Abstract
Objective
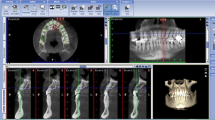
The purpose of this study is to evaluate the relationship between anatomic structures and mandibular posterior region using cone-beam computed tomography (CBCT) in terms of endodontic surgery.
Methods
A total of 150 CBCT images were used to investigate the proximity of the anatomical structures and the mandibular posterior teeth. The buccal and lingual bone thickness overlying each root, buccolingual, and mesiodistal dimension of the roots were measured at the level of 3 mm apical resection, and the mental foramen (MF) distance to the premolar teeth and the distance of the mandibular canal (MC) to all the posterior teeth were measured.
Results
The thinnest part of the buccal cortical bone was measured in the first premolar teeth (1.70 mm) and in the mesial root of the first molar (2.25 mm) while the thickest region was measured in the distal root of the second molar tooth (6.95 mm). The maximum amount of substance to be removed was measured at the distal root of the second molar tooth (11.26 mm), and at least the first premolar tooth (5.52 mm) was measured for buccal resection. The distal root of the second molar tooth was found to be the closest tooth root to the MC with a mean of 2.75 mm, and the closest distance was measured as 0 mm.
Conclusions
It is important to evaluate the parameters such as mandibular buccal and lingual bone thickness, location of the MC and the MF, and root size for atraumatic endodontic surgical approach. Evaluation of these data before endodontic surgery provides guidance to the clinician in the planning of endodontic surgery.
Clinical relevance
The mandibular posterior region, which is difficult to reach with traditional surgical approach, is now easily reached using an operation microscope. For this reason, endodontic surgical procedures have become popular in mandibular posterior teeth. Therefore, the relationship between the mandibular posterior teeth and anatomical structures that are important in the planning of surgical access line is examined in this study.




Similar content being viewed by others
References
Lui JN, Khin MM, Krishnaswamy G, Chen NN (2014) Prognostic factors relating to the outcome of endodontic microsurgery. J Endod 40:1071–1076. https://doi.org/10.1016/j.joen.2014.04.005
Lavasani SA, Tyler C, Roach SH, McClanahan SB, Ahmad M, Bowles WR (2016) Cone-beam computed tomography: anatomic analysis of maxillary posterior teeth-impact on endodontic microsurgery. J Endod 42:890–895. https://doi.org/10.1016/j.joen.2016.03.002
Ahn SY, Kim NH, Kim S, Karabucak B, Kim E (2018) Computer-aided design/computer-aided manufacturing-guided endodontic surgery: guided osteotomy and apex localization in a mandibular molar with a thick buccal bone plate. J Endod 44:665–670. https://doi.org/10.1016/j.joen.2017.12.009
Friedman S (2011) Outcome of endodontic surgery: a meta-analysis of the literature-part 1: comparison of traditional root-end surgery and endodontic microsurgery. J Endod 37:577–578; author reply 578-80. https://doi.org/10.1016/j.joen.2011.01.020
Marti E, Penarrocha M, Garcia B, Martinez JM, Gay-Escoda C (2008) Distance between periapical lesion and mandibular canal as a factor in periapical surgery in mandibular molars. J Oral Maxillofac Surg 66:2461–2466. https://doi.org/10.1016/j.joms.2008.06.033
Wang X, Chen K, Wang S, Tiwari SK, Ye L, Peng L (2017) Relationship between the mental foramen, mandibular canal, and the surgical access line of the mandibular posterior teeth: a cone-beam computed tomographic analysis. J Endod 43:1262–1266. https://doi.org/10.1016/j.joen.2017.03.043
Chong BS, Gohil K, Pawar R, Makdissi J (2017) Anatomical relationship between mental foramen, mandibular teeth and risk of nerve injury with endodontic treatment. Clin Oral Investig 21:381–387. https://doi.org/10.1007/s00784-016-1801-8
Zahedi S, Mostafavi M, Lotfirikan N (2018) Anatomic study of mandibular posterior teeth using cone-beam computed tomography for endodontic surgery. J Endod 44:738–743. https://doi.org/10.1016/j.joen.2018.01.016
Guerrero ME, Botetano R, Beltran J, Horner K, Jacobs R (2014) Can preoperative imaging help to predict postoperative outcome after wisdom tooth removal? A randomized controlled trial using panoramic radiography versus cone-beam CT. Clin Oral Investig 18:335–342. https://doi.org/10.1007/s00784-013-0971-x
Lvovsky A, Bachrach S, Kim HC, Pawar A, Levinzon O, Ben Itzhak J, Solomonov M (2018) Relationship between root apices and the mandibular canal: a cone-beam computed tomographic comparison of 3 populations. J Endod 44:555–558. https://doi.org/10.1016/j.joen.2017.12.020
Jadu FM, Alhazmi D, Badr FF, Jan AM (2017) Quantitative assessment of mandibular canal compression assessed by cone beam computed tomography. Oral Surg Oral Med Oral Pathol Oral Radiol 124:413–419. https://doi.org/10.1016/j.oooo.2017.07.006
Zhang X, Xu N, Wang H, Yu Q (2017) A cone-beam computed tomographic study of apical surgery-related morphological characteristics of the distolingual root in 3-rooted mandibular first molars in a Chinese population. J Endod 43:2020–2024. https://doi.org/10.1016/j.joen.2017.07.022
Lauber R, Bornstein MM, von Arx T (2012) Cone beam computed tomography in mandibular molars referred for apical surgery. Schweiz Monatsschr Zahnmed 122:12–24
Song M, Kim SG, Shin SJ, Kim HC, Kim E (2013) The influence of bone tissue deficiency on the outcome of endodontic microsurgery: a prospective study. J Endod 39:1341–1345. https://doi.org/10.1016/j.joen.2013.06.036
Jin GC, Kim KD, Roh BD, Lee CY, Lee SJ (2005) Buccal bone plate thickness of the Asian people. J Endod 31:430–434
Kim D, Ha JH, Jin MU, Kim YK, Kim SK (2016) Proximity of the mandibular molar root apex from the buccal bone surface: a cone-beam computed tomographic study. Restor Dent Endod 41:182–188. https://doi.org/10.5395/rde.2016.41.3.182
Tilk MA, Lommel TJ, Gerstein H (1979) A study of mandibular and maxillary root widths to determine dowel size. J Endod 5:79–82. https://doi.org/10.1016/s0099-2399(79)80153-3
Tilotta-Yasukawa F, Millot S, El Haddioui A, Bravetti P, Gaudy JF (2006) Labiomandibular paresthesia caused by endodontic treatment: an anatomic and clinical study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102:e47–e59. https://doi.org/10.1016/j.tripleo.2006.02.017
Gonzalez-Martin M, Torres-Lagares D, Gutierrez-Perez JL, Segura-Egea JJ (2010) Inferior alveolar nerve paresthesia after overfilling of endodontic sealer into the mandibular canal. J Endod 36:1419–1421. https://doi.org/10.1016/j.joen.2010.03.008
Poveda R, Bagan JV, Fernandez JM, Sanchis JM (2006) Mental nerve paresthesia associated with endodontic paste within the mandibular canal: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102:e46–e49. https://doi.org/10.1016/j.tripleo.2006.03.022
Chkoura A, El Wady W (2013) Position of the mental foramen in a Moroccan population: a radiographic study. Imaging Sci Dent 43:71–75. https://doi.org/10.5624/isd.2013.43.2.71
Khojastepour L, Mirbeigi S, Mirhadi S, Safaee A (2015) Location of mental foramen in a selected Iranian population: a CBCT assessment. Iran Endod J 10:117–121
Udhaya K, Saraladevi KV, Sridhar J (2013) The morphometric analysis of the mental foramen in adult dry human mandibles: a study on the south Indian population. J Clin Diagn Res 7:1547–1551. https://doi.org/10.7860/jcdr/2013/6060.3207
Goyushov S, Tozum MD, Tozum TF (2018) Assessment of morphological and anatomical characteristics of mental foramen using cone beam computed tomography. Surgical and radiologic anatomy 40:1133–1139. https://doi.org/10.1007/s00276-018-2043-z
Phillips JL, Weller RN, Kulild JC (1990) The mental foramen: 1. Size, orientation, and positional relationship to the mandibular second premolar. J Endod 16:221–223
Phillips JL, Weller RN, Kulild JC (1992) The mental foramen: 3. Size and position on panoramic radiographs. J Endod 18:383–386
Kovisto T, Ahmad M, Bowles WR (2011) Proximity of the mandibular canal to the tooth apex. J Endod 37:311–315. https://doi.org/10.1016/j.joen.2010.11.030
Sato I, Ueno R, Kawai T, Yosue T (2005) Rare courses of the mandibular canal in the molar regions of the human mandible: a cadaveric study. Okajimas Folia Anat Jpn 82:95–101
Burklein S, Grund C, Schafer E (2015) Relationship between root apices and the Mandibular Canal: a cone-beam computed tomographic analysis in a German population. J Endod 41:1696–1700. https://doi.org/10.1016/j.joen.2015.06.016
Kosumarl W, Patanaporn V, Jotikasthira D, Janhom A (2017) Distances from the root apices of posterior teeth to the maxillary sinus and mandibular canal in patients with skeletal open bite: a cone-beam computed tomography study. Imaging Sci Dent 47:157–164. https://doi.org/10.5624/isd.2017.47.3.157
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors. The study was approved by the Ethics Committee of Bolu Abant İzzet Baysal University (Decision No: 2018/132). The study was performed in accordance with the ethical standards aid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
The Ethics Committee approved Informed Consent dismissal.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Uğur Aydın, Z., Göller Bulut, D. Relationship between the anatomic structures and mandibular posterior teeth for endodontic surgery in a Turkish population: a cone-beam computed tomographic analysis. Clin Oral Invest 23, 3637–3644 (2019). https://doi.org/10.1007/s00784-019-02834-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02834-y