Abstract
Purpose
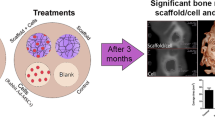
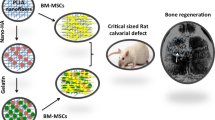
The aim of this experiment was to examine the capacity of collagen–glycosaminoglycan scaffolds, with or without mesenchymal stem cells, to satisfactorily repair a 5-mm rat calvarial defect.
Methods
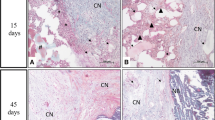
Fifty-five Wistar rats were used in the study. The defects were either left empty to serve as controls (n = 7) or filled with cell-free scaffolds (n = 11), cell-seeded scaffolds that were pre-cultured in standard culture medium (n = 13), cell-seeded scaffolds that were pre-cultured in osteoinductive factor-supplemented medium (n = 12) or particulate autogenous bone (n = 12). The animals were sacrificed at 12 weeks after surgery, and specimens were prepared for histomorphometric analysis. The linear bone healing and the bone area within the defect were measured.
Results
Comparable results were obtained using cell-free collagen–glycosaminoglycan scaffolds and autogenous bone both in terms of linear bone healing (P < 0.986) and area of new bone (P < 0.846). While the test groups showed significantly more bone formation compared to the empty defect control group, the linear bone healing and area of new bone within the defect were significantly lower in the cell-seeded scaffolds than in the cell-free scaffolds. The results have demonstrated that a cell-free collagen–glycosaminoglycan scaffold is capable of repairing a 5-mm rat calvarial defect as effectively as autogenous bone and that seeding the scaffold with pre-cultured mesenchymal stem cells prior to implantation offered no beneficial effect and resulted in incomplete healing of the defect.
Conclusions
The results thus suggest that the scaffold has immense potential for tissue repair showing favorable osteoconductive properties, biocompatibility and degradability.








Similar content being viewed by others
References
Wan DC, Siedhoff MT, Kwan MD, Nacamuli RP, Wu BM, Longaker MT (2007) Refining retinoic acid stimulation for osteogenic differentiation of murine adipose-derived adult stromal cells. Tissue Eng 13:1623–1631
Glowacki J, Mizuno S (2008) Collagen scaffolds for tissue engineering. Biopolymers 89:338–344
Bruder SP, Kurth AA, Shea M, Hayes WC, Jaiswal N, Kadiyala S (1998) Bone regeneration by implantation of purified, culture-expanded human mesenchymal stem cells. J Orthop Res 16:155–162
Farrell E, O'Brien FJ, Doyle P, Fischer J, Yannas I, Harley BA, O’Connell B, Prendergast PJ, Campbell VA (2006) A collagen–glycosaminoglycan scaffold supports adult rat mesenchymal stem cell differentiation along osteogenic and chondrogenic routes. Tissue Eng 12:459–468
Farrell E, Byrne EM, Fischer J, O'Brien FJ, O'Connell BC, Prendergast PJ, Campbell VA (2007) A comparison of the osteogenic potential of adult rat mesenchymal stem cells cultured in 2-D and on 3-D collagen glycosaminoglycan scaffolds. Technol Health Care 15:19–31
Byrne EM, Farrell E, McMahon LA, Haugh MG, O'Brien FJ, Campbell VA, Prendergast PJ, O'Connell BC (2008) Gene expression by marrow stromal cells in a porous collagen–glycosaminoglycan scaffold is affected by pore size and mechanical stimulation. J Mater Sci Mater Med 19:3455–3463
Kumarasuriyar A, Jackson RA, Grondahl L, Trau M, Nurcombe V, Cool SM (2005) Poly(beta-hydroxybutyrate-co-beta-hydroxyvalerate) supports in vitro osteogenesis. Tissue Eng 11:1281–1295
Bonzani IC, Adhikari R, Houshyar S, Mayadunne R, Gunatillake P, Stevens MM (2007) Synthesis of two-component injectable polyurethanes for bone tissue engineering. Biomaterials 28:423–433
Silva GA, Coutinho OP, Ducheyne P, Shapiro IM, Reis RL (2007) The effect of starch and starch-bioactive glass composite microparticles on the adhesion and expression of the osteoblastic phenotype of a bone cell line. Biomaterials 28:326–334
Hollinger JO, Winn S, Bonadio J (2000) Options for tissue engineering to address challenges of the aging skeleton. Tissue Eng 6:341–350
O'Brien FJ, Harley BA, Yannas IV, Gibson L (2004) Influence of freezing rate on pore structure in freeze-dried collagen–GAG scaffolds. Biomaterials 25:1077–1086
O'Brien FJ, Harley BA, Yannas IV, Gibson LJ (2005) The effect of pore size on cell adhesion in collagen–GAG scaffolds. Biomaterials 26:433–441
O'Brien FJ, Harley BA, Waller MA, Yannas IV, Gibson LJ, Prendergast PJ (2007) The effect of pore size on permeability and cell attachment in collagen scaffolds for tissue engineering. Technol Health Care 15:3–17
Barry FP, Boynton RE, Haynesworth S, Murphy JM, Zaia J (1999) The monoclonal antibody SH-2, raised against human mesenchymal stem cells, recognizes an epitope on endoglin (CD105). Biochem Biophys Res Commun 265:134–139
Kearney EM, Prendergast PJ, Campbell VA (2008) Mechanisms of strain-mediated mesenchymal stem cell apoptosis. J Biomech Eng 130:061004
Rochefort GY, Vaudin P, Bonnet N, Pages JC, Domenech J, Charbord P, Eder V (2005) Influence of hypoxia on the domiciliation of mesenchymal stem cells after infusion into rats: possibilities of targeting pulmonary artery remodeling via cells therapies? Respir Res 6:125
McMahon LA, Reid AJ, Campbell VA, Prendergast PJ (2008) Regulatory effects of mechanical strain on the chondrogenic differentiation of MSCs in a collagen–GAG scaffold: experimental and computational analysis. Ann Biomed Eng 36:185–194
Nguyen PD, Lin CD, Allori AC, Ricci JL, Saadeh PB, Warren SM (2009) Establishment of a critical-sized alveolar defect in the rat: a model for human gingivoperiosteoplasty. Plast Reconstr Surg 123(3):817–825
Gosain AK, Song L, Yu P, Mehrara BJ, Maeda CY, Gold LI, Longaker MT (2000) Osteogenesis in cranial defects: reassessment of the concept of critical size and the expression of TGF-beta isoforms. Plast Reconstr Surg 106(2):360–371
Bosch C, Melsen B, Vargervik K (1998) Importance of the critical-size bone defect in testing bone-regenerating materials. J Craniofac Surg 9:310–316
Donos N, Lang NP, Karoussis IK, Bosshardt D, Tonetti M, Kostopoulos L (2004) Effect of GBR in combination with deproteinized bovine bone mineral and/or enamel matrix proteins on the healing of critical-size defects. Clin Oral Implants Res 15:101–111
Furlaneto FA, Nagata MJ, Fucini SE, Deliberador TM, Okamoto T, Messora MR (2007) Bone healing in critical-size defects treated with bioactive glass/calcium sulfate: a histologic and histometric study in rat calvaria. Clin Oral Implants Res 18:311–318
Sawyer AA, Song SJ, Susanto E, Chuan P, Lam CX, Woodruff MA, Hutmacher DW, Cool SM (2009) The stimulation of healing within a rat calvarial defect by mPCL-TCP/collagen scaffolds loaded with rhBMP-2. Biomaterials 30:2479–2488
Alhag M, Farrell E, Toner M, Claffey N, Lee TC, O'Brien FJ (2011) Evaluation of early healing events around mesenchymal stem cell-seeded collagen–glycosaminoglycan scaffold. An experimental study in Wistar rats. Oral Maxillofac Surg 15:31–39
Inoda H, Yamamoto G, Hattori T (2004) Histological investigation of osteoinductive properties of rh-BMP2 in a rat calvarial bone defect model. J Craniomaxillofac Surg 32:365–369
Petrovic L, Schlegel AK, Schultze-Mosgau S, Wiltfang J (2006) Different substitute biomaterials as potential scaffolds in tissue engineering. Int J Oral Maxillofac Implants 21:225–231
Mizuno M, Shindo M, Kobayashi D, Tsuruga E, Amemiya A, Kuboki Y (1997) Osteogenesis by bone marrow stromal cells maintained on type I collagen matrix gels in vivo. Bone 20:101–107
Khan SN, Tomin E, Lane JM (2000) Clinical applications of bone graft substitutes. Orthop Clin North Am 31:389–398
Buser D, Hoffmann B, Bernard JP, Lussi A, Mettler D, Schenk RK (1998) Evaluation of filling materials in membrane-protected bone defects. A comparative histomorphometric study in the mandible of miniature pigs. Clin Oral Implants Res 9:137–150
Sung HJ, Meredith C, Johnson C, Galis ZS (2004) The effect of scaffold degradation rate on three-dimensional cell growth and angiogenesis. Biomaterials 25:5735–5742
Laschke MW, Haufel JM, Thorlacius H, Menger MD (2005) New experimental approach to study host tissue response to surgical mesh materials in vivo. J Biomed Mater Res A 74:696–704
Meikle MC, Papaioannou S, Ratledge TJ, Speight PM, Watt-Smith SR, Hill PA, Reynolds JJ (1994) Effect of poly DL-lactide-co-glycolide implants and xenogeneic bone matrix-derived growth factors on calvarial bone repair in the rabbit. Biomaterials 15:513–521
Ericsson I, Persson LG, Berglundh T, Marinello CP, Lindhe J, Klinge B (1995) Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol 22:255–261
Lee CR, Breinan HA, Nehrer S, Spector M (2000) Articular cartilage chondrocytes in type I and type II collagen–GAG matrices exhibit contractile behavior in vitro. Tissue Eng 6:555–565
Ma L, Gao C, Mao Z, Zhou J, Shen J (2004) Biodegradability and cell-mediated contraction of porous collagen scaffolds: the effect of lysine as a novel crosslinking bridge. J Biomed Mater Res A 71:334–342
Mueller SM, Schneider TO, Shortkroff S, Breinan HA, Spector M (1999) alpha-smooth muscle actin and contractile behavior of bovine meniscus cells seeded in type I and type II collagen–GAG matrices. J Biomed Mater Res 45:157–166
Torres DS, Freyman TM, Yannas IV, Spector M (2000) Tendon cell contraction of collagen–GAG matrices in vitro: effect of cross-linking. Biomaterials 21:1607–1619
Ohgushi H, Caplan AI (1999) Stem cell technology and bioceramics: from cell to gene engineering. J Biomed Mater Res 48:913–927
Wang J, Glimcher MJ (1999) Characterization of matrix-induced osteogenesis in rat calvarial bone defects: I. Differences in the cellular response to demineralized bone matrix implanted in calvarial defects and in subcutaneous sites. Calcif Tissue Int 65:156–165
Wang J, Glimcher MJ (1999) Characterization of matrix-induced osteogenesis in rat calvarial bone defects: II. Origins of bone-forming cells. Calcif Tissue Int 65:486–493
Terada S, Sato M, Sevy A, Vacanti JP (2000) Tissue engineering in the twenty-first century. Yonsei Med J 41:685–691
Lee KY, Alsberg E, Mooney DJ (2001) Degradable and injectable poly(aldehyde guluronate) hydrogels for bone tissue engineering. J Biomed Mater Res 56:228–233
Mizuno M, Imai T, Fujisawa R, Tani H, Kuboki Y (2000) Bone sialoprotein (BSP) is a crucial factor for the expression of osteoblastic phenotypes of bone marrow cells cultured on type I collagen matrix. Calcif Tissue Int 66:388–396
Iwata H, Sakano S, Itoh T, Bauer TW (2002) Demineralized bone matrix and native bone morphogenetic protein in orthopaedic surgery. Clin Orthop Relat Res 395:99–109
Acknowledgments
This study was supported by the Higher Education Authority of Ireland, under the Programme for Research in Third Level Institutions (PRTLI) Cycle 3, and by a Science Foundation Ireland President of Ireland Young Researcher award (FJOB).
Conflict of interest
The authors of the study have no financial or personal relationships or affiliations that could influence (or bias) the authors’ decisions, work or manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alhag, M., Farrell, E., Toner, M. et al. Evaluation of the ability of collagen–glycosaminoglycan scaffolds with or without mesenchymal stem cells to heal bone defects in Wistar rats. Oral Maxillofac Surg 16, 47–55 (2012). https://doi.org/10.1007/s10006-011-0299-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10006-011-0299-0