Abstract
Objectives
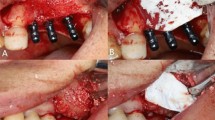
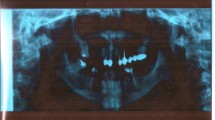
To investigate the effectiveness of hydraulic pressure-assisted sinus augmentation (SA) in a rabbit sinus model in terms of radiographical and histological healing.
Materials and methods
Bilateral SA was performed in 12 rabbits. Each sinus was randomly assigned to either a hydraulic pressure-assisted SA (test) or a conventional SA (control) group. Healing periods of 2 and 4 weeks were applied (n = 6 for each week). Healing pattern including newly formed bone (NB) and residual bone substitute material (RM) was analyzed with microcomputed tomographically, histologically, and histomorphometrically.
Results
No sinus membrane perforation was detected in either group. In the microcomputed tomographic analysis, the test group exhibited higher apico-coronal spread of RM compared to the control group (p < 0.05). Particularly, the test group exhibited several masses of NB out of the cluster of RM. Histologically, the test group showed an elongated shape of the augmented space, whereas the control group generally presented a dome shape. Histomorphometrically, the total augmented area and the area of NB (1.32 ± 0.56 vs. 0.84 ± 0.40 mm2 at 2 weeks, 2.24 ± 1.09 vs. 2.22 ± 0.85 mm2 at 4 weeks) were not significantly different between the test and the control groups at both healing periods (p > 0.05).
Conclusion
Hydraulic pressure-assisted SA led to new bone formation in the distant areas from the bony access hole, but similar histological healing pattern to conventional SA.
Clinical relevance
Hydraulic pressure-assisted SA is a promising option for treating pneumatized posterior maxilla.






Similar content being viewed by others
References
Boyne PJ, James RA (1980) Grafting of the maxillary sinus floor with autogenous marrow and bone. J Oral Surg 38:613–616
Tatum H (1986) Maxillary and sinus implant reconstructions. Dent Clin North Am 30:207–229
Jensen J (1990) Reconstruction of the severely resorbed maxilla with bone grafting and osseointegrated implants: a preliminary report. J Oral Maxillofac Surg 48:27–32
Lundgren S, Cricchio G, Hallman M, Jungner M (2000) Rasmusson L and Sennerby L (2017) Sinus floor elevation procedures to enable implant placement and integration: techniques, biological aspects and clinical outcomes. Periodontol 73:103–120. https://doi.org/10.1111/prd.12165
Pjetursson BE, Lang NP (2000) (2014) Sinus floor elevation utilizing the transalveolar approach. Periodontol 66:59–71. https://doi.org/10.1111/prd.12043
Pjetursson BE, Tan WC, Zwahlen M, Lang NP (2008) A systematic review of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation. J Clin Periodontol 35:216–240. https://doi.org/10.1111/j.1600-051X.2008.01272.x
Tan WC, Lang NP, Zwahlen M, Pjetursson BE (2008) A systematic review of the success of sinus floor elevation and survival of implants inserted in combination with sinus floor elevation. Part II: transalveolar technique. J Clin Periodontol 35:241–254. https://doi.org/10.1111/j.1600-051X.2008.01273.x
Pjetursson BE, Rast C, Bragger U, Schmidlin K, Zwahlen M, Lang NP (2009) Maxillary sinus floor elevation using the (transalveolar) osteotome technique with or without grafting material. Part I: Implant survival and patients’ perception. Clin Oral Implants Res 20:667–676. https://doi.org/10.1111/j.1600-0501.2009.01704.x
Ferrigno N, Laureti M, Fanali S (2006) Dental implants placement in conjunction with osteotome sinus floor elevation: a 12-year life-table analysis from a prospective study on 588 ITI implants. Clin Oral Implants Res 17:194–205. https://doi.org/10.1111/j.1600-0501.2005.01192.x
Rosen PS, Summers R, Mellado JR, Salkin LM, Shanaman RH, Marks MH, Fugazzotto PA (1999) The bone-added osteotome sinus floor elevation technique: multicenter retrospective report of consecutively treated patients. Int J Oral Maxillofac Implants 14:853–858
Farina R, Franceschetti G, Travaglini D, Consolo U, Minenna L, Schincaglia GP, Riccardi O, Bandieri A, Maietti E, Trombelli L (2018) Morbidity following transcrestal and lateral sinus floor elevation: a randomized trial. J Clin Periodontol 45:1128–1139. https://doi.org/10.1111/jcpe.12985
Gatti F, Gatti C, Tallarico M, Tommasato G, Meloni SM, Chiapasco M (2018) Maxillary sinus membrane elevation using a special drilling system and hydraulic pressure: a 2-year prospective cohort study. Int J Periodontics Restorative Dent 38:593–599. https://doi.org/10.11607/prd.3403
Boffano P, Forouzanfar T (2014) Current concepts on complications associated with sinus augmentation procedures. J Craniofac Surg 25:e210–e212. https://doi.org/10.1097/scs.0000000000000438
Al Almaie S, Kavarodi A, Al Faidhi A (2013) Maxillary sinus functions and complications with lateral window and osteotome sinus floor elevation procedures followed by dental implants placement: a retrospective study in 60 patients. J Contemp Dent Pract 14:405–413
Katranji A, Fotek P, Wang HL (2008) Sinus augmentation complications: etiology and treatment. Implant Dent 17:339–349. https://doi.org/10.1097/ID.0b013e3181815660
Bensaha T, El Mjabber H (2016) Evaluation of new bone formation after sinus augmentation with two different methods. Int J Oral Maxillofac Surg 45:93–98. https://doi.org/10.1016/j.ijom.2015.09.003
Better H, Slavescu D, Barbu H, Cochran DL, Chaushu G (2014) Minimally invasive sinus lift implant device: a multicenter safety and efficacy trial preliminary results. Clin Implant Dent Relat Res 16:520–526. https://doi.org/10.1111/cid.12021
Chaushu L, Chaushu G, Better H, Naishlos S, Kolerman R, Aragoneses JM, Calvo-Guirado JL, Nissan J (2020) Sinus augmentation with simultaneous, non-submerged, implant placement using a minimally invasive hydraulic technique. Medicina (Kaunas) 56:75. https://doi.org/10.3390/medicina56020075
Cho YS, Chong D, Yang SM, Kang B (2017) Hydraulic transcrestal sinus lift: different patterns of elevation in pig sinuses. Implant Dent 26:706–710. https://doi.org/10.1097/ID.0000000000000608
Cho YS, Hwang KG, Jun SH, Tallarico M, Kwon AM, Park CJ (2020) Radiologic comparative analysis between saline and platelet-rich fibrin filling after hydraulic transcrestal sinus lifting without adjunctive bone graft: a randomized controlled trial. Clin Oral Implants Res 31:1087–1093. https://doi.org/10.1111/clr.13655
Kim DY, Itoh Y, Kang TH (2012) Evaluation of the effectiveness of a water lift system in the sinus membrane-lifting operation as a sinus surgical instrument. Clin Implant Dent Relat Res 14:585–594. https://doi.org/10.1111/j.1708-8208.2010.00292.x
Kim JM, Sohn DS, Heo JU, Park JS, Jung HS, Moon JW, Lee JH, Park IS (2012) Minimally invasive sinus augmentation using ultrasonic piezoelectric vibration and hydraulic pressure: a multicenter retrospective study. Implant Dent 21:536–542. https://doi.org/10.1097/ID.0b013e3182746c3d
Lopez MA, Andreasi Bassi M, Confalone L, Carinci F (2014) Maxillary sinus floor elevation via crestal approach: the evolution of the hydraulic pressure technique. J Craniofac Surg 25:e127–e132. https://doi.org/10.1097/SCS.0000000000000457
Tallarico M, Meloni SM, Xhanari E, Pisano M, Cochran DL (2017) Minimally invasive sinus augmentation procedure using a dedicated hydraulic sinus lift implant device: a prospective case series study on clinical, radiologic, and patient-centered outcomes. Int J Periodontics Restorative Dent 37:125–135. https://doi.org/10.11607/prd.2914
Troedhan AC, Kurrek A, Wainwright M, Jank S (2010) Hydrodynamic ultrasonic sinus floor elevation—an experimental study in sheep. J Oral Maxillofac Surg 68:1125–1130. https://doi.org/10.1016/j.joms.2009.12.014
Bensaha T (2012) Outcomes of flapless crestal maxillary sinus elevation under hydraulic pressure. Int J Oral Maxillofac Implants 27:1223–1229
Lim HC, Zhang ML, Lee JS, Jung UW, Choi SH (2015) Effect of different hydroxyapatite:beta-tricalcium phosphate ratios on the osteoconductivity of biphasic calcium phosphate in the rabbit sinus model. Int J Oral Maxillofac Implants 30:65–72. https://doi.org/10.11607/jomi.3709
Kim S, Chung JH, Shin SY, Shin SI, Hong JY, Lim HC (2020) Collagenated synthetic bone substitute material for sinus floor elevation at sites with a perforated Schneiderian membrane. J Clin Med 9:3764. https://doi.org/10.3390/jcm9113764
Lim HC, Son Y, Hong JY, Shin SI, Jung UW, Chung JH (2018) Sinus floor elevation in sites with a perforated Schneiderian membrane: What is the effect of placing a collagen membrane in a rabbit model? Clin Oral Implants Res 29:1202–1211. https://doi.org/10.1111/clr.13385
Paik JW, Cha JK, Paeng KW, Kim MJ, Thoma DS, Jung RE, Jung UW (2020) Volume stability of the augmented sinus using a collagenated bovine bone mineral grafted in case of a perforated Schneiderian membrane: An experimental study in rabbits. J Clin Periodontol 47:649–656. https://doi.org/10.1111/jcpe.13273
Gruber R, Kandler B, Fuerst G, Fischer MB, Watzek G (2004) Porcine sinus mucosa holds cells that respond to bone morphogenetic protein (BMP)-6 and BMP-7 with increased osteogenic differentiation in vitro. Clin Oral Implants Res 15:575–580. https://doi.org/10.1111/j.1600-0501.2004.01062.x
Guo J, Weng J, Rong Q, Zhang X, Zhu S, Huang D, Li X, Chen S (2015) Investigation of multipotent postnatal stem cells from human maxillary sinus membrane. Sci Rep 5:11660. https://doi.org/10.1038/srep11660
Scala A, Botticelli D, Rangel IG Jr, de Oliveira JA, Okamoto R, Lang NP (2010) Early healing after elevation of the maxillary sinus floor applying a lateral access: a histological study in monkeys. Clin Oral Implants Res 21:1320–1326. https://doi.org/10.1111/j.1600-0501.2010.01964.x
Scala A, Lang NP, Velez JU, Favero R, Bengazi F, Botticelli D (2016) Effects of a collagen membrane positioned between augmentation material and the sinus mucosa in the elevation of the maxillary sinus floor. An experimental study in sheep. Clin Oral Implants Res 27:1454–1461. https://doi.org/10.1111/clr.12762
Acknowledgements
The authors appreciate the research team at the Department of Periodontology, Kyung Hee University. Bone substitute material (Maxpore) was kindly supported by Shinhung.
Author information
Authors and Affiliations
Contributions
Conceptualization: YH, HCL; Methodology: SYS, JHC, HCL; Formal analysis and investigation: JYL, SK; Writing—original draft preparation: JYL; Writing—review and editing: YH, HCL; Resources: SYS; Supervision: JHC.
Corresponding authors
Ethics declarations
Ethics approval
This article does not contain any studies with human participants performed by any of the authors. All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Consent to participate
The present study does not require informed consent.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, JY., Kim, S., Shin, SY. et al. Effectiveness of hydraulic pressure-assisted sinus augmentation in a rabbit sinus model: a preclinical study. Clin Oral Invest 26, 1581–1591 (2022). https://doi.org/10.1007/s00784-021-04131-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04131-z