Abstract
Introduction
To investigate the factors associated with changes in vertebral bone mineral density during teriparatide treatment.
Materials and methods
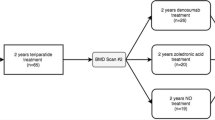
Single centre, longitudinal study involving 145 osteoporotic postmenopausal women treated with teriparatide. Clinical evaluation, bone mineral density (BMD) measurements assessment and laboratory analyses were performed at baseline then after 12 and 18 months of treatment. Bone non-response to treatment was defined as no significant increase in BMD at 18 months as compared to baseline.
Results
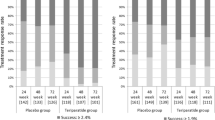
Of the 145 women initially included, 109 completed the 18-month course of the treatment. 75% of them had a history of prior osteoporotic treatment. Baseline mean age was 60 ± 8 years. Mean baseline vertebral T-score was − 3.7 ± 0.7 and 83 (76%) women had suffered at least one vertebral fracture. At the end of treatment, 18 women (17%) were classified as non-responders. In the responder group (n = 91), vertebral BMD increased by 0.091 ± 0.04 g/cm2 (12.2 ± 5.3%). Clinical characteristics, baseline BMDs and the percentage of women previously treated with bisphosphonates as well as the duration of prior treatment did not significantly differ between the two groups of responders and non-responders. At baseline, non-responders had significant mean lower C-terminal fragment of type 1 collagen (CTX) values than responders (p < 0.01). Only baseline CTX values (r = 0.30 p < 0.01) were independently correlated to vertebral BMD changes during teriparatide treatment.
Conclusion
A minority of treated women had no vertebral densitometric gain after 18 months of teriparatide therapy. Low levels of baseline bone remodeling were the main factor associated with poor response to treatment.


Similar content being viewed by others
References
Thomas T (2006) Intermittent parathyroid hormone therapy to increase bone formation. Jt Bone Spine 73:262–269
Neer RM, Arnaud CD, Zanchetta JR, Prince R, Gaich GA et al (2001) Effect of parathyroid hormone (1–34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med 344:1434–1441
Chen P, Miller PD, Delmas PD, Misurski DA, Krege JH et al (2006) Change in lumbar spine BMD and vertebral fracture risk reduction in teriparatide-treated postmenopausal women with osteoporosis. J Bone Miner Res 21:1785–1790
Chen P, Miller PD, Recker R, Resch H, Rana A et al (2007) Increases in BMD correlate with improvements in bone microarchitecture with teriparatide treatment in postmenopausal women with osteoporosis. J Bone Miner Res 22:1173–1180
Krege JH, Lane NE, Harris JM, Miller PD (2014) PINP as a biological response marker during teriparatide treatment for osteoporosis. Osteoporos Int 25:2159–2171
Eastell R, Krege JH, Chen P, Glass EV, Reginster J-Y et al (2006) Development of an algorithm for using PINP to monitor treatment of patients with teriparatide. Curr Med Res Opin 22:61–66
Glover SJ, Eastell R, McCloskey EV, Rogers A, Garnero P et al (2009) Rapid and robust response of biochemical markers of bone formation to teriparatide therapy. Bone 45:1053–1058
Eastell R, Mitlak BH, Wang Y, Hu M, Fitzpatrick LA et al (2019) Bone turnover markers to explain changes in lumbar spine BMD with abaloparatide and teriparatide: results from ACTIVE. Osteoporos Int 30:667–673
Blumsohn A, Marin F, Nickelsen T, Brixen K, Sigurdsson G et al (2011) Early changes in biochemical markers of bone turnover and their relationship with bone mineral density changes after 24 months of treatment with teriparatide. Osteoporos Int 22:1935–1946
Chen P, Satterwhite JH, Licata AA, Lewiecki EM, Sipos AA et al (2005) Early changes in biochemical markers of bone formation predict BMD response to teriparatide in postmenopausal women with osteoporosis. J Bone Miner Res 20:962–970
Niimi R, Kono T, Nishihara A, Hasegawa M, Matsumine A et al (2014) An algorithm using the early changes in PINP to predict the future BMD response for patients treated with daily teriparatide. Osteoporos Int 25:377–384
Lu C, Chen Y, Zhang B, Chen Y, Bai F et al (2017) Response to teriparatide in Chinese patients with established osteoporosis: osteocalcin and lumbar spine bone-mineral density changes from teriparatide phase III study. Clin Interv Aging 12:1717–1723
Tsujimoto M, Chen P, Miyauchi A, Sowa H, Krege JH et al (2011) PINP as an aid for monitoring patients treated with teriparatide. Bone 48:798–803
Gallagher JC, Rosen CJ, Chen P, Misurski DA, Marcus R et al (2006) Response rate of bone mineral density to teriparatide in postmenopausal women with osteoporosis. Bone 39:1268–1275
Elraiyah T, Ahmed AH, Wang Z, Farr JN, Murad MH et al (2016) Predictors of teriparatide treatment failure in patients with low bone mass. Bone Rep 4:17–22
Heaney RP, Watson P (2011) Variability in the measured response of bone to teriparatide. Osteoporos Int 22:1703–1708
Obermayer-Pietsch BM, Marin F, McCloskey EV, Hadji P, Farrerons J et al (2008) Effects of two years of daily teriparatide treatment on BMD in postmenopausal women with severe osteoporosis with and without prior antiresorptive treatment. J Bone Miner Res 23:1591–1600
Schwarz P, Jorgensen NR, Mosekilde L, Vestergaard P (2012) Effects of increasing age, dosage, and duration of PTH treatment on BMD increase–a meta-analysis. Calcif Tissue Int 90:165–173
Boonen S, Marin F, Obermayer-Pietsch B, Simões ME, Barker C et al (2008) Effects of previous antiresorptive therapy on the bone mineral density response to two years of teriparatide treatment in postmenopausal women with osteoporosis. J Clin Endocrinol Metab 93:852–860
Niimi R, Kono T, Nishihara A, Hasegawa M, Matsumine A et al (2014) Determinants associated with bone mineral density increase in response to daily teriparatide treatment in patients with osteoporosis. Bone 66:26–30
Niimi R, Kono T, Nishihara A, Hasegawa M, Kono T et al (2016) A retrospective analysis of nonresponse to daily teriparatide treatment. Osteoporos Int 27:2845–2853
Middleton ET, Steel SA, Doherty SM (2007) The effect of prior bisphosphonate exposure on the treatment response to teriparatide in clinical practice. Calcif Tissue Int 81:335–340
Geusens P, Marin F, Kendler DL, Russo LA, Zerbini CAF et al (2018) Effects of teriparatide compared with risedronate on the risk of fractures in subgroups of postmenopausal women with severe osteoporosis: the VERO trial. J Bone Miner Res 33:783–794
Ettinger B, San Martin J, Crans G, Pavo I (2004) Differential effects of teriparatide on BMD after treatment with raloxifene or alendronate. J Bone Miner Res 19:745–751
Pouilles JM, Tremollieres F, Todorovsky N, Ribot C (1991) Precision and sensitivity of dual-energy x-ray absorptiometry in spinal osteoporosis. J Bone Miner Res 6:997–1002
Miller PD, Delmas PD, Lindsay R, Watts NB, Luckey M et al (2008) Early responsiveness of women with osteoporosis to teriparatide after therapy with alendronate or risedronate. J Clin Endocrinol Metab 93:3785–3793
Ste-Marie LG, Schwartz SL, Hossain A, Desaiah D, Gaich GA et al (2006) Effect of teriparatide [rhPTH(1–34)] on BMD when given to postmenopausal women receiving hormone replacement therapy. J Bone Miner Res 21:283–291
Delmas PD, Licata AA, Reginster JY, Crans GG, Chen P et al (2006) Fracture risk reduction during treatment with teriparatide is independent of pretreatment bone turnover. Bone 39:237–243
Marcus R, Wang O, Satterwhite J, Mitlak B (2003) The skeletal response to teriparatide is largely independent of age, initial bone mineral density, and prevalent vertebral fractures in postmenopausal women with osteoporosis. J Bone Miner Res 18:18–23
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Anna, G., Anne-Lise, F., Clémence, D. et al. Factors associated with bone response to teriparatide in young postmenopausal women with osteoporosis. J Bone Miner Metab 41, 278–285 (2023). https://doi.org/10.1007/s00774-023-01412-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-023-01412-3