Abstract
Objective
The objective of this work was to investigate in vivo the effects of calcium hydroxide-based intracanal medication (ICM) on the levels of bacteria, pro-inflammatory cytokines (PICs), and matrix metalloproteinases (MMPs) in root canals and periradicular tissues of teeth with failure of the root canal treatment and apical periodontitis.
Materials and methods
Twenty infected root canals of single-rooted teeth were randomly assigned into two groups according to the irrigant used for chemomechanical preparation (CMP) (n = 10 per group): G1 – 2% chlorhexidine (CHX) gel and G2 – 6% sodium hypochlorite (NaOCl). Root canal contents were taken by using paper points before CMP (S1) and after 30 days of calcium hydroxide-based ICM (S2). Microbial reduction was calculated by means of colony-forming unit count (CFU/mL), with PICs and MMPs (pg/mL) being measured by using enzyme-linked immunosorbent assay (ELISA).
Results
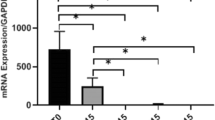
Culturable bacteria (101.2 ± 79.2), PICs (IL-1β 1.2 ± 0.4 and TNF-α 8.8 ± 4.7), MMP-2 (803.7 ± 96.4), MMP-3 (453.9 ± 229.3), MMP-8 (245.9 ± 122.4), MMP-9 (129.4 ± 29.6), and MMP-13 (70.8 ± 12.8) were present in all S1 samples. After 30 days of ICM (S2), a 99.5% microbial reduction was observed, together with a significant reduction of PICs in all groups. Overall, it was observed a decrease in the levels of MMPs (S2), except MMP-13, which was found in increased levels after ICM (P < .05), independently of the groups.
Conclusions
Calcium hydroxide-based intracanal medications have had a positive effect on the microbial reduction by decreasing the levels of PICs and MMPs. Both auxiliary chemical substances (i.e., 2% CHX and 6% NaOCl) presented similar effects when calcium hydroxide was used as intracanal medication.
Clinical relevance
Teeth with failure of the root canal treatment and apical periodontitis, and consequently with high levels of bacteria, PIC, and MMP, may present a better prognosis after a 30 days of a calcium hydroxide-based ICM.
Similar content being viewed by others
References
Gomes BP, Lilley JD, Drucker DB (1996) Associations of endodontic symptoms and signs with particular combinations of specific bacteria. Int Endod J 29:69–75
Pinheiro ET, Gomes BP, Ferraz CC, Sousa EL, Teixeira FB, Souza-Filho FJ (2003a) Microorganisms from canals of root-filled teeth with periapical lesions. Int Endod J 36(1):1–11
Pinheiro ET, Gomes BP, Ferraz CC, Teixeira FB, Zaia AA, Souza-Filho FJ (2003b) Evaluation of root canal microorganisms isolated from teeth with endodontic failure and their antimicrobial susceptibility. Oral Microbiol Immunol 18:100–103
Endo MS, Martinho FC, Zaia AA, Ferraz CC, Almeida JF, Gomes BP (2012) Quantification of cultivable bacteria and endotoxin in post-treatment apical periodontitis before and after chemo-mechanical preparation. Eur J Clin Microbiol Infect Dis 31:2575–2583
Zhang C, Hou BX, Zhao HY, Sun Z (2012) Microbial diversity in failed endodontic root-filled teeth. Chin Med J 125:1163–1168
Barbosa-Ribeiro M, De-Jesus-Soares A, Zaia AA, Ferraz CC, Almeida JF, Gomes BP (2016) Antimicrobial susceptibility and characterization of virulence genes of Enterococcus faecalis isolates from teeth with failure of the endodontic treatment. J Endod 42:1022–1028
Martinho FC, Chiesa WM, Leite FR, Cirelli JA, Gomes BP (2011) Antigenicity of primary endodontic infection against macrophages by the levels of PGE(2) production. J Endod 7:602–607
Endo MS, Ferraz CC, Zaia AA, Almeida JF, Gomes BP (2013) Quantitative and qualitative analysis of microorganisms in root-filled teeth with persistent infection: monitoring of the endodontic retreatment. Eur J Dent 7:302–309
Zhao L, Chen J, Cheng L, Wang X, Du J, Wang F, Peng Z (2013) Effects of Enterococcus faecalis lipoteichoic acid on receptor activator of nuclear factor-κB ligand and osteoprotegerin expression in periodontal ligament fibroblasts. Int Endod J 47:163–172
Hong CY, Lin SK, Kok SH, Cheng SJ, Lee MS, Wang TM, Chen CS, Lin LD, Wang JS (2004) The role of lipopolysaccharide in infectious bone resorption of periapical lesion. J Oral Pathol Med 33:162–169
Pezelj-Ribarić S, Magasić K, Prpić J, Miletić I, Karlović Z (2007) Tumor necrosis factor alpha in periapical tissue exudates of teeth with apical periodontitis. Mediat Inflamm 2007:69416
Martinho FC, Chiesa WM, Leite FR, Cirelli JA, Gomes BP (2012) Correlation between clinical/radiographic features and inflammatory cytokine networks produced by macrophages stimulated with endodontic content. J Endod 8:740–745
Martinho FC, Chiesa WM, Leite FR, Cirelli JA, Gomes BP (2010) Antigenic activity of bacterial endodontic contents from primary root canal infection with periapical lesions against macrophage in the release of interleukin-1beta and tumor necrosis factor alpha. J Endod 36:1467–1474
Sousa EL, Martinho FC, Leite FR, Nascimento GG, Gomes BP (2014) Macrophage cell activation with acute apical abscess contents determined by interleukin-1 Beta and tumor necrosis factor alpha production. J Endod 40:1752–1757
Lim GC, Torabinejad M, Kettering J, Linkhardt TA, Finkelman RD (1994) Interleukin 1-beta in symptomatic and asymptomatic human periradicular lesions. J Endod 20:225–227
Ataoglu H, Alptekin NO, Haliloglu S, Gursel M, Ataoglu T, Serpek B, Durmus E (2002) Interleukin-1beta, tumor necrosis factor-alpha levels and neutrophil elastase activity in peri-implant crevicular fluid. Clin Oral Implants Res 13:470–476
Ahmed GM, El-Baz AA, Hashem AA, Shalaan AK (2013) Expression levels of matrix metalloproteinase-9 and gram-negative bacteria in symptomatic and asymptomatic periapical lesions. J Endod 39:444–448
Sambandam V, Neelakantan P (2014) Matrix metalloproteinases (MMP) in restorative dentistry and endodontics. J Clin Pediatri Dent 39:57–59
Ozeki N, Kawai R, Yamaguchi H (2014) IL-1β-induced matrix metalloproteinase-13 is activated by a disintegrin and metalloprotease-28-regulated proliferation of human osteoblast-like cells. Expl Cell Res 323:165–177
Ozeki N, Hase N, Kawai R, Yamaguchi H, Hiyama T, Kondo A, Nakata K, Mogi M (2015) Unique proliferation response in odontoblastic cells derived from human skeletal muscle stem cells by cytokine-induced matrix metalloproteinase-3. Exp Cell Res 331:105–114
Hannas AR, Pereira JC, Granjeiro JM, Tjäderhane L (2007) The role of matrix metalloproteinases in the oral environment. Acta Odontol Scand 65:1–13
Martinho FC, Gomes CC, Nascimento GG, Gomes APM, Leite FRM (2018) Clinical comparison of the effectiveness of 7- and 14-day intracanal medications in root canal disinfection and inflammatory cytokines. Clin Oral Investig 22:523–530
Gomes BP, Vianna ME, Zaia AA, Almeida JF, Souza-Filho FJ, Ferraz CC (2013) Chlorhexidine in endodontics. Braz Dent J 24:89–102
Gomes BP, Vianna ME, Sena NT, Zaia AA, Ferraz CC, de Souza Filho FJ (2006) In vitro evaluation of the antimicrobial activity of calcium hydroxide combined with chlorhexidine gel used as intracanal medicament. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102:544–550
Duque TM, Prado M, Herrera DR, Gomes BPFA (2018) Periodontal and endodontic infectious/inflammatory profile in primary periodontal lesions with secondary endodontic involvement after a calcium hydroxide-based intracanal medication. Clin Oral Investig
Martinho FC, Gomes BP (2008) Quantification of endotoxins and cultivable bacteria in root canal infection before and after chemomechanical preparation with 2.5% sodium hypochlorite. J Endod 34:268–272
Gomes BP, Berber VB, Kokaras AS, Chen T, Paster BJ (2015) Microbiomes of endodontic-periodontal lesions before and after chemomechanical preparation. J Endod 41:1975–1984
Abi-Rached GP, Herrera DR, Zaia AA, Ferraz CC, Almeida JF, Gomes BP (2014) Efficacy of ethylene-diamine-tetra-acetic acid associated with chlorhexidine on intracanal medication removal: a scanning electron microscopy study. Microsc Res Tech 77:735–739
Zhender M (2006) Root canal irrigants. J Endod 32:389–398
Sousa EL, Martinho FC, Nascimento GG, Leite FR, Gomes BP (2014) Quantification of endotoxins in infected root canals and acute apical abscess exudates: monitoring the effectiveness of root canal procedures in the reduction of endotoxins. J Endod 40:177–181
Marinho ACS, To TT, Darveau RP, Gomes BPFA (2018) Detection and function of lipopolysaccharide and its purified lipid A after treatment with auxiliary chemical substances and calcium hydroxide dressings used in root canal treatment. Int Endod J 51:1118–1129
Henriques LC, de Brito LC, Tavares WL, Teles RP, Vieira LQ, Teles FR, Sobrinho AP (2016) Microbial ecosystem analysis in root canal infections refractory to endodontic treatment. J Endod 42:1239–1245
Herrera DR, Martinho FC, de-Jesus-Soares A, Zaia AA, Ferraz CCR, Almeida JFA, Gomes BPFA (2017) Clinical efficacy of EDTA ultrasonic activation in the reduction of endotoxins and cultivable bacteria. Int Endod J 50:933–940
Zandi H, Rodrigues RC, Kristoffersen AK, Enersen M, Mdala I, Ørstavik D, Rôças IN, Siqueira JF Jr (2016) Antibacterial effectiveness of 2 root canal irrigants in root-filled teeth with infection: a randomized clinical trial. J Endod 42:1307–1313
van Deuren M, Dofferhoff AS, van der Meer JW (1992) Cytokines and the response to infection. J Pathol 168:349–356
Shin SJ, Lee W, Lee JI, Baek SH, Kum KY, Shon WJ, Bae KS (2011) Matrix metalloproteinase-8 and substance P levels in gingival crevicular fluid during endodontic treatment of painful, nonvital teeth. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 112:548–554
Bauvois B (2012) New facets of matrix metalloproteinases MMP-2 and MMP-9 as cell surface transducers: outside-in signaling and relationship to tumor progression. Biochim Biophys Acta 1825:29–36
Carneiro E, Menezes R, Garlet GP, Garcia RB, Bramante CM, Figueira R, Sogayar M, Granjeiro JM (2009) Expression analysis of matrix metalloproteinase-9 in epithelialized and nonepithelialized apical periodontitis lesions. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 107:127–132
Dezerega A, Madrid S, Mundi V, Valenzuela MA, Garrido M, Paredes R, García-Sesnich J, Ortega AV, Gamonal J, Hernández M (2012) Pro-oxidant status and matrix metalloproteinases in apical lesions and gingival crevicular fluid as potential biomarkers for asymptomatic apical periodontitis and endodontic treatment response. J Inflamm (Lond) 9:8
Geijersstam A, Sorsa T, Stackelberg S, Tervahartiala T, Haapasalo M (2005) Effect of E. faecalis on the release of serine proteases elastase and cathepsin G, and collagenase-2 (MMP-8) by human polymorphonuclear leukocytes (PMNs). Int Endod J 8:667–677
Matsui H, Yamasaki M, Nakata K, Amano K, Nakamura H (2011) Expression of MMP-8 and MMP-13 in the development of periradicular lesions. Int Endod J 44:739–745
Wahlgren J, Salo T, Teronen O, Luoto H, Sorsa T, Tjäderhane L (2002) Matrix metalloproteinase-8 (MMP-8) in pulpal and periapical inflammation and periapical root-canal exudates. Int Endod J 35:897–904
Funding
This work was supported by the Brazilian agencies São Paulo Research Foundation (FAPESP, grant no. 2015/23479-5), National Council for Scientific and Technological Development (CNPq, grant no. 308162/2014-5) and Coordination for the Improvement of Higher Education Personnel (CAPES). We are thankful to Maicon R Z Passini, from the Piracicaba Dental School-UNICAMP for the technical support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The present study was approved by the Research Ethics Committee of the Piracicaba Dental School, State University of Campinas – UNICAMP, São Paulo, SP, Brazil. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Barbosa-Ribeiro, M., Arruda-Vasconcelos, R., de-Jesus-Soares, A. et al. Effectiveness of calcium hydroxide-based intracanal medication on infectious/inflammatory contents in teeth with post-treatment apical periodontitis. Clin Oral Invest 23, 2759–2766 (2019). https://doi.org/10.1007/s00784-018-2719-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2719-0