Abstract
Background
Studies assessing the effect of implementing good practice management guidelines (GPMG) in carotid revascularization within the same hospital are scarce. Thus, we aimed to evaluate the impact of GPMG implementation on the clinical outcomes of carotid revascularization procedures within a quaternary hospital.
Method
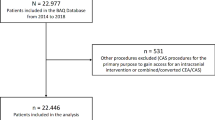
We retrospectively studied 177 patients with atherosclerotic carotid disease who underwent revascularization (carotid endarterectomy and carotid artery stenting) at a quaternary hospital between January 2012 and December 2019. The patients were divided into two groups: the pre-guideline group with 73 patients and the post-guideline group with 104 patients who underwent the procedures before and after the implementation of GPMG, respectively.
Results
Twelve (16.4%) and 3 (2.9%) patients had neurological complications in the pre- and post-guideline groups, respectively (p = 0.001); most complications were cases of ischemic stroke. There were fewer complications in men than in women (OR = 0.22; 95% CI 0.06–0.77). A significant decrease in neurological complications was observed in the carotid artery stenting group (pre-guideline 25.7% vs post-guideline 13.2%; p = 0.004). Logistic regression analysis of the predisposing factors for neurological complications in carotid endarterectomy and carotid artery stenting demonstrated that the implementation of GPMG was a determining factor for the improved results (odds ratio = 0.11, 95% CI 0.02–0.59).
Conclusions
Implementing GPMG for carotid revascularization resulted in better clinical results, with decreased neurological complications in patients that underwent angioplasty and endarterectomy.
Similar content being viewed by others
Data availability
The data used in this study can be provided by the authors on reasonable request.
Code availability
Not applicable.
References
Feasby TE, Quan H, Ghali WA (2002) Hospital and surgeon determinants of carotid endarterectomy outcomes. Arch Neurol 59:1877–1881
Flaherty ML, Kissela B, Khoury JC, Alwell K, Moomaw CJ, Woo D, Khatri P, Ferioli S, Adeoye O, Broderick JP, Kleindorfer D (2013) Carotid artery stenosis as a cause of stroke. Neuroepidemiology 40:36–41
Klaiman T, Pracilio V, Kimberly L, Cecil K, Legnini M (2014) Leveraging effective clinical registries to advance medical care quality and transparency. Popul Health Manag 17:127–133
Lozano R, Naghavi M, Foreman K, et al. (2012) Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380:2095–2128
Mead GE, Wardlaw JM, Lewis SC, Dennis MS (2006) No evidence that severity of stroke in internal carotid occlusion is related to collateral arteries. J Neurol Neurosurg Psychiatry 77:729–733
Meschia JF, Klaas JP, Brown RD, Brott TG (2017) Evaluation and management of atherosclerotic carotid stenosis. Mayo Clin Proc 92:1144–1157
Puech-Leão P, Wolosker N, Zerati AE, Nascimento LD (2011) Impact of endovascular technique in vascular surgery training at a large university hospital in Brazil. J Surg Educ 68:19–23
Queiroz ACS, de Albuquerque LG, Malik AM (2013) Gestão estratégica de pessoas e inovação: estudos de caso no contexto hospitalar. R Adm 48:658–670
Shean KE, McCallum JC, Soden PA, Deery SE, Schneider JR, Nolan BW, Rockman CB, Schermerhorn ML (2017) Regional variation in patient selection and treatment for carotid artery disease in the Vascular Quality Initiative. J Vasc Surg 66:112–121
Stabellini N, Wolosker N, Leiderman DBD, da Silva MFA, Nogueira WA, Amaro E, Teivelis MP (2020) Epidemiological analysis of carotid artery stenosis intervention during 10 years in the public health system in the largest city in Brazil: stenting has been more common than endarterectomy. Ann Vasc Surg 66:378–384
White CJ, Anderson HV, Brindis RG, Cates CU, Cohen DJ, Ho K, Hopkins LN, Jaff MR, Koroshetz WJ, Rosenfield KA (2008) The Carotid Artery Revascularization and Endarterectomy (CARE) registry: objectives, design, and implications. Catheter Cardiovasc Interv 71:721–725
Acknowledgements
We would like to thank Editage (www.editage.com) for the English language editing.
Author information
Authors and Affiliations
Contributions
Ideation of the article: Rodrigo Massaud/Nelson Wolosker/Gisele Silva
Data collection: Rodrigo Massaud/Andreia Vaccari
Statistical analysis: Marcelo Silva/Rodrigo Massaud
Manuscript writing: all authors
Manuscript review: all authors
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the Institutional Ethics Committee. The protocol used for patients was in accordance with the hospital’s ethical standards set by the Ethics Committee for Analysis of Research Projects on Human Experimentation.
Consent
Our study was exempted from the requirement for informed consent because it employed a secondary database with de-identified data. The responsible researcher is committed to data confidentiality.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Comments
This manuscript deserves to be published and needs to be studied by carotid treatment practitioners, surgery or endovascular both. The authors can demonstrate markedly superior outcomes from carotid treatment when best practice guidelines and standardization of decision-making are implemented. This particular series is from a hospital with an open medical staff, where standardization without guidelines may be more difficult and there is great variability in decision-making and technique. For those of us (like me) who have always practiced in an academic medical center with a closed staff, daily dialog with a close per group and close oversight of outcomes by neurologists serves much the same purpose. But the principle is the same; application of current data and best practices leads to superior patient outcomes—which should always be our objective.
If one closely reads the Appendix, one finds that we will not agree with every recommendation. For example, I personally do not believe in protamine reversal, with the belief that it may be implicated in some strokes, and likewise I do not agree that all patches are the same, since we have seen a higher rate of central patch rupture with autologous vein. These are just a few examples that I picked out. But these are small points, and probably we could find many such areas of minor disagreement without any real clinical consequence. We should instead look at the larger picture, that is, that application of contemporary scholarship and scrupulous adjudication of results is the best way to treat patients. For this advance, I commend these authors on their scholarly approach to the issue. We appreciate the comments and plan periodic revisions to the guideline.
Christopher M. Loftus
PA, USA
This article is part of the Topical Collection on Vascular Neurosurgery – Other
Institution where work was performed: Hospital Israelita Albert Einstein
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Massaud, R.M., da Silva, M.F.A., Vaccari, A.M.H. et al. Impact of implementing good care and management practice guidelines in carotid revascularization procedures. Acta Neurochir 164, 1047–1053 (2022). https://doi.org/10.1007/s00701-022-05111-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05111-2