Abstract
Glucocorticoid monotherapy has been the mainstay treatment of giant cell arteritis (GCA) for decades. We aimed to evaluate the role of leflunomide as a steroid-sparing agent in GCA. This open-label study included incipient GCA patients followed for at least 48 weeks at a single secondary/tertiary rheumatology centre. At the time of diagnosis, patients received glucocorticoids. At week 12 of follow-up, leflunomide 10 mg qd was recommended as an adjunctive therapy to all patients without contraindications. The decision to start the leflunomide was patient-dependent. The number of relapses, a cumulative glucocorticoid dose during follow-up and treatment-related adverse events (AE) were recorded and compared between glucocorticoid-only and leflunomide groups. Seventy-six patients (65.8% female, median (IQR) age 73.7 (66.1–78.8) years) were followed for a median (IQR) 96 (86–96) weeks. Thirty out of 76 (39.5%) patients received leflunomide at week 12 (leflunomide group); the others continued treatment with glucocorticoid (glucocorticoid-only group). During the first 48 weeks of follow-up, 22 patients relapsed, 4 (13.3%) in leflunomide group and 18 (39.1%) in glucocorticoid-only group. The difference was statistically significant (p = 0.02; NNT 3.9 (95% CI 2.2–17.4)). Furthermore, 17/30 (56.7%) patients in the leflunomide group managed to stop glucocorticoid at week 48 (with one relapse (5.9%) shortly afterwards). The cumulative glucocorticoid dose at the last visit was lower in the leflunomide group than in the glucocorticoid-only group (p = 0.01). Our findings indicate the steroid-sparing effect of leflunomide in GCA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Giant cell arteritis (GCA) is the most common primary vasculitis of large and medium-sized arteries in the Western countries [1]. It is a rheumatologic emergency. Early diagnosis and timely initiation of anti-inflammatory treatment can prevent at least some of the severe complications, e.g. permanent loss of vision [2,3,4]. The glucocorticoids, with their quick onset of action, have been the anchor drug in GCA for decades. Unfortunately, almost a half of the patients relapse during the glucocorticoid tapering [4]. The chronic and persistent disease course leads to disease-related damage accrual, and adverse events complicate the prolonged immunosuppressive treatment [5]. Several different conventional synthetic and biologic disease-modifying anti-rheumatic drugs (csDMARDs, bDMARDs) have been investigated for their steroid-sparing effect in GCA. Only tocilizumab has persuasively showed a superior efficacy compared to glucocorticoids [6, 7]. However, bDMARDs are contraindicated in some patients and are associated with a significant cost. Among csDMARDs, methotrexate has been probably the most commonly used in GCA, despite the very modest evidence supporting its use and its relatively slow onset of action [8,9,10]. Even if methotrexate was effective, it is contraindicated in chronic kidney disease, which is common in the population most often affected by GCA.
Leflunomide that has been shown to be effective and safe not only in rheumatoid arthritis, but also in systemic vasculitides, e.g. granulomatosis with polyangiitis and Takayasu arteritis, was never formally studied in GCA [11,12,13,14]. It has shown promise in two case series of relapsing or persistently active GCA or polymyalgia rheumatica [15, 16]. In both, the clinical and laboratory response to leflunomide was swift, present already in a median of 2 and 3 months, respectively, and enabled a glucocorticoid dose reduction or even discontinuation. A recent meta-analysis of GCA treatments did not emphasise the role of leflunomide [17].
To date, no study has explored the effectiveness of leflunomide as a part of a treatment plan in an incipient GCA population. Our main objective was to assess the glucocorticoid-sparing potential of leflunomide in new-onset GCA and then also explore its safety profile.
Methods
Setting
This prospective observational study was performed at the Department of Rheumatology, University Medical Centre Ljubljana, a secondary/tertiary level teaching hospital, using our previously described, fast-track protocol that was implemented over 6 years ago [4]. Most of the GCA cases from the region representing approximately a half of the Slovenian population are managed at our department.
Patients
We included patients diagnosed with GCA between July 2014 and December 2016. The diagnosis of GCA was based on the corresponding clinical and laboratory features, and the positive result of a temporal artery biopsy (TAB) or colour Doppler sonography (CDS) or positron emission tomography/computed tomography (PET/CT).
Baseline evaluation and follow-up
Baseline patient work-up included a thorough history of the GCA symptoms, comorbidities, a complete physical examination, extensive laboratory and imaging tests or TAB.
Follow-up visits with predetermined clinical and laboratory tests were performed at 4, 12, 24, 48, 54 (± 2), and at 96 (± 2) weeks after diagnosis by two rheumatologists (AH or RJ). Additional unscheduled visits were arranged for patients who relapsed during the glucocorticoid tapering, or after glucocorticoid discontinuation.
We recorded the number of relapses during the first 48 weeks of treatment, as well as a cumulative glucocorticoid dose for each patient at the last follow-up visit.
Treatment strategy and patient stratification
In line with the EULAR recommendations, we started treating all the patients with glucocorticoids at the time of the GCA diagnosis [18]. The initial dose of oral methylprednisolone was 0.8 mg/kg body weight qd, but no less than 32 mg qd and no more than 48 mg qd. The patients with cranial GCA complicated by ischaemic complications, e.g. visual disturbances, and all those with extracranial large vessel GCA additionally received methylprednisolone 250 mg intravenously for three consecutive days prior to oral methylprednisolone.
The glucocorticoid tapering was started after 2 to 4 weeks. The dose was reduced by 4 mg weekly down to 16 mg qd, then 2 mg each other week down to 8 mg qd, then 1 mg monthly down to maintenance dose 4 mg qd. At week 48, we discontinued the glucocorticoids in patients in the leflunomide group who were in remission during the first 48 weeks of follow-up. The patients in the leflunomide group with a relapse and those who chose to remain in the glucocorticoid-only group continued the treatment with the lowest effective glucocorticoid dose even after week 48.
At week 12, the add-on therapy with leflunomide 10 mg qd was proposed to all patients without contraindications for leflunomide (e.g. liver failure, bone marrow suppression). The final decision for the treatment with leflunomide was brought by each patient alone.
If GCA relapsed, i.e. worsened during the glucocorticoid taper after an initial remission, the methylprednisolone was temporary increased by 8–12 mg qd on top of the last previously effective dose and leflunomide (10 mg qd) was added in the patients who were not already on it. In patients that relapsed while on both methylprednisolone and leflunomide, the methylprednisolone dose was increased as described above and the dose of leflunomide was escalated from 10 to 20 mg qd. Leflunomide was replaced with methotrexate 15 mg weekly in the patients with active vasculitis and an adverse event attributable to leflunomide, or if leflunomide 20 mg qd was ineffective.
Adverse events
We meticulously recorded any adverse events with a particular focus on the following 16 adverse events attributable to either glucocorticoids or leflunomide: severe infections (defined as the need for antibiotic therapy or hospital admission), skin bruises, skin ulcers, steroid diabetes, steroid myopathy, osteoporotic fracture, cataracts, hair loss, weight loss, diarrhoea, significant increase of blood pressure (with the need to increase antihypertensive therapy), bone marrow toxicity, leflunomide-induced pneumonitis, skin rash and polyneuropathy.
Statistical analysis
As described above, the patients were stratified into glucocorticoid-only and leflunomide groups. The categorical variables were summarised as medians and interquartile ranges or means with their standard deviations and the categorical values as percentages. To test for differences between the observed groups, we used the Mann-Whitney test for metric, and the Fisher’s exact test for categorical variables. MedCalc Version 12.2 was used for the statistical analyses.
Ethics committee approval
The study was approved by the Slovenian National Medical Ethics Committee.
Results
Baseline patient characteristics and treatment
During the 30-month period, we identified 85 new GCA cases. The nine patients who died before the week 48 of the follow-up were excluded from the analysis. Three of these patients succumbed to a stroke, five to infection and one committed suicide. Three of these nine patients were treated with both glucocorticoids and leflunomide, and the remaining six with glucocorticoids only.
The baseline demographic and clinical characteristics of the 76 patients (67% female), who were followed for at least 48 weeks, are presented in Table 1, column A. Their median age (IQR) was 73.3 (66.1–78.8) years and the median (IQR) disease duration time was 30 (21–60) days. Forty-one (53.9%) patients had cranial GCA, and the others extracranial large vessel involvement. Forty-three (56.6%) patients initially received an intravenous methylprednisolone pulse. The mean (SD) starting dose of oral methylprednisolone was 47 (6) mg qd, or 0.7 (0.1) mg/kg body weight qd.
Follow-up and patient stratification
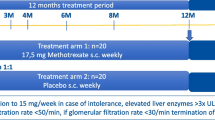
At week 12, 30 (39.5%) patients started leflunomide 10 mg qd (i.e. the leflunomide group) and 46 (60.5%) patients chose not to (i.e. the glucocorticoid-only group) as depicted in Fig. 1. There were no significant differences in the baseline characteristics between the leflunomide and glucocorticoid-only groups (Table 1, columns B and C). During the median (IQR) follow-up of 96 (86–96) weeks, 22 (28.9%) patients relapsed. The median (IQR) time to relapse was 26 (13–30) weeks and the median (IQR) methylprednisolone dose at relapse 6 (4–12) mg qd. Four (13.3%) and 18 (39.1%) patients relapsed in the leflunomide and glucocorticoid-only groups, respectively (Fig. 1). The difference in the relapse rates between the groups was significant (p = 0.020), with the number needed to treat (NNT) for leflunomide of 3.9 (95% CI 2.2–17.4) in the per protocol analysis. However, the significance was lost in the intention to treat analysis (p = 0.50).
Relapses in the glucocorticoid-only group were treated with increased doses of glucocorticoids and the addition of leflunomide in 12 patients or methotrexate in one patient. One patient from the leflunomide group stopped leflunomide due to ineffectiveness defined as the second relapse after leflunomide was increased 20 mg qd per protocol.
At week 48, the glucocorticoids were discontinued in 17/30 (56.7%) patients in the leflunomide group. One patient (5.9%) relapsed shortly thereafter, and the other 16 (53.3%) remained in remission up until their last follow-up visit.
At the last follow-up visit, there was a significant difference between the cumulative glucocorticoid doses in the leflunomide and glucocorticoid-only groups (4390 (4132–5558) mg, vs. 5340 (4652–5792) mg, p = 0.01).
Adverse events
Sixty-four (84.2%) patients developed at least one of the listed treatment-related adverse events. We observed 164 adverse events (Table 2, column A). One hundred twenty-five (76.2%) adverse events were attributed solely to glucocorticoids and 18 (11.0%) to leflunomide alone. Twenty-one (12.8%) adverse events were attributable to the combination of glucocorticoids and leflunomide.
Seven (23.3%) patients from the leflunomide group stopped leflunomide due to one or more adverse events: four had hair loss, two had diarrhoea, two lost weight and one had elevated liver enzymes. The only adverse event that was significantly more common in the leflunomide group was hair loss with 40.0% vs. 14.7% in the glucocorticoid-only group, p = 0.030. The patients recovered after stopping leflunomide. None of the patients experienced bone marrow toxicity, pneumonitis or polyneuropathy.
Interestingly, severe infections were numerically but not statistically significantly lower in the leflunomide group than in the glucocorticoid-only group (13.3 vs. 29.4%). The frequencies of adverse events are shown in Table 2, columns B and C.
Discussion
The management of GCA remains challenging, despite our better understanding of the disease pathogenesis, improved diagnostic possibilities, utilisation of the fast-track protocols and recently approved biologic therapy. Unanswered questions like the best initial treatment regimen in GCA, the length of GCA treatment and the optimal way to handle a persistent/relapsing disease make daily practice difficult. The glucocorticoids have been the mainstay therapy for decades and only recently tocilizumab was shown to be effective and glucocorticoid sparing [7, 10]. Other conventional synthetic disease-modifying anti-rheumatic drugs, e.g. methotrexate, have been tried as glucocorticoid-sparing therapies in GCA without much success [8, 19]. Leflunomide, which is effective and safe in patients with rheumatoid arthritis and also in selected vasculitides, has been thus far largely ignored in GCA although it may have therapeutic implications in GCA since it inhibits dendritic cell maturation as well as monocyte and lymphocyte activation and also the production of several cytokines, including tumour necrosis factor alpha and interleukins (ILs) IL-2, IL-6 and IL-12, and of metalloproteinases (MMP 1, MMP 3, MMP 9), which were all implicated in the pathogenesis of GCA [20,21,22,23].
The presented study is the first ever to assess the potential therapeutic role of leflunomide in an incipient GCA population. We focused on its potential steroid-sparing effect and paid a close attention to its safety. In an intention to treat analysis, we found no significant difference in terms of effectiveness between the glucocorticoid-only and leflunomide groups. However, in patients who tolerated leflunomide, its addition to the standard glucocorticoid therapy significantly decreased the frequency of relapses, with a NNT of approximately four patients at a significantly lower cumulative glucocorticoid dose at week 96. The majority of our GCA patients who were treated with leflunomide remained in remission even after discontinuation of glucocorticoids at week 48. This effect was reached already at the initial leflunomide dose of 10 mg qd. Low-dose leflunomide was previously found to be effective, with a rapid onset of response, in the two case series on difficult to treat GCA [15, 16]. Although leflunomide was well tolerated in our cohort, seven (23.3%) patients discontinued leflunomide due to one or more adverse events. This was comparable to the 25% drop-out due to adverse events in the studies in rheumatoid arthritis, bearing in mind that in those, the discontinuation rate correlated with a higher loading dose of leflunomide [24]. Considering that hair loss was the most common adverse event associated with leflunomide, and there were no cases of serious adverse events, e.g. leflunomide-related pneumonitis or leflunomide hypersensitivity reactions, we speculate that the risk of persistent and relapsing GCA and prolonged treatment with glucocorticoids in monotherapy outweigh the risk of the leflunomide-related toxicity. Also, while we discontinued leflunomide due to hair loss, glucocorticoids were not discontinued in spite of their adverse events, even hair loss. Supporting this view, the frequency of serious infections was lower in the leflunomide group than in the glucocorticoid-only group, suggesting that serious infections are mainly driven by prolonged glucocorticoid use and the higher cumulative dose of glucocorticoids in the glucocorticoid-only group. This difference was however not statistically significant.
The main strength of our study is its external validity since it provides an insight into an alternative management option for the most common adult vasculitis by means of a prospective inclusion of an unselected real-world GCA population managed following a pre-defined systematic treatment and follow-up plan. Its single-centre, open-label design and the relatively small sample size preclude drawing any firm conclusions, but the observations nonetheless suggests that the addition of leflunomide to the standard glucocorticoid regimen may at least warrant a more formal evaluation.
In conclusion, in our open-label study, adding leflunomide to the EULAR-recommended glucocorticoid regimen in GCA showed promise in reducing the relapse rate at a lower cumulative glucocorticoid dose in over three quarters of patients who tolerated the therapy.
References
Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, Flores-Suarez LF, Gross WL, Guillevin L, Hagen EC, Hoffman GS, Jayne DR, Kallenberg CG, Lamprecht P, Langford CA, Luqmani RA, Mahr AD, Matteson EL, Merkel PA, Ozen S, Pusey CD, Rasmussen N, Rees AJ, Scott DG, Specks U, Stone JH, Takahashi K, Watts RA (2013) 2012 revised international Chapel Hill consensus conference nomenclature of vasculitides. arthritis rheum 65:1–11. https://doi.org/10.1002/art.37715
Patil P, Williams M, Maw WW, Achilleos K, Elsideeg S, Dejaco C, Borg F, Gupta S, Dasgupta B (2015) Fast track pathway reduces sight loss in giant cell arteritis: results of a longitudinal observational cohort study. Clin Exp Rheumatol 33:S-103–S-106
Diamantopoulos AP, Haugeberg G, Lindland A, Myklebust G (2016) The fast-track ultrasound clinic for early diagnosis of giant cell arteritis significantly reduces permanent visual impairment: towards a more effective strategy to improve clinical outcome in giant cell arteritis? Rheumatology (Oxford) 55:66–70. https://doi.org/10.1093/rheumatology/kev289
Hocevar A, Rotar Z, Jese R, Semrl SS, Pizem J, Hawlina M, Tomsic M (2016) Do early diagnosis and glucocorticoid treatment decrease the risk of permanent visual loss and early relapses in giant cell arteritis: a prospective longitudinal study. Medicine (Baltimore) 95:e3210. https://doi.org/10.1097/MD.0000000000003210
Kermani TA, Sreih AG, Cuthbertson D, Carette S, Hoffman GS, Khalidi NA, Koening CL, Langford CA, McAlear CA, Monach PA, Moreland L, Pagnoux C, Seo P, Warrington KJ, Ytterberg SR, Merkel PA, Vasculitis Clinical Research C (2018) Evaluation of damage in giant cell arteritis. Rheumatology (Oxford) 57:322–328. https://doi.org/10.1093/rheumatology/kex397
Kermani TA, Dasgupta B (2017) Current and emerging therapies in large-vessel vasculitis. Rheumatology (Oxford). https://doi.org/10.1093/rheumatology/kex385
Villiger PM, Adler S, Kuchen S, Wermelinger F, Dan D, Fiege V, Butikofer L, Seitz M, Reichenbach S (2016) Tocilizumab for induction and maintenance of remission in giant cell arteritis: a phase 2, randomised, double-blind, placebo-controlled trial. Lancet 387:1921–1927. https://doi.org/10.1016/S0140-6736(16)00560-2
Mahr AD, Jover JA, Spiera RF, Hernandez-Garcia C, Fernandez-Gutierrez B, Lavalley MP, Merkel PA (2007) Adjunctive methotrexate for treatment of giant cell arteritis: an individual patient data meta-analysis. Arthritis Rheum 56:2789–2797. https://doi.org/10.1002/art.22754
Hoffman GS, Cid MC, Hellmann DB, Guillevin L, Stone JH, Schousboe J, Cohen P, Calabrese LH, Dickler H, Merkel PA, Fortin P, Flynn JA, Locker GA, Easley KA, Schned E, Hunder GG, Sneller MC, Tuggle C, Swanson H, Hernandez-Rodriguez J, Lopez-Soto A, Bork D, Hoffman DB, Kalunian K, Klashman D, Wilke WS, Scheetz RJ, Mandell BF, Fessler BJ, Kosmorsky G, Prayson R, Luqmani RA, Nuki G, McRorie E, Sherrer Y, Baca S, Walsh B, Ferland D, Soubrier M, Choi HK, Gross W, Segal AM, Ludivico C, Puechal X, International Network for the Study of Systemic V (2002) A multicenter, randomized, double-blind, placebo-controlled trial of adjuvant methotrexate treatment for giant cell arteritis. Arthritis Rheum 46:1309–1318. https://doi.org/10.1002/art.10262
Stone JH, Klearman M, Collinson N (2017) Trial of tocilizumab in giant-cell arteritis. N Engl J Med 377:1494–1495. https://doi.org/10.1056/NEJMc1711031
Metzler C, Miehle N, Manger K, Iking-Konert C, de Groot K, Hellmich B, Gross WL, Reinhold-Keller E, German Network of Rheumatic D (2007) Elevated relapse rate under oral methotrexate versus leflunomide for maintenance of remission in Wegener’s granulomatosis. Rheumatology (Oxford) 46:1087–1091. https://doi.org/10.1093/rheumatology/kem029
Metzler C, Fink C, Lamprecht P, Gross WL, Reinhold-Keller E (2004) Maintenance of remission with leflunomide in Wegener’s granulomatosis. Rheumatology (Oxford) 43:315–320. https://doi.org/10.1093/rheumatology/keh009
de Souza AW, da Silva MD, Machado LS, Oliveira AC, Pinheiro FA, Sato EI (2012) Short-term effect of leflunomide in patients with Takayasu arteritis: an observational study. Scand J Rheumatol 41:227–230. https://doi.org/10.3109/03009742.2011.633553
de Souza AW, de Almeida AR, de Cinque AH, Oliveira PB, Pinheiro FA, Oliveira AC, Sato EI (2016) Leflunomide in Takayasu arteritis - a long term observational study. Rev Bras Reumatol Engl Ed 56:371–375. https://doi.org/10.1016/j.rbre.2016.02.003
Adizie T, Christidis D, Dharmapaliah C, Borg F, Dasgupta B (2012) Efficacy and tolerability of leflunomide in difficult-to-treat polymyalgia rheumatica and giant cell arteritis: a case series. Int J Clin Pract 66:906–909. https://doi.org/10.1111/j.1742-1241.2012.02981.x
Diamantopoulos AP, Hetland H, Myklebust G (2013) Leflunomide as a corticosteroid-sparing agent in giant cell arteritis and polymyalgia rheumatica: a case series. Biomed Res Int 2013:120638–120633. https://doi.org/10.1155/2013/120638
Berti A, Cornec D, Medina Inojosa JR, Matteson EL, Murad MH (2018) Treatments for giant cell arteritis: meta-analysis and assessment of estimates reliability using the fragility index. Semin Arthritis Rheum. https://doi.org/10.1016/j.semarthrit.2017.12.009
Mukhtyar C, Guillevin L, Cid MC, Dasgupta B, de Groot K, Gross W, Hauser T, Hellmich B, Jayne D, Kallenberg CG, Merkel PA, Raspe H, Salvarani C, Scott DG, Stegeman C, Watts R, Westman K, Witter J, Yazici H, Luqmani R, European Vasculitis Study G (2009) EULAR recommendations for the management of large vessel vasculitis. Ann Rheum Dis 68:318–323. https://doi.org/10.1136/ard.2008.088351
Yates M, Loke YK, Watts RA, MacGregor AJ (2014) Prednisolone combined with adjunctive immunosuppression is not superior to prednisolone alone in terms of efficacy and safety in giant cell arteritis: meta-analysis. Clin Rheumatol 33:227–236. https://doi.org/10.1007/s10067-013-2384-2
Kirsch BM, Zeyda M, Stuhlmeier K, Grisar J, Smolen JS, Watschinger B, Stulnig TM, Horl WH, Zlabinger GJ, Saemann MD (2005) The active metabolite of leflunomide, A77 1726, interferes with dendritic cell function. Arthritis Res Ther 7:R694–R703. https://doi.org/10.1186/ar1727
Fragoso YD, Brooks JB (2015) Leflunomide and teriflunomide: altering the metabolism of pyrimidines for the treatment of autoimmune diseases. Expert Rev Clin Pharmacol 8:315–320. https://doi.org/10.1586/17512433.2015.1019343
Elkayam O, Yaron I, Shirazi I, Judovitch R, Caspi D, Yaron M (2003) Active leflunomide metabolite inhibits interleukin 1beta, tumour necrosis factor alpha, nitric oxide, and metalloproteinase-3 production in activated human synovial tissue cultures. Ann Rheum Dis 62:440–443
Litinsky I, Paran D, Levartovsky D, Wigler I, Kaufman I, Yaron I, Yaron M, Caspi D, Elkayam O (2006) The effects of leflunomide on clinical parameters and serum levels of IL-6, IL-10, MMP-1 and MMP-3 in patients with resistant rheumatoid arthritis. Cytokine 33:106–110. https://doi.org/10.1016/j.cyto.2005.12.009
Alcorn N, Saunders S, Madhok R (2009) Benefit-risk assessment of leflunomide: an appraisal of leflunomide in rheumatoid arthritis 10 years after licensing. Drug Saf 32:1123–1134. https://doi.org/10.2165/11316650-000000000-00000
Funding
The authors would like to acknowledge funding from the Slovenian Research Agency (ARRS) for the National Research Program P3-0314.
Author information
Authors and Affiliations
Contributions
All the authors have accepted responsibility for the entire content of this submitted manuscript and approved submission.
Corresponding author
Ethics declarations
This study was conducted as part of the National Research Program (#P3-0314) and has been approved by the Slovenian Ethical Committee. It has therefore been performed in accordance with the ethical standards laid down in 1964 Declaration of Helsinki and its later amendments. Informed consent was obtained from all individuals included in this study.
Disclosures
None.
Additional information
Rheumatology in Slovenia: Clinical practice and translational research
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Hočevar, A., Ješe, R., Rotar, Ž. et al. Does leflunomide have a role in giant cell arteritis? An open-label study. Clin Rheumatol 38, 291–296 (2019). https://doi.org/10.1007/s10067-018-4232-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-018-4232-x