Abstract
Purpose
Approaches for lumbar corpectomies can be roughly categorized into anterolateral (AL) and posterolateral (PL) approaches. It remains controversial to date whether one approach is superior to the other, and no comparative studies exist for the two approaches for lumbar corpectomies.
Methods
A systematic review of the literature was performed through a MEDLINE/PubMed search. Studies and case reports describing technique plus outcomes and possible complications were included. Thereafter, estimated blood loss (EBL), length of operation (LOO), utilized implants, neurological outcomes, complication rates, and reoperation rates were analyzed.
Results
A total of 64 articles reporting on 702 patients including 513 AL and 189 PL corpectomies were included in this paper. All patients in the PL group were instrumented via the same approach used for corpectomy, while in the AL group the majority (68.3%) of authors described the use of an additional approach for instrumentation. The EBL was higher in the AL group (1393 ± 1341 ml vs. 982 ± 567 ml). The LOO also was higher in the AL group (317 ± 178 min vs. 258 ± 93 min). The complication rate (20.5% vs. 29.1%, p = 0.048) and the revision rate (3.1% vs. 9.5%, p = 0.004) were higher in the PL group. Neurological improvement rates were 43.8% (AL) vs. 39.2% (PL), and deterioration was only noted in the AL group (6.0%), while 50.2% (AL) and 60.8% (PL) showed no change from initial presentation to the last follow-up.
Conclusion
While neurological outcomes of both approaches are comparable, the results of the present review demonstrated lower complication and revision rates in anterolateral corpectomies. Nevertheless, individual patient characteristics must be considered in decision-making.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lumbar corpectomies represent one of the most challenging spinal procedures. Common indications for lumbar corpectomy include fractures due to trauma, osteoporosis, or neoplastic infiltration of vertebral bodies [23, 49, 63]. Despite the abundant availability of literature addressing the outcome of thoracolumbar corpectomies, only a few studies report isolated outcome data specifically for lumbar corpectomies [15, 22, 39, 42, 53, 61, 63, 69, 70, 80, 83, 88].
Due to the anatomical differences between the lumbar spine and thoracic spine, numerous distinctions between corpectomy approaches have been described. Biomechanically, the lumbar spine is more flexible than the thoracic spine. The rib cage makes the thoracic spine less mobile, and hence thoracic corpectomies require less instrumentation compared to lumbar corpectomies [57, 63]. Adjacent segment disease is less common in the thoracic spine. Moreover, proximal or distal junctional failure related to the apex of the thoracic kyphosis or the thoracolumbar junction may occur [33]. Additionally, approach-related obstacles such as abdominal organs, vasculature, lumbosacral plexus, and lumbar spinal nerve roots may pose challenges [79].
Lumbar corpectomy approaches may be categorized as anterolateral (AL) and posterolateral (PL). Traditionally, the AL approach was considered the gold standard for accessing the lumbar anterior column, as it provides direct visualization of the vertebral body [79, 84]. However, AL approaches may be less familiar to spine surgeons and frequently require additional posterior instrumentation in order to achieve a biomechanically stable fusion construct [49, 80]. Corpectomy via a PL approach was viewed as more challenging due to the lack of direct visualization of the pathology via a small transpedicular working channel. Moreover, the placement of a vertebral body replacement (VBR) device for anterior column reconstruction via a posterior route is complicated by the lumbar nerve roots that cannot be sacrificed, as it may be acceptable in the thoracic spine [36]. With recent technical advances such as expandable cages and neuronavigation, several limitations of the PL approach could be mitigated to a certain extent [33, 64]. Advantages of the PL approach include early visualization of neural structures as well as the possibility of transpedicular instrumentation in a single session.
The aim of the present review was to compare technical nuances and approach-related morbidity of the AL and the PL approach for lumbar corpectomy.
Methods
A systematic review of articles reporting on lumbar corpectomies, including approach-related morbidity, technical details, and outcomes, was performed according to the preferred reporting items for systematic reviews and meta-analyses (PRISMA) statement. A primary source for the electronic database search was MEDLINE/PubMed, supplemented by Google Scholar and reference lists of reviewed articles. Search strings included “lumbar corpectomy” and “thoracolumbar corpectomy” combined with the terms “anterior,” “posterior,” and “lateral” as well as “anterolateral” and “posterolateral.” We screened articles published between January 1999 and December 2021.
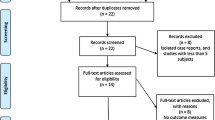
Retrospective and prospective studies as well as case reports were included if they reported clinical data as well as technical descriptions of AL and PL lumbar corpectomy approaches. Publications on thoracolumbar corpectomies were only included if outcome data of lumbar corpectomies were reported separately. A detailed description of our screening algorithm is provided in Fig. 1. To classify the level of evidence of the included studies, we adhered to the guidelines by Rutka (2017). Studies and patients were divided into AL and PL approaches and evaluated separately. The number of resected vertebral bodies and extent of instrumented fusion as well as the device used for VBR and the underlying pathology leading to the corpectomy procedure were assessed. For a more detailed analysis of interbody fusion, we evaluated if the instrumentation was performed over the same or an additional posterior approach in the case of an AL corpectomy.
Statistical analysis
For the statistical analysis, we separated the collected data into an AL and a PL group. We analyzed estimated blood loss (EBL), length of operation (LOO), and rates of neurological improvement and deterioration, as well as reoperation rates due to approach-related complications of each study. Rates were stated in percentages. The entire analysis was based on the number of patients included in the articles, in which the respective parameters were reported. We used the Mann–Whitney U test to compare the means of continuous variables (EBL and LOO). For categorical variables (complications and outcomes), the chi-square test was performed. A p-value of < 0.05 was considered statistically significant.
Results
Included studies
Sixty-four articles reporting a total of 702 patients were included in this systematic review. Anterolateral corpectomies were described in 41 articles, PL in 25, including two articles reporting on both AL and PL corpectomies. The latter two were included in both groups as they provided a separate analysis of patients. The included articles consisted of 38 retrospective studies, two prospective studies, and 24 case reports. There were 36 evidence level IV studies, three level III (one study PL only, two studies both AL and PL) studies, and one level II study (PL only) (Table 1). Among the included articles, 17 reported exclusively on lumbar corpectomies. In the remaining 47 studies, information about lumbar corpectomy patients was either provided separately or the necessary data was easily extractable.
Indications
Data from 513 patients with AL lumbar corpectomies could be extracted. Indications included traumatic fractures in 223 patients (58.5%), tumors in 107 (28.1%), infections in 86 (22.6%), osteoporotic lesions in 70 (18.4%), and degenerative changes or deformity in 27 (7.1%) patients. Posterolateral lumbar corpectomy was reported in 189 patients, including 99 (73.9%) patients with trauma, 74 (55.2%) with neoplasia, 12 (9.0%) with infection, three (1.6%) with degenerative changes or deformity, and one patient (0.5%) with osteoporosis (Table 2).
Procedures
Overall, a median of 1 (1–2) vertebral bodies was resected per patient. The majority of articles reported the use of expandable cages (AL 61.0%; PL 64.0%) and static cages (AL 14.6%; PL 16.0%) for VBR. The remaining articles described autologous bone only, bone cement, or a variety of the aforementioned VBR devices.
In the AL group, an additional approach for posterior transpedicular instrumentation was reported in 28 papers (68.3%), eight (19.5%) fused with unilateral anterior screw/plate constructs, and four (9.8%) used both anterior and posterior approach instrumentation, while information was not available in one (2.4%) article. In the PL group, a transpedicular instrumentation was performed in the same operative session in 23 (92.0%) papers, while one (4.0%) paper described the use of an additional approach, and one (4.0%) described both approaches. The majority of authors in the AL group (56.1%) described instrumentation one level above and below the corpectomy compared to the PL with two levels above and below instrumentation (64.0%) (Table 1).
The overall EBL and LOO averaged 1200 ± 1057 ml (data from 32 articles) and 301 ± 159 min (data from 27 articles) respectively. The EBL tended to be higher in the AL group (1393 ± 1341 ml) compared to the PL group (982 ± 567 ml, p = 0.787). The LOO turned out to be 317 ± 178 min in the AL group, and 258 ± 93 min in the PL group (p = 0.796).
Among papers reporting on AL corpectomies, a great heterogeneity regarding the technical nuances and access routes was noted. The choice for an access route was described based on the corpectomy level and the surgeon’s comfort as well as on the underlying pathology. Moreover, a clear time-based trend was observed. Earlier publications reported larger incisions, cylindrical cages or bone cement for VBR, and open pedicle screw instrumentation [6, 16, 20, 48, 55]. More recent articles tended to describe smaller openings, wide rectangular footplate cages, and percutaneous pedicle screw placement [1, 25, 56, 73, 80, 84].
Complications
The 115 approach-related complications were reported in 34 articles including 499 patients (AL 351; PL 148), resulting in an overall complication rate of 32.8% (Table 3). In the PL group (29.1%), the complication rate was significantly higher than in the AL group (20.5%; p = 0.048).
Implant-related complications (PL 8.1% vs. 3.7%; p = 0.045) and durotomy (PL 10.1% vs AL 1.4% p < 0.001) were significantly more common in the PL group. Surgical wound problems (AL 4.0% vs. 2.7%, p = 0.610) and nerve damage (AL 3.4% vs 2.7% p = 0.797) occurred at slightly different rates in both groups. Adjacent segment disease was reported in 1.7% of articles in the AL group, and in 2.7% of those in the PL group, thus significantly more in the PL group (p = 0.492). Vascular injury (2.3%), organ damage (1.7%), and pulmonary complications (2.3%) were only described in the AL group. Postoperative hematoma (2.7%) was exclusively reported in the PL group (Fig. 2).
Outcomes
A total of 25 patients required revision surgery for the abovementioned approach-related complications resulting in an overall revision rate of 5.0%. Revision surgery was significantly more frequently required in the PL group (9.5%) than in the AL group (3.1%, p = 0.004). Implant-related complications represented the most common reason for revision surgery (2.0% in the AL group, 4.7% in the PL group) (Fig. 3).
Neurological outcomes could be extracted from 39 studies with 371 patients (AL 251; PL 120).
In the AL group, 43.8% of patients improved, 6.0% deteriorated, and 50.2% showed no change from initial presentation to the last follow-up. In the PL group, 39.2% of patients improved, 60.8% showed no change, and none of the patients deteriorated (p = 0.158) (Fig. 4).
Discussion
To date, there are no studies comparing AL and PL approaches for lumbar corpectomies, and only few comparative studies for thoracic and thoracolumbar approaches exist [49, 85]. The main focus of this review was to analyze the AL and PL lumbar corpectomy approaches comparing technical issues, complications, and outcomes. One of the main challenges was to identify as many mutual parameters as possible to perform a direct comparison between the two approaches. The most common parameters outlined in the analyzed studies were represented by indications for surgery, procedure-related issues, perioperative complications, including revision surgery, as well as the clinical outcome.
Indications
Overall, we identified traumatic burst fractures as the most frequent indication for both AL and PL corpectomies while neoplastic infiltration of the vertebral bodies represented the second most common indication. While technically more challenging and associated with higher complication rates, the posterior approach is more versatile. In more complicated traumatic lumbar fractures with extensive damage to both the anterior and the posterior column, both columns can be addressed through a single PL approach [61]. The same is true for neoplastic vertebral infiltrations. Most of these lesions are due to metastases of breast, lung, colorectal, prostate, and kidney tumors. These infiltrations are mainly located extradurally and predominantly affect the anterior part of the vertebral bodies [30]. Spinal cord compression as a result of epidural spread often leads to the first clinical symptoms in these patients, so that a posterior approach with decompression, tumor mass reduction, VBR devices, and instrumented fusion is indicated. If the surgical goal is gross total tumor resection, the removal of all affected parts up to a complete en bloc vertebrectomy followed by circumferential reconstruction of both columns can be performed via a single-stage PL approach [33, 39, 49, 67]. Lumbar corpectomy for spinal infections was more commonly addressed via an AL approach, as anterolateral access corridors allow for more radical debridement and drainage of frequently accompanying psoas abscesses under direct visualization [44, 47].
Variations in access routes in relation to the corpectomy levels
Especially among AL approaches, several variations including a lateral retroperitoneal pre- or transpsoas approach, an anterior retroperitoneal or transperitoneal approach, and a lateral transdiaphragmatic approach to the thoracolumbar junction are performed. Since the upper, middle, and lower lumbar spine confront the surgeon with particular approach-related challenges, the choices for the abovementioned access routes were described depending on the corpectomy level. When accessing the upper lumbar vertebral bodies at the thoracolumbar junction, pleura, diaphragm, peritoneum, and overlying ribs are potential obstacles that need to be taken into consideration. While most authors described a partial rib resection, the greatest variation in thoracolumbar junction access corridors was found regarding the diaphragm. In general, the upper lumbar vertebrae can be accessed either via a craniocaudal-supradiaphragmatic or a caudocranial-infradiaphragmatic route [65]. While some authors reported detachment and anterior retraction of the diaphragm [88], others described incision and distraction of the diaphragm [73]. These variations appeared to be mostly dependent on the available retractor system.
In the middle lumbar spine, both retroperitoneal transpsoas and pre-psoas approaches via a far lateral or an anterolateral incision were commonly found. Most frequently, authors described the choice for either trans- or pre-psoas access routes based on the thickness of the psoas muscle in axial computed tomography or magnetic resonance images slices and the surgeons’ preference as well as the level affected. Due to the origin of the psoas muscle, a retroperitoneal pre-psoas approach may be easier in higher lumbar levels compared to the middle lumbar spine.
Another choice for the side of the approach refers to the coronary alignment of a potential deformity [63, 80]. Far lateral transpsoas approaches were rarely reported in lower lumbar spine corpectomies. In most cases, the iliac crest makes a strict lateral transpsoas approach challenging or even impossible. Moreover, splitting of the psoas muscle in the lower lumbar spine involves the risk for lumbosacral plexus injuries [79]. Therefore, L5 resections were commonly performed via a retroperitoneal oblique pre-psoas approach between vascular and muscle structures. Another option is to approach the lower lumbar spine through a strict anterior retroperitoneal approach with the advantage of a direct anterior visualization of the vertebras [15, 69]. In cases of extensive scar formation from previous abdominal surgeries, a transperitoneal access route was described by some authors [6, 83].
Assistance from an access surgeon may be helpful to mitigate the risk of surgical site morbidity in AL approaches [37]. Therefore, AL corpectomies may be more commonly performed in centers in which an access surgeon is readily available. However, whether the aid of an access surgeon is beneficial in reducing approach-related morbidity is still controversially discussed [34, 40, 72].
Overall, after anterior or lateral corpectomy procedures, a 4-point fixation directly adjacent to the resected vertebral body with lateral plates might not provide sufficient stability. Therefore, posterior instrumented fusion is commonly needed to gain additional stability [79].
Posterolateral approaches on the other hand are generally performed in a similar fashion throughout the entire lumbar spine. Approach variations are mostly dictated by the underlying pathology and the extent of bony resection required for adequate decompression and reconstruction [74]. However, the lumbar nerve roots may present a major obstacle in anterior column reconstruction following PL corpectomy [36]. Lumbar nerve routes exit the thecal sac in a rectangular trajectory close to the thoracolumbar junction and become more oblique towards the lumbosacral junction. Therefore, inserting a VBR device in the lower lumbar spine is described as less challenging, requires less nerve root and thecal sac retraction, and increases in complexity towards the upper lumbar spine. This is especially true for multilevel PL corpectomies [39, 79].
For both AL and PL corpectomies, minimally invasive variations have been described [1, 11, 11, 19, 21, 35, 53, 73]. However, due to the great heterogeneity of minimally invasive and less invasive variations, a detailed quantitative analysis was beyond the scope of the present review.
Biomechanical considerations
A major point of controversy when comparing AL and PL approaches is the biomechanical stability after corpectomy. This is especially true regarding the choice of the VBR device as well as the need for an additional posterior approach for instrumentation after an AL corpectomy.
When performing a PL approach for corpectomy, a circumferential reconstruction including anterior column reconstruction as well as posterior bilateral pedicle screw instrumentation may be performed via the same approach. In AL corpectomies, however, several options exist. It is possible to perform unilateral instrumentation via a unilateral screw-plate or screw-rod construct via the same approach or to perform an additional posterior approach for bilateral pedicle screw instrumentation. In this review, it was found that the majority of articles reporting AL corpectomies described the use of an additional posterior approach for bilateral pedicle screw instrumentation. It was found, however, that overall implant-related complication rates were higher in PL corpectomies than in AL corpectomies regardless of the approach used for instrumentation. Clinical case series and biomechanical studies of the cervical spine have shown that especially in multilevel corpectomies, additional posterior instrumentation is required to ensure a biomechanically stable construct [31, 32]. Lumbar biomechanical studies, however, revealed that 60% of the segmental stability in the lumbar spine is provided by the anterior column [38]. This indicates the importance of appropriately sized and shaped VBR devices. In a cadaveric corpectomy model, round and wide rectangular footprint cages along with either unilateral plate or bilateral pedicle screw instrumentation were compared in six degrees of freedom range of motion test. The results of this study suggested that regardless of unilateral or bilateral instrumentation, wide rectangular footprint cages provided more stability if compared to cylindrical footprint cages. This indicates that the footprint of the cage had more impact on lumbar segmental stiffness than the mode of instrumentation [54]. Similar findings were reported in several other cadaveric studies indicating that rectangular footprint cages offer a more favorable axial loading distribution and hence more segmental stability than cages with a circular footprint [59, 60].
The fact that only AL approaches offer enough space to insert a wide rectangular footprint cage has been described as a potential benefit over PL approaches [73, 84]. Due to inconsistent reporting of the cage footprint shape used in AL approaches, it was not possible to quantitatively assess a clear correlation between cage footprint and implant-related complications in this review. However, in a retrospective study of 52 AL corpectomies in the thoracic and lumbar spine, Smith et al. [73] reported transitioning from cylindric to wide rectangular cages over the course of the study. Implant failure related to cage subsidence was observed in 13.5% of patients with cylindric footprint cages as opposed to 0% if a wide footprint cage was used.
Outcomes and approach-related morbidity
Overall, the neurological improvement rates were similar in both groups. However, in the PL group, no neurological deterioration was reported, while in the AL group, deterioration occurred in 6.0% of patients.
The LOO was insignificantly higher for AL corpectomies. This may be attributable to the fact that the majority of articles reported the use of an additional posterior approach for instrumentation after AL corpectomy. Similarly, the mean EBL was higher in the AL group. In a study comparing thoracolumbar AL and PL approaches, it was observed that the EBL was only higher if additional posterior instrumentation was performed [49]. Overall, the complication and the revision rates were higher in the PL group than in the AL group. Since complete exposure of the thecal sac and the lumbar nerve roots is routinely required in PL corpectomies, accidental durotomies were far more common in PL corpectomies. In AL approaches, exposure of the dura is only required in cases of direct dural compression through bony fragments of the vertebral bodies. Moreover, achieving dural exposure over an AL approach is technically more challenging than in PL approaches, and not routinely accomplished.
In AL transpsoas approaches, the risk of lumbosacral plexus injury has been described as a major concern. Rates of postoperative thigh weakness after transpsoas surgery as high as 27% have been reported [14, 81]. For that reason, many spine surgeons advocate for the strict use of intraoperative neuromonitoring in AL transpsoas surgery in order to mitigate lumbosacral plexus damage [45, 46]. In a prospective multicentric study, dynamically evoked electromyography was utilized in 102 patients undergoing retroperitoneal transpsoas surgery. Postoperatively, 27.5% of patients experienced transient mild hip flexion weakness that resolved over 6 months in all patients. The authors concluded that rather than an actual nerve damage, a retraction-induced muscle trauma is responsible for postoperative lower extremity weakness after transpsoas surgery [81].
Overall, our results suggest higher approach-related morbidity in PL approaches for corpectomies in the lumbar spine. In a study comparing AL and PL approaches to the thoracolumbar spine, a similar morbidity rate of anterior-only and posterior-only approaches was found. Significantly increased morbidity was only described in cases of a combined anterior and posterior approach [49]. Similarly, a study reporting AL and PL corpectomies for neoplastic infiltration of the thoracic and thoracolumbar spine found no significant difference regarding complications or approach-related morbidity [85]. However, since these comparative studies report pooled outcomes of thoracic and lumbar corpectomies, the conclusions can be extrapolated to the lumbar spine only to a limited extent. When looking at the development in AL approaches over time, we observed a trend towards smaller accesses, wide footprint cages, and percutaneous posterior instrumentation in more recent studies. Recent technical advances such as neuronavigation, minimally invasive retractor systems, and modern cage devices might be responsible for the overall more favorable outcomes of AL corpectomies.
Limitations
The major limitation of this study is the quality and quantity of available studies reporting on lumbar corpectomies. Most studies analyzed both thoracic and lumbar corpectomies together. Therefore, parameters such as EBL, LOO, and neurological outcome and complications could frequently not be included if they were not explicitly attributed to lumbar corpectomy patients.
Only 17 studies were focused exclusively on outcomes of lumbar corpectomies, and no study provided comparative data on AL versus PL lumbar corpectomies.
The majority of patient outcome data analyzed in this review originated from AL corpectomies (64.1%). Additionally, most of the studies included were case series without control groups as highlighted in Table 1. Due to the heterogeneity and inconsistency of the analyzed outcome parameters, a statistical analysis was only performed for a fraction of the included studies. The results of this review should therefore be interpreted as trends rather than statistical evidence.
Conclusion
Both anterolateral and posterolateral lumbar corpectomies are challenging procedures with significant blood loss and high complication rates. While neurological outcomes of both approaches are similar, the results of this present review demonstrated significantly lower complication and revision rates in anterolateral corpectomies. However, especially outcomes of lumbar corpectomies via posterolateral approaches are scarcely reported, and to date, no comparative studies exist. This warrants further investigation by studies directly aimed at comparing outcomes between anterolateral and posterolateral corpectomies in the lumbar spine ideally including recent technological advancements like minimal-invasive approaches.
Data availability
Not applicable.
Code availability
Not applicable.
Abbreviations
- AL:
-
Anterolateral
- EBL:
-
Estimated blood loss
- LOO:
-
Length of operation
- PL:
-
Posterolateral
- VBR:
-
Vertebral body replacement
References
Adkins DE, Sandhu FA, Voyadzis J-M (2013) Minimally invasive lateral approach to the thoracolumbar junction for corpectomy. J Clin Neurosci 20:1289–1294. https://doi.org/10.1016/j.jocn.2012.09.051
Alhashash M, Shousha M (2022) Minimally invasive short-segment anteroposterior surgery for thoracolumbar osteoporotic fractures with canal compromise: a prospective study with a minimum 2-year follow-up. Asian Spine J 16(1):28–37. https://doi.org/10.31616/asj.2020.0573
Alshareef MA, Klapthor G, Lowe SR, Barley J, Cachia D, Frankel BM (2020) Strategies for posterior-only minimally invasive surgery in thoracolumbar metastatic epidural spinal cord compression. Surg Neurol Int 11:462. https://doi.org/10.25259/SNI_815_2020
Amaral R, Marchi L, Oliveira L, Coutinho T, Pimenta L (2013) Acute lumbar burst fracture treated by minimally invasive lateral corpectomy. Case Rep Orthop 2013:953897. https://doi.org/10.1155/2013/953897
Aryan HE, Lu DC, Acosta FL, Ames CP (2007) Corpectomy followed by the placement of instrumentation with titanium cages and recombinant human bone morphogenetic protein–2 for vertebral osteomyelitis. J Neurosurg Spine 6:23–30
Bhat AL, Lowery GL, Sei A (1999) The use of titanium surgical mesh-bone graft composite in the anterior thoracic or lumbar spine after complete or partial corpectomy. Eur Spine J 8:304–309
Byvaltsev VA, Kalinin AA, Polkin RA, Shepelev VV, Aliyev MA, Dyussembekov YK (2021) Minimally invasive corpectomy and percutaneous transpedicular stabilization in the treatment of patients with unstable injures of the thoracolumbar spine: Results of retrospective case series. J Craniovertebr Junction Spine 12:294
Carminucci A, Assina R, Hernandez RN, Goldstein IM (2017) Direct midline posterior corpectomy and fusion of a lumbar burst fracture with retrospondyloptosis. World Neurosurg 99:809-e11
Cho Y (2017) Corpectomy and circumferential fusion for advanced thoracolumbar Kümmell’s disease. Musculoskelet Surg 101:269–274
Choi J-I, Kim B-J, Ha S-K, Kim S-D, Lim D-J, Kim S-H (2017) Single-stage transpedicular vertebrectomy and expandable cage placement for treatment of unstable mid and lower lumbar burst fractures. Clin Spine Surg 30:E257–E264
Chou D, Lu DC (2011) Mini-open transpedicular corpectomies with expandable cage reconstruction. J Neurosurg Spine 14:71–77
Chou D, Wang VY, Gupta N (2009) Transpedicular corpectomy with posterior expandable cage placement for L1 burst fracture. J Clin Neurosci 16:1069–1072
Crabtree KL, Spurgeon A, Arzi H, Beaver B, Arnold PM (2011) L5 vertebral osteomyelitis treated with L5 corpectomy and anterior instrumentation: case report. Evid-Based Spine-Care J 2:49–54
Cummock MD, Vanni S, Levi AD, Yu Y, Wang MY (2011) An analysis of postoperative thigh symptoms after minimally invasive transpsoas lumbar interbody fusion. J Neurosurg Spine 15:11–18. https://doi.org/10.3171/2011.2.SPINE10374
Dai L-Y, Jiang L-S (2010) Anterior-only instrumentation and grafting after L5 corpectomy for non-traumatic lesions. Acta Orthopædica Belgica 76:94
Detwiler PW, Porter RW, Crawford NR, Apostolides PJ, Dickman CA (1999) Lumbosacral junction fixation and fusion after complete L-5 spondylectomy: case report. Neurosurg Focus 7:E5
Dhillon CS, Nanakkal AS, Chhasatia NP, Medagam NR, Khatavi A (2021) A rare case of contiguous three-level lumbar burst fractures-treated with combined posterior stabilization and anterior fusion. J Orthop Case Rep 11:71
Dhillon CS, Tantry R, Ega SR, Pophale C, Medagam NR, Chhasatia N (2020) Langerhans cell histiocytosis in the adult lumbar spine–a case report and literature review. J Orthop Case Rep 10:28
Donnelly DJ, Abd-El-Barr MM, Lu Y (2015) Minimally invasive muscle sparing posterior-only approach for lumbar circumferential decompression and stabilization to treat spine metastasis—technical report. World Neurosurg 84:1484–1490
Dvorak MF, Kwon BK, Fisher CG, Eiserloh HL III, Boyd M, Wing PC (2003) Effectiveness of titanium mesh cylindrical cages in anterior column reconstruction after thoracic and lumbar vertebral body resection. Spine 28:902–908
Eck JC (2011) Minimally invasive corpectomy and posterior stabilization for lumbar burst fracture. Spine J 11:904–908
Elnady B, Shawky A, Abdelrahman H, Elmorshidy E, El-Meshtawy M, Said GZ (2017) Posterior only approach for fifth lumbar corpectomy: indications and technical notes. Int Orthop 41:2535–2541
Foreman PM, Naftel RP, Moore TA, Hadley MN (2016) The lateral extracavitary approach to the thoracolumbar spine: a case series and systematic review. J Neurosurg Spine 24:570–579. https://doi.org/10.3171/2015.6.SPINE15169
Gallia GL, Sciubba DM, Bydon A, Suk I, Wolinsky J-P, Gokaslan ZL, Witham TF (2007) Total L-5 spondylectomy and reconstruction of the lumbosacral junction. J Neurosurg Spine 7:103–111
Gandhi SD, Liu DS, Sheha ED, Colman MW (2021) Prone transpsoas lumbar corpectomy: simultaneous posterior and lateral lumbar access for difficult clinical scenarios. J Neurosurg Spine 35:284–291
Gassie K, Erben Y, Fortich S, Carames GP, Sandhu SJS, Abode-Iyamah K (2021) Multilevel L4 and L5 corpectomy for burst fracture via an anterior transperitoneal approach followed by posterior stabilization: technical and anatomic considerations. Cureus 13(10)
Gezercan Y, Çavuş G, Ökten AI, Menekşe G, Çıkılı M, Adamhasan F, Arslan A, Açık V (2016) Single-stage posterolateral transpedicular approach with 360-degree stabilization and vertebrectomy in primary and metastatic tumors of the spine. World Neurosurg 95:214–221
Grobost P, Boudissa M, Kerschbaumer G, Ruatti S, Tonetti J (2020) Early versus delayed corpectomy in thoracic and lumbar spine trauma. A long-term clinical and radiological retrospective study. Orthop Traumatol Surg Res 106:261–267
Haque MU, Wilson AN, Blecher HD, Reich SM (2013) Lumbar hemangioma masking a plasma cell tumor—case report and review of the literature. Spine J 13:e11–e15
Harel R, Angelov L (2010) Spine metastases: current treatments and future directions. Eur J Cancer 46:2696–2707. https://doi.org/10.1016/j.ejca.2010.04.025
Hartmann S, Kavakebi P, Wipplinger C, Tschugg A, Girod PP, Lener S, Thomé C (2018) Retrospective analysis of cervical corpectomies: implant-related complications of one- and two-level corpectomies in 45 patients. Neurosurg Rev 41:285–290. https://doi.org/10.1007/s10143-017-0854-8
Hartmann S, Thomé C, Keiler A, Fritsch H, Hegewald AA, Schmölz W (2015) Biomechanical testing of circumferential instrumentation after cervical multilevel corpectomy. Eur Spine J 24:2788–2798. https://doi.org/10.1007/s00586-015-4167-8
Hofstetter CP, Chou D, Newman CB, Aryan HE, Girardi FP, Härtl R (2011) Posterior approach for thoracolumbar corpectomies with expandable cage placement and circumferential arthrodesis: a multicenter case series of 67 patients. J Neurosurg Spine 14:388–397
Holt RT, Majd ME, Vadhva M, Castro FP (2003) The efficacy of anterior spine exposure by an orthopedic surgeon. Clin Spine Surg 16:477–486
Huangxs S, Christiansen PA, Tan H, Smith JS, Shaffrey ME, Uribe JS, ... Yen CP (2020) Mini-open lateral corpectomy for thoracolumbar junction lesions. Oper Neurosurg 18(6):640–647
Hunt T, Shen FH, Arlet V (2006) Expandable cage placement via a posterolateral approach in lumbar spine reconstructions. J Neurosurg Spine 5:271–274
Jagannathan J, Chankaew E, Urban P, Dumont AS, Sansur CA, Kern J, Peeler B, Elias WJ, Shen F, Shaffrey ME, Whitehill R, Arlet V, Shaffrey CI (2008) Cosmetic and functional outcomes following paramedian and anterolateral retroperitoneal access in anterior lumbar spine surgery. J Neurosurg Spine 9:454–465. https://doi.org/10.3171/SPI.2008.9.11.454
James KS, Wenger KH, Schlegel JD, Dunn HK (1994) Biomechanical evaluation of the stability of thoracolumbar burst fractures. Spine 19:1731–1740
Jandial R, Kelly B, Chen MY (2013) Posterior-only approach for lumbar vertebral column resection and expandable cage reconstruction for spinal metastases. J Neurosurg Spine 19:27–33
Jarrett CD, Heller JG, Tsai L (2009) Anterior exposure of the lumbar spine with and without an “access surgeon”: morbidity analysis of 265 consecutive cases. J Spinal Disord Tech 22:559–564. https://doi.org/10.1097/BSD.0b013e318192e326
Joubert C, Adetchessi T, Peltier E, Graillon T, Dufour H, Blondel B, Fuentes S (2015) Corpectomy and vertebral body reconstruction with expandable cage placement and osteosynthesis via the single stage posterior approach: a retrospective series of 34 patients with thoracic and lumbar spine vertebral body tumors. World Neurosurg 84:1412–1422
Knoeller SM, Huwert O, Wolter T (2012) Single stage corpectomy and instrumentation in the treatment of pathological fractures in the lumbar spine. Int Orthop 36:111–117
Koller H, Mühlenkamp K, Hitzl W, Koller J, Ferraris L, Hostettler IC, Hempfing A (2021) Surgical outcomes with anatomic reduction of high-grade spondylolisthesis revisited: an analysis of 101 patients. J Neurosurg Spine 1:1–11
Korovessis P, Repantis T, Iliopoulos P, Hadjipavlou A (2008) Beneficial influence of titanium mesh cage on infection healing and spinal reconstruction in hematogenous septic spondylitis: a retrospective analysis of surgical outcome of twenty-five consecutive cases and review of literature. Spine 33:E759–E767
Le TV, Burkett CJ, Deukmedjian AR, Uribe JS (2013) Postoperative lumbar plexus injury after lumbar retroperitoneal transpsoas minimally invasive lateral interbody fusion. Spine 38:E13-20. https://doi.org/10.1097/BRS.0b013e318278417c
Lehmen JA, Gerber EJ (2015) MIS lateral spine surgery: a systematic literature review of complications, outcomes, and economics. Eur Spine J 24(Suppl 3):287–313. https://doi.org/10.1007/s00586-015-3886-1
Lener S, Hartmann S, Barbagallo GM, Certo F, Thomé C, Tschugg A (2018) Management of spinal infection: a review of the literature. Acta Neurochir 160:487–496
Liljenqvist U, Lerner T, Bullmann V, Hackenberg L, Halm H, Winkelmann W (2003) Titanium cages in the surgical treatment of severe vertebral osteomyelitis. Eur Spine J 12:606–612
Lu DC, Lau D, Lee JG, Chou D (2010) The transpedicular approach compared with the anterior approach: an analysis of 80 thoracolumbar corpectomies. J Neurosurg Spine 12:583–591
Lu DC, Wang V, Chou D (2009) The use of allograft or autograft and expandable titanium cages for the treatment of vertebral osteomyelitis. Neurosurgery 64:122–129; discussion 129–130. https://doi.org/10.1227/01.NEU.0000336332.11957.0B
Lu DC, Wang V, Chou D (2009) The use of allograft or autograft and expandable titanium cages for the treatment of vertebral osteomyelitis. Neurosurgery 64:122–130
McFarland III JR, Branch D, Gonzalez A, Campbell G, Lall RR (2020) L5 fracture dislocation secondary to cold abscess treated by posterior corpectomy with expandable cage placement. Cureus 12(6)
Mühlbauer M, Pfisterer W, Eyb R, Knosp E (2000) Minimally invasive retroperitoneal approach for lumbar corpectomy and anterior reconstruction. J Neurosurg Spine 93:161–167
Mundis GM, Eastlack RK, Moazzaz P, Turner AWL, Cornwall GB (2015) Contribution of round vs. rectangular expandable cage endcaps to spinal stability in a cadaveric corpectomy model. Int J Spine Surg 9:53 https://doi.org/10.14444/2053
Nairus JG, Richman JD, Douglas RA (1996) Retroperitoneal pseudomeningocele complicated by meningitis following a lumbar burst fracture: a case report. Spine 21:1090–1093
Nakashima H, Kanemura T, Satake K, Ito K, Tanaka S, Segi N, ... Imagama S (2021) Transdiaphragmatic approach as a novel less invasive retroperitoneal approach at thoracolumbar junction: Comparison with conventional diaphragmatic incision. Spine Surgery and Related Research, 2020-0191. Chicago
Oxland TR (2016) Fundamental biomechanics of the spine–what we have learned in the past 25 years and future directions. J Biomech 49:817–832. https://doi.org/10.1016/j.jbiomech.2015.10.035
Payer M, Sottas C (2008) Mini-open anterior approach for corpectomy in the thoracolumbar spine. Surg Neurol 69:25–31
Pekmezci M, Tang JA, Cheng L, Modak A, McClellan RT, Buckley JM, Ames CP (2012) Comparison of expandable and fixed interbody cages in a human cadaver corpectomy model, part I: endplate force characteristics. J Neurosurg Spine 17:321–326
Pekmezci M, Tang JA, Cheng L, Modak A, McClellan RT, Buckley JM, Ames CP (2016) Comparison of expandable and fixed interbody cages in a human cadaver corpectomy model. Clin Spine Surg 29:387–393
Pham MH, Tuchman A, Chen TC, Acosta FL, Hsieh PC, Liu JC (2017) Transpedicular corpectomy and cage placement in the treatment of traumatic lumbar burst fractures. Clin Spine Surg 30:360–366
Reddy Mallepally A, Marathe N, Shrivastava AK, Tandon V, Chhabra HS (2021) Functional outcomes of nerve root sparing posterior corpectomy in lumbar vertebral burst fractures. Global Spine J. https://doi.org/10.1177/2192568220984128
Richardson B, Paulzak A, Rusyniak WG, Martino A (2017) Anterior lumbar corpectomy with expandable titanium cage reconstruction: a case series of 42 patients. World Neurosurg 108:317–324. https://doi.org/10.1016/j.wneu.2017.08.179
Sasani M, Özer AF (2009) Single-stage posterior corpectomy and expandable cage placement for treatment of thoracic or lumbar burst fractures. Spine 34:E33–E40
Scheufler K-M (2007) Technique and clinical results of minimally invasive reconstruction and stabilization of the thoracic and thoracolumbar spine with expandable cages and ventrolateral plate fixation. Neurosurgery 61:798–809
Senel A, Kaya AH, Kuruoglu E, Celik F (2007) Circumferential stabilization with ghost screwing after posterior resection of spinal metastases via transpedicular route. Neurosurg Rev 30:131–137
Shen FH, Marks I, Shaffrey C, Ouellet J, Arlet V (2008) The use of an expandable cage for corpectomy reconstruction of vertebral body tumors through a posterior extracavitary approach: a multicenter consecutive case series of prospectively followed patients. Spine J 8:329–339
Shimada Y, Hongo M, Miyakoshi N, Kasukawa Y, Ando S, Itoi E, Abe E (2007) Giant cell tumor of fifth lumbar vertebrae: two case reports and review of the literature. Spine J 7:499–505
Shousha M, El-Saghir H, Boehm H (2014) Corpectomy of the fifth lumbar vertebra, a challenging procedure. Clin Spine Surg 27:347–351
Singh K, Park DK (2012) Lumbar extracavitary corpectomy with a single stage circumferential arthrodesis: surgical technique and clinical series. Am J Orthop 41:316
Sirinoglu D, Sarigul B, Derdiyok O, Baskurt O, Aydin MV (2021) Mini-open lateral approach for anterior lumbar corpectomy combined with posterior screw-rod system augmentation for correction of kyphosis. Trauma Case Reports 32:100428
Smith MW, Rahn KA, Shugart RM, Belschner CD, Stout KS, Cheng I (2011) Comparison of perioperative parameters and complications observed in the anterior exposure of the lumbar spine by a spine surgeon with and without the assistance of an access surgeon. Spine J 11:389–394. https://doi.org/10.1016/j.spinee.2011.03.014
Smith WD, Dakwar E, Le TV, Christian G, Serrano S, Uribe JS (2010) Minimally invasive surgery for traumatic spinal pathologies: a mini-open, lateral approach in the thoracic and lumbar spine. Spine 35:S338–S346
Spiessberger A, Arvind V, Gruter B, Cho SK (2020) Thoracolumbar corpectomy/spondylectomy for spinal metastasis: a pooled analysis comparing the outcome of seven different surgical approaches. Eur Spine J 29:248–256. https://doi.org/10.1007/s00586-019-06179-8
Srikantha U, Lokanath YK, Hari A, Nirmala S, Varma RG (2019) Minimally invasive lateral transpsoas approach for lumbar corpectomy and stabilization. Surg Neurol Int 10:153. https://doi.org/10.25259/SNI_292_2019
Street J, Fisher C, Sparkes J, Boyd M, Kwon B, Paquette S, Dvorak M (2007) Single-stage posterolateral vertebrectomy for the management of metastatic disease of the thoracic and lumbar spine: a prospective study of an evolving surgical technique. Clin Spine Surg 20:509–520
Tanaka M, Singh M, Fujiwara Y, Uotani K, Arataki S, Yamauchi T, Nakanishi K (2021) Minimally invasive thoracolumbar corpectomy and percutaneous pedicle screw fixation with computer-assisted rod-bending system in single lateral position. World Neurosurg 151:138–144
Tezer M, Ozturk C, Erturer E, Aydogan M, Hamzaoglu A (2006) Bilateral L5 radiculopathy due to osteoporotic LI vertebral fracture: a case report. J Spinal Cord Med 29:430–435
Theologis AA, Buchowski JM (2019) Vertebral body resection and lumbar corpectomies. In Seminars in Spine Surgery (Vol. 31, No. 2, pp. 70–80). WB Saunders
Theologis AA, Tabaraee E, Toogood P, Kennedy A, Birk H, McClellan RT, Pekmezci M (2016) Anterior corpectomy via the mini-open, extreme lateral, transpsoas approach combined with short-segment posterior fixation for single-level traumatic lumbar burst fractures: analysis of health-related quality of life outcomes and patient satisfaction. J Neurosurg Spine 24:60–68. https://doi.org/10.3171/2015.4.SPINE14944
Tohmeh AG, Rodgers WB, Peterson MD (2011) Dynamically evoked, discrete-threshold electromyography in the extreme lateral interbody fusion approach. J Neurosurg Spine 14:31–37. https://doi.org/10.3171/2010.9.SPINE09871
Tu C-H, Chiu Y-P, Ji H-R, Chiu C-D (2021) Primary osseous chondrosarcoma in the lumbar spine: case report and literature review with analysis. J Int Med Res. https://doi.org/10.1177/03000605211058890
Vazan M, Ryang Y-M, Gerhardt J, Zibold F, Janssen I, Ringel F, Gempt J, Meyer B (2017) L5 corpectomy—the lumbosacral segmental geometry and clinical outcome—a consecutive series of 14 patients and review of the literature. Acta Neurochir 159:1147–1152
Walker CT, Xu DS, Godzik J, Turner JD, Uribe JS, Smith WD (2018) Minimally invasive surgery for thoracolumbar spinal trauma. Ann Transl Med 6:102. https://doi.org/10.21037/atm.2018.02.10
Wiggins GC, Mirza S, Bellabarba C, West GA, Chapman JR, Shaffrey CI (2001) Perioperative complications with costotransversectomy and anterior approaches to thoracic and thoracolumbar tumors. Neurosurg Focus 11:1–9
Wong GKC, Kwan MCL, Ng RYT, Yu SCH, Poon WS (2011) Flow diverters for treatment of intracranial aneurysms: current status and ongoing clinical trials. J Clin Neurosci 18:737–740. https://doi.org/10.1016/j.jocn.2010.10.011
Wong ML, Lau HC, Kaye AH (2014) A modified posterolateral transpedicular approach to thoracolumbar corpectomy with nerve preservation and bilateral cage reconstruction. J Clin Neurosci 21:988–992
Zidan I, Khedr W, Fayed AA, Farhoud A (2019) Retroperitoneal extrapleural approach for corpectomy of the first lumbar vertebra: technique and outcome. J Korean Neurosurg Soc 62:61
Funding
Open access funding provided by University of Innsbruck and Medical University of Innsbruck.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Medical University of Innsbruck, Austria, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Spine – Other
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wipplinger, C., Lener, S., Orban, C. et al. Technical nuances and approach-related morbidity of anterolateral and posterolateral lumbar corpectomy approaches—a systematic review of the literature. Acta Neurochir 164, 2243–2256 (2022). https://doi.org/10.1007/s00701-022-05240-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05240-8