Abstract
Objective
This systematic review evaluated the impacts of non-surgical periodontal therapy (NSPT) in patients with chronic kidney disease (CKD) and periodontitis in order to explore causality and assess the potential benefits of co-management.
Methods
This systematic review and meta-analyses were conducted by searching MEDLINE, EMBASE, PubMed, Cochrane Library, and Open GREY. Interventional studies of adult patients suffering from CKD and periodontitis were investigated. Effect of NSPT on renal function was analyzed.
Results
A total of 109 participants from four case-series studies and 97 participants from one randomized controlled trial were included in this review. Sixty percent of the eligible studies (3/5) aimed at the effect of NSPT on nutritional status and systemic inflammation in dialysis patients. The other two studies concluded a beneficial impact of NSPT on estimated glomerular filtration rate (eGFR) in patients with CKD stages 2–4. Moreover, two meta-analyses were accomplished on eGFR and serum creatinine to evaluate the changes between baseline and 3-month follow-up. The pooled mean of eGFR was not significantly different pre- and post-NSPT using random and fixed-effect models. The change for creatinine was not significant using the random effect model but was significant when the fixed effect model was used (p < 0.001).
Conclusions
There is insufficient evidence to conclude the potential benefit of NSPT on renal function in CKD patients with periodontitis.
Clinical relevance
Periodontitis contributes to the inflammatory burden and has been associated with impaired kidney function in many observational studies. However, well-designed clinical trials in pre-dialysis patients investigating the impact of NSPT on renal function–related parameters are missing.



Similar content being viewed by others
References
Vos T et al (2016) Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388(10053):1545–1602. https://doi.org/10.1016/S0140-6736(16)31678-6
Jha V, Garcia-Garcia G, Iseki K, Li Z, Naicker S, Plattner B, Saran R, Wang AY, Yang CW (2013) Chronic kidney disease: global dimension and perspectives. Lancet 382(9888):260–272. https://doi.org/10.1016/S0140-6736(13)60687-X
Webster AC, Nagler EV, Morton RL, Masson P (2017) Chronic kidney disease. Lancet 389(10075):1238–1252. https://doi.org/10.1016/S0140-6736(16)32064-5
Honeycutt AA, Segel JE, Zhuo X, Hoerger TJ, Imai K, Williams D (2013) Medical costs of CKD in the Medicare population. J Am Soc Nephrol 24(9):1478–1483. https://doi.org/10.1681/ASN.2012040392
Kahn LS, Vest BM, Madurai N, Singh R, York TR, Cipparone CW, Reilly S, Malik KS, Fox CH (2015) Chronic kidney disease (CKD) treatment burden among low-income primary care patients. Chronic Illn 11(3):171–183. https://doi.org/10.1177/1742395314559751
Levin A, Foley RN (2000) Cardiovascular disease in chronic renal insufficiency. Am J Kidney Dis 36(6 Suppl 3):S24–S30
Ene-Iordache B, Perico N, Bikbov B, Carminati S, Remuzzi A, Perna A, Islam N, Bravo RF, Aleckovic-Halilovic M, Zou H, Zhang L, Gouda Z, Tchokhonelidze I, Abraham G, Mahdavi-Mazdeh M, Gallieni M, Codreanu I, Togtokh A, Sharma SK, Koirala P, Uprety S, Ulasi I, Remuzzi G (2016) Chronic kidney disease and cardiovascular risk in six regions of the world (ISN-KDDC): a cross-sectional study. Lancet Glob Health 4(5):e307–e319. https://doi.org/10.1016/S2214-109X(16)00071-1
Kassebaum NJ, Bernabe E, Dahiya M, Bhandari B, Murray CJ, Marcenes W (2014) Global burden of severe periodontitis in 1990-2010: a systematic review and meta-regression. J Dent Res 93(11):1045–1053. https://doi.org/10.1177/0022034514552491
Page RC, Offenbacher S, Schroeder HE, Seymour GJ, Kornman KS (1997) Advances in the pathogenesis of periodontitis: summary of developments, clinical implications and future directions. Periodontol 2000 14:216–248
Hajishengallis G, Lambris JD (2012) Complement and dysbiosis in periodontal disease. Immunobiology 217(11):1111–1116. https://doi.org/10.1016/j.imbio.2012.07.007
Cobb CM (1996) Non-surgical pocket therapy: mechanical. Ann Periodontol 1(1):443–490. https://doi.org/10.1902/annals.1996.1.1.443
Darveau RP, Tanner A, Page RC (1997) The microbial challenge in periodontitis. Periodontol 14:12–32
Cobb CM (2002) Clinical significance of non-surgical periodontal therapy: an evidence-based perspective of scaling and root planing. J Clin Periodontol 29(Suppl 2):6–16
Zhao D, Khawaja AT, Jin L, Li KY, Tonetti M, Pelekos G (2018) The directional and non-directional associations of periodontitis with chronic kidney disease: a systematic review and meta-analysis of observational studies. J Periodontal Res 53:682–704. https://doi.org/10.1111/jre.12565
Kshirsagar AV, Offenbacher S, Moss KL, Barros SP, Beck JD (2007) Antibodies to periodontal organisms are associated with decreased kidney function. The Dental Atherosclerosis Risk in Communities study. Blood Purif 25(1):125–132. https://doi.org/10.1159/000096411
Fisher MA, Taylor GW, Papapanou PN, Rahman M, Debanne SM (2008) Clinical and serologic markers of periodontal infection and chronic kidney disease. J Periodontol 79(9):1670–1678. https://doi.org/10.1902/jop.2008.070569
Salimi S, Ng N, Seliger SL, Parsa A (2014) Periodontal disease, renal dysfunction and heightened leukocytosis. Nephron Clin Pract 128(1–2):107–114. https://doi.org/10.1159/000366445
Borrell LN, Papapanou PN (2005) Analytical epidemiology of periodontitis. J Clin Periodontol 32(Suppl 6):132–158. https://doi.org/10.1111/j.1600-051X.2005.00799.x
Elihimas Junior UF, Elihimas HC, Lemos VM, Leao Mde A, Sa MP, Franca EE, Lemos A, Valente LM, Markman Filho B (2014) Smoking as risk factor for chronic kidney disease: systematic review. J Bras Nefrol 36(4):519–528. https://doi.org/10.5935/0101-2800.20140074
Ritz E, Rychlik I, Locatelli F, Halimi S (1999) End-stage renal failure in type 2 diabetes: a medical catastrophe of worldwide dimensions. Am J Kidney Dis 34(5):795–808. https://doi.org/10.1016/S0272-6386(99)70035-1
Kshirsagar AV, Craig RG, Moss KL, Beck JD, Offenbacher S, Kotanko P, Klemmer PJ, Yoshino M, Levin NW, Yip JK, Almas K, Lupovici EM, Usvyat LA, Falk RJ (2009) Periodontal disease adversely affects the survival of patients with end-stage renal disease. Kidney Int 75(7):746–751. https://doi.org/10.1038/ki.2008.660
de Souza CM, Braosi AP, Luczyszyn SM, Olandoski M, Kotanko P, Craig RG, Trevilatto PC, Pecoits-Filho R (2014) Association among oral health parameters, periodontitis, and its treatment and mortality in patients undergoing hemodialysis. J Periodontol 85(6):e169–e178. https://doi.org/10.1902/jop.2013.130427
Tonetti MS, D’Aiuto F, Nibali L, Donald A, Storry C, Parkar M, Suvan J, Hingorani AD, Vallance P, Deanfield J (2007) Treatment of periodontitis and endothelial function. N Engl J Med 356(9):911–920. https://doi.org/10.1056/NEJMoa063186
Chambrone L, Foz AM, Guglielmetti MR, Pannuti CM, Artese HP, Feres M, Romito GA (2013) Periodontitis and chronic kidney disease: a systematic review of the association of diseases and the effect of periodontal treatment on estimated glomerular filtration rate. J Clin Periodontol 40(5):443–456. https://doi.org/10.1111/jcpe.12067
Deschamps-Lenhardt S, Martin-Cabezas R, Hannedouche T, Huck O (2019) Association between periodontitis and chronic kidney disease: systematic review and meta-analysis. Oral Dis 25(2):385–402. https://doi.org/10.1111/odi.12834
Lee CF, Lin CL, Lin MC, Lin SY, Sung FC, Kao CH (2014) Surgical treatment for patients with periodontal disease reduces risk of end-stage renal disease: a nationwide population-based retrospective cohort study. J Periodontol 85(1):50–56. https://doi.org/10.1902/jop.2013.130015
Graziani F, Cei S, La Ferla F, Vano M, Gabriele M, Tonetti M (2010) Effects of non-surgical periodontal therapy on the glomerular filtration rate of the kidney: an exploratory trial. J Clin Periodontol 37(7):638–643. https://doi.org/10.1111/j.1600-051X.2010.01578.x
Vilela EM, Bastos JA, Fernandes N, Ferreira AP, Chaoubah A, Bastos MG (2011) Treatment of chronic periodontitis decreases serum prohepcidin levels in patients with chronic kidney disease. Clinics (Sao Paulo) 66(4):657–662
Guo N, Lin G (2017) Effects of nonsurgical periodontal therapy on serum inflammatory factor levels in patients with chronic kidney disease and periodontitis. Biomedical Research (India) 28(9):3899–3902
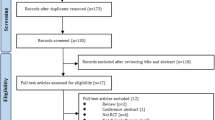
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341. https://doi.org/10.1016/j.ijsu.2010.02.007
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, Cochrane Bias Methods G, Cochrane Statistical Methods G (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928. https://doi.org/10.1136/bmj.d5928
Higgins JPT, Altman DG, Sterne JAC (editors). Chapter 8: assessing risk of bias in included studies. In: Higgins JPT, Green S (editors). Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated march 2011). The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org
Sterne JA, Hernan MA, Reeves BC, Savovic J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan AW, Churchill R, Deeks JJ, Hrobjartsson A, Kirkham J, Juni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schunemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Kokotovic D, Burcharth J, Helgstrand F, Gogenur I (2017) Systemic inflammatory response after hernia repair: a systematic review. Langenbeck's Arch Surg 402:1023–1037. https://doi.org/10.1007/s00423-017-1618-1
The Grading of Recommendations, Assessment, Development and Evaluation (GRADE) Working Group (2013) Handbook for grading the quality of evidence and the strength of recommendations using the GRADE approach. Available at: http://gdt.guidelinedevelopment.org/app/handbook/handbook.html Updated October 2013
Ryan R, Hill S (2016) How to GRADE the quality of the evidence. Cochrane Consumers and Communication Group, available at http://cccrg.cochrane.org/author-resources. Version 3.0 December 2016
Luo D, Wan X, Liu J, Tong T (2016) Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat Methods Med Res 27:1785–1805. https://doi.org/10.1177/0962280216669183
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135. https://doi.org/10.1186/1471-2288-14-135
Fu R, Vandermeer BW, Shamliyan TA, O'Neil ME, Yazdi F, Fox SH, Morton SC (2013) Handling Continuous Outcomes in Quantitative Synthesis. Methods Guide for Comparative Effectiveness Reviews. (Prepared by the Oregon Evidence-based Practice Center under Contract No. 290-2007-10057-I) AHRQ Publication No. 13-EHC103-EF. Rockville, MD: Agency for Healthcare Research and Quality. www.effectivehealthcare.ahrq.gov/reports/final.cfm
Higgins JPT, Deeks JJ (editors) (2011) Chapter 7: selecting studies and collecting data. In: Higgins JPT, Green S (editors), Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated march 2011). The Cochrane Collaboration, . Available from www.handbook.cochrane.org
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Borenstein M, Hedges LV, Higgins JP, Rothstein HR (2010) A basic introduction to fixed-effect and random-effects models for meta-analysis. Res Synth Methods 1(2):97–111. https://doi.org/10.1002/jrsm.12
Deeks JJ, Higgins JPT, Altman DG (editors) (2011) Chapter 9: Analysing data and undertaking meta-analyses. In: Higgins JPT, Green S (editors). Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated march 2011). The Cochrane Collaboration, 2011. Available from www.handbook.cochrane.org
Fang F, Wu B, Qu Q, Gao J, Yan W, Huang X, Ma D, Yue J, Chen T, Liu F, Liu Y (2015) The clinical response and systemic effects of non-surgical periodontal therapy in end-stage renal disease patients: a 6-month randomized controlled clinical trial. J Clin Periodontol 42(6):537–546. https://doi.org/10.1111/jcpe.12411
Almeida S, Figueredo CM, Lemos C, Bregman R, Fischer RG (2017) Periodontal treatment in patients with chronic kidney disease: a pilot study. J Periodontal Res 52(2):262–267
Siribamrungwong M, Yothasamutr K, Puangpanngam K (2014) Periodontal treatment reduces chronic systemic inflammation in peritoneal dialysis patients. Ther Apher Dial 18(3):305–308
Siribamrungwong M, Puangpanngam K (2012) Treatment of periodontal diseases reduces chronic systemic inflammation in maintenance hemodialysis patients. Ren Fail 34(2):171–175
Artese HP, Sousa CO, Luiz RR, Sansone C, Torres MC (2010) Effect of non-surgical periodontal treatment on chronic kidney disease patients. Braz Oral Res 24(4):449–454
Borah MF, Schoenfeld PY, Gotch FA, Sargent JA, Wolfsen M, Humphreys MH (1978) Nitrogen balance during intermittent dialysis therapy of uremia. Kidney Int 14(5):491–500
Ikizler TA, Pupim LB, Brouillette JR, Levenhagen DK, Farmer K, Hakim RM, Flakoll PJ (2002) Hemodialysis stimulates muscle and whole body protein loss and alters substrate oxidation. Am J Physiol Endocrinol Metab 282(1):E107–E116. https://doi.org/10.1152/ajpendo.2002.282.1.E107
Ghebremichael-Weldeselassie Y, Whitaker HJ, Farrington CP (2014) Self-controlled case series method with smooth age effect. Stat Med 33(4):639–649. https://doi.org/10.1002/sim.5949
Petersen I, Douglas I, Whitaker H (2016) Self controlled case series methods: an alternative to standard epidemiological study designs. BMJ 354:i4515. https://doi.org/10.1136/bmj.i4515
Chen LP, Chiang CK, Chan CP, Hung KY, Huang CS (2006) Does periodontitis reflect inflammation and malnutrition status in hemodialysis patients? Am J Kidney Dis 47(5):815–822. https://doi.org/10.1053/j.ajkd.2006.01.018
Inker LA, Astor BC, Fox CH, Isakova T, Lash JP, Peralta CA, Kurella Tamura M, Feldman HI (2014) KDOQI US commentary on the 2012 KDIGO clinical practice guideline for the evaluation and management of CKD. Am J Kidney Dis 63(5):713–735. https://doi.org/10.1053/j.ajkd.2014.01.416
Kocyigit I, Yucel HE, Cakmak O, Dogruel F, Durukan DB, Korkar H, Unal A, Sipahioglu MH, Oymak O, Gurgan CA, Tokgoz B (2014) An ignored cause of inflammation in patients undergoing continuous ambulatory peritoneal dialysis: periodontal problems. Int Urol Nephrol 46(10):2021–2028
Grubbs V, Garcia F, Jue BL, Vittinghoff E, Ryder M, Lovett D, Carrillo J, Offenbacher S, Ganz P, Bibbins-Domingo K, Powe NR (2017) The Kidney and Periodontal Disease (KAPD) study: a pilot randomized controlled trial testing the effect of non-surgical periodontal therapy on chronic kidney disease. Contemp Clin Trials 53:143–150. https://doi.org/10.1016/j.cct.2016.12.017
Sharma P, Cockwell P, Dietrich T, Ferro C, Ives N, Chapple ILC (2017) INfluence of successful periodontal intervention in REnal disease (INSPIRED): study protocol for a randomised controlled pilot clinical trial. Trials 18(1):535. https://doi.org/10.1186/s13063-017-2236-5
Jamieson L, Skilton M, Maple-Brown L, Kapellas K, Askie L, Hughes J, Arrow P, Cherian S, Fernandes D, Pawar B, Brown A, Boffa J, Hoy W, Harris D, Mueller N, Cass A (2015) Periodontal disease and chronic kidney disease among aboriginal adults; an RCT. BMC Nephrol 16:181. https://doi.org/10.1186/s12882-015-0169-3
Teeuw WJ, Slot DE, Susanto H, Gerdes VE, Abbas F, D'Aiuto F, Kastelein JJ, Loos BG (2014) Treatment of periodontitis improves the atherosclerotic profile: a systematic review and meta-analysis. J Clin Periodontol 41(1):70–79. https://doi.org/10.1111/jcpe.12171
Funding
This review was supported by The University of Hong Kong, Hong Kong SAR, China.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhao, D., Khawaja, A.T., Jin, L. et al. Effect of non-surgical periodontal therapy on renal function in chronic kidney disease patients with periodontitis: a systematic review and meta-analysis of interventional studies. Clin Oral Invest 24, 1607–1618 (2020). https://doi.org/10.1007/s00784-019-03066-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-03066-w