Abstract
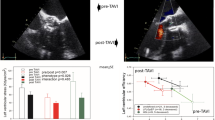
The 16-mm ATS mechanical valve is one of the smallest prosthetic valves used for aortic valve replacement (AVR) in patients with a very small aortic annulus, and its clinical outcomes are reportedly satisfactory. Here, we analyzed the left ventricular (LV) performance after AVR with the 16-mm ATS mechanical valve, based on the concept of cardiac energetics analysis. Eleven patients who underwent AVR with the 16-mm ATS mechanical valve were enrolled in this study. All underwent echocardiographic examination at three time points: before AVR, approximately 1 month after AVR, and approximately 1 year after AVR. LV contractility (end-systolic elastance [Ees]), afterload (effective arterial elastance [Ea]), and efficiency (ventriculoarterial coupling [Ea/Ees] and the stroke work to pressure–volume area ratio [SW/PVA]) were noninvasively measured by echocardiographic data and blood pressure measurement. Ees transiently decreased after AVR and then recovered to the pre-AVR level at the one-year follow-up. Ea significantly decreased in a stepwise manner. Consequently, Ea/Ees and SW/PVA were also significantly improved at the one-year follow-up compared with those before AVR. The midterm LV performance after AVR with the 16-mm ATS mechanical valve was satisfactory. AVR with the 16-mm ATS mechanical valve is validated as an effective treatment for patients with a very small aortic annulus. The cardiac energetics variables, coupling with the conventional hemodynamic variables, can contribute to a better understanding of the patients’ clinical conditions, and those may serve as promising indices of the cardiac function.

Similar content being viewed by others
References
Nicks R, Cartmill T, Bernstein L. Hypoplasia of the aortic root. The problem of aortic valve replacement. Thorax. 1970;25:339–46.
Konno S, Imai Y, Iida Y, Nakajima M, Tatsuno K. A new method for prosthetic valve replacement in congenital aortic stenosis associated with hypoplasia of the aortic valve ring. J Thorac Cardiovasc Surg. 1975;70:909–17.
Manouguian S, Seybold-Epting W. Patch enlargement of the aortic valve ring by extending the aortic incision into the anterior mitral leaflet. New operative technique. J Thorac Cardiovasc Surg. 1979;78:402–12.
Ennker IC, Albert A, Dalladaku F, Rosendahl U, Ennker J, Florath I. Midterm outcome after aortic root replacement with stentless porcine bioprostheses. Eur J Cardiothorac Surg. 2011;40:429–34.
Nakamura Y, Nakano K, Tagusari O, Kataoka G, Seike Y, Domoto S, Ito Y. An alternative option for elderly patients with a small aortic annulus: the 16 mm ATS valve. J Heart Valve Dis. 2009;18:691–7.
Kobayashi Y, Fukushima Y, Hayase T, Kojima K, Endo G. Clinical outcome of aortic valve replacement with 16-mm ATS-advanced performance valve for small aortic annulus. Ann Thorac Surg. 2010;89:1195–9.
Burkhoff D, Sagawa K. Ventricular efficiency predicted by an analytical model. Am J Physiol. 1986;250:R1021–7.
Suga H. Ventricular energetics. Physiol Rev. 1990;70:247–77.
Sunagawa K, Maughan WL, Burkhoff D, Sagawa K. Left ventricular interaction with arterial load studied in isolated canine ventricle. Am J Physiol. 1983;245:H773–80.
Tanoue Y, Sese A, Ueno Y, Joh K, Hijii T. Bidirectional Glenn procedure improves the mechanical efficiency of a total cavopulmonary connection in high-risk fontan candidates. Circulation. 2001;103:2176–80.
Tanoue Y, Ando H, Fukumura F, Umesue M, Uchida T, Taniguchi K, Tanaka J. Ventricular energetics in endoventricular circular patch plasty for dyskinetic anterior left ventricular aneurysm. Ann Thorac Surg. 2003;75:1205–9.
Tanoue Y, Sese A, Imoto Y, Joh K. Ventricular mechanics in the bidirectional glenn procedure and total cavopulmonary connection. Ann Thorac Surg. 2003;76:562–6.
Tanoue Y, Kado H, Maeda T, Shiokawa Y, Fusazaki N, Ishikawa S. Left ventricular performance of pulmonary atresia with intact ventricular septum after right heart bypass surgery. J Thorac Cardiovasc Surg. 2004;128:710–7.
Tanoue Y, Kado H, Shiokawa Y, Fusazaki N, Ishikawa S. Midterm ventricular performance after Norwood procedure with right ventricular-pulmonary artery conduit. Ann Thorac Surg. 2004;78:1965–71.
Tanoue Y, Kado H, Ushijima T, Tominaga R. Consequences of a hypertensive right ventricle on left ventricular performance of patients with pulmonary atresia and intact ventricular septum after right heart bypass surgery. Prog Pediatr Cardiol. 2010;29:43–8.
Tanoue Y, Maeda T, Oda S, Baba H, Oishi Y, Tokunaga S, Nakashima A, Tominaga R. Left ventricular performance in aortic valve replacement. Interact CardioVasc Thorac Surg. 2009;9:255–9.
Tanoue Y, Tomita Y, Morita S, Tominaga R. Ventricular energetics in aortic root replacement for annuloaortic ectasia with aortic regurgitation. Heart Vessels. 2009;24:41–5.
Imasaka KI, Tomita Y, Tanoue Y, Tominaga R, Tayama E, Onitsuka H, Ueda T. Early mitral valve surgery for chronic severe mitral regurgitation optimizes left ventricular performance and left ventricular mass regression. J Thorac Cardiovasc Surg. 2012;146:61–6.
Nagata H, Ihara K, Yamamura K, Tanoue Y, Shiokawa Y, Tominaga R, Hara T. Left ventricular efficiency after ligation of patent ductus arteriosus for premature infants. J Thorac Cardiovasc Surg. 2013;146:1353–8.
Tanoue Y, Oishi Y, Sonoda H, Nishida T, Nakashima A, Tominaga R. Left ventricular performance after aortic valve replacement in patients with low ejection fraction. J Artif Organs. 2013;15:444–50.
Jamieson WR, Ye J, Higgins J, Cheung A, Fradet GJ, Skarsgard P, Germann E, Chan F, Lichtenstein SV. Effect of prosthesis-patient mismatch on long-term survival with aortic valve replacement: assessment to 15 years. Ann Thorac Surg. 2010;89:51–9.
Head SJ, Mokhles MM, Osnabrugge RL, Pibarot P, Mack MJ, Takkenberg JJ, Bogers AJ, Kappetein AP. The impact of prosthesis-patient mismatch on long-term survival after aortic valve replacement: a systematic review and meta-analysis of 34 observational studies comprising 27186 patients with 133141 patient-years. Eur Heart J. 2012;33:1518–29.
Baumgartner H, Hung J, Bermejo J, Chambers JB, Evangelista A, Griffin BP, Iung B, Otto CM, Pellikka PA, Quiñones M. Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr. 2009;22:1–23.
Teichholz LE, Kreulen T, Herman MV, Gorlin R. Problems in echocardiographic volume determinations: echocardiographic-angiographic correlations in the presence of absence of asynergy. Am J Cardiol. 1976;37:7–11.
Lang RM, Bierig M, Devereux RB, Flachskampf M, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18:1440–63.
Nozawa T, Yasumura Y, Futaki S, Tanaka N, Uenishi M, Suga H. Efficiency of energy transfer from pressure-volume area to external mechanical work increases with contractile state and decreases with afterload in the left ventricle of the anesthetized closed-chest dog. Circulation. 1988;77:1116–24.
Conflict of interest
There is no conflict of interest or disclosure for any of the authors with any companies/organizations whose product/services discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Appendix
Appendix
Theoretical background
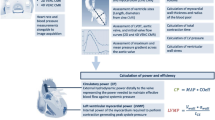
The cardiac energetics variables include Ees, Ea, and Ea/Ees and SW/PVA. Ees represents the load-independent index of contractility; Ea represents the index of afterload; and Ea/Ees and SW/PVA are the indices of ventricular efficiency. As particularly described in previous investigations, Ees is the slope of the end-systolic pressure–volume relation [8], and Ea is the ratio of end-systolic pressure to stroke volume [9]. Ea/Ees represents ventriculoarterial coupling between the LV and the arterial system [7]. SW represents the external mechanical work, and PVA represents the total mechanical energy generated by ventricular contraction. The ratio of SW to PVA can be understood as the energy efficiency. These variables are actually determined from the multiple LV pressure–volume loops with a conductance catheter system. Furthermore, SW/PVA can be theoretically predicted by Ees and Ea as follows: SW/PVA = 1/(1 + 0.5 Ea/Ees) [26].
Validity of approximated Ees and Ea
We previously described the approximation methods of Ees and Ea as follows: approximated Ees = mean arterial pressure/minimal ventricular volume; approximated Ea = maximal ventricular pressure/(maximal ventricular volume – minimal ventricular volume) [10]. With this modification, the cardiac energetics variables can be easily calculated.The important point is that end-systolic ventricular volume and end-diastolic ventricular volume according to the pressure–volume loop are not same as minimal ventricular volume and maximal ventricular volume, respectively. Normally, end-systolic ventricular volume is larger than minimal ventricular volume and end-diastolic ventricular volume is lower than maximal ventricular volume. Another important point is that end-systolic ventricular pressure is smaller than maximal ventricular pressure. In these points, the present approximated Ees and Ea are not precisely identical with Ees and Ea measured with a conductance catheter system. In particular, the approximated Ees is calculated not as the ratio of end-systolic pressure to end-systolic ventricular volume, but as the ratio of mean arterial blood pressure to minimal ventricular volume, and therefore, the volume intercept is not defined as zero [15]. The high correlations between Ees and the approximated Ees and between Ea and the approximated Ea were experimentally validated in the basic study using a canine right heart bypass preparation with a conductance catheter system [10]. This modification has the advantages that ventricular volume and blood pressure are measured with the cardiac catheterization, which enables the cardiac energetics analysis in various clinical situations [10–15]. Further modifying this modification in the recent study, the LV performance has been analyzed with the echocardiographic ventricular volume calculation and noninvasively measured blood pressure [16–20]. This modification can be the promising analysis method of ventricular efficiency.
Rights and permissions
About this article
Cite this article
Ushijima, T., Tanoue, Y., Uchida, T. et al. Cardiac energetics analysis after aortic valve replacement with 16-mm ATS mechanical valve. J Artif Organs 17, 250–257 (2014). https://doi.org/10.1007/s10047-014-0769-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-014-0769-x