Abstract
Research indicates that adolescent psychological symptoms are associated with subsequent mental health disorders. Studies also show the association of leisure activity with improved current and future mental health. However, research is limited on whether social leisure time activity is a mediating link in the association between psychological symptoms and later psychiatric morbidity. We examined whether adolescence-related social leisure time activity, per se, is a mediating link in the association between adolescent psychological symptoms and later psychiatric morbidity. The study population was based on the Northern Finland Birth Cohort 1986 Study (NFBC 1986; n = 6709; 3227 males). Psychological symptoms at age 15–16 years were measured with the Youth Self Report (YSR) questionnaire. Study participants’ psychiatric morbidity by the age of 33 years was assessed using the diagnoses from the nationwide health care registers. Our results showed an association between psychological symptoms and leisure time activities that varied depending on the level of social activity. Leisure time activity was found to be a mediating link between psychological symptoms in adolescence and psychiatric disorders in early adulthood. Adolescence-related leisure time activities, which differed with regard to social interactions, appeared to serve as a mediating link between adolescent psychological symptoms and later onset of psychiatric disorders. Socially active leisure time during adolescence is related to better long-term mental health, while socially inactive leisure time associates with the likelihood of later psychiatric morbidity. To prevent psychiatric disorders, enhancing such leisure time activities in society is highly recommended.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Psychological symptoms occurring during childhood and adolescence are shown to associate with later psychiatric morbidity, particularly in depression and anxiety disorders [1,2,3]. The processes of development of these symptoms into psychiatric disorders are related to several biological and environmental factors which may be either protective or risk-increasing [4] Biological factors, such as genetic vulnerability for psychiatric disorders, have been a continuous research interest for decades [5, 6]. The impact of different environmental factors on mental health disorders is increasingly emphasized in literature [7, 8].
From the family perspective, environmental factors can be categorized into family-related factors and factors outside of the family [9, 10]. Family-related demographics, such as socioeconomic status, parental educational level and marital status, are shown to impact on psychiatric morbidity of offspring [11, 12]. In addition, family functioning (i.e., communication, interactions and relationships within family) is associated with mental health among offspring [13, 14]. Environmental factors outside of the family include various social environments, such as school and neighborhood. These social environments have been shown to have a positive effect on the development of the young person but may also have unfavorable effects by exposing to adverse events, such as bullying or insecurity [1, 15].
Adolescence is a significant age stage in terms of psychological development and later mental health. During this a lot of changes are happening in the development and life of a young person. Maintaining balance during the changes of puberty is challenging. Social relationships and leisure time usually form a significant part of young people’s daily routines and, thus, have a significant impact on young people’s development and general well-being [16, 17] Leisure time activity has been reported to be an environmental factor associated with mental health of children and adolescents [18, 19]. Hobbies such as sports and arts generally associate with positive mental health of those involved [20, 21]. Children and adolescents with active leisure time activities have been documented to have fewer psychological symptoms than their peers without these activities [22,23,24]. People’s behavior and perception of themselves is widely linked to those social groups, where they belong. Social leisure time, therefore, has significant health effects and factors promoting well-being [25]
On the other hand, psychological symptoms of disturbing level have been found to reduce participation in leisure time activities and social relationships. For example, [26] reported that higher levels of internalizing symptoms predicted lower levels of organized activity participation among young people. They interpreted that especially depressive symptoms such as low energy, loss of interest and negative mood can result in less involvement in activities. In addition, [27] showed that children and adolescents with high levels of depressive symptoms may be less active but they may be more involved with increased screen time, which may in turn be associated with increased depressive symptoms.
Recently, we showed at the population level that socially active leisure time in adolescence (ages 15–16 years) was associated with lower incidence of diagnosed psychiatric disorders by young adulthood (from age 16–33 years) [28]. Our finding raised the further research question of whether social leisure time activity, per se, is a mediating link in the association between psychological symptoms and later psychiatric morbidity of the study participants. This study will add new perspective to development of psychological symptoms to diagnosed psychiatric disorders.
Thus, in the current study, following the segmentation approach of the mediation analysis [29], three research objectives and hypotheses were formed: (1) psychological symptoms in adolescence impact on the level of social leisure time activity (SLA), (2) the level of SLA in adolescence affects the onset of psychiatric disorders in young adulthood, and, consequently, (3) SLA in adolescence mediates the relationship between psychological symptoms in adolescence and the onset of psychiatric disorders at ages 16–33 years.
Methods
Study population
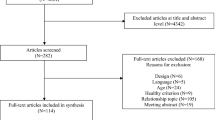
The study population consists of the members of the 1986 Northern Finland Birth Cohort Study (NFBC1986). The Northern Finland Birth Cohort 1986 is a longitudinal follow-up study. It covers all children born alive in Oulu and Lapland from 1 July 1985 to 30 June 1986, altogether 9432 children (4865 boys). For follow-up surveys, 9215 cohort members had a known mailing address in 2001 when the 16-year follow-up study was conducted (https://www.oulu.fi/nfbc/node/18149) Of them, 7344 participants participated in the postal survey at the age of 15–16. In that survey, questions related to Youth Self-Report (YSR) [30] and leisure time activities were answered by 7133 cohort members, of whom 6910 gave permission to use their data for research purposes. The life-time psychiatric disorders of the cohort members are based on the nationwide Care Register for Health Care data covering all inpatient treatment from birth until 2018 and all specialized level outpatient visits for the years 1998–2018. For the purpose of this study, 201 cohort members were excluded because of mental disorder diagnoses set before 16 years of age. Thus, as shown in Fig. 1, the current study comprised 6709 participants, covering 71% of the total 1986 Birth Cohort. Due to missing data on some family-related factors, 5863 participants were included in the logistic regression analyses.
Data sources
The psychiatric disorders were based on the data of specialized level outpatient visits available for the years 1998–2018 and on the inpatient data from the Care Register for Health Care (CRHC) from birth of the cohort members until 2018. The main and secondary diagnoses were taken into account in the screening for psychiatric disorders of the cohort members.
Data on parental mental disorders (F00–F69, F80–F99, main and secondary diagnoses) were defined based on the information from the following national registers: inpatient treatment from the health care register (until 2018), specialized level outpatient visits (1998–2018) and primary health care from the Care Register for Health Care (2011–2018) and disability pension data from the Finnish Center for Pensions (until 2016).
Cohort study participants and their parents were asked for signed consent for use of the data for research purposes. The research was approved by the Ethical Evaluation Board of the Department of Health and Welfare (§28/2009), the Ethical Committee of the Northern Ostrobothnia Hospital District (EETTMK: 108/2017) and the Faculty of Medicine of the University of Oulu, Oulu, Finland. In addition, the administration of each registry gave permission to use individual-level registry-based information for scientific research.
Measures
The level of social leisure time activity in adolescence
The study participants were categorized into three hierarchical and mutually exclusive groups of social leisure activity (SLA) based on their answers to leisure activity questions in a postal questionnaire completed at 15–16 years of age. The following SLA groups were formed: 1. High level of social leisure activity (high SLA) (n = 2111), i.e., the participant belongs to a community or sports club (of the high SLA group, 1,653 (78.6%) belonged to a sports club and 593 (28.1%) belonged to a parish club or scouts and 135 (6.4%), belonged to a sports club and to a parish club or scouts), 2. Middle level of social leisure activity (middle SLA; n = 4485), i.e., the participant has leisure time activity, where other people have to be considered, but he/she does not belong to a community or a sports club, such as dancing or badminton, and 3. Low level of social leisure activity (low SLA) (n = 215), i.e., the participant only has activities that can be done alone, such as reading, cycling or listening to music. The detailed description of the definition of SLA groups is presented in our earlier publication [28].
Psychological symptoms in adolescence according to Youth Self Report (YSR) questionnaire
The 16-year follow-up survey was conducted between the years 2001 and 2002 ((https://www.oulu.fi/sites/default/files/postikysely_eng_1.pdf)). It contained a self-assessment postal questionnaire on health and well-being, including questions on physical health, psychosocial well-being, living habits and the Youth Self Report (YSR) questionnaire.
The YSR is a self-report questionnaire for 11–18 years developed by [31]. In the 16-year postal survey, the items of the YSR were based on 1991 version. The categorization of the 88 items into eight subscales was based on the 2001 version of the modified scale [30, 32, 33]. The adolescent assesses on how each statement comes true now or came true in the last 6 months. The eight subscales of the YSR include scales for (1) anxious/depressed (13 items), (2) withdrawn/depressed (7 items), (3) somatic complaints (10 items), (4) social problems (10 items), (5) thought problems (12 items), (6) attention problems (7 items), (7) rule-breaking behavior (12 items) and (8) aggressive behavior (17 items).
Furthermore, three combined scales were formed by combining selected subscales, the first named as internalizing symptoms scale (including subscales for anxious/depressed, withdrawn/depressed and somatic complaints) and the second as externalizing symptoms scale (including subscales for rule-breaking behavior and aggressive behavior). The rest of the subscales (social problems, thought problems and attention problems) were included in the combined scale “other psychological symptoms”. The YSR total score included the scores of all eight subscales.
For statistical analyses, the sum score of the total YSR, of each subscale and of each combined scale was calculated. If less than three items were missing in a subscale, missing values were replaced by the mean of the subscale from that study participant. If three or more items were missing, the corresponding subscale was removed for that person. Mean-imputated subscales were used to compute YSR total score as well as internalizing, externalizing and other symptoms.
For further statistical analyses, the sum scores of the YSR scales were dichotomized at 82nd percentile of the distribution of a scale [34]. In that study, the 82nd percentile was suggested to be the optimal cutoff score for indicating the presence of a mental health condition. In our study, these cutoffs were calculated separately for males (total score 33.0, internalizing symptoms 10.5, externalizing symptoms 14.0 and other symptoms 10.0) and females (total score 47.0, internalizing symptoms 18.0, externalizing symptoms 16.0 and other symptoms 14.1). The gender-specific values were calculated, because it is known that psychological symptoms are linked to age [35,36,37].
Psychiatric disorders of the study participants
The main outcome variables were diagnosed psychiatric disorders of the study subjects set for the first time at ages 16–33 years. In addition to any psychiatric disorders (ICD-10 codes: F00–F99), the following main diagnostic categories were analyzed: mental and behavioral disorders due to psychoactive substance use (F10–F19); schizophrenia, schizotypal, delusional and other non-mood psychotic disorders (F20–F29); mood (affective) disorders (F30–F39); anxiety, dissociative, stress-related, somatoform and other nonpsychotic mental disorders (F40–F49), and behavioral and emotional disorders with onset usually occurring in childhood and adolescence (F90–F98). These psychiatric diagnostic categories were chosen, because the preliminary analyses (data not presented) showed them to be the most prevalent diagnostic categories, justifying the purpose of the subsequent statistical analysis.
Family-related covariates
In our study, the selection of the family-related covariates as indicators for environmental factors was based on the previous literature reporting significant findings on their association with mental health and welfare of offspring; single parenthood [38], parents’ education [39] and parental mental health problems [11]. Information of family structure and parents’ education was based on a postal questionnaire that the parents filled in when the cohort participants were aged 15–16 (https://www.oulu.fi/sites/default/files/postikysely_eng_2.pdf). In the current study, the variable biological parents not living together means that the parents have never lived together, they are divorced from marriage or from co-habiting, or a parent has died. Parental educational level indicates that at least secondary level of education was completed by the study participant’s mother or father. The data of parent’s mental disorders (F00–F69, F80–F99, main and secondary diagnoses) were extracted from the following nationwide registers: inpatient treatment from the Care Register for Health Care (until 2018), specialized level outpatient visits (1998–2018) and primary care (2011–2018), from the Care Register for Health Care and information of disability pensions from the Finnish Center for Pensions (until 2016). The distribution of the family-related covariates is presented in supplementary material. See Appendix 1.
Statistical methods
In our study, the analyses relating to the concept of mediator was based on the segmentation approach described by Memon et al. [29] 2018. In the segmentation approach (Fig. 2), three research aims, and hypotheses are developed as follows: (1) independent variable (X, i.e., in our study, psychological symptoms in adolescence) effects mediator (M, i.e., social leisure time activity in adolescence), (2) mediator (M) effects outcome variable (Y, i.e., psychiatric morbidity by young adulthood) and (3) M mediates the relationship between X and Y. Statistical significance of group differences in categorical variables was assessed with Pearson Chi-square test and in continuous variables with Mann–Whitney U test. The association of the level of social leisure time activity and psychological symptoms (YSR scores in adolescence) with psychiatric disorder diagnosed at ages 16 through 33 years was examined using a binary logistic regression analysis after controlling for gender and family-related covariates (biological parents living together, parental education level and parental psychiatric disorders) of the study participants).
The primary analyses relating to the YSR scale were based on the cutoff point of 82nd percentile of distribution, which is suggested to indicate the presence of a mental health condition [34]. This cutoff point was applied to the sum score of the total YSR scale and to sum scores of the subscales for internalizing symptoms, externalizing symptoms, and other symptoms. In logistic regression analyses, Model 1 was formed for the total YSR scale and Model 2 for its three subscales (internalizing, externalizing and other symptoms). To evaluate the robustness of our findings, we also conducted sensitivity analyses, in which YSR sum scores were entered to the models as continuous variables (see Supplemental Table 1).
In terms of the eight subscales of the YSR (anxious/depressed, withdrawn/depressed, somatic complaints, social problems, thought problems, attention problems, rule-breaking behavior, aggressive behavior (17 items), the association of these subscales with the levels of SLA and psychiatric disorder diagnosed between ages 16–33 years were explored and visualized with boxplots (see Supplemental Figures 1-2). In additional analysis (see Supplemental Table 2), the association of each of the eight subscales (using 82nd cutoff for sum score) and the level of SLA in adolescence to likelihood of later psychiatric disorder was examined after controlling for covariates.
The statistical software used in analyses was IBM SPSS Statistics 25.
Results
Association of psychological symptoms with social leisure time activity in adolescence
In the current study sample (n = 6709), the proportion of study participants exceeding the cutoff of 82nd percentile (indicating the presence of a mental health condition) of the total YSR scores was 26.2% (n = 54/206) in low-SLA, 18.5% (n = 817/4422) in middle-SLA and 15.1% (n = 315/2081) in high-SLA groups (p < = 0.001). The corresponding proportions for internalizing psychological symptoms were 33.0% (n = 31), 19.0% (n = 848) and 15.7% (n = 330) (p < 0.001) and for externalizing symptoms, 14.6% (n = 31), 21.1% (n = 943), and 16.4% (n = 343) (p < 0.001). In psychological symptoms other than internalizing or externalizing symptoms, the proportions were 32.5% (n = 67) in low-SLA, 19.5% (n = 865) in middle-SLA, and 16.4% (n = 342) in high-SLA groups of the study participants (p < 0.001).
SLA and psychological symptoms in adolescence in relation to later psychiatric morbidity
Table 1 shows the incidence of psychiatric disorders diagnosed at ages 16–33 years of the study participants (n = 6709) in relation to the level of SLA and psychological symptoms assessed in adolescence (ages 15–16). Overall, the incidence of any psychiatric disorders diagnosed for the first time at 16–33 years of age was 14.6% (n = 979), the incidence (from highest to lowest) being 7.7% (n = 525) in anxiety, 7.6% (n = 511) in affective disorders, 2.9% (n = 197) in substance use, 1.4% (n = 96) in psychotic and 1.1% (n = 76) in behavioral disorders.
The level of SLA in adolescence was statistically significantly associated with the incidence of any and specific psychiatric disorders, except in psychotic disorders. The incidence of psychiatric disorders was highest in the low SLA group, being 21.8% in any psychiatric disorder (range from 1.9% in psychotic disorders to 15.0% in anxiety disorders). Furthermore, the incidence was lowest in the high SLA group, being 11.8% in any psychiatric disorder (range from 1.0% in behavioral disorders to 6.1% in anxiety disorders).
The proportion of study participants presenting clinical-level psychological symptoms in adolescence (the YSR scores ≥ 82nd percentile of the YSR scores) was statistically significantly associated with the incidence of any and all specific psychiatric disorder groups. In total YSR scores, the prevalence of study participants exceeding the 82nd percentile of the scores was 23.6% in any psychiatric disorders (range from 2.6% in behavioral disorders to 13.8% in affective disorders). The corresponding prevalence for internalizing symptoms was 22.1% in any psychiatric disorders (range from 2.1% in behavioral disorders to 13.4% in affective disorders), for externalizing symptoms 20.4% in any psychiatric disorder (range from 2.5% in psychotic disorders to 11.8% in affective disorders) and for other psychological symptoms, 23.6% in any psychiatric disorders (range from 2.6% in behavioral disorders to 13.8% in affective disorders).
SLA and psychological symptoms in adolescence as predictors for later psychiatric morbidity
Table 2 presents the results of the adjusted logistic regression analyses examining the association of the level of social leisure time activity and self-reported psychological symptoms in adolescence (ages 15–16 years) with likelihood of psychiatric disorder diagnosed for the first time between ages 16 and 33 years. In Model 1, high total YSR scores in adolescence were related to increased likelihood for any or all specific psychiatric disorders among the study participants. Furthermore, low-SLA was associated with increased likelihood for any psychiatric disorders and for anxiety and behavioral disorders, while high-SLA was related to decreased likelihood for any psychiatric disorders, substance use and affective disorders. As Model 2 shows, in high-SLA group the likelihood for any psychiatric disorder and for affective disorders was decreased, whereas it was increased in those study participants with high scores in internalizing and other symptoms. High-SLA was associated with decreased likelihood for substance use disorders, while the likelihood for that disorder was increased in those with high scores in externalizing and other symptoms in adolescence. Increased likelihood for anxiety disorders was linked with low-SLA as well as with high scores in internalizing and other symptoms in adolescence. Furthermore, behavioral disorders associated with low-SLA and with high scores in externalizing symptoms. The increased likelihood for psychotic disorder was related to high scores of other psychological symptoms (social problems, thought problems and attention problems), besides than externalizing and internalizing, but not with any level of SLA in adolescence.
Figure 3 illustrates the association of SLA and YSR in adolescence with the incidence of psychiatric disorder. Among the study participants with high YSR scores in adolescence, the highest incidence of any psychiatric disorder was observed in the low SLA group, 35.2%, degreasing to 19.4% in the high SLA group. Furthermore, among the study participants with a low YSR in adolescence, the incidence of psychiatric disorders was notably lower, being 17.1% in the low SLA group and dropping to 10.4% in the high SLA group.
A sensitivity analysis was conducted using continuous YSR scores instead of using the YSR 82nd percentile cutoffs in logistic regression models 1 and 2 (see Supplemental Table 1). There were no major changes in statistically significant associations of the levels of SLA and YSR scores with psychiatric disorders. The associations with YSR subscale for other psychological symptoms remained beyond statistical significance only in psychotic disorders and anxiety disorders.
Discussion
Earlier research has provided wide evidence that active leisure time associates with positive mental health. There is also some research suggesting that leisure time activity can serve as protecting factor for psychiatric morbidity. However, the role of different types of hobbies in the development process of psychological symptoms into mental disorders is not clear. Identification of whether different types of leisure time activities mediate this transition would facilitate the development of preventive psychosocial actions and, thus, might reduce the need for later psychiatric treatment.
In this study we were able to investigate at the population level the role of leisure time as a link between psychological symptoms and psychiatric disorders. Regarding the mediation approach applied in our study, we were able to show the association between adolescence-related psychological symptoms and leisure time activities that differed in terms of the level of social activity. Among the study participants, a high level of psychological symptoms was associated with participation in socially low-level leisure time activity in adolescence. One indicator of this link was the observed association of high scores in internalizing symptoms with a low level of social leisure time activity (low-SLA). Respectively, a decreased level of internalizing symptoms was associated with a high level of social leisure time activity (high-SLA). These findings are consistent with previous studies reporting that individual’s depressive symptoms associate with spending less time in social interactions [40, 41].
Second, our study indicated the association between the level of social leisure time activity in adolescence and subsequent psychiatric disorders in early adulthood. The level of adolescence-related social leisure time activity was statistically significantly associated with the incidence of psychiatric disorders later in life and, specifically, with all analyzed psychiatric diagnostic categories, except in psychotic disorders. Our finding is in line with the studies documenting that participation in meaningful social leisure time activities has a positive longitudinal impact on mental health [3, 42]
Thirdly, adolescence-related leisure time activity as a mediating link between psychological symptoms in youth and psychiatric disorders in early adulthood was established in our study. This was seen, for example, in our finding that high total YSR score, together with low social leisure time activity, in adolescence was related to increased likelihood for any psychiatric diagnoses. Similarly, high social leisure time activity was related to decreased likelihood for psychiatric disorders regardless of high YSR scores in adolescence. We were able to adjust our analyses with commonly known family-related risk factors for psychiatric morbidity of the offspring, such as parents’ mental health disorders [12], parental educational level [39] and living with a single parent [38]. Thus, the impact of these risk factors on the occurrence of psychological symptoms as well as on the possibility to participate in leisure time activities in adolescence is controlled with regard to the onset of psychiatric disorders of the study subjects. Worth to noticing is, however, that when interpreting the findings of our study it is important to consider that severity of primary psychological symptoms may have affected to participation in hobbies and, thus, also be the main reason to manifestation of psychiatric disorders.
In general, previous research has widely acknowledged the association of adolescence-related psychological symptoms with later psychiatric morbidity [43,44,45]. For example, in the longitudinal study of Ormel and workgroup [46], it was found that adult mental health disorders are often preceded by psychological symptoms with onset during adolescence. The results of our study further suggest that the development of symptoms into diagnosed psychiatric disorders is mediated by a variety of factors, such as social leisure time activity in our study.
Exploring mediating links between symptoms and disorders gives new potential to construct targeted preventive actions for children and adolescents. In these actions, development of interaction skills and community’s ability to enhance individual’s sense of belonging to the community are primary targets, because they are known to associate with positive psychological outcomes and resilience among young people [47, 48]. For example, in the cohort study of Scardera and coworkers, 18 years with anxiety, depression or suicide risk reported fewer mental health problems after a year after receiving community support [49]. In addition, participation in organized leisure activities has shown to predict a low level of internalizing symptoms and to support positive mental health [50]. Early community-based activities have also been reported to have a long-term positive impact on mental health. Furthermore, participating in scouting in adolescence has been found to associate with better mental health at the age of 50 [51]. Their study reported that community-based support had a positive effect especially on children growing up in socially disadvantaged households. Therefore, it is highly important to organize various community leisure time activities especially for children and young people who are exposed to different adversities.
Strengths and limitations
The strength of this study is the well-documented sample of young people who were followed for psychiatric morbidity from the age to 15–16 years until the age of 33 years. The 1986 Northern Finland Birth Cohort Study population can be considered as representative of Finnish adolescents. The national health care registers used in the current study have shown to be reliable for research purposes. [33]. Another strength of this study was that psychological symptoms were assessed with the Youth Self Report (YSR) questionnaire, which is a widely and commonly used measure for assessing youth emotional and behavioral problems. [52]. The third strength of this study is that mental disorder diagnoses of the study participants were extracted from nationwide healthcare registers including all inpatient hospitalizations and specialized level outpatient visits. The diagnoses in health care registers are always set by doctors and the diagnoses are based on criteria of the ICD classification of diseases.
A limitation of the study is that the small number of cases in the subgroup analyses may have caused lack of power in statistical analyses (Type II error). In addition, due to the many statistical comparisons performed in this study the possibility of chance findings (Type I error) cannot be excluded.
Conclusion
Our study presents new information that adolescence-related leisure time activities that differ with regard to social interactions can serve as a mediating link between adolescent psychological symptoms and later onset of psychiatric disorders. Socially active leisure time during adolescence is related to better long-term mental health, while socially inactive leisure time associates with the likelihood of later psychiatric morbidity. To prevent psychiatric disorders, it is highly recommended that such leisure time activities are enhanced in society.
Change history
12 April 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00787-023-02202-y
References
Fryers T, Brugha T (2013) Childhood determinants of adult psychiatric disorder. Clin Pract Epidemiol Ment Health 9:1–50. https://doi.org/10.2174/1745017901309010001
Hansen E, Sund E, Knudtsen MS, Krokstad S, Holmen T (2015) Cultural activity participation and associations with self-perceived health, life-satisfaction and mental health: the Young HUNT Study Norway. BMC Public Health 15(1):1–8. https://doi.org/10.1186/s12889-015-1873-4
Doré I, O’Loughlin JL, Beauchamp G, Martineau M, Fournier L (2016) Volume and social context of physical activity in association with mental health, anxiety and depression among youth. Prev Med 91:344–350. https://doi.org/10.1016/j.ypmed.2016.09.006
Keyes C, Dhingra S, Simoes., E. (2010) Change in level of positive mental health as a predictor of future risk of mental illness. Am J Public Health 100(12):2366–2371. https://doi.org/10.2105/AJPH.2010.192245
Kendler KS, Prescott CA, Myers J, Neale MC (2003) The structure of genetic and environmental risk factors for common psychiatric and substance use disorders in men and women. Arch Gen Psychiatry 60(9):929–937. https://doi.org/10.1001/archpsyc.60.9.929
Patel V, Flisher AJ, Hetrick S, McGorry P (2007) Mental health of young people: a global public-health challenge. Lancet 369(9569):1302–1313. https://doi.org/10.1016/S0140-6736(07)60368-7
Gass K, Jenkins J, Dunn J (2007) Are sibling relationships protective? A longitudinal study. J Child Psychol Psychiatry 48(2):167–175
Hughes K, Lowey H, Quigg Z, Bellis MA (2016) Relationships between adverse childhood experiences and adult mental well-being: results from an English national household survey. BMC Public Health 16:222. https://doi.org/10.1186/s12889-016-2906
Bentzies K, Mychasiuk R (2009) Fostering family resiliency: a review of the key protective factors. Child Fam Soc Work 14(1):103–114. https://doi.org/10.1111/j.1365-2206.2008.00586.x
Rose RJ, Viken RJ, Dick DM, Bates JE, Pulkkinen L, Kaprio J (2003) It does take a village: nonfamilial environments and children’s behaviour. Psychol Sci 14(3):273–277. https://doi.org/10.1111/1529-1006.03434
Merikukka M, Räsänen S, Hakko H, Ristikari T, Gissler M, Niemelä M (2018) Association between parental hospital-treated somatic illnesses in childhood and later mental disorders among offspring up to early adulthood: an explorative study in the 1987 Finnish Birth Cohort. Scand J Public Health. https://doi.org/10.1177/1403494818774729
Sciaraffa M, Zeanah P, Zeanah C (2018) Understanding and promoting resilience in the context of adverse childhood experiences. Early Childhood Educ J 46(3):343–353
Lewandowski A, Palermo T, Stinson J, Handley S, Chambers C (2010) Systematic review of family functioning in families of children and adolescents with chronic pain. J Pain 11(11):1027–1038. https://doi.org/10.1016/j.jpain.2010.04.005
Myllyaho T, Siira V, Wahlberg KE, Hakko H, Tikkanen V, Läksy K, Roisko R, Niemelä M, Räsänen S (2021) Dysfunctional family functioning in high socioeconomic status families as a risk factor for the development of psychiatric disorders in adoptees: the Finnish Adoptive Family Study of Schizophrenia. Social Psychiatry Psychiatri Epidemiol. https://doi.org/10.1007/s00127-020-02016-2
Grych J, Taylor E, Banyard V, Hamby S (2020) Applying the dual factor model of mental health to understanding protective factors in adolescence. Am J Orthopsychiatr 90(4):458–467. https://doi.org/10.1037/ort0000449
Urke H, Holsen I, Larsen T (2021) Positive youth development and mental well-being in late adolescence: the role of body appreciation. Findings from a prospective study in norway. Front Psychol. https://doi.org/10.3389/fpsyg.2021.696198
Brizio A, Gabbatore I, Tirassa M, Bosco F (2015) “No more a child, not yet an adult”: studying social cognition in adolescence. Front Psychol. https://doi.org/10.3389/fpsyg.2015.01011
Aaltonen S, Kujala U, Kaprio J (2014) Factors behind Leisure-time physical activity behavior based on finnish twin studies: the role of genetic and environmental influences and the role of motives. Biomed Res Int. https://doi.org/10.1155/2014/931820
Santini Z, Meilstrup C, Hinrichen C, Nielsen L, Koyanagi A, Koushede V, Ekholm O, Rich Madsen K (2020) Associations between multiple leisure activities, mental health and substance use among adolescents in denmark: a nationwide cross-sectional study. Front Behav Neurosci. https://doi.org/10.3389/fnbeh.2020.593340
Oberle E, Xuejun RJ, Guhn M, Schonert-Reichl KA, Gadermann AM (2019) Benefits of extracurricular participation in early adolescence: associations with peer belonging and mental health. J Youth Adolesc 48(11):2255–2270. https://doi.org/10.1007/s10964-019-01110-2
Kleppang A, Thurston M, Hartz I, Hagquist C (2019) Psychological distress among Norwegian adolescents: changes between 2001 and 2009 and associations with leisure time physical activity and screen-based sedentary behavior. Scand J Public Health 47(2):166–173. https://doi.org/10.1177/1403494817716374
Ferreira V, Jardim T, Póvoa T, Viana R, Sousa A, Jardim P (2020) Physical inactivity during leisure and school time is associated with the presence of common mental disorders in adolescence. Rev Saude Publica 54:128
Ma L, Hagquist C, Kleppang AL (2020) Leisure time physical activity and depressive symptoms among adolescents in Sweden. BMC Public Health 20(1):997. https://doi.org/10.1186/s12889-020-09022-8
Bélair MA, Kohenn DE, Kingsbury M, Colman I (2018) Relationship between leisure time physical activity, sedentary behaviour and symptoms of depression and anxiety: evidence from a population-based sample of Canadian adolescents. BMJ Open 8(10):e021119. https://doi.org/10.1136/bmjopen-2017-021119
Jetten J, Haslam C, von Hippel C, Bentleym S, Cruwys T, Steffens N, Haslam A (2022) “Let’s get physical” — or social: the role of physical activity versus social group memberships in predicting depression and anxiety over time. J Affective Disorders. https://doi.org/10.1016/j.jad.2022.03.027
Bohnert A, Kane P, Garber J (2008) Organized activity participation and internalizing and externalizing symptoms: reciprocal relations during adolescence. J Youth Adolescence 37:239–250. https://doi.org/10.1007/s10964-007-9195-1
Kremer P, Elshaug C, Leslie E, Toumbourou J, Patton G, Williams J (2013) Physical activity, leisure-time screen use and depression among children and young adolescents. J Sci Med Sport 17(2):183–187. https://doi.org/10.1016/j.jsams.2013.03.012
Timonen J, Niemelä M, Hakko H, Alakokkare A, Räsänen S (2021) Associations between adolescents’ social leisure activities and the onset of mental disorders in young adulthood. J Youth Adolesc 50:1757–1765. https://doi.org/10.1007/s10964-021-01462-8
Memon MA, Jun-Hwa C, Ramayah T, Hiram T, Chuach F (2018) Mediation analysis issues and recommendations. J Appl Struct Equ Model 2(1):i–ix. https://doi.org/10.47263/JASEM.2(1)01
Achenbach TM (1991) Manual for the Youth Self-Report and 1991 Profile. University of Vermont, Department of Psychiatry, Burlington
Achenbach TM, Edelbrock C (1987) Manual for Youth Self-Report and Profile. University of Vermont, Department of Psychiatry, Burlington, VT
Achenbach TM., & Rescorla LA. (2001). Manual for the ASEBA School-Age Forms & Profiles. University of Vermont, Research Center for Children, Youth, and Families, Burlington
Miettunen J, Murray GK, Jones PB, Mäki P, Ebeling H, Taanila A, Joukamaa M, Savolainen J, Törmänen S, Järvelin M-R, Veijola J, Moilanen I (2014) Longitudinal associations between childhood and adulthood externalizing and internalizing psychopathology and adolescent substance use. Psychol Med 44:1727–1738. https://doi.org/10.1017/S0033291713002328
Hurtig T, Taanila A, Ebeling H, Miettunen J, Moilanen I (2005) Attention and behavioural problems of Finnish adolescents may be related to the family environment. Europ Child Adolescent Psych 14(8):471–478. https://doi.org/10.1007/s00787-005-0492-5
Solmi M, Radua J, Olivola M, Croce E, Soardo L, Salazar de Pablo G, Shin J, Kirkbride JB, Jones P, Kim J, Kim JY, Carvalho A, Seeman M, Correll C, Fusar-Poli P (2021) Age at onset of mental disorders worldwide: large-scale meta-analysis of 192 epidemiological studies. Mol Psychiatry. https://doi.org/10.1038/s41380-021-01161-7
Van Drookenbroeck F, Spruyt B, Keppens G (2018) Gender differences in mental health problems among adolescents and the role of social support: results from the Belgian health interview surveys 2008 and 2013. BMC Psychiatry. https://doi.org/10.1186/s12888-018-1591-4
Seedat S, Scott K, Angermayer M, Berglund P, Bromet E, Brugha T, Demyttenaere K, Girolamo G, Haro J, Jin R, Karam E, Kovess-Masfety V, Levinson D, Mora M, Ono Y, Ormel J, Pennell B-E, Poseda-Villa J, Sampson N, Williams D, Kessler R (2009) Cross-national associations between gender and mental disorders in the World Health Organization World Mental Health Surveys. Arch Gen Psychiatry 66(7):785–795. https://doi.org/10.1001/archgenpsychiatry.2009.36
Amato P (2000) The Consequences of divorce for adults and children. J Marriage Family 62(4):1269–1287. https://doi.org/10.1111/j.1741-3737.2000.01269.x
Paananen R, Santalahti P, Merikukka M, Rämö A, Wahlbeck K, Gissler M (2013) Socioeconomic and regional aspects in the use of specialized psychiatric care—a Finnish nationwide follow-up study. EUR J Public Health 23(3):372–377. https://doi.org/10.1093/eurpub/cks147
Brown LH, Strauman T, Barrantes-Vidal N, Silvia PJ, Kwapil TR (2011) An experience-sampling study of depressive symptoms and their social context. J Nerv Ment Dis 199(6):403–409
Elmer T, Stadtfeld C (2020) Depressive symptoms are associated with social isolation in face-to-face interaction networks. Sci Rep 10:1444. https://doi.org/10.1038/s41598-020-58297-9
Hoegh Poulsen P, Biering K, Andersen JH (2016) The association between leisure time physical activity in adolescence and poor mental health in early adulthood: a prospective cohort study. BMC Public Health 16:3. https://doi.org/10.1186/s12889-015-2658-5
Phillip J, Zeiler M, Waldherr K, Truttman K, Wolfgang D, Karwautz A, Wagner G (2018) Prevalence of emotional and behavioral problems and subthreshold psychiatric disorders in Austrian adolescents and the need for prevention. Soc Psychiatry Psychiatric Epidemiol 53(2):1–13. https://doi.org/10.1007/s00127-018-1586-y
Kessler R, Amminger G, Aguilar-Gaxiola S, Alenso J, Lee S, Ustün T (2007) Age of onset of mental disorders: a review of recent literature. Curr Opin Psychiatry 20(4):359–364
Sourander A, Multimäki P, Nikolakaros G, Haavisto A, Ristikari T, Helenius H, Parkkola K, Piha J, Tamminen T, Moilanen I, Kumpulainen K, Almqvist F (2005) Childhood predictors of psychiatric disorders among boys: a prospective community-based follow-up study from age 8 years to early adulthood. J Am Acad Child Adolesc Psychiatry 44(8):725–838. https://doi.org/10.1097/01.chi.0000164878.79986.2f
Ormel J, Raven D, van Oort F, Hartman CA, Reijneveld SA, Veenstra R, Vollebergh WAM, Buitelaar J, Verhulst FC, Oldehinkel AJ (2015) Mental health in Dutch adolescents: a Trails report on prevalence, severity, age of onset, continuity and co-morbidity of DSM disorders. Psychol Med 45(2):345–360. https://doi.org/10.1017/S0033291714001469
Lerner RM, Lerner JV, Almerigi JB, Theokas C, Phelps E, Gestsdottir S, Naudeau S, Jelicic H, Alberts A, Ma L, Smith LM (2005) Positive youth development, participation in community youth development programs, and community contributions of fifth-grade adolescents: findings from the first wave of the 4-h study of positive youth development. J Early Adolescence 25(1):17–71. https://doi.org/10.1177/0272431604272461
Ungar M (2012) Researching and theorizing resilience across cultures and contexts. Prev Med 55(5):387–389. https://doi.org/10.1016/j.ypmed.2012.07.021
Scardera S, Perret L, Ouellet-Morin I (2020) Association of social support during adolescence with depression, anxiety, and suicidal ideation in young adults. JAMA Netw Open 3(12):e2027491. https://doi.org/10.1001/jamanetworkopen.2020.27491
McWood L, Erath S, Pettit G, Bates J, Dodge K, Landsford J (2021) Organized activity involvement predicts internalizing and externalizing problems in adolescence. J Youth Adolesc 50:2181–2193. https://doi.org/10.1007/s10964-021-01491-3
Dibben C, Playfort C, Mitchell R (2017) Be(ing) prepared: guide and Scout participation, childhood social position and mental health at age 50—a prospective birth cohort study. Epidemiol Community Health 71:275–281. https://doi.org/10.1136/jech-2016-207898
Ebesutani C, Bernstein A, Martinez IJ, Chorpita FB, Weisz J (2011) The youth self report: applicability and validity across younger and older youths. J Clin Child Adolesc Psychol 40(2):338–346. https://doi.org/10.1080/15374416.2011.546041
Funding
Open Access funding provided by University of Oulu including Oulu University Hospital. This study was supported by a grant from ITLA Children’s Foundation (Researchers JT and MN), Stiftelsen Alma och K.A Snellman Foundation (Researcher JT), and Strategic Research Council(SRC) established with in the Academy of Finland, decision number 352509 (Researcher MN).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study obtained approval from the Ethical Review Board of the National Institute for Health and Welfare (§28/2009), the Ethics Committee of Northern Ostrobothnia Hospital District (EETTMK: 108/2017) and Oulu University, Faculty of Medicine, Oulu, Finland.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants involved in the study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Timonen, J., Niemelä, M., Hakko, H. et al. Social leisure time activities as a mediating link between self-reported psychological symptoms in adolescence and psychiatric morbidity by young adulthood: the Northern Finland 1986 Birth Cohort study. Eur Child Adolesc Psychiatry 32, 2569–2580 (2023). https://doi.org/10.1007/s00787-022-02107-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-022-02107-2