Abstract
Background
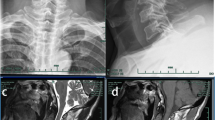
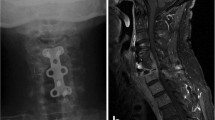
The combination of cervical spondylodiscitis and esophageal fistula is rare but life-threatening. Due to both the rarity of these conditions’ coincidence and the complexity and heterogeneity of individual cases, there is no optimal treatment or management approach. The aims of this study are to obtain an overview of patients’ outcomes and to discuss treatment options.
Method
This study is a retrospective analysis of patients who presented with cervical spondylodiscitis and associated esophageal fistula between January 2010 and November 2018. We examined reports of 59 patients who suffered from cervical spondylodiscitis and included nine patients (15.25%) who had an esophageal fistula as the underlying cause. We assessed clinical findings, treatment, and outcome.
Results
Three of the nine patients were female, and the mean age of the sample was 64.56 years. Six of the patients had a history of esophagopharyngeal cancer and had undergone tumor resection followed by radiotherapy. Two of the remaining patients’ fistulas were caused by an iatrogenic injury during cervical spine surgery and a swallowed toothpick; in the final case, the origin remained unclear. Five patients presented with tetraparesis or tetraplegia, and the other four patients were neurologically intact. In seven cases, dorsal instrumentation was initially performed. Three patients secondarily received a ventral approach for debridement, and one received explantation of the ventral implants. Two patients died during the hospital stay, and three were transferred to a palliative care unit. Thus, the spondylodiscitis and esophageal fistula were cured in only four patients. At discharge, two patients were neurologically intact, two others remained in tetraparesis.
Conclusions
Cervical spondylodiscitis in association with an esophageal fistula carries high morbidity and high mortality. Because patients whose infections are not cured have high morbidity, we recommend using interdisciplinary and individual management, including definite surgical treatment of the discitis and fistula, in every case.


Similar content being viewed by others
Abbreviations
- ENT:
-
Ear, nose, and throat
References
Benazzo M, Spasiano R, Bertino G, Occhini A, Gatti P (2008) Sternocleidomastoid muscle flap in esophageal perforation repair after cervical spine surgery: concepts, techniques, and personal experience. J Spinal Disord Tech 21:597–605. https://doi.org/10.1097/BSD.0b013e31815c5f96
Bernard L, Dinh A, Ghout I, Simo D, Zeller V, Issartel B, Le Moing V, Belmatoug N, Lesprit P, Bru JP, Therby A, Bouhour D, Denes E, Debard A, Chirouze C, Fevre K, Dupon M, Aegerter P, Mulleman D Duration of treatment for spondylodiscitis study g (2015) antibiotic treatment for 6 weeks versus 12 weeks in patients with pyogenic vertebral osteomyelitis: an open-label, non-inferiority, randomised, controlled trial. Lancet 385:875–882. https://doi.org/10.1016/S0140-6736(14)61233-2
Boulis NM, Armstrong WS, Chandler WF, Orringer MB (1999) Epidural abscess: a delayed complication of esophageal stenting for benign stricture. Ann Thorac Surg 68:568–570
Cheung WY, Luk KD (2012) Pyogenic spondylitis. Int Orthop 36:397–404. https://doi.org/10.1007/s00264-011-1384-6
Cheung JP, Wei WI, Luk KD (2013) Cervical spine complications after treatment of nasopharyngeal carcinoma. Eur Spine J 22:584–592. https://doi.org/10.1007/s00586-012-2600-9
Cheung JP, Mak KC, Tsang HH, Luk KD (2015) A lethal sequelae of spinal infection complicating surgery and radiotherapy for head and neck cancer. Asian Spine J 9:617–620. https://doi.org/10.4184/asj.2015.9.4.617
Cordero-Jimenez A, Tenor-Serrano R, Munoz-Palza C, Solano-Romero JR (2012) Spinal-esophageal fistula in a patient treated with concurrent chemotherapy and radiotherapy. Acta Otorrinolaringol Esp 63:241–243. https://doi.org/10.1016/j.otorri.2011.01.006
Feldmeier JJ (2012) Hyperbaric oxygen therapy and delayed radiation injuries (soft tissue and bony necrosis): 2012 update. Undersea Hyperb Med 39:1121–1139
Ghobrial GM, Franco D, Theofanis T, Margiotta PJ, Andrews E, Wilson JR, Harrop JS, Heller JE (2017) Cervical spondylodiscitis: presentation, timing, and surgical management in 59 patients. World Neurosurg 103:664–670. https://doi.org/10.1016/j.wneu.2017.04.119
Gouliouris T, Aliyu SH, Brown NM (2010) Spondylodiscitis: update on diagnosis and management. J Antimicrob Chemother 65(Suppl 3):iii11–iii24. https://doi.org/10.1093/jac/dkq303
Hanwright PJ, Purnell CA, Dumanian GA (2015) Flap reconstruction for esophageal perforation complicating anterior cervical spinal fusion: an 18-year experience. Plast Reconstr Surg Glob Open 3:e400. https://doi.org/10.1097/GOX.0000000000000350
Hershman SH, Kunkle WA, Kelly MP, Buchowski JM, Ray WZ, Bumpass DB, Gum JL, Peters CM, Singhatanadgige W, Kim JY, Smith ZA, Hsu WK, Nassr A, Currier BL, Rahman RK, Isaacs RE, Smith JS, Shaffrey C, Thompson SE, Wang JC, Lord EL, Buser Z, Arnold PM, Fehlings MG, Mroz TE, Riew KD (2017) Esophageal perforation following anterior cervical spine surgery: case report and review of the literature. Glob Spine J 7:28S–36S. https://doi.org/10.1177/2192568216687535
Heyboer M 3rd, Sharma D, Santiago W, McCulloch N (2017) Hyperbaric oxygen therapy: side effects defined and quantified. Adv Wound Care (New Rochelle) 6:210–224. https://doi.org/10.1089/wound.2016.0718
Iannettoni MD, Whyte RI, Orringer MB (1995) Catastrophic complications of the cervical esophagogastric anastomosis. J Thorac Cardiovasc Surg 110:1493–1500; discussion 1500-1491. https://doi.org/10.1016/S0022-5223(95)70072-2
Kakuta T, Kosugi S, Kanda T, Hatakeyama K (2010) Purulent spondylitis related to anastomotic fistula after esophageal cancer surgery. Interact Cardiovasc Thorac Surg 11:204–206. https://doi.org/10.1510/icvts.2010.235515
Lemaignen A, Ghout I, Dinh A, Gras G, Fantin B, Zarrouk V, Carlier R, Loret JE, Denes E, Greder A, Lescure FX, Boutoille D, Tattevin P, Issartel B, Cottier JP, Bernard L, group DTSs (2017) Characteristics of and risk factors for severe neurological deficit in patients with pyogenic vertebral osteomyelitis: a case-control study. Medicine (Baltimore) 96:e6387. https://doi.org/10.1097/MD.0000000000006387
Metcalfe S, Morgan-Hough C (2009) Cervical epidural abscess and vertebral osteomyelitis following non-traumatic oesophageal rupture: a case report and discussion. Eur Spine J 18(Suppl 2):224–227. https://doi.org/10.1007/s00586-009-0889-9
Mishra B, Singhal S, Aggarwal D, Kumar N, Kumar S (2015) Non operative management of traumatic esophageal perforation leading to esophagocutaneous fistula in pediatric age group: review and case report. World J Emerg Surg 10:19. https://doi.org/10.1186/s13017-015-0012-y
Navarro R, Javahery R, Eismont F, Arnold DJ, Bhatia NN, Vanni S, Levi AD (2005) The role of the sternocleidomastoid muscle flap for esophageal fistula repair in anterior cervical spine surgery. Spine (Phila Pa 1976) 30:E617–E622
Petri NM, Mestrovic J, Andric D, Krzelj V, Stipancevic H (2003) Esophagotracheal fistula after lithium disc battery ingestion successfully treated with hyperbaric oxygen therapy. Int J Pediatr Otorhinolaryngol 67:921–926
Sealy WC (1963) Rupture of the esophagus. Am J Surg 105:505–510
Shiban E, Janssen I, Wostrack M, Krieg SM, Ringel F, Meyer B, Stoffel M (2014) A retrospective study of 113 consecutive cases of surgically treated spondylodiscitis patients. A single-center experience. Acta Neurochir 156:1189–1196. https://doi.org/10.1007/s00701-014-2058-0
Shiban E, Janssen I, da Cunha PR, Rainer J, Stoffel M, Lehmberg J, Ringel F, Meyer B (2016) Safety and efficacy of polyetheretherketone (PEEK) cages in combination with posterior pedicel screw fixation in pyogenic spinal infection. Acta Neurochir 158:1851–1857. https://doi.org/10.1007/s00701-016-2924-z
van Berge Henegouwen DP, Roukema JA, de Nie JC, vd Werken C (1991) Esophageal perforation during surgery on the cervical spine. Neurosurgery 29:766–768
Yuan H, Ding H, Hu L, Buser Z, Zhao H, Li X (2017) Treatment for early postoperative esophageal fistula complicated with anterior cervical surgery. J Orthop Surg (Hong Kong) 25:2309499016684418. https://doi.org/10.1177/2309499016684418
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The Ethics Committee approved this study (No. 238/17S). For this type of study, formal consent is not required, because all patients signed forms consenting to allow the clinic to store and analyze their data, tissue and blood samples for scientific purposes.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Infection
Rights and permissions
About this article
Cite this article
Janssen, I., Shiban, E., Rienmüller, A. et al. Treatment considerations for cervical and cervicothoracic spondylodiscitis associated with esophageal fistula due to cancer history or accidental injury: a 9-patient case series. Acta Neurochir 161, 1877–1886 (2019). https://doi.org/10.1007/s00701-019-03985-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-019-03985-3