Abstract
The objective of the study was to analyze the prognostic factors of radiographic progression in a series of patients with early rheumatoid arthritis (RA) after 2 years of therapy with a structured algorithm using disease-modifying antirheumatic drugs (DMARDs) and very low doses of oral glucocorticoids. One hundred and five patients (81% female) with early RA (disease duration <2 years) treated with the same therapeutic protocol using gold salts and methotrexate in a step-up strategy, together with methylprednisolone (4 mg/day), were followed up for 2 years. The outcome variable was radiographic progression after 2 years of DMARD therapy using the modified Larsen method. Clinical, biological, immunogenetic, and radiographic data were analyzed at study entry and after 1 and 2 years of follow-up. Radiographic progression (increase of four or more units in the Larsen score) was observed in 32% of patients after 2 years of follow-up. The percentage of erosive disease increased from 18.3% at baseline to 28.9% at 12 months and 44.6% at 24 months, in spite of a significant improvement in disease activity. New erosions appeared in 33% of patients after 2 years. Several baseline parameters were associated with radiographic progression in the univariate analysis: shared epitope (SE) homozygozity, HLA-DRB*04 alleles, female gender, hemoglobin, erythrocyte sedimentation rate, and anticyclic citrullinated peptide antibodies (anti-CCP). In the multivariate analysis, female gender [odds ratio (OR) 5.5, 95% confidence interval (CI): 1.1–28.2, p = 0.04], DRB1*04 alleles (OR 3.1, 95% CI 1.1–9, p = 0.03) and, marginally, anti-CCP antibodies (OR 3.6, 95% CI 0.9–14.5, p = 0.06), were associated with progression. Female patients with both DRB1*04 alleles and anti-CCP antibodies showed the highest scores in radiographic progression. The presence, but not the titer, of anti-CCP antibodies predicted progression. The positive predictive value of the multivariate model for progression was only 53.9% whereas the negative predictive value was 80.3%. In a series of early RA patients treated with a structured algorithm using DMARDs and very low doses of glucocorticoids, radiographic progression was observed in one third of patients after 2 years. Female gender, DRB1*04 alleles (rather than the SE), and the presence of anti-CCP antibodies at baseline (independently of the titer) were the most important predictors of progression. The utility of these parameters in clinical practice is limited by their relatively low positive predictive value.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is a systemic chronic inflammatory disease of unknown etiology associated with progressive joint destruction and disability, together with relevant social and economics costs [1]. Radiographic joint damage is considered one of the most important outcome measures in RA [2], with the erosive changes that appear early in the disease course [3] being considered predictors of poor prognosis in the long-term [4]. Current therapeutic strategies in RA are directed at preventing progressive joint destruction [5].
The clinical course of RA is variable, and the rate of radiographic progression differs between patients. Various studies have attempted to identify prognostic factors of radiographic progression in patients with early RA. These studies have found that various factors, including serum autoantibodies [rheumatoid factor (RF)] [6, 7], anticyclic citrullinated peptide (anti-CCP) antibodies [8, 9], HLA-DRB1 genotype [10, 11], or elevated inflammatory activity [12] are associated with worse radiographic outcome, although controversy remains, as there was no absolute agreement between studies. However, in these studies, patients were not treated with a standardized structured therapeutic strategy, making it difficult to elucidate the possible influence of the type of antirheumatic therapy on the rate of radiographic progression. Recently, we presented our preliminary data on a 1-year radiographic progression in a cohort of early RA patients after the introduction of a structured therapeutic algorithm with disease-modifying antirheumatic drugs (DMARDs) and low doses of glucocorticoids in a clinical setting [13]. The present study investigates the baseline prognostic factors of radiographic progression in a series of 105 Spanish patients with early RA 2 years after the introduction of this therapeutic strategy.
Materials and methods
Patients
Patients who fulfilled the American College of Rheumatology (ACR, formerly the American Rheumatism Association) [14] criteria for the classification of RA, with symptoms of <24 months, were enrolled in this study. All were outpatients attending the rheumatology units of the Hospital Clinic of Barcelona or the Hospital Parc Tauli of Sabadell between 1998 and 2003, and were followed for 2 years. Patients who were treated previously with DMARDs or prednisone or equivalent at a dose of >10 mg/day were excluded. The study was approved by the Hospital Clinic ethics committee.
Study design
We conducted a prospective open-label study where all patients were treated according to a therapeutic protocol, with early introduction of DMARDs using a step-up approach. In all cases, intramuscular sodium aurothiomalate at a dose of 50 mg/week (25 mg/week during the first 2 weeks) was prescribed as the first-choice DMARD together with methylprednisolone 4 mg/day. Nonsteroidal anti-inflammatory drugs and intraarticular steroid therapy were used according to clinical judgment. Methotrexate at an increasing dose of 7.5 to 20 mg was begun if adverse effects without clinical improvement or no ACR20 response were observed at month 6. If an ACR50 response at 6 months was observed, gold salts were scheduled every 2–3 weeks, but if a patient had an ACR20 response but no ACR50 response, combination therapy with sodium aurothiomalate and methotrexate was initiated. Glucocorticoid therapy was tapered according to clinical judgment. After the first year of therapy, patients were treated without an established protocol algorithm and according to the criteria of the treating physician, but with an aggressive approach using other DMARDs in monotherapy or in combination in cases with a poor response to previous DMARDs. Biological therapy was initiated in a few cases in patients with a poor response to DMARDs.
Disease activity was assessed at 0, 3, 6, 12, 18, and 24 months. At study entry, demographic characteristics, disease duration, serum RF determined by nephelometry (NV < 25 UI/l), anti-CCP antibodies measured by a second-generation ELISA test (Immunoscan RA, Eurodiagnostica, distributed by Diasorin, Madrid, Spain; NV < 50 UI/l), and HLA-DRB1 genotype determined by direct DNA sequencing were analyzed. At baseline, 6, 12, 18, and 24 months, we recorded the following parameters: pain using a visual analog scale (VAS), the 28 tender and swollen joint count, patient and physician assessment of disease status, the 28-joint disease activity score (DAS28), functional status using the modified Health Assessment Questionnaire (mHAQ) [15], hemoglobin, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) determined by nephelometry.
Radiographic assessment
Radiographies of hands and feet were obtained at baseline and after 12 and 24 months of follow-up. The modified Larsen method was used to evaluate radiographic damage; 32 joints were assessed with the scores ranging from 0 to 200; each wrist was considered a unit and its score was multiplied by 5 [16]. An erosion joint count (EJC), defined as the number of joints with any cortical erosion out of the 32 joints evaluated, was also done. All radiographs were read by the same observer (RS) in chronological order. The minimal clinically important difference was used as a measure of radiographic progression [17]. Using this approach, a change of two or more units in the Larsen score was considered as indicative of progression after 1 year in early RA. Therefore, in this study, definite radiographic progression was defined as an increase of four or more units in the Larsen score between baseline and 24 months. The appearance of new erosions (increase in the EJC) was also evaluated.
Statistical analysis
The statistical analysis was performed using the STATA statistical program, version 8.2. The outcome measure was radiographic progression measured by the Larsen method, as previously defined. The univariate analysis of categorical variables used the chi-square test or Fisher’s exact test and continuous variables were assessed with the Student t-test or the Mann–Whitney test, when appropriate. For paired samples, the t-test or Wilcoxon test were used. For multiple group comparisons, one-way analysis of variance or the Kruskal–Wallis test was performed. All marginally significant variables (p < 0.25) in the univariate analysis were entered into the multivariate analysis (stepwise logistic regression model) as independent variables. The sensitivity, specificity, and positive and negative predictive values of the final multivariate model were also analyzed. For all tests, p values less than or equal to 0.05 were considered significant.
Intraobserver agreement in the radiographic Larsen score was assessed with a k-statistic on 25 randomly chosen pairs of hand and foot radiographs; the k value was 0.77 [confidence interval (CI) 0.61–0.93].
Results
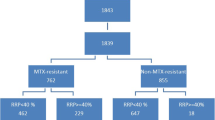
One hundred and fifteen patients were initially enrolled. Ten patients did not complete the 2-year follow-up for varying reasons: irregular or lost follow-up (six patients), death (two patients), transfer out (one patient), and doubts about disease duration (one patient). The final cohort included 105 patients whose hands and feet radiographs at 0 and 24 months were available in 100 patients (in 104 patients at baseline, in 97 patients at 1 year, and in 101 patients at 2 years). Baseline characteristics of the 105 patients are shown in Table 1. Eighty-one percent of the patients were female. The majority of patients had RF and anti-CCP antibodies in their sera. In 73 patients (69.5%) the disease duration was <1 year. Most patients (75.7%) presented high disease activity (DAS28 > 5.1) at study entry, which decreased significantly after 1 and 2 years (19.6 and 15.2%, respectively, p < 0.001). At 1 year, ACR20 and ACR50 responses were achieved by 73.3 and 44.8% of the patients, respectively. After 2 years, the percentages of ACR 20 and ACR50 responses were 73.3 and 55.2%, respectively. European League Against Rheumatism (EULAR) response (good or moderate) criteria were achieved by 78% of the patients at month 12 and by 81.9% of the patients at month 24 (Table 2). Drug treatment at 6, 12, and 24 months is shown in Fig. 1. After 2 years, sodium aurothiomalate was taken by 41 patients. The reasons for withdrawal of gold were inefficacy (28 patients) or adverse events (22 patients), mucocutaneous side-effects, 12 patients; proteinuria, 7 patients; and others, 3 patients. After 2 years, 62.5% of the patients were still taking oral glucocorticoids at a mean daily dose of methylprednisolone of 2.3 ± 2.5 mg/day. During the follow-up, 18 patients received DMARDs other than gold or methotrexate and 10 patients received biological therapy; in all but one of these patients, TNF-alpha blockers were initiated during the second year of follow-up.
Drug therapies administered at 6, 12, and 24 months of follow-up. *Other DMARDs combined with methotrexate (MTX) different from gold. **Leflunomide n = 1, infliximab n = 1. §Leflunomide n = 1, cyclosporine A n = 4, infliximab n = 5, etanercept n = 1, adalimumab n = 1, hydroxychloroquine n = 1. ‡Leflunomide n = 1. ¶Leflunomide n = 6, leflunomide + infliximab n = 2, etanercept n = 1, cyclosporine A n = 1, hydroxychloroquine n = 1
Radiographic outcome
Erosions were observed at study entry in 19 patients (18.3%), in 28 patients (28,9%) at month 12, and in 45 patients (44.6%) at month 24. After 2 years, mean EJC and Larsen scores increased from 0.4 ± 0.9 to 1 ± 1.4 and from 1.2 ± 2.7 to 6.1 ± 9.3, respectively. Two-year radiographic progression occurred in 32 out of 100 patients (32%), as previously defined. New hand or foot erosions were observed in 33% of the patients.
Prognostic markers of radiographic progression
In the univariate analysis, the following clinical and biological parameters were significantly associated with Larsen radiographic progression: hemoglobin, ESR, female gender, shared epitope (SE), SE homozygozity, HLA-DRB1*04 genotype, and anti-CCP antibodies. The highest odds ratios (OR) were observed with SE homozygozity, female gender, anti-CCP antibodies, and HLA-DRB1*04 alleles. A marginal significance was also observed for RF and mHAQ (Table 3).
In the multiple regression analysis, the final model included only female gender (OR 5.5) and DRB1*04 alleles (OR 3.1) as independent factors associated with Larsen radiographic progression. The presence of anti-CCP antibodies was also marginally associated with progression (OR 3.6, p = 0.06) (Table 4). The sensitivity and specificity of this multivariate model were 53.9 and 81.7%, respectively, whereas the positive predictive value and the negative predictive value were 56 and 80.3%, respectively.
To elucidate which combination of variables selected for the multivariate model were associated with greater radiographic Larsen progression, different combination groups were analyzed. The mean change in Larsen score was 8.7 ± 12 in female patients with both anti-CCP (+) and DRB1*04 (+) (n = 25), 3 ± 4.8 in female patients with anti-CCP (+) and DRB1*04 (−) (n = 23), and only 1.1 ± 2 (p < 0.01) in females with both anti-CCP (−) and DRB1*04 (−) (n = 17). The other combination groups yielded an insufficient sample size for analysis.
To analyze whether the titer of baseline anti-CCP antibodies were relevant in determining radiographic progression, we compared the values of these antibodies in anti-CCP positive patients with and without Larsen progression; the median values of anti-CCP antibodies in patients with radiographic progression were not significantly different to those of patients without progression [628 UI/l (C25/C75, 247:1,600) vs 750 UI/l (C25/C75, 247:1,600), p = 0.68].
Finally, when the EJC (evidence of one or more new erosions after 2 years) was used as a criteria of radiographic progression, only the presence of two copies of the SE (p < 0.05) and the presence of anti-CCP antibodies (p = 0.05) were significantly associated with progression.
Discussion
This study, together with other studies focusing on progression of radiographic damage in early RA after the introduction of DMARDs [6–10, 18, 19], clearly shows that early introduction of a therapeutic strategy with DMARDs in recent-onset RA improves clinical and biological parameters of disease activity, but does not prevent radiographic progression in a significant proportion of patients. Patients with erosive disease increased from 18.3 to 44.6% and the Larsen score increased to a mean of almost five points after 2 years. Larsen radiographic progression was observed in 32% of patients, in spite of the use of DMARDs and very low dose of glucocorticoids. However, in our cohort of RA patients, more than half still had nonerosive disease after 2 years of follow-up.
Our results are in agreement with those observed in the prospective study by Combe et al. [18] in Mediterranean patients with early RA, which found that, using the modified Sharp–van der Heijde method and the smallest statistical difference as the measure of progression, the rate of progression was 41.3% after 3 years of DMARD therapy. However, in this and other studies analyzing prognostic factors of radiological progression in early RA [18–21], patients were treated with different DMARDs without a structured therapeutic strategy, making it difficult to establish the possible influence of the antirheumatic drug therapy on disease progression. It is known that the effects of different DMARDs on radiographic damage may differ, even after an apparently similar clinical benefit [22]. In contrast, our patients were treated with the same therapeutic algorithm, with gold salts as the first DMARD and with methotrexate in monotherapy or in combination when a partial or no response was achieved or when there were adverse events to gold. Although the use of aurothiomalate in RA has declined significantly in recent years, its effects on radiographic progression are well established and are similar to those of methotrexate [23].
To our knowledge, there is only one reported study focusing on radiographic progression in RA using a structured therapeutic algorithm. In this study in an early RA-based population and using hydroxychloroquine in monotherapy as the first DMARD, with surprising results on clinical efficacy, Goronzy et al. [24] found a prevalence of radiographic progression (defined as the appearance off new erosions) of 52% after 2 years, a higher figure than that observed in our cohort (33%) using the same criteria. The different therapeutic strategy employed by of Goronzy et al. using antimalarials, which have a modest effect on the prevention of structural damage [25], as the first-choice DMARD, and the systematic use of very low doses of glucocorticoids, which were shown to retard radiographic progression [26], in our cohort, may explain the differences.
The present study clearly shows that there are several prognostic factors of radiographic progression in early RA. Three parameters emerged as the most important predictors of progression: female gender, the HLA-DRB1 genotype (DRB*04 allele and SE homozygozity rather than the SE itself), and the presence of anti-CCP antibodies. Other parameters often associated with worse radiographic outcome, such as disease activity measured by clinical or laboratory tests [12], were not found to be predictors of radiographic damage. Women had greater radiographic progression than men, as observed in other studies [20, 27], although others reports only found a nonsignificant trend [18, 24]. We also found that patients with HLADRB1*04 alleles or with SE homozygozity had greater joint destruction than patients with other genotypes [10, 11, 28]; this finding were also observed in Mediterranean populations [29], where the course of RA is reported to be more benign [30]. We have confirmed that the SE is associated with significant joint damage progression only when included in DRB1*04 alleles (or in the presence of homozygozity), but not when included in other DRB1 genotypes such as DRB1*01 alleles.
RF is one of the most powerful predictors of joint damage in early RA populations in most [6, 7, 10, 18, 21] but not all studies [20]; however, in our study, although a trend was evident with an OR of 3, a risk very similar to those observed in other studies [31], the association with progression was not significant. In contrast, the presence of anti-CCP antibodies at baseline was associated with radiographic progression. Recent studies of anti-CCP antibodies have also shown that these antibodies are not only very useful diagnostic markers of RA in patients with early arthritis due to their high specificity [32], but are also associated with poor radiological outcome in RA patients [8, 9]. Recent reports confirm the prognostic significance of these antibodies in early RA to be even greater than RF [33, 34]. Berglin et al. [35] reported that anti-CCP antibodies detected in preclinical phases of RA predict a poor radiographic outcome in early RA after 2 years of follow-up, whereas RF does not. However, our results are in contrast to those of our preliminary study [13] where anti-CCP were not associated with greater progression after 1 year of follow up; the shorter follow up, the smaller sample size, or the fact that the anti-CCP were determined using a first generation ELISA technique (CCP1) in this first study could explain this discrepancy. In fact, a recent study demonstrated a higher value of anti-CCP2 antibodies compared to anti-CCP1 antibodies in determining disease progression [36]. It is interesting to note that the anti-CCP antibody titer does not seem to be relevant in predicting radiographic outcome: the median titers of anti-CCP antibodies were not significantly different between anti-CCP-positive patients with and without radiographic progression, results that differ from a recent report where baseline values of anti-CCP were higher in RA patients with a worse radiographic outcome [35]. Methodological issues or the use of a different ELISA kit may explain these differences.
Our study had some limitations, which includes the relatively small sample size, the problem of the missing values of some variables, inherent to this type of longitudinal studies, and the short follow-up period. Although it was thought that patients with erosive RA frequently develop erosions during the first 2 years of the disease [3, 37], recent studies shown that erosions may develop for the first time after 2 years of disease evolution [38]. Therefore, it is not unlikely that some of the patients with erosive disease in our studies could develop erosions and joint damage in the near future. In addition, a small percentage of patients received TNF-blocking agents during the follow up. The potential of these agents in delaying structural damage is recognized [39] and this may have had some influence on the degree of disease progression in the present study. However, the small number of cases treated (ten patients, all but one during the second year, and with evidence of radiographic progression in three) suggests that these agents had no influence on our overall results.
Although some baseline parameters were associated with greater radiological progression in this and other studies of patients with early RA treated early with DMARDs, it is difficult to use these parameters in normal clinical practice to provide a differentiated therapeutic strategy, mainly because their predictive value for progressive disease is far from 100%. In our study, the multivariate model that included female gender, the presence of HLA-DRB1*04 alleles and anti-CCP, showed a relatively low sensitivity and positive predictive value for detecting radiological progression. However, the percentages for specificity and negative predictive value were higher (around 80%), suggesting that it may be the absence of these parameters which could have greater clinical relevance in predicting patients who will not suffer disease progression. In our cohort of female patients with RA, those with positive HLA-DRB1*04 and anti-CCP had a much greater rate of radiological progression than those with negative DRB1*04 and anti-CCP. A recent study found that the association of HLA-DRB1*04 and anti-CCP also resulted in greater disease progression compared with cases with one or neither of these factors [40].
In conclusion, in one third of patients with early RA treated with DMARDs and very low doses of glucocorticoids, significant radiographic progression was observed after 2 years, despite a systematic scheduled therapeutic strategy. Female gender, the SE included in HLA-DRB1*04 alleles (or with homozygozity), and the presence of anti-CCP antibodies at baseline (rather than the titer) were the most significant predictors of radiographic progression. However, in our opinion, the positive predictive value of these parameters is probably not high enough to advise its use in clinical practice to predict progression or to recommend more aggressive therapeutic approaches in these patients.
References
Sherrer YS, Bloch DA, Mitchell DM, Young DY, Fries J (1986) The development of disability in rheumatoid arthritis. Arthritis Rheum 29:494–500
van der Heijde DM (2000) Radiographic imaging: the “gold standard” for assessment of disease progression in rheumatoid arthritis. Rheumatology (Oxford) 39:9–16 (Suppl)
Fuchs HA, Kaye JJ, Callahan LF, Nance EP, Pincus T (1989) Evidence of significant radiographic damage in rheumatoid arthritis within the first 2 years of disease. J Rheumatol 16:585–591
Corbett M, Dalton S, Young A, Silman A, Shipley M (1993) Factors predicting death, survival and functional outcome in a prospective study of early rheumatoid disease over fifteen years. Ann Rheum Dis 32:717–723
American College of Rheumatology Subcommittee on Rheumatoid Arthritis Guidelines (2002) Guidelines for the management of rheumatoid arthritis. 2002 update. Arthritis Rheum 46:328–346
Jansen MA, van der Horst-Bruinsma IE, van Schaardenburg D, Bezemer PD, Dijkmans BA (2001) Predictors of radiographic joint damage in patients with early rheumatoid arthritis. Ann Rheum Dis 60:924–927
Brennan P, Harrison B, Barrett E, Chakravarty K, Scott D, Silman A, Symmons D (1996) A simple algorithm to predict the development of radiological erosions in patients with early rheumatoid arthritis: prospective cohort study. BMJ 24:471–476
Kroot E-J, de Jong BA, van Leeuwen MA, Swinkels H, van den Hoogen FH, van’t Hof M et al (2000) The prognostic value of anti-cyclic citrullinated peptide antibody in patients with recent-onset rheumatoid arthritis. Arthritis Rheum 43:1831–1835
Kastbom, Strandberg G, Lindroos A, Skogh T (2004) Anti-CCP antibody test predicts the disease course during 3 years in early rheumatoid arthritis (the Swedish TIRA project). Ann Rheum Dis 63:1085–1089
Mattey DL, Hassell AB, Dawes PT, Cheung NT, Poulton KV,Thomson W et al (2001) Independent association of rheumatoid factor and the HLA-DRB1 shared epitope with radiographic outcome in rheumatoid arthritis. Arthritis Rheum 44:1529–1533
Eberhardt K, Fex E, Johnson U, Wollheim FA (1996) Associations of HLA-DRB and -DQB genes with two and five year outcome in rheumatoid arthritis. Ann Rheum Dis 55:34–39
van Leeuwen MA, van Rijswijk MH, van der Heijde DM, Te Meerman GJ, van Riel PL, Houtman PM et al (1993) The acute-phase response in relation to radiographic progression in early rheumatoid arthritis: a prospective study during the first three years of the disease. Br J Rheumatol 32:9–13 (Suppl)
Sanmarti R, Gómez A, Ercilla G, Gratacós J, Larrosa M, Suris X et al (2003) Radiological progression in early rheumatoid arthritis after DMARDs: a one-year follow-up study in a clinical setting. Rheumatology (Oxford) 42:1044–1049
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS et al (1988) The America Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31:315–324
Pincus T, Summey JA, Soraci SA Jr, Wallston KA, Hummon NP (1983) Assessment of patient satisfaction in activities of daily living using a modified Stanford health Assessment Questionnaire. Arthritis Rheum 26:1346–1353
Kirwan JR (2000) Using the Larsen index to assess radiographic progression in rheumatoid arthritis. J Rheumatol 27:264–268
Bruynesteyn K, van der Heijde D, Boers M, Lassere M, Boonen A. Edmonds J et al (2001) Minimal clinically important difference in radiological progression of joint damage over 1 year in rheumatoid arthritis: preliminary results of a validation study with clinical experts. J Rheumatol 28: 904–910
Combe B, Dougados M, Goupille P, Cantagrel A, Eliaou JF, Sibilia J et al (2001) Prognostic factors for radiographic damage in early rheumatoid arthritis. A multiparameter prospective study. Arthritis Rheum 44:1736–1743
van Zeben D, Hazes JM, Zwinderman AH, Vanderbroucke JP, Breedveld FC (1993) Factors predicting outcome of rheumatoid arthritis: results of a follow-up study. J Rheumatol 20:1288–1296
Fex E, Jonsson K, Johnson U, Eberhardt K (1996) Development of radiographic damage during the first 5–6 years of rheumatoid arthritis. A prospective follow-up study of a Swedish cohort. Br J Rheumatol 1106–1115
van der Heide A, Remme CA, Hofman DM, Jacobs JW, Bijlsma JW (1995) Prediction of progression of radiologic damage in newly diagnosed rheumatoid arthritis. Arthritis Rheum 38:1466–1474
Wick MC, Lindblad S, Weiss RJ, Klareskog L, van Vollenhoven RF (2004) Clinical and radiological disease-course in a Swedish DMARD-treated early RA-inception cohort: an observational study. Scand J Rheumatol 33:380–384
Rau R, Herborn G, Menninger H, Sangha O (2002) Radiographic outcome after three years of patients with early erosive rheumatoid arthritis treated with intramuscular methotrexate or parenteral gold. Extension of a one-year double-blind study in 174 patients. Rheumatology (Oxford) 41:196–204
Goronzy JJ, Matteson EL, Fulbright JW, Warrington KJ, Chang-Miller A, Hunder GG et al (2004) Prognostic markers of radiographic progression in early rheumatoid arthritis. Arthritis Rheum 50:43–54
Jones G, Halbert J, Crotty M, Shanahan EM, Batterham M, Ahern M (2003) The effect of treatment on radiological progression in rheumatoid arthritis: a systematic review of randomized placebo-controlled trials. Rheumatology (Oxford) 42:6–13
Wassenberg S, Rau R, Steinfeld P, Zeidler H (2005) Low-dose prednisolone therapy study group. Very low-dose prednisolone in early rheumatoid arthritis retards radiographic progression over two years: a multicenter, double-blind placebo-controlled trial. Arthritis Rheum 52:3371–3380
Belghomari H, Saraux A, Allain J, Guedes C, Youinou P, Le Goff P (1999) Risk factors for radiographic articular destruction of hands and wrists in rheumatoid arthritis. J Rheumatol 26:2534–2538
Weyand CM, Hicock KC, Conn DL, Goronzy JJ (1992) The influence of HLA-DRB1 genes on disease severity in rheumatoid arthritis. Ann Intern Med 117:801–806
Hajeer AH, Dababneh A, Makki RF, Thomson W, Poulton K, Gonzalez-Gay MA (2000) Different gene loci within the HLA-DR and TNF regions are independently associated with susceptibility and severity in Spanish rheumatoid arthritis patients. Tissue Antigens 55:319–325
Drosos AA, Lanchbury JS, Panayi GS, Moutsopoulos HM (1992) Rheumatoid arthritis in Greek and British patients. A comparative clinical, radiologic, and serologic study. Arthritis Rheum 35:745–748
Morel J, Combe B (2005) How to predict prognosis in early rheumatoid arthritis. Best Pract Res Clin Rheumatol 19:137–146
Zendman AJ, Vossenaar ER, Van Venrooij WJ (2004) Autoantibodies to citrullinated (poly)peptides: a key diagnostic and prognostic marker for rheumatoid arthritis. Autoimmunity 37:295–299
De Rycke L, Peene I, Hoffman IE, Kruithof E, Union A, Meheus L et al (2004) Rheumatoid factor and anticitrullinated protein antibodies in rheumatoid arthritis: diagnostic value, associations with radiological progression rate, and extra-articular manifestations. Ann Rheum Dis 63:1587–1593
Meyer O, Labarre C, Dougados M, Goupille P, Cantagrel A, DuboisA et al (2003) Anticitrullinated protein/peptide antibody assays in early rheumatoid arthritis for predicting five year radiographic damage. Ann Rheum Dis 62:120–126
Berglin E, Johansson T, Sundin U, Jidell E, Wadell G, Hallmans G et al (2005) Radiological outcome in rheumatoid arthritis is predicted by the presence of antibodies against cyclic citrullinated peptide before and at disease onset, and by IgA-rheumatoid factor at disease onset. Ann Rheum Dis 65:453–458
van Gaalen FA, Visser H, Huizinga TW (2005) A comparison of the diagnostic accuracy and prognostic value of the first and second anti-cyclic citrullinated peptides (CCP1 and CCP2) autoantibody tests for rheumatoid arthritis. Ann Rheum Dis 64:1510–1512
Scott DL (2002) The diagnosis and prognosis of early arthritis: rationale for new prognostic criteria. Arthritis Rheum 46:286–290
Bukhari M, Harrison B, Lunt M, Scott DG, Symmons DP, Silman AJ (2001) Time to first occurrence of erosions in inflammatory polyarthritis: results from a prospective community-based study. Arthritis Rheum 44:1248–1253
Bresnihan B (2002) Preventing joint damage as the best measure of biologic drug therapy. J Rheumatol 65:39–43 (Suppl)
van Gaalen FA, van Aken J, Huizinga TW, Schreuder GM, Breedveld FC, Zanelli E et al (2004) Association between HLA class II genes and autoantibodies to cyclic citrullinated peptides (CCPs) influences the severity of rheumatoid arthritis. Arthritis Rheum 50:2113–2121
Acknowledgements
We are grateful to Emma Arcos of the Department of Biostatistics (Unitat d’Avaluació i suport) of the Hospital Clinic of Barcelona for the statistical analysis. We would also like to thank M. A. Romera, L. Rubio, and I. Machuca for laboratory support. This study was supported by a grant from the Spanish Ministry of Health (FIS 98/1278) and a grant from the Fundacio Marató TV3 (No. 2003 TV030330-0), Catalonia, Spain.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Sanmartí, R., Gómez-Centeno, A., Ercilla, G. et al. Prognostic factors of radiographic progression in early rheumatoid arthritis: a two year prospective study after a structured therapeutic strategy using DMARDs and very low doses of glucocorticoids. Clin Rheumatol 26, 1111–1118 (2007). https://doi.org/10.1007/s10067-006-0462-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-006-0462-4