Abstract
Background
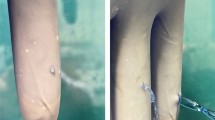
The transmission of blood-borne pathogens during surgery is a major concern. Surgical gloves are the primary barrier between the surgeon and the patient. Surgical procedures that need manual handling of bony surfaces or sharp instruments have the highest risk of glove perforations. The frequencies and the sites of surgical glove perforations in arthroplasty procedures were assessed.
Methods
We assessed the surgical glove perforations in total hip and knee arthroplasty procedures. Double standard latex gloves were used. A total of 983 outer and 511 inner gloves were tested. The gloves of all the surgical team members were tested for perforations during the first and second hours of surgery.
Results
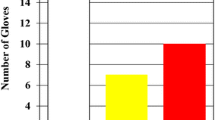
There were 18.4% outer and 8.4% inner glove perforations. The most frequent site of perforation was the second digit of the nondominant hand (25.5%). We found that hip and knee arthroplasty had significantly more glove perforation risk for the surgeon in the first half of the operation rather than the second half, and 57.8% of the perforations were at the index finger and the thumb.
Conclusions
Arthroplasty procedures still have high glove perforation rates despite the use of double gloving with frequent changes. Extra augmentation of the gloves in selected areas of the hand, in addition to double gloving, may be safer and more cost-effective than double gloving alone.
Similar content being viewed by others
References
Laine T, Aarnio P. How often does glove perforation occur in surgery? Comparison between single gloves and a double-gloving system. Am J Surg 2001;181:564–566.
Laine T, Kaipia A, Santavirta J, Aarnio P. Glove perforations in open and laparoscopic abdominal surgery: the feasibility of double gloving. Scand J Surg 2004;93:73–76.
Sebold JE, Jordan LR. Intraoperative glove perforation. Clin Orthop Relat Res 1993;297:242–244.
European Committee for Standardisation. EN 455-1:1993 E. Medical gloves for single use. Par. 1: requirements and testing for freedom from holes. Milton Keynes, England: British Standards Institute.
Landovitz RJ. Occupational and nonoccupational postexposure prophylaxis for HIV in 2009. Top HIV Med 2009;17:104–108. Review. Erratum in: Top HIV Med 2009;17:134.
De Carli G, Puro V, Ippolito G; Studio Italiano Rischio Occupazionale da HIV Group. Risk of hepatitis C virus transmission following percutaneous exposure in healthcare workers. Infection 2003;31(Suppl 2):22–27.
Sulkowski MS, Ray SC, Thomas DL. Needlestick transmission of hepatitis C. JAMA 2002;8;287:2406–2413.
Bennett NT, Howard RJ. Quantity of blood inoculated in a needlestick injury from suture needles. J Am Coll Surg 1994;178:107–110.
Misteli H, Weber WP, Reck S, Rosenthal R, Zwahlen M, Fueglistaler P, Bolli MK, et al. Surgical glove perforation and the risk of surgical site infection. Arch Surg 2009;144:553–558; discussion.
Lefebvre DR, Strande LF, Hewitt CW. An enzyme-mediated assay to quantify inoculation volume delivered by suture needlestick injury: two gloves are better than one. J Am Coll Surg 2008;206:113–122. Epub 2007 Sep 17.
Krikorian R, Lozach-Perlant A, Ferrier-Rembert A, Hoerner P, Sonntag P, Garin D, Crance JM. Standardization of needlestick injury and evaluation of a novel virus-inhibiting protective glove. J Hosp Infect 2007;66:339–345. Epub 2007 Aug 6.
Thomas S, Agarwal M, Mehta G. Intraoperative glove perforation — single versus double gloving in protection against skin contamination. Postgrad Med J 2001;77:458–460.
Al-Habdan I, Corea JR, Sadat-Ali M. Double or single gloves: which is safer in pediatric orthopedic surgery? J Pediatr Orthop 2006;26:409–411.
Sadat-Ali M, Al-Habdan I, AlBluwi M, Corea JR, Al-Othman A, Shriyan D, et al. Can double gloves improve surgeon-patient barrier efficiency? Int Surg 2006;91:181–184.
Laine T, Aarnio P. Glove perforation in orthopaedic and trauma surgery. J Bone Joint Surg (Br) 2004;86:898–900.
Thanni LOA, Yinusa W. Incidence of glove failure during orthopedic operations and the protective effect of double gloves. J Natl Med Assoc 2003;95:1184–1188.
Tanner J, Parkinson H. Double gloving to reduce surgical crossinfection. Cochrane Database Syst Rev 2002;3:CD003087.
Tanner J, Parkinson H. Double gloving to reduce surgical crossinfection. Cochrane Database Syst Rev 2006;19:CD003087.
Doebbeling BN, Wenzel RP. The direct costs of universal precautions in a teaching hospital. JAMA 1990;24–31;264:2083–2087.
Siegel JD, Reinehart E, Jackson M, Chiarello L. Health Care Infection Control Practices Advisory Committee. 2007 Guideline for isolation precautions: Preventing transmission of infectious agents in health care settings. Am J Infect Control 2007;35(10 Suppl 2):S65–S164.
Lafrenière R, Bohnen JMA, Pasieka J, Spry CC. Infection control in the operating room: current practices or sacred cows? J Am Coll Surg 2001;193:407–416.
Chapman S, Duff P. Frequency of glove perforations and subsequent blood contact in association with selected obstetric surgical procedures. Am J Obstet Gynecol 1993;168:1354–1357.
Murta EFC, Silva CS, Junior ORA. Frequency of glove perforation and the protective effect of double gloves in gynecological surgery. Arch Gynecol Obstet 2003;268:82–84.
Author information
Authors and Affiliations
About this article
Cite this article
Demircay, E., Unay, K., Bilgili, M.G. et al. Glove perforation in hip and knee arthroplasty. J Orthop Sci 15, 790–794 (2010). https://doi.org/10.1007/s00776-010-1547-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-010-1547-0