Abstract
Background
Long-term dopamine agonist (DA) therapy is recommended as a first-line approach for the management of microprolactinomas. However, DA therapy may be poorly tolerated by some patients, and therefore some patients continue to prefer surgery over DA therapy.
Aim
The aim of our study was to evaluate factors associated with favorable outcomes after surgical treatment of microprolactinomas in women.
Methods
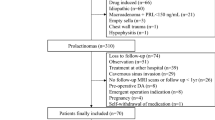
Thirty-two women (mean age 31.0 ± 8.2 years) with confirmed microprolactinomas who were operated using transsphenoidal approach were included to the study. Twenty-two (61 %) women had previous DA therapy and ten (39 %) women preferred surgery as a first treatment. Mean follow-up was 4.2 ± 2.7 years. Surgery was considered to be effective and remission achieved if serum prolactin was normal without DA therapy and there were no signs of tumor re-growth on neuroimaging.
Results
Nine (47.4 %) patients in whom remission was achieved did not receive preoperative DA therapy when compared to one (7.7 %) patient in whom remission was not achieved (p = 0.02). Remission after operation was achieved in nine out of ten (90 %) patients who did not receive DA therapy compared to ten out of 22 patients (45.5 %) who were treated with DAs (p = 0.01). The independent factor associated with good outcome following surgical treatment was no preoperative DA therapy (RR = 14.57 (1.43–148.1), p = 0.02). Surgical complications were permanent diabetes insipidus in two patients (6.3 %) and transient DI in five (15.6 %) patients.
Conclusions
The main factor associated with favorable microprolactinoma surgery outcome in women was the absence of preoperative DA therapy.
Similar content being viewed by others
References
Acharya V (2004) Review of pregnancy reports in patients on pergolide treatment. Eli Lilly, Co., Indianapolis
Amar AP, Couldwell WT, Chen JCT, Weiss MH (2002) Predictive value of serum prolactin levels measured immediately after transsphenoidal surgery. J Neurosurg 97:307–314
Casanueva FF, Molitch ME, Schlechte JA, Abs R, Bonert V, Bronstein MD, Brue T, Cappabianca P, Colao A, Fahlbusch R, Fideleff H, Hadani M, Kelly P, Kleinberg D, Laws E, Marek J, Scanlon M, Sobrinho LG, Wass JA, Giustina A (2006) Guidelines of the Pituitary Society for the diagnosis and management of prolactinomas. Clin Endocrinol 65:265–273
Couldwell WT, Rovit RL, Weiss MH (2003) Role of surgery in the treatment of microprolactinomas. Neurosurg Clin N Am 14:89–92
Gillam MP, Molitch ME, Lombardi G, Colao A (2006) Advances in the treatment of prolactinomas. Endocrinol Rev 27:485–534
Guieu R, Dufour H, Grisoli F, Jaquet P, Guieu Y, Rosso JP, Munier M, Dicostanzo V, Brue T, Enjalbert A, Begoud D, Rochat H (1999) An ultrarapid prognostic index in microprolactinoma surgery. J Neurosurg 90:1037–1041
Hamilton DK, Vance ML, Boulos PT, Laws ER (2005) Surgical outcoms in hyporesponsive prolactinomas: analysis of patients with resistance or intolerance to dopamine agonists. Pituitary 8(1):53–60
Horvath J, Fross RD, Kleiner-Fisman G, Lerch R, Stalder H, Liaudat S, Raskoff WJ, Flachsbart KD, Rakowski H, Pache JC, Burkhard PR, Lang AE (2004) Severe multivalvular heart disease: a new complication of the ergot derivate dopamine agonists. Mov Disord 19:656–662
Kissner DG, Jarrett JC (1980) Side effects of bromocriptine. N Engl J Med 302:749–750
Kreutzer J, Buslei R, Wallaschofski H, Hofmann B, Nimsky C, Fahlbusch R, Buchfelder M (2008) Operative treatment of prolactinomas: indications and results in a current consecutive series of 212 patients. Eur J Endocrinol 158:11–18
Landolt AM, Keller PJ, Froesch ER, Mueller J (1982) Bromocriptine: does it jeopardise the result of later surgery for prolactinomas? Lancet 2:657–658
Losa M, Mortini P, Barzaghi R, Giola I, Giovanelli M (2002) Surgical treatment of prolactin-secreting pituitary adenomas: early results and long-term outcome. J Clin Endocrinol Metab 87:3180–3186
Molitch ME (2002) Medical management of prolactin-secreting pituitary adenomas. Pituitary 5:55–65
Pan L, Zhang N, Wang EM, Wang BJ, Dai JZ, Cai PW (2000) Gamma knife radiosurgery as primary treatment for prolactinomas. J Neurosurg 93(Suppl 3):10–13
Pinero A, Marcos-Alberca P, Fortes J (2005) Cabergoline-related severe restrictive mitral regurgitation. N Engl J Med 353:1976–1977
Rains CP, Bryson HM, Cabergoline FA (1995) A review of its pharmacological properties and therapeutic potential in the treatment of hyperprolactinaemia and inhibition of lactation. Drugs 49:255–279
Raymond JP, Goldstein E, Konopka P, Leleu MF, Merceron RE, Loria Y (1985) Follow-up of children born of bromocriptine-treated mothers. Horm Res 22:239–246
Serri O, Rasio E, Beauregard H, Hardy J, Somma M (1983) Recurrence of hyperprolactinemia after selective transsphenoidal adenectomy in women with prolactinoma. N Engl J Med 309:280–282
Shristava RK, Arginteanu MS, King WA, Port KD (2002) Giant prolactinomas: clinical management and long-term follow up. J Neurosurg 97:299–306
Sughrue ME, Chang EF, Tyrell JB, Kunwar S, Wilson CB, Blevins LS Jr (2009) Pre-operative dopamine agonist therapy improves post-operative tumor control following prolactinoma resection. Pituitary 12:158–164
Turner HE, Adams CB, Wass JA (1999) Trans-sphenoidal surgery for microprolactinoma: an acceptable alternative to dopamin agonists? Eur J Endocrinol 140:43–47
Thomson JA, Davies DL, McLaren EH, Teasdale GM (1994) Ten year follow-up of microprolactinoma treated by transsphenoidal surgery. BMJ 309:1409
Tyrell JB, Lamborn KR, Hannegan LT, Applebury CB, Wilson CB (1999) Transsphenoidal microsurgical therapy of prolactinomas: initial outcomes and long-term results. Neurosurgery 44:254–261
Wang MY, Weiss MH (2001) Is there a role for surgery for microprolactinomas? Semin Neurosurg 12:289–294
Webster J (1996) A comparative review of the tolerability profiles of dopamin agonists in the treatment of hyperprolactinaemia and inhibition of lactation. Drug Saf 14:228–238
Webster J, Piscitelli G, Polli A, Cl F, Ismail I, Scanlon MF (1994) A comparison of cabergoline and bromocriptine in the treatment of hyperprolactinaemic amenorrhea. Cabergoline Comparative Study Group. N Engl J Med 331:904–909
Zada G, Kelly DF, Cohan P, Wang C, Swerdloff R (2003) Endonasal transsphenoidal approach for pituitary adenomas and other sellar lesions: an assessment of efficacy, safety, and patient impressions. J Neurosurg 98:350–358
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tamasauskas, A., Sinkunas, K., Bunevicius, A. et al. Transsphenoidal surgery for microprolactinomas in women: results and prognosis. Acta Neurochir 154, 1889–1893 (2012). https://doi.org/10.1007/s00701-012-1450-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-012-1450-x