG, O'Neill SJ (2007) Epithelial expression of TLR4 is modulated in COPD and by steroids, salmeterol and cigarette smoke. Respir Res 8:84. https://doi.org/10.1186/1465-9921-8-84
Ren L, Leung WK, Darveau RP, Jin L (2005) The expression profile of lipopolysaccharide-binding protein, membrane-bound CD14, and toll-like receptors 2 and 4 in chronic periodontitis. J Periodontol 76(11):1950–1959. https://doi.org/10.1902/jop.2005.76.11.1950
Tang L, Zhou XD, Wang Q, Zhang L, Wang Y, Li XY, Huang DM (2011) Expression of TRAF6 and pro–inflammatory cytokines through activation of TLR2, TLR4, NOD1, and NOD2 in human periodontal ligament fibroblasts. Arch Oral Biol 56(10):1064–1072. https://doi.org/10.1016/j.archoralbio.2011.02.020
Sun JY, Li DL, Dong Y, Zhu CH, Liu J, Li JD, Zhou T, Gou JZ, Li A, Zang WJ (2016) Baicalin inhibits toll–like receptor 2/4 expression and downstream signaling in rat experimental periodontitis. Int Immunopharmacol 36:86–93. https://doi.org/10.1016/j.intimp.2016.04.012
Kikkert R, Laine ML, Aarden LA, Van Winkelhoff AJ (2007) Activation of toll-like receptors 2 and 4 by gram-negative periodontal bacteria. Oral Microbiol Immunol 22(3):145–151. https://doi.org/10.1111/j.1399-302X.2007.00335.x
Fernández A, Cárdenas AM, Astorga J, Veloso P, Alvarado A, Merino P, Pino D, Reyes-Court D, Hernández M (2019) Expression of Toll–like receptors 2 and 4 and its association with matrix metalloproteinases in symptomatic and asymptomatic apical periodontitis. Clin Oral Invest 23(12):4205–4212. https://doi.org/10.1007/s00784-019-02861-9
Bagavant H, Dunkleberger ML, Wolska N, Sroka M, Rasmussen A, Adrianto I, Montgomery C, Sivils K, Guthridge JM, James JA, Merrill JT, Deshmukh US (2019) Antibodies to periodontogenic bacteria are associated with higher disease activity in lupus patients. Clin Exp Rheumatol 37(1):106–111
Rutter-Locher Z, Smith TO, Giles I, Sofat N (2017) Association between systemic lupus erythematosus and periodontitis: a systematic review and meta–analysis. Front Immunol 8:1295. https://doi.org/10.3389/fimmu.2017.01295
Calderaro DC, Ferreira GA, Corrêa JD, Mendonça SMS, Silva TA, Costa FO, Teixeira AL (2017) Is chronic periodontitis premature in systemic lupus erythematosus patients? Clin Rheumatol 36(3):713–718. https://doi.org/10.1007/s10067-016-3385-8
Fabbri C, Fuller R, Bonfá E, Guedes LK, D’Alleva PSR, Borba EF (2014) Periodontitis treatment improves systemic lupus erythematosus response to immunosuppressive therapy. Clin Reumatol 33(4):505–509. https://doi.org/10.1007/s10067-013-2473-2
Zhang Q, Zhang X, Feng G, Fu T, Yin R, Zhang L, Feng X, Li L, Gu Z (2017) Periodontal disease in Chinese patients with systemic lupus erythematosus. Rheumatol Int 37(8):1373-1379. https://doi.org/10.1007/s00296-017-3759-5
Graves DT, Corrêa JD, Silva TA (2019) The oral microbiota is modified by systemic diseases. J Dent Res 98(2):148–156. https://doi.org/10.1177/0022034518805739
Yamaba S, Yamada S, Kajikawa T, Awata T, Sakashita H, Tsushima K, Fujihara C, Yanagita M, Murakami S (2015) PLAP–1/asporin regulates TLR2– and TLR4–induced inflammatory responses. J Dent Res 94(12):1706–1714. https://doi.org/10.1177/0022034515606859
Kizawa H, Kou I, Iida A, Sudo A, Miyamoto Y, Fukuda A, Mabuchi A, Kotani A, Kawakami A, Yamamoto S, Uchida A, Nakamura K, Notoya K, Nakamura Y, Ikegawa S (2005) An aspartic acid repeat polymorphism in asporin inhibits chondrogenesis and increases susceptibility to osteoarthritis. Nat Genet 37:138–144. https://doi.org/10.1038/ng1496
He CF, Liu YS, Cheng YL, Gao JP, Pan TM, Han JW, Quan C, Sun LD, Zheng HF, Zuo XB, Xu SX, Sheng YJ, Yao S, Hu WL, Li Y, Yu ZY, Yin XY, Zhang XJ, Cui Y, Yang S (2010) TNIP1, SLC15A4, ETS1, RasGRP3 and IKZF1 are associated with clinical features of systemic lupus erythematosus in a Chinese Han population. Lupus 19:1181–1186. https://doi.org/10.1177/0961203310367918
Javinani A, Ashraf-Ganjouei A, Aslani S, Jamshidi A, Mahmoudi M (2019) Exploring the etiopathogenesis of systemic lupus erythematosus: a genetic perspective. Immunogenet 71(4):283–297. https://doi.org/10.1007/s00251-019-01103-2
Funding
This work was supported by the Research Support Foundation of Maranhão State (FAPEMA) [grant number 009699/2015] and the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) [Finance Code 001].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Ethical approval
The study was approved by the Research Ethics Committee of the University Hospital of the Federal University of Maranhão (CAAE: 22437713.6.0000.5086).
Informed consent
All participants signed informed consent forms prior to the present study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Marques, C.P.C., Rodrigues, V.P., de Carvalho, L.C. et al. Expression of Toll-like receptors 2 and 4 in the saliva of patients with systemic lupus erythematosus and chronic periodontitis. Clin Rheumatol 40, 2727–2734 (2021). https://doi.org/10.1007/s10067-020-05560-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05560-z