Abstract
Purpose
Negative pressure wound therapy on closed incisions (iNPWT) is a wound dressing system developed to promote wound healing and avoid complications after surgical procedures. The effect of iNPWT is well established in various surgical fields, however, the effect on postoperative wound complications after ventral hernia repair remains unknown. The aim of this systematic review and meta-analysis was to investigate the effect of iNPWT on patients undergoing open ventral hernia repair (VHR) compared with conventional wound dressing.
Materials and methods
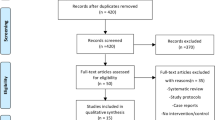
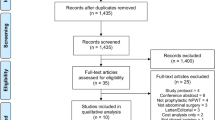
This systematic review and meta-analysis followed the PRISMA guidelines. The databases PubMed, Embase, Cochrane Library, Web of science and Cinahl were searched for original studies comparing iNPWT to conventional wound dressing in patients undergoing VHR. The primary outcome was surgical site occurrence (SSO), secondary outcomes included surgical site infection (SSI) and hernia recurrence.
Results
The literature search identified 373 studies of which 10 were included in the meta-analysis including a total of 1087 patients. Eight studies were retrospective cohort studies, one was a cross-sectional pilot study, and one was a randomized controlled trial. The meta-analysis demonstrated that iNPWT was associated with a decreased risk of SSO (OR 0.27 [0.19, 0.38]; P < 0.001) and SSI (OR 0.32 [0.17, 0.55]; P < 0.001). There was no statistically significant association with the risk of hernia recurrence (OR 0.62 [0.27, 1.43]; P = 0.26).
Conclusion
Based on the findings of this systematic review and meta-analysis iNPWT following VHR was found to significantly reduce the incidence of SSO and SSI, compared with standard wound dressing. INPWT should be considered for patients undergoing VHR.






Similar content being viewed by others
Availability of data and materials
The data that support the findings of this study are available from the corresponding author, VBH, upon reasonable request.
Code availability
Not applicable.
References
Muse TO, Zwischenberger BA, Miller MT, Borman DA, Davenport DL, Roth JS (2018) Outcomes after Ventral hernia repair using the rives-stoppa, endoscopic, and open component separation techniques. Am Surg 84(3):433–437
Jensen KK, Dressler J, Baastrup NN, Kehlet H, Jørgensen LN (2019) Enhanced recovery after abdominal wall reconstruction reduces length of postoperative stay: an observational cohort study. Surgery 165(2):393–397. https://doi.org/10.1016/j.surg.2018.07.035
Jensen KK, Henriksen NA, Jorgensen LN (2014) Endoscopic component separation for ventral hernia causes fewer wound complications compared to open components separation: a systematic review and meta-analysis. Surg Endosc 28(11):3046–3052. https://doi.org/10.1007/s00464-014-3599-2
Plymale MA, Ragulojan R, Davenport DL, Roth JS (2017) Ventral and incisional hernia: the cost of comorbidities and complications. Surg Endosc 31(1):341–351. https://doi.org/10.1007/s00464-016-4977-8
Cox TC, Blair LJ, Huntington CR, Colavita PD, Prasad T, Lincourt AE et al (2016) The cost of preventable comorbidities on wound complications in open ventral hernia repair. J Surg Res 206(1):214–222. https://doi.org/10.1016/j.jss.2016.08.009
Nissen AT, Henn D, Moshrefi S, Gupta D, Nazerali R, Lee GK (2019) Health-related quality of life after ventral hernia repair with biologic and synthetic mesh. Ann Plast Surg 82(5S Suppl4):S332–S338. https://doi.org/10.1097/sap.0000000000001768
Cobb WS, Warren JA, Ewing JA, Burnikel A, Merchant M, Carbonell AM (2015) Open retromuscular mesh repair of complex incisional hernia: predictors of wound events and recurrence. J Am Coll Surg 220(4):606–613. https://doi.org/10.1016/j.jamcollsurg.2014.12.055
Fleischmann W, Lang E, Russ M (1997) Treatment of infection by vacuum sealing. Unfallchirurg 100(4):301–304. https://doi.org/10.1007/s001130050123
Argenta LC, Morykwas MJ (1997) Vacuum-assisted closure: a new method for wound control and treatment: clinical experience. Ann Plast Surg 38(6):563–576
Norman G, Goh EL, Dumville JC, Shi C, Liu Z, Chiverton L et al (2020) Negative pressure wound therapy for surgical wounds healing by primary closure. Cochrane Database Syst Rev 5(5):Cd009261. https://doi.org/10.1002/14651858.CD009261.pub5
Swanson EW, Cheng HT, Susarla SM, Lough DM, Kumar AR (2016) Does negative pressure wound therapy applied to closed incisions following ventral hernia repair prevent wound complications and hernia recurrence? A systematic review and meta-analysis. Plast Surg (Oakv) 24(2):113–118
Hyldig N, Birke-Sorensen H, Kruse M, Vinter C, Joergensen JS, Sorensen JA et al (2016) Meta-analysis of negative-pressure wound therapy for closed surgical incisions. Br J Surg 103(5):477–486. https://doi.org/10.1002/bjs.10084
Condé-Green A, Chung TL, Holton LH 3rd, Hui-Chou HG, Zhu Y, Wang H et al (2013) Incisional negative-pressure wound therapy versus conventional dressings following abdominal wall reconstruction: a comparative study. Ann Plast Surg 71(4):394–397. https://doi.org/10.1097/SAP.0b013e31824c9073
(2012) Abstracts of the Thirty-Second Annual Meeting of the Surgical Infection Society. Dallas, Texas, USA. April 18-21, 2012. Surg Infect (Larchmt) 13(Suppl 1):S9–39. https://doi.org/10.1089/sur.2012.9908
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ (Clinical research ed) 339:b2700. https://doi.org/10.1136/bmj.b2700
Haskins IN, Horne CM, Krpata DM, Prabhu AS, Tastaldi L, Perez AJ et al (2018) A call for standardization of wound events reporting following ventral hernia repair. Hernia 22(5):729–736. https://doi.org/10.1007/s10029-018-1748-6
Breuing K, Butler CE, Ferzoco S, Franz M, Hultman CS, Kilbridge JF et al (2010) Incisional ventral hernias: review of the literature and recommendations regarding the grading and technique of repair. Surgery 148(3):544–558. https://doi.org/10.1016/j.surg.2010.01.008
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ (Clinical research ed) 355:i4919. https://doi.org/10.1136/bmj.i4919
McGuinness LA, Higgins JPT (2021) Risk-of-bias VISualization (robvis): an R package and Shiny web app for visualizing risk-of-bias assessments. Res Synth Methods 12(1):55–61. https://doi.org/10.1002/jrsm.1411
Review Manager (RevMan) [Computer program]. Version 5.4.1, The Cochrane Collaboration. (2020)
Hopkins B, Eustache J, Ganescu O, Cipolla J, Kaneva P, Fried GM et al (2020) S116: impact of incisional negative pressure wound therapy on surgical site infection after complex incisional hernia repair: a retrospective matched cohort study. Surg Endosc. https://doi.org/10.1007/s00464-020-07857-1
Diaconu SC, McNichols CHL, Ngaage LM, Liang Y, Ikheloa E, Bai J et al (2020) Closed-incision negative-pressure therapy decreases complications in ventral hernia repair with concurrent panniculectomy. Hernia 24(1):49–55. https://doi.org/10.1007/s10029-018-1865-2
Gassman A, Mehta A, Bucholdz E, Abthani A, Guerra O, Maclin MM Jr et al (2015) Positive outcomes with negative pressure therapy over primarily closed large abdominal wall reconstruction reduces surgical site infection rates. Hernia 19(2):273–278. https://doi.org/10.1007/s10029-014-1312-y
Licari L, Campanella S, Carolla C, Viola S, Salamone G (2020) Closed incision negative pressure therapy achieves better outcome than standard wound care: clinical outcome and cost-effectiveness analysis in open ventral hernia repair with synthetic mesh positioning. Cureus 12(5):e8283. https://doi.org/10.7759/cureus.8283
Olona C, Duque E, Caro A, Jiménez A, Moreno F, Coronas JM et al (2014) Negative-pressure therapy in the postoperative treatment of incisional hernioplasty wounds: a pilot study. Adv Skin Wound Care 27(2):77–80. https://doi.org/10.1097/01.ASW.0000442873.48590.b5
Soares KC, Baltodano PA, Hicks CW, Cooney CM, Olorundare IO, Cornell P et al (2015) Novel wound management system reduction of surgical site morbidity after ventral hernia repairs: a critical analysis. Am J Surg 209(2):324–332. https://doi.org/10.1016/j.amjsurg.2014.06.022
Pauli EM, Krpata DM, Novitsky YW, Rosen MJ (2013) Negative pressure therapy for high-risk abdominal wall reconstruction incisions. Surg Infect (Larchmt) 14(3):270–274. https://doi.org/10.1089/sur.2012.059
Bueno-Lledó J, Franco-Bernal A, Garcia-Voz-Mediano MT, Torregrosa-Gallud A, Bonafé S (2021) Prophylactic single-use negative pressure dressing in closed surgical wounds after incisional hernia repair: a randomized, controlled trial. Ann Surg 273(6):1081–1086. https://doi.org/10.1097/sla.0000000000004310
Parker SG, Halligan S, Liang MK, Muysoms FE, Adrales GL, Boutall A et al (2020) International classification of abdominal wall planes (ICAP) to describe mesh insertion for ventral hernia repair. Br J Surg 107(3):209–217. https://doi.org/10.1002/bjs.11400
de Vries FEE, Atema JJ, Lapid O, Obdeijn MC, Boermeester MA (2017) Closed incision prophylactic negative pressure wound therapy in patients undergoing major complex abdominal wall repair. Hernia 21(4):583–589. https://doi.org/10.1007/s10029-017-1620-0
Scalise A, Calamita R, Tartaglione C, Pierangeli M, Bolletta E, Gioacchini M et al (2016) Improving wound healing and preventing surgical site complications of closed surgical incisions: a possible role of Incisional Negative Pressure Wound Therapy. A systematic review of the literature. Int Wound J 13(6):1260–1281. https://doi.org/10.1111/iwj.12492
Schlosser KA, Otero J, Lincourt A, Augenstein VA (2019) Management of surgical incisions using incisional negative-pressure therapy. Plast Reconstr Surg. https://doi.org/10.1097/prs.0000000000005307
Jensen KK, Brondum TL, Harling H, Kehlet H, Jorgensen LN (2016) Enhanced recovery after giant ventral hernia repair. Hernia 20(2):249–256. https://doi.org/10.1007/s10029-016-1471-0
Jensen KK, Brøndum TL, Leerhøy B, Belhage B, Hensler M, Arnesen RB et al (2020) Preoperative, single, high-dose glucocorticoid administration in abdominal wall reconstruction: a randomized, double-blinded clinical trial. Surgery 167(4):757–764. https://doi.org/10.1016/j.surg.2019.12.007
Jensen KK, Munim K, Kjaer M, Jorgensen LN (2017) Abdominal wall reconstruction for incisional hernia optimizes truncal function and quality of life: a prospective controlled study. Ann Surg 265(6):1235–1240. https://doi.org/10.1097/sla.0000000000001827
Jensen KK, Emmertsen KJ, Laurberg S, Krarup PM (2020) Long-term impact of incisional hernia on quality of life after colonic cancer resection. Hernia 24(2):265–272. https://doi.org/10.1007/s10029-019-01978-w
Zwanenburg PR, Timmermans FW, Timmer AS, Middelkoop E, Tol BT, Lapid O et al (2021) A systematic review evaluating the influence of incisional Negative Pressure Wound Therapy on scarring. Wound Repair Regen 29(1):8–19. https://doi.org/10.1111/wrr.12858
Chopra K, Gowda AU, Morrow C, Holton L 3rd, Singh DP (2016) The economic impact of closed-incision negative-pressure therapy in high-risk abdominal incisions: a cost-utility analysis. Plast Reconstr Surg 137(4):1284–1289. https://doi.org/10.1097/prs.0000000000002024
Görgülü T (2015) A complication of management of closed incision with negative-pressure wound therapy. Aesthet Surg J 35(5):Np113–Np115. https://doi.org/10.1093/asj/sju120
Howell R, Hadley S, Strauss E, Pelham F (2011) Blister formation with negative pressure dressing after total knee arthroplasty. Curr Orthopaedic Practice 22(2):176–179. https://doi.org/10.1097/BCO.0b013e31820b3e21
Rodriguez-Unda N, Soares KC, Azoury SC, Baltodano PA, Hicks CW, Burce KK et al (2015) Negative-pressure wound therapy in the management of high-grade ventral hernia repairs. J Gastrointest Surg 19(11):2054–2061. https://doi.org/10.1007/s11605-015-2894-0
Singh D (2018) The role of closed incision negative pressure therapy in abdominal wall reconstruction: a current review of the evidence. Plast Reconstr Surg 142(3 Suppl):156s-s162. https://doi.org/10.1097/prs.0000000000004872
Funding
No funding was received for the current study.
Author information
Authors and Affiliations
Contributions
All authors listed in this manuscript meet the authorship requirements set out by the International Committee of Medical Journal Editors (ICMJE). Conception and design were done by KKJ and EO. Literature search and data collection were by EO, MW and VBH. Analysis and interpretation were done by EO and VBH. VBH drafted the manuscript. Critical revision of the article was done by KKJ, EO, MW and VBH. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Drs. Berner-Hansen, Oma, Willaume and Jensen have no conflict of interest or financial ties to disclose.
Ethical approval
Ethical approval was not required for this type of study.
Human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was not required for this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Berner-Hansen, V., Oma, E., Willaume, M. et al. Prophylactic negative pressure wound therapy after open ventral hernia repair: a systematic review and meta-analysis. Hernia 25, 1481–1490 (2021). https://doi.org/10.1007/s10029-021-02485-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-021-02485-7