Abstract
The instant screening of patients with a tendency towards developing Alzheimer’s disease (AD) is significant for providing preventive measures and treatment. However, the current imaging-based technology cannot meet the requirements in the early stage. Developing biosensor-based liquid biopsy technology could be overcoming this bottleneck problem. Herein, we developed a simple, low-cost, and sensitive electrochemical aptamer biosensor for detecting phosphorylated tau protein threonine 231 (P-tau231), the earliest and one of the most efficacious abnormally elevated biomarkers of AD. Gold nanoparticles (AuNPs) were electrochemically synthesized on a glassy carbon electrode as the transducer, exhibiting excellent conductivity, and were applied to amplify the electrochemical signal. A nucleic acid aptamer was designed as the receptor to capture the P-tau231 protein, specifically through the formation of an aptamer-antigen complex. The proposed biosensor showed excellent sensitivity in detecting P-tau 231, with a broad linear detection range from 10 to 107 pg/mL and a limit of detection (LOD) of 2.31 pg/mL. The recoveries of the biosensor in human serum ranged from 97.59 to 103.26%, demonstrating that the biosensor could be used in complex practical samples. In addition, the results showed that the developed biosensor has good repeatability, reproducibility, and stability, which provides a novel method for the early screening of AD.
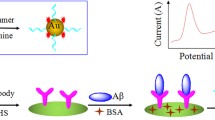
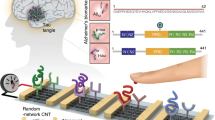
Graphical Abstract







Similar content being viewed by others
Data availability
The data in our study are available from the corresponding author upon reasonable request.
Abbreviations
- AD :
-
Alzheimer’s disease
- P-tau231 :
-
Phosphorylated tau protein threonine 231
- LOD :
-
Limit of detection
- P-tau181 :
-
Phosphorylated tau protein threonine 181
- P-tau217 :
-
Phosphorylated tau protein threonine 217
- CSF :
-
Cerebrospinal fluid
- Aβ :
-
β-Amyloid
- PET-CT :
-
Positron Emission Tomography-Computed Tomography
- MCH :
-
6-Mercapto-1-hexanol
- BSA :
-
Bovine serum albumin
- GCE :
-
Glassy carbon electrode
- SEM :
-
Scanning electron microscopy
- EDS :
-
Energy-dispersive X-ray spectroscopy
- CV :
-
Cyclic voltammetry
- DPV :
-
Differential pulse voltammetry
- EIS :
-
Electrochemical impedance spectroscopy
- PBS :
-
Phosphate-buffered saline
- CA19-9 :
-
Cancer antigen 19–9
- RSD :
-
Relative standard deviation
References
Scheltens P, De Strooper B, Kivipelto M et al (2021) Alzheimer’s disease. The Lancet 397:1577–1590. https://doi.org/10.1016/S0140-6736(20)32205-4
Jia L, Du Y, Chu L et al (2020) Prevalence, risk factors, and management of dementia and mild cognitive impairment in adults aged 60 years or older in China: a cross-sectional study. Lancet Public Health 5:e661–e671. https://doi.org/10.1016/S2468-2667(20)30185-7
Ren R, Qi J, Lin S et al (2022) The China Alzheimer Report 2022. Gen Psychiatry 35:e100751. https://doi.org/10.1136/gpsych-2022-100751
(2023) 2023 Alzheimer’s disease facts and figures. Alzheimers Dement 19:1598–1695. https://doi.org/10.1002/alz.13016
Venkatramani A, Panda D (2019) Regulation of neuronal microtubule dynamics by tau: implications for tauopathies. Int J Biol Macromol 133:473–483. https://doi.org/10.1016/j.ijbiomac.2019.04.120
Puzzo D, Privitera L, Leznik E et al (2008) Picomolar amyloid-β positively modulates synaptic plasticity and memory in hippocampus. J Neurosci 28:14537–14545. https://doi.org/10.1523/JNEUROSCI.2692-08.2008
Pluta R, Ouyang L, Januszewski S et al (2021) Participation of amyloid and tau protein in post-ischemic neurodegeneration of the hippocampus of a nature identical to Alzheimer’s disease. Int J Mol Sci 22:2460. https://doi.org/10.3390/ijms22052460
Therriault J, Vermeiren M, Servaes S et al (2023) Association of phosphorylated tau biomarkers with amyloid positron emission tomography vs tau positron emission tomography. JAMA Neurol 80:188. https://doi.org/10.1001/jamaneurol.2022.4485
Gonzalez MC, Ashton NJ, Gomes BF et al (2022) Association of plasma p-tau181 and p-tau231 concentrations with cognitive decline in patients with probable dementia with Lewy bodies. JAMA Neurol 79:32. https://doi.org/10.1001/jamaneurol.2021.4222
Suárez-Calvet M, Karikari TK, Ashton NJ et al (2020) Novel tau biomarkers phosphorylated at T181, T217 or T231 rise in the initial stages of the preclinical Alzheimer’s continuum when only subtle changes in Aβ pathology are detected. EMBO Mol Med 12:e12921. https://doi.org/10.15252/emmm.202012921
Neddens J, Temmel M, Flunkert S et al (2018) Phosphorylation of different tau sites during progression of Alzheimer’s disease. Acta Neuropathol Commun 6:52. https://doi.org/10.1186/s40478-018-0557-6
Handels RLH, Wolfs CAG, Aalten P et al (2014) Diagnosing Alzheimer’s disease: a systematic review of economic evaluations. Alzheimers Dement 10:225–237. https://doi.org/10.1016/j.jalz.2013.02.005
Chatterjee P, Pedrini S, Ashton NJ et al (2022) Diagnostic and prognostic plasma biomarkers for preclinical Alzheimer’s disease. Alzheimers Dement 18:1141–1154. https://doi.org/10.1002/alz.12447
Ashton NJ, Janelidze S, Mattsson-Carlgren N et al (2022) Differential roles of Aβ42/40, p-tau231 and p-tau217 for Alzheimer’s trial selection and disease monitoring. Nat Med 28:2555–2562. https://doi.org/10.1038/s41591-022-02074-w
Kiđemet-Piskač S, Babić Leko M, Blažeković A et al (2018) Evaluation of cerebrospinal fluid phosphorylated tau 231 as a biomarker in the differential diagnosis of Alzheimer’s disease and vascular dementia. CNS Neurosci Ther 24:734–740. https://doi.org/10.1111/cns.12814
Ashton NJ, Puig‐Pijoan A, Milà‐Alomà M, et al (2022) Plasma and CSF biomarkers in a memory clinic: head‐to‐head comparison of phosphorylated tau immunoassays. Alzheimers Dement alz.12841. https://doi.org/10.1002/alz.12841
Milà-Alomà M, Ashton NJ, Shekari M et al (2022) Plasma p-tau231 and p-tau217 as state markers of amyloid-β pathology in preclinical Alzheimer’s disease. Nat Med. https://doi.org/10.1038/s41591-022-01925-w
Meyer P, Ashton NJ, Karikari TK et al (2022) Plasma p-tau231, p-tau181, PET biomarkers, and cognitive change in older adults. Ann Neurol 91:548–560. https://doi.org/10.1002/ana.26308
Gonzalez-Ortiz F, Kac PR, Brum WS et al (2023) Plasma phospho-tau in Alzheimer’s disease: towards diagnostic and therapeutic trial applications. Mol Neurodegener 18:18. https://doi.org/10.1186/s13024-023-00605-8
Chen L, Niu X, Wang Y et al (2022) Plasma tau proteins for the diagnosis of mild cognitive impairment and Alzheimer’s disease: a systematic review and meta-analysis. Front Aging Neurosci 14:942629. https://doi.org/10.3389/fnagi.2022.942629
Ashton NJ, Benedet AL, Pascoal TA et al (2022) Cerebrospinal fluid p-tau231 as an early indicator of emerging pathology in Alzheimer’s disease. BioMedicine 76:103836. https://doi.org/10.1016/j.ebiom.2022.103836
Ashton NJ, Pascoal TA, Karikari TK et al (2021) Plasma p-tau231: a new biomarker for incipient Alzheimer’s disease pathology. Acta Neuropathol (Berl) 141:709–724. https://doi.org/10.1007/s00401-021-02275-6
Graff-Radford J, Yong KXX, Apostolova LG, et al (2021) New insights into atypical Alzheimer’s disease in the era of biomarkers. Lancet Neurol 20:222–234. https://doi.org/10.1016/S1474-4422(20)30440-3
Kac PR, Gonzalez-Ortiz F, Simrén J et al (2022) Diagnostic value of serum versus plasma phospho-tau for Alzheimer’s disease. Alzheimers Res Ther 14:65. https://doi.org/10.1186/s13195-022-01011-w
Montoliu-Gaya L, Benedet AL, Tissot C et al (2023) Mass spectrometric simultaneous quantification of tau species in plasma shows differential associations with amyloid and tau pathologies. Nat Aging 3:661–669. https://doi.org/10.1038/s43587-023-00405-1
Soares JC, Soares AC, Rodrigues VC et al (2019) Detection of the prostate cancer biomarker PCA3 with electrochemical and impedance-based biosensors. ACS Appl Mater Interfaces 11:46645–46650. https://doi.org/10.1021/acsami.9b19180
Kinghorn A, Fraser L, Liang S et al (2017) Aptamer bioinformatics. Int J Mol Sci 18:2516. https://doi.org/10.3390/ijms18122516
Campuzano S, Yáñez-Sedeño P, Pingarrón JM (2019) Nanoparticles for nucleic-acid-based biosensing: opportunities, challenges, and prospects. Anal Bioanal Chem 411:1791–1806. https://doi.org/10.1007/s00216-018-1273-6
Wehmeyer KR, White RJ, Kissinger PT, Heineman WR (2021) Electrochemical affinity assays/sensors: brief history and current status. Annu Rev Anal Chem 14:109–131. https://doi.org/10.1146/annurev-anchem-061417-125655
Xu Y, Wang X, Ding C, Luo X (2021) Ratiometric antifouling electrochemical biosensors based on multifunctional peptides and MXene loaded with Au nanoparticles and methylene blue. ACS Appl Mater Interfaces 13:20388–20396. https://doi.org/10.1021/acsami.1c04933
Xiao T, Huang J, Wang D et al (2020) Au and Au-based nanomaterials: synthesis and recent progress in electrochemical sensor applications. Talanta 206:120210. https://doi.org/10.1016/j.talanta.2019.120210
Phan LMT, Cho S (2022) Fluorescent aptasensor and colorimetric aptablot for p-tau231 detection: toward early diagnosis of Alzheimer’s disease. Biomedicines 10:93. https://doi.org/10.3390/biomedicines10010093
Teng I-T, Li X, Yadikar HA et al (2018) Identification and characterization of DNA aptamers specific for phosphorylation epitopes of tau protein. J Am Chem Soc 140:14314–14323. https://doi.org/10.1021/jacs.8b08645
Wang W, Liu Y, Shi T et al (2020) Biosynthesized quantum dot for facile and ultrasensitive electrochemical and electrochemiluminescence immunoassay. Anal Chem 92:1598–1604. https://doi.org/10.1021/acs.analchem.9b04919
Le HTN, Cho S (2021) Sensitive electrochemical detection of phosphorylated-tau threonine 231 in human serum using interdigitated wave-shaped electrode. Biomedicines 10:10. https://doi.org/10.3390/biomedicines10010010
Acknowledgements
We thanked Biorender (https://www.biorender.com/) for their high-quality artwork. We thanked Grammarly (https://app.grammarly.com/) for correction of grammatical errors and improvements to readability.
Funding
The study was supported by the National Natural Science Foundation of China (82030065 to Prof. Qin Zhou, 82102502 to Prof. Feiyun Cui, and 82071833 to Prof. Qingfei Kong).
Author information
Authors and Affiliations
Contributions
Methodology: Qingfei Kong, Chunhan Liu, and Yanlin Zhang; writing—original draft preparation: Chunhan Liu; formal analysis and writing—review and editing: Yifan He and Ruiting Zhang; investigation: Yuhan Wang; conceptualization, funding acquisition, resources, and supervision: Feiyun Cui, Qin Zhou, and Qingfei Kong; all authors contributed to the article.
Corresponding authors
Ethics declarations
Consent for publication
All authors contributed to the article and approved the submitted version.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kong, Q., Liu, C., Zhang, Y. et al. Nucleic acid aptamer-based electrochemical sensor for the detection of serum P-tau231 and the instant screening test of Alzheimer’s disease. Microchim Acta 191, 328 (2024). https://doi.org/10.1007/s00604-024-06395-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00604-024-06395-0