Abstract
Adolescent mental health and well-being have been adversely impacted by the COVID-19 pandemic. In this preregistered longitudinal study, we evaluated whether adolescents’ well-being improved after playing the multiplayer serious game app Grow It! During the first lockdown (May–June 2020), 1282 Dutch adolescents played the Grow It! app (age = 16.67, SD = 3.07, 68% girls). During the second lockdown (December–May 2020 onwards), an independent cohort of 1871 adolescents participated (age = 18.66, SD = 3.70, 81% girls). Adolescents answered online questionnaires regarding affective and cognitive well-being, depressive symptoms, anxiety, and impact of COVID-19 at baseline. Three to six weeks later, the baseline questionnaire was repeated and user experience questions were asked (N = 462 and N = 733 for the first and second cohort). In both cohorts, affective and cognitive well-being increased after playing the Grow It! app (t = − 6.806, p < 0.001; t = − 6.77, p < 0.001; t = − 6.12, p < 0.001; t = − 5.93, p < 0.001; Cohen’s d range 0.20–0.32). At the individual level, 41–53% of the adolescents increased in their affective or cognitive well-being. Adolescents with higher risk profiles (i.e., more depressive symptoms, lower atmosphere at home, and more COVID-19 impact) improved more strongly in their well-being. Positive user evaluations and app engagement were unrelated to changes in affective and cognitive well-being. This proof-of-concept study tentatively suggests that Grow It! supported adolescents during the pandemic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mental health is broadly defined as the presence of positive indicators and the absence of negative indicators such as depressive symptoms or anxiety [1]. Well-being, in turn, entails both cognitive appraisal of life satisfaction (cognitive well-being) as well as affective components such as happiness (affective well-being) [2]. Investing in well-being may, as such, improve mental health.
Already before the COVID-19 pandemic, the need for psychological and psychiatric professional services outweighed the resources, resulting in long waiting lists [3]. COVID-19-induced social restrictions, such as homeschooling, social distancing, and limited opportunities for sports and leisure, have negatively impacted adolescent well-being and mental health [4,5,6,7,8]. Moreover, there is growing evidence on health-related outcomes such as decreases in physical activity during quarantine that may have contributed to an increase in adolescent mental health problems and depressive symptoms [9, 10], all in all making the shortage of professional services even more pressing [10]. Mobile Health (mHealth) can improve early identification, prevention, and treatment of mental health problems [11, 12], without being limited to professional resources: it is scalable and accessible, as adolescents can use mHealth interventions whenever and wherever they want. Moreover, feasibility studies suggest that adolescents perceive mHealth as less stigmatizing compared to face-to-face health care [13]. Even though several tools are currently available, the effects of online support are still poorly understood [14].
Grow It! has been developed for adolescents aged 12–25 years to improve adolescents’ affective and cognitive well-being, and consists of two components. Firstly, adolescents monitor their emotions and behaviors in daily life by utilizing the experience sampling method (ESM). This reporting on emotions at several random times per day may increase reflection and self-insights [15]. Second, Grow It! teaches how to cope with setbacks and promotes emotional resilience by offering daily challenges. As cognitive behavioral therapy (CBT) is one of the most effective interventions widely applied in psychological (preventive) care [16,17,18], the daily challenges are based on CBT and are aimed at strengthening adaptive coping, supporting physical activation and preventing emotional problems. The smartphone app, game mechanics and the daily challenges were co-created by adolescents, child psychologists/psychiatrists, researchers, and game designers. The developmental process, feasibility, and acceptability of the Grow It! app have been described elsewhere [19].
The Grow It! app was first launched during the COVID-19 pandemic. The current preregistered study tested four research questions: (1) first, we tested whether adolescents’ affective and cognitive well-being increased after playing the Grow It! app. We further described (2) how many adolescents increased in their affective and cognitive well-being. Finally, we explored (3) to which extent individual background characteristics and (4) user evaluations and engagement were associated with changes in affective and cognitive well-being.
Methods
Procedure and participants
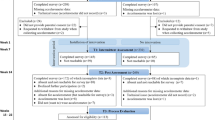
In May 2020, during the first lockdown, 1282 adolescents (cohort 1: mean age 16.67 years, SD = 3.07, 68% girls) played the Grow It! app for 6 weeks (Fig. 1). In December 2020, during the second lockdown, another 1,871 adolescents (cohort 2: mean age 18.66 years, SD = 3.70, 81% girls) played the app for 3 weeks. To participate, adolescents needed to be able to read and write Dutch, live in the Netherlands, and own a smartphone. Non-probability convenience sampling took place via advertisements and a promotion video on (social) media and through online announcements by schoolteachers. All study information was published on our website, where it was also possible to contact the team of researchers, and sign the informed consent on a secure webpage for participants and also for parents if the age of the child was < 16 years. After the online baseline questionnaire (codebook), participants received an SMS with a unique login code to activate the app. Table 1 shows sample characteristics, Table 2 shows descriptive statistics of all study variables.
The Grow It! study was conducted in accordance with the guidelines proposed in the World Medical Association Declaration of Helsinki and has been approved by the Medical Ethical Committee of the Erasmus Medical Centre (registration number: MEC2020-0287).
Description of the Grow It! app
The Grow It! application is a multiplayer serious gaming smartphone tool (Android/iOS) aimed at promoting well-being (Fig. 2). Participants are randomly allocated to a team of four to six players. Within the app, each team collaborates in nurturing and embellishing their virtual tree, which grows each time the team reaches a predefined number of points (‘spurt’). Individual players earn points by filling out ESM questionnaires five random times per day between 9:00 and 21:00 and by completing daily challenges aimed at promoting adaptive coping including: social support, acceptance, problem-solving, and distraction. For instance, take a picture of a red car (photo challenge: aimed at distraction), ask someone what they like about you and write it down (assignment: aimed at social support), or ask someone whether he/she is having difficulties with and come up with a solution together. Write it down (assignment: aimed at problem solving)! Every day, adolescents can choose one out of three challenges. To demonstrate the successful accomplishment of a challenge, adolescents can either upload pictures, answer a free text form, or select the right answer option. Team members can communicate and motivate each other by means of positive stickers (chat function). Its privacy and security were approved by the privacy and security office of Erasmus MC, and the app complies with the Dutch General Data Protection Regulation (GDPR) and NEN-norm 7510:2017 (Dutch standard of information security management systems in healthcare).
Measures
Well-being
As primary outcome, well-being was assessed at baseline and follow-up using two items [2]. The first item refers to affective well-being: “How happy did you feel in the past week?” rated on a seven-point scale ((1) not at all to (7) very much). Previous work shows good convergent validity of this single items measurement of affective well-being [19]. The second item assessed cognitive well-being: “How satisfied were you with your life in the past week?” and was rated on a ten-point scale ((1) not at all to (10) very much). The single item measure of cognitive well-being has been demonstrated to have good reliabilities that are comparable to multiple-item scales [20].
Depressive symptoms
Depressive symptoms were measured at baseline and follow-up with the short 12-item Children’s Depression Inventory questionnaire (CDI [21]). Each item has three statements from which the adolescent could choose the one that would best describe him/her over the last week. For example: ‘I am sad sometimes’ (0), ‘I am often sad’ (1), and ‘I am sad all the time’ (2). Total scores ranged from 0 to 24, with higher scores indicating more depressive symptoms. Cronbach’s α was good in cohort 1 and cohort 2 (Baseline: 0.84, 0.84 Follow-up: 0.84, 0.83) and in previous work (α = 0.80) [21].
Anxiety symptoms
Anxiety was measured at baseline and follow-up with the nine items of the Generalized Anxiety Disorder scale from the Screen for Child Anxiety Related Disorders (SCARED child version [22]). Participants were asked to choose one response that would best describe their feelings in the last 2 weeks. Example items are: “In the last 2 weeks I was nervous”, “In the last 2 weeks, I was worried whether other people would like me”. The response scale runs from “not at all” (0), “a little bit or sometimes” (1) to “definitely or often” (2). High scores on the SCARED indicate more anxiety. Cronbach’s α was good in cohort 1 and cohort 2 (Baseline: 0.88, 0.85 Follow-up: 0.89, 0.86) and comparable to previous research (α = 0.90) [23].
Impact of COVID-19
To measure the impact of COVID-19, we used three items from the CoronaVirus Health Impact Survey Questionnaire [24] tapping into difficulties with cancellations of (important) events, financial problems, and optimism about the future. Items are scored on a five-point Likert scale (1 = not at all, 3 = quite, 5 = very much). Moreover, to assess the atmosphere at home since COVID-19 participants were asked to rate the atmosphere at home from 1 = uncomfortable/not pleasant at all to 4 = a little bit pleasant and 7 = very comfortable/pleasant. As an indication of governmental restrictions related to COVID-19, we calculated the COVID-19 stringency index ([25]; 0–100).
User information of Grow It! app
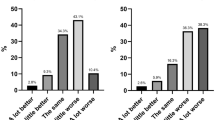
Following the guidelines to measure user experience [26], evaluation of the app was measured at follow-up by asking participants what grade they would give to the Grow It! app, with an answer scale from 1 to 10. Also, participants were asked whether they would recommend the Grow It! app to their friends and what kind of effect the app had on their behavior and feelings. App engagement was operationalized in terms of the percentage of completed daily challenges in the Grow It! app (0–100%) and the compliance of the ESM is the percentage ESM questionnaires that were completed in the Grow It! app (0–100%) [27].
Education level
One item in the baseline questionnaire assessed adolescent education level (primary school, low = (preparatory school for) technical and vocational training, middle = (preparatory school for) professional education, high = (preparatory school for) university).
Statistical analyses
Before testing our hypotheses, we ran tests for cohort -differences (Appendix A1) and attrition (Appendix A2). Because participants between cohort 1 and cohort 2 differed on sex, mean age, cultural identity and COVID-19 stringency index, hypotheses were tested separately for cohort 1 and cohort 2 and sensitivity analyses were added to assess the effects of attrition (Appendix A3). To assess our first hypothesis (1), we conducted paired samples t tests to compare the affective and cognitive well-being from baseline to follow-up. To determine (2) how many adolescents increased in well-being, we followed a method by Grice and colleagues on persons and effect sizes [26]. We considered an individual change of 0.2 SD (small effects size according to Cohen’s D) as a meaningful increase or decrease [32,29,30,31,32]. To understand (3) how background characteristics and (4) user experience and app engagement (challenges and compliance) would be associated with changes in affective and cognitive well-being after playing the Grow It! app, we had preregistered ANOVA and correlations with change rates. Here, we improved our analytical plan and conducted repeated measure models for each predictor (between * within effect). To correct for multiple testing, for each research question separately, the false discovery rate (FDR) was applied [33]. All statistical calculations were performed using IBM SPSS Statistics (version 25).
Results
After playing the Grow It! app, affective well-being statistically increased from baseline to follow-up in both cohort 1 (t(461) = − 6.806, p < 0.001, d = 0.32) and in cohort 2 (t(732) = − 6.77, p < 0.001, d = 0.23). Similarly, cognitive well-being statistically improved from baseline to follow-up in cohort 1 (t(461) = − 6.12, p < 0.001, d = 0.27) and cohort 2 (t (732) = − 5.93, p < 0.001 *, d = 0.20; see Table 3 and Figs. 3, 4). Exploratory sensitivity analyses were carried out in a regression framework to rule out confounders (gender, age, education level, COVID-19 stringency), which yielded similar results (Appendix A3). Together, these results confirm our first hypothesis. In addition, we explored changes in two other indicators of well-being, namely symptoms of depression and anxiety. Depressive symptoms significantly decreased from baseline to follow-up in both cohorts (cohort 1: t(461) = − 2.91, p = 0.004*, d = 0.08, cohort 2: t (732) = − 7.34, p < 0.001, d = 0.17). Moreover, anxiety significantly decreased in cohort 2 (t (732) = − 4.69, p < 0.001, d = 0.14), but not in cohort 1. Notably, the effect sizes for the significant decreases in depressive symptoms and anxiety symptoms are small. Looking at the individual level, 41–53% of the adolescents increased meaningfully in their cognitive and affective well-being (d: ≥ 0.2), respectively, from baseline to follow-up. More specifically, in cohort 1, 45% adolescents increased, 21% decreased (d: ≤ 0.2), and 34% remained stable in their affective well-being. In cohort 2, 42% increased, 23% decreased, 35% remained stable in affective well-being. Furthermore, 53% increased, 26% decreased and 21% remained stable in cognitive well-being in cohort 1. In cohort 2, 45% increased, 30% decreased, and 25% remained stable in cognitive well-being. Each group is described in detail in Appendix A4-A7.
Table 4 shows the results of repeated measures ANOVA to test whether within-person changes in affective or cognitive well-being over time, would be related to between-person differences in demographics, mental health status, coping strategies and impact of COVID-19. Except for an association with education level in cohort 1, none of the demographics (sex, age, cultural identity) were related to changes in well-being. Mental health status was unrelated to changes of well-being. However, stronger increases in well-being were found for adolescents with higher baseline scores of depression (cohort 1–2, see Fig. 5) and among more anxious adolescents (cohort 1). More positive changes in well-being were further associated with a stronger impact of COVID-19 (i.e., more financial problems, lower optimism about the future, lower atmosphere at home (cohort 1), and more difficulties with cancelled events (cohort 2). Finally, changes in well-being were more positive with a lower COVID-19 stringency (i.e., fewer lockdown measures; cohort 1). In contrast to our preregistered hypotheses, neither more positive evaluations nor more engagement (compliance and challenges) were related to the strength of changes over time in affective and cognitive well-being.
Discussion
This preregistered study presents the first evaluation on changes in well-being after playing the Grow It! app [18], a multiplayer mHealth tool which combines ESM with gamified CBT in a large community sample of adolescents carried out during the COVID-19 pandemic. Both cognitive and affective well-being increased significantly during the course of the study—and symptoms of depression and anxiety significantly decreased. Changing COVID-19 related restrictions could not explain this result. Between 41 and 53% of the adolescents improved meaningfully in their cognitive and affective well-being (> 0.2 SD over 3 or 6 weeks of Grow It! app engagement). Overall, improvements in cognitive and affective well-being were stronger among adolescents with higher risk profiles in terms of baseline emotional problems, home context, and COVID-19 impact, and under circumstances with fewer lockdown measures. Grow It! Players’ engagement and satisfaction were unrelated to improvements in well-being. Even though it is not yet possible to draw firm conclusions regarding the effectiveness of the app with this study, our findings provide the first tentative insights that well-being improves and depressive and anxiety symptoms decrease: a proof of concept.
Changes in affective and cognitive well-being after playing the Grow It! app
Grow It! is based on two elements, which have proven successful in reducing mental health problems in face-to-face clinical practice, self-monitoring and insight of emotions and CBT [15,16,17,18,19]. Already after using the Grow It! app for 3 or 6 weeks, the majority of participating adolescents improved in their affective and cognitive well-being (41–53%)—in a period in which the overall well-being of adolescents in the general population decreased [6]. Without a control group, however, it is hard to establish how Grow It! has contributed to this change, and how the effects of COVID-19 and Grow It! upon well-being are intertwined. The study also noticed differences between participants. A group of adolescents did not change meaningfully (21–35%) and a smaller group decreased in their well-being (< 0.2 SD, 21–30%).
Adolescents who reported more depressive symptoms (cohort 1–2) or anxiety symptoms (cohort 1) at baseline increased more strongly in their well-being over the course of our study. This suggests that self-monitoring emotions and being challenged toward adaptive coping, as Grow It! does, is particularly helpful for those at risk. Although mHealth will probably never replace a professional, it could become a helpful add-on tool to already promote self-reflection and activate coping in times of being on a waiting list, or in a blended approach during treatment [31]. Future research will have to determine how Grow It! can help to prevent mental health problems among other high-risk populations, such as chronically ill children or children of parents with mental illness (COPMI) [13].
Even though this study describes a large longitudinal study with pre-registered analyses, the presented findings here should be interpreted in light of several limitations. As the COVID-19 pandemic has drastically disrupted the daily lives of all young people in the Netherlands [3,4,5,6,7,8], we decided not to add a control group to our study but instead make the app available to every young Dutch person aged 12–25 years. Moreover, as the current study started during COVID-19, we had no pre-COVID data from participants. Future research is needed, preferably with a Randomized controlled trial (RCT) design, in which the influence of societal circumstances can be separated from effects of the Grow It! app. This way, alternative explanations of our results cannot definitely be ruled out. Currently, an RCT to better understand the effectiveness of the Grow It! app among adolescents at risk for emotional problems is ongoing. Retention rates (35.41% of n = 1282 in cohort 1, 39% of n = 1871 in cohort 2) were suboptimal, but comparable with other full online youth intervention studies [34] while they were influenced by the fact that participants were not paid and that the study on the Grow It! was carried out during a crisis with no possibility of face-to-face contact to motivate participants. Our nationwide approach to promote Grow It! through (social) media also led to an oversampling of girls, adolescents who have a smartphone, adolescents who are often engaged in online behavior, adolescents with higher education level, as well as adolescents in treatment for mental health problems. This suggests the presence of sampling bias and therefore limits the generalizability of our results to the population. It also informs us that this may be the population that is most interested, motivated for and in need of mHealth support [35]. Whether indeed the Grow It! app may work as a targeted preventive intervention tool especially for adolescents at risk for mental health problems and what the individual underlying working mechanisms are remain important topics of further research.
Lessons learned and consequences for the future
Carrying out a study among adolescents during the COVID-19 pandemic has taught us several important lessons. 1. We were able to reach many adolescents who had an interest in their emotional wellbeing and in strengthening their resilience in times of stress. 2. Since adolescents spend several hours per day online [36], online study recruitment (e.g., through social media, influencers), inclusion (e.g., through video-calls), and datacollection (e.g., with smartphone apps) turned out to be a feasible approach which integrates very well into their daily live. 3. Moreover, not only adolescents were eager to use the Grow It! app – parents, teachers and healthcareprofessionals had a great interest in offering our supportive Mhealth application to the young in this stressful situation. In the past two years COVID-19 has impacted the well-being of almost all adolescents, but youth at high risk for psychological problems (i.e., adolescents with parental psychopathology or with a chronic illness) might specifically benefit from this Mhealth support tool. Future preventive intervention studies will focus on these high risk populations. As a society, one way to take care of each other is to invest in scalable interventions to prevent adolescent mental health problems. Currently there are several Mhealth tools available and advice on how to improve mental health is omnipresent through social media, but very few interventions or advice are grounded in solid scientific research and are developed by independent parties who put the interests of adolescents first. In sum, mental health of adolescents is a crucial societal resource, which can be guarded through investing in scientifically based, user-friendly online support for adolescents.
Conclusion
After 3 or 6 weeks of playing Grow It!, a multiplayer game based on self-monitoring (ESM) and CBT-based challenges, adolescents’ cognitive and affective well-being had significantly increased. Overall, 41–53% of the adolescents had meaningful increase in their affective or cognitive well-being during our study. Positive effects appeared stronger for adolescents with a high-risk profile at baseline (i.e., more depressive symptoms, lower atmosphere at home, higher COVID-19 impact). Even though the findings will need to be replicated in an RCT, these first findings suggest that Grow It! has contributed to adolescent well-being during COVID-19, especially among adolescents with higher risk profiles.
Availability of data and materials
Online codebook available at OSF https://osf.io/2at58/?view_only=b691104ecc3d45ad8b48e1bd60ad7125.
Code availability
Syntax will be made public on https://osf.io/2at58/?view_only=b691104ecc3d45ad8b48e1bd60ad7125.
References
World Health Organization (2004) Promoting mental health: Concepts, emerging evidence, practice: Summary report. World Health Organization
Diener E, Oishi S (eds) (2018) Handbook of well-being. Noba Scholar
Rijksinstituut voor Volksgezondheid en Milieu (2021) Wachttijden Geestelijke Gezondheidszorg. Rijksinstituut voor Volksgezondheid en Milieu (RIVM). https://www.volksgezondheidenzorg.info/onderwerp/wachttijden/geestelijke-gezondheidszorg#node-wachttijden-geestelijke-gezondheidszorg-naar-diagnose
Masten AS, Motti-Stefanidi F (2020) Multisystem resilience for children and youth in disaster: reflections in the context of COVID-19. Advers Resil Sci 1(2):95–106. https://doi.org/10.1007/s42844-020-00010-w
Keijsers L, Bülow A (2021) Growing up in times of COVID-19: When a window of opportunity is temporarily closed. New Common. https://doi.org/10.1007/978-3-030-65355-2
Barendse M, Flannery JE, Cavanagh C, Aristizabal M, Becker SP, Berger E et al (2021) Longitudinal change in adolescent depression and anxiety symptoms from before to during the COVID-19 pandemic: an international collaborative of 12 samples. In: Multilevel governance of global environmental change: perspectives from science, sociology and the law. https://doi.org/10.5281/zenodo.4495772
Fischer K, Tieskens J, Luijten M, Zijlmans J, van Oers H, de Groot R et al (2021) Internalizing problems before and during the COVID-19 pandemic in dutch children and adolescents with and without pre-existing mental health problems. medRxiv. https://doi.org/10.1101/2021.10.05.21264160
Golberstein E, Wen H, Miller BF (2020) Coronavirus disease 2019 (COVID-19) and mental health for children and adolescents. JAMA Pediatr 174(9):819–820. https://doi.org/10.1001/jamapediatrics.2020.1456
Panchal U, Salazar de Pablo G, Franco M, Moreno C, Parellada M, Arango C, Fusar-Poli P (2021) The impact of COVID-19 lockdown on child and adolescent mental health: systematic review. Eur Child Adolesc Psychiatry. https://doi.org/10.1007/s00787-021-01856-w
Orgilés M, Morales A, Delvecchio E, Mazzeschi C, Espada JP (2020) Immediate psychological effects of the COVID-19 quarantine in youth from Italy and Spain. Front Psychol 11:2986
Revet A, Hebebrand J, Anagnostopoulos D, Kehoe LA, Gradl-Dietsch G, Klauser P (2021) Perceived impact of the COVID-19 pandemic on child and adolescent psychiatric services after 1 year (February/March 2021): ESCAP CovCAP survey. Eur Child Adolesc Psychiatry. https://doi.org/10.1007/s00787-021-01851-1
Clarke AM, Kuosmanen T, Barry MM (2015) A systematic review of online youth mental health promotion and prevention interventions. J Youth Adolesc 44(1):90–113. https://doi.org/10.1007/s10964-014-0165-0
Bergin AD, Vallejos EP, Davies EB, Daley D, Ford T, Harold G et al (2020) Preventive digital mental health interventions for children and young people: a review of the design and reporting of research. NPJ Digital Med 3(1):1–9. https://doi.org/10.1038/s41746-020-00339-7
Singh S, Zaki RA, Farid NDN (2019) A systematic review of depression literacy: Knowledge, help-seeking and stigmatising attitudes among adolescents. J Adolesc 74:154–172. https://doi.org/10.1016/j.adolescence.2019.06.004
Punukollu M, Marques M (2019) Use of mobile apps and technologies in child and adolescent mental health: a systematic review. Evid Based Ment Health 22(4):161–166. https://doi.org/10.1136/ebmental-2019-300093
Van Os J, Verhagen S, Marsman A et al (2017) The experience sampling method as an mHealth tool to support self-monitoring, self-insight, and personalized health care in clinical practice. Depress Anxiety 34(6):481–493. https://doi.org/10.1002/da.22647
Havinga PJ, Maciejewski DF, Hartman CA, Hillegers MHJ, Schoevers RA, Penninx BW (2021) Prevention programmes for children of parents with a mood/anxiety disorder: Systematic review of existing programmes and meta-analysis of their efficacy. Br J Clin Psychol. https://doi.org/10.1111/bjc.12277
National Collaborating Centre for Mental Health (2010) The NICE guideline on the treatment and management of depression in adults. The BritishPsychological Society and The Royal College of Psychiatrists. ISBN:978190467185540
BPSW N, en NJi, NVO (2020) Kinderen van Ouders met Psychische Problemen/Verslavingsproblemen (KOPP/KOV). Available: https://richtlijnenjeugdhulp.nl/wp-content/uploads/2020/12/Richtlijn_KOPP-KOV_Richtlijn_V4_2020-2022_DEF.pdf
Beyens I, Pouwels JL, van Driel II, Keijsers L, Valkenburg PM (2020) The effect of social media on well-being differs from adolescent to adolescent. Sci Rep 10(1):1–11. https://doi.org/10.1038/s41598-020-67727-7
Cheung F, Lucas RE (2014) Assessing the validity of single-item life satisfaction measures: results from three large samples. Qual Life Res 23(10):2809–2818. https://doi.org/10.1007/s11136-014-0726-4
Allgaier AK, Frühe B, Pietsch K, Saravo B, Baethmann M, Schulte-Körne G (2012) Is the Children’s Depression Inventory Short version a valid screening tool in pediatric care? A comparison to its full-length version. J Psychosom Res 73(5):369–374. https://doi.org/10.1016/j.jpsychores.2012.08.016
Birmaher B, Khetarpal S, Brent D, Cully M, Balach L, Kaufman J et al (1997) The screen for child anxiety related emotional disorders (scared): Scale construction and psychometric characteristics. J Am Acad Child Adolesc Psychiatry 36:545–555
Garnefski N, Kraaij V (2006) Cognitive emotion regulation questionnaire–development of a short 18-item version (CERQ-short). Personality Individ Differ 41(6):1045–1053. https://doi.org/10.1016/j.paid.2006.04.010
Merikangas K, Milham M, Stringaris A. The coronavirus health impact survey (crisis) V0.3, 2020. Available: https://github.com/nimh-mbdu/CRISIS
Hannah Ritchie EO-O, Beltekian D, Mathieu E, Hasell J, Macdonald B, Giattino C, Appel C, Rodés-Guirao L, Roser M (2020) Coronavirus pandemic (covid-19). Our World in Data. Available: https://ourworldindata.org/coronavirus
M. Schrepp, User Experience Questionnaire Handbook. All You Need to Know to Apply the UEQ Successfully in Your Project. Berlin, Germany: ResearchGate GmbH, 2015, https://doi.org/10.13140/RG.2.1.2815.0245
van Roekel E, Keijsers L, Chung JM (2019) A review of current ambulatory assessment studies in adolescent samples and practical recommendations. J Res Adolesc 29(3):560–577. https://doi.org/10.1111/jora.12471
Grice JW, Medellin E, Jones I, Horvath S, McDaniel H, O’lansen C, Baker M (2020) Persons as effect sizes. Advances in methods and practices in psychological. Science 3(4):443–455. https://doi.org/10.1177/2515245920922982
Engel L, Beaton DE, Touma Z (2018) Minimal clinically important difference: a review of outcome measure score interpretation. Rheum Dis Clin 44(2):177–188. https://doi.org/10.1016/j.rdc.2018.02.002
Sawilowsky SS (2009) New effect size rules of thumb. J Mod Appl Stat Methods 8(2):26. https://doi.org/10.22237/jmasm/1257035100
Ferguson RJ, Robinson AB, Splaine M (2002) Use of the reliable change index to evaluate clinical significance in SF-36 outcomes. Qual Life Res 11(6):509–516
Benjamini Y, Yekutieli D (2001) The control of the false discovery rate in multiple testing under dependency. Ann Statist. https://doi.org/10.1214/aos/1013699998
Wentzel J, van der Vaart R, Bohlmeijer ET, van Gemert-Pijnen JE (2016) Mixing online and face-to-face therapy: how to benefit from blended care in mental health care. JMIR Mental Health. https://doi.org/10.2196/mental.4534
Goldberg SB, Lam SU, Simonsson O, Torous J, Sun S (2022) Mobile phone-based interventions for mental health: a systematic meta-review of 14 meta-analyses of randomized controlled trials. PLOS Digital Health 1(1):e0000002
van Driel II, Pouwels JL, Beyens I., Keijsers, L, Valkenburg PM (2019) Posting, scrolling, chatting and snapping: Youth (14-15) and social media in 2019. Universiteit van Amsterdam, Center for Research on Children, Adolescents, and the Media (CcaM)
Funding
Municipality Rotterdam—award number SUB.20.03.00149.SBSA. Stichting Vriendenv an het Sophia WAR21-70/WO. ZonMw.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethics approval
The METC [MEC-2020-0287] of the Erasmus MC approved this study.
Informed consent
All participants signed informed consent.
Consent for publication
Agreed.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Dietvorst, E., Legerstee, J.S., Vreeker, A. et al. The Grow It! app—longitudinal changes in adolescent well-being during the COVID-19 pandemic: a proof-of-concept study. Eur Child Adolesc Psychiatry 32, 1097–1107 (2023). https://doi.org/10.1007/s00787-022-01982-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-022-01982-z