Abstract
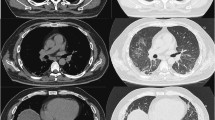
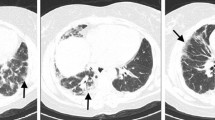
Patients with clinically amyopathic dermatomyositis (CADM) have a risk of developing rapidly progressive interstitial lung disease (ILD). CADM-ILD is associated with the anti-MDA-5 antibody. In the USA, however, patients with CADM have these antibodies less frequently than those in Japan. In addition, those with this disorder are less often complicated with rapidly progressive ILD than those in Japan. We present a case of a 42-year-old Japanese-American female with a 3-month history of a rash on her hands and face with joint pain. Based on the negative results from lupus tests, her primary care provider and a rheumatologist treated her with steroids, hydroxychloroquine, and methotrexate. During treatment, the patient started noticing shortness of breath because of pneumonia, which was revealed by a CT scan. The woman was finally diagnosed with acute respiratory failure due to CADM with ILD. She underwent a double lung transplant as well as treatment with multiple immunosuppressive agents and repeated plasma exchange but died 15 days after transplantation. Her clinical course is similar to that of Japanese patients with CADM-ILD. Outside Japan, primary care providers, rheumatologists, and dermatologists, as well as pulmonary physicians, may be less familiar with this disorder than those in Japan. Since CADM-ILD progresses very quickly and could be fatal, these doctors should be aware of this disease to treat such patients as soon as possible, particularly when seeing a patient of Japanese descent.


Similar content being viewed by others
References
Bottai M, Tjarnlund A, Santoni G, Werth VP, Pilkington C, de Visser M, Alfredsson L, Amato AA, Barohn RJ, Liang MH, Singh JA, Aggarwal R, Arnardottir S, Chinoy H, Cooper RG, Danko K, Dimachkie MM, Feldman BM, Garcia-De La Torre I, Gordon P, Hayashi T, Katz JD, Kohsaka H, Lachenbruch PA, Lang BA, Li Y, Oddis CV, Olesinka M, Reed AM, Rutkowska-Sak L, Sanner H, Selva-O'Callaghan A, Wook Song Y, Vencovsky J, Ytterberg SR, Miller FW, Rider LG, Lundberg IE, International Myositis Classification Criteria Project consortium tEr, the Juvenile Dermatomyositis Cohort Biomarker S, Repository (2017) EULAR/ACR classification criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups: a methodology report. RMD Open 3 (2):e000507. https://doi.org/10.1136/rmdopen-2017-000507
Mukae H, Ishimoto H, Sakamoto N, Hara S, Kakugawa T, Nakayama S, Ishimatsu Y, Kawakami A, Eguchi K, Kohno S (2009) Clinical differences between interstitial lung disease associated with clinically amyopathic dermatomyositis and classic dermatomyositis. Chest 136(5):1341–1347. https://doi.org/10.1378/chest.08-2740
Suda T, Fujisawa T, Enomoto N, Nakamura Y, Inui N, Naito T, Hashimoto D, Sato J, Toyoshima M, Hashizume H, Chida K (2006) Interstitial lung diseases associated with amyopathic dermatomyositis. Eur Respir J 28(5):1005–1012
Kang EH, Lee EB, Shin KC, Im CH, Chung DH, Han SK, Song YW (2005) Interstitial lung disease in patients with polymyositis, dermatomyositis and amyopathic dermatomyositis. Rheumatology (Oxford) 44(10):1282–1286
Sato S, Hoshino K, Satoh T, Fujita T, Kawakami Y, Kuwana M (2009) RNA helicase encoded by melanoma differentiation-associated gene 5 is a major autoantigen in patients with clinically amyopathic dermatomyositis: association with rapidly progressive interstitial lung disease. Arthritis Rheum 60(7):2193–2200. https://doi.org/10.1002/art.24621
Moghadam-Kia S, Oddis CV, Sato S, Kuwana M, Aggarwal R (2017) Antimelanoma differentiation-associated gene 5 antibody: expanding the clinical spectrum in North American patients with dermatomyositis. J Rheumatol 44(3):319–325. https://doi.org/10.3899/jrheum.160682
Galimberti F, Li Y, Fernandez AP (2016) Clinically amyopathic dermatomyositis: clinical features, response to medications and malignancy-associated risk factors in a specific tertiary-care-centre cohort. Br J Dermatol 174(1):158–164. https://doi.org/10.1111/bjd.14227
Fiorentino D, Chung L, Zwerner J, Rosen A, Casciola-Rosen L (2011) The mucocutaneous and systemic phenotype of dermatomyositis patients with antibodies to MDA5 (CADM-140): a retrospective study. J Am Acad Dermatol 65(1):25–34. https://doi.org/10.1016/j.jaad.2010.09.016
Hamaguchi Y, Kuwana M, Hoshino K, Hasegawa M, Kaji K, Matsushita T, Komura K, Nakamura M, Kodera M, Suga N, Higashi A, Ogusu K, Tsutsui K, Furusaki A, Tanabe H, Sasaoka S, Muro Y, Yoshikawa M, Ishiguro N, Ayano M, Muroi E, Fujikawa K, Umeda Y, Kawase M, Mabuchi E, Asano Y, Sodemoto K, Seishima M, Yamada H, Sato S, Takehara K, Fujimoto M (2011) Clinical correlations with dermatomyositis-specific autoantibodies in adult Japanese patients with dermatomyositis: a multicenter cross-sectional study. Arch Dermatol 147(4):391–398. https://doi.org/10.1001/archdermatol.2011.52
Sato S, Murakami A, Kuwajima A, Takehara K, Mimori T, Kawakami A, Mishima M, Suda T, Seishima M, Fujimoto M, Kuwana M (2016) Clinical utility of an enzyme-linked immunosorbent assay for detecting anti-melanoma differentiation-associated gene 5 autoantibodies. PLoS One 11(4):e0154285. https://doi.org/10.1371/journal.pone.0154285
Sato S, Hirakata M, Kuwana M, Suwa A, Inada S, Mimori T, Nishikawa T, Oddis CV, Ikeda Y (2005) Autoantibodies to a 140-kd polypeptide, CADM-140, in Japanese patients with clinically amyopathic dermatomyositis. Arthritis Rheum 52(5):1571–1576. https://doi.org/10.1002/art.21023
Li L, Wang Q, Yang F, Wu C, Chen S, Wen X, Liu C, Li Y (2017) Anti-MDA5 antibody as a potential diagnostic and prognostic biomarker in patients with dermatomyositis. Oncotarget 8(16):26552–26564. https://doi.org/10.18632/oncotarget.15716
Li L, Wang Q, Wen X, Liu C, Wu C, Yang F, Zeng X, Li Y (2017) Assessment of anti-MDA5 antibody as a diagnostic biomarker in patients with dermatomyositis-associated interstitial lung disease or rapidly progressive interstitial lung disease. Oncotarget 8(44):76129–76140. https://doi.org/10.18632/oncotarget.19050
Hall JC, Casciola-Rosen L, Samedy LA, Werner J, Owoyemi K, Danoff SK, Christopher-Stine L (2013) Anti-melanoma differentiation-associated protein 5-associated dermatomyositis: expanding the clinical spectrum. Arthritis Care Res (Hoboken) 65(8):1307–1315. https://doi.org/10.1002/acr.21992
Lundberg IE, Tjarnlund A, Bottai M, Werth VP, Pilkington C, de Visser M, Alfredsson L, Amato AA, Barohn RJ, Liang MH, Singh JA, Aggarwal R, Arnardottir S, Chinoy H, Cooper RG, Danko K, Dimachkie MM, Feldman BM, Garcia-De La Torre I, Gordon P, Hayashi T, Katz JD, Kohsaka H, Lachenbruch PA, Lang BA, Li Y, Oddis CV, Olesinska M, Reed AM, Rutkowska-Sak L, Sanner H, Selva-O'Callaghan A, Song YW, Vencovsky J, Ytterberg SR, Miller FW, Rider LG, International Myositis Classification Criteria Project Consortium tER, the Juvenile Dermatomyositis Cohort Biomarker S, Repository (2017) 2017 European League Against Rheumatism/American College of Rheumatology Classification Criteria for adult and juvenile idiopathic inflammatory myopathies and their major subgroups. Arthritis Rheumatol 69(12):2271–2282. https://doi.org/10.1002/art.40320
Kim J, Kim YW, Lee SM, Kim YS, Kim YT, Song YW (2009) Successful lung transplantation in a patient with dermatomyositis and acute form of interstitial pneumonitis. Clin Exp Rheumatol 27(1):168–169
Shoji T, Bando T, Fujinaga T, Okubo K, Yukawa N, Mimori T, Date H (2010) Living-donor lobar lung transplantation for interstitial pneumonia associated with dermatomyositis. Transpl Int 23(5):e10–e11. https://doi.org/10.1111/j.1432-2277.2010.01066.x
Shoji T, Bando T, Fujinaga T, Chen F, Sasano H, Yukawa N, Mimori T, Date H (2013) Living-donor lobar lung transplantation for rapidly progressive interstitial pneumonia associated with clinically amyopathic dermatomyositis: report of a case. Gen Thorac Cardiovasc Surg 61(1):32–34. https://doi.org/10.1007/s11748-012-0106-3
Leclair V, Labirua-Iturburu A, Lundberg IE (2018) Successful lung transplantation in a case of rapidly progressive interstitial lung disease associated with antimelanoma differentiation-associated gene 5 antibodies. J Rheumatol 45(4):581–583. https://doi.org/10.3899/jrheum.171047
Deitchman AR, Kalchiem-Dekel O, Todd N, Reed RM (2019) Rapidly progressive interstitial lung disease due to anti-melanoma differentiation associated protein-5 requiring a bilateral lung transplant, and complicated by kennel cough. Respir Med Case Rep 28:100886. https://doi.org/10.1016/j.rmcr.2019.100886
Acknowledgments
The authors thank the patient’s sister for providing the medical records, radiographs, and lung specimens.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Takada, T., Asakawa, K. & Barrios, R. A Japanese-American female with rapidly progressive interstitial lung disease associated with clinically amyopathic dermatomyositis. Clin Rheumatol 40, 1159–1165 (2021). https://doi.org/10.1007/s10067-020-05292-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05292-0