Abstract
Purpose
Clinically relevant postoperative pancreatic fistulas (CR-POPF) occurring after distal pancreatectomy often cause intra-abdominal infections. We monitored the presence of bacterial contamination in the ascitic fluid after distal pancreatectomy to clarify the bacterial origin of intra-abdominal infections associated with CR-POPF.
Methods
In 176 patients who underwent distal pancreatectomy, ascitic fluid bacterial cultures were performed on postoperative days (POD) 1–4 and when the drainage fluid became turbid. The association between postoperative ascitic bacterial contamination and CR-POPF incidence was investigated.
Results
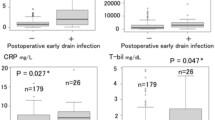
CR-POPF occurred in 18 cases (10.2%). Among the patients with CR-POPF, bacterial contamination was detected in 0% on POD 1, in 38.9% on POD 4, and in 72.2% on the day (median, day 9.5) when the drainage fluid became turbid. A univariate analysis revealed a significant difference in ascitic bacterial contamination on POD 4 (p < 0.001) and amylase level on POD 3–4 (p < 0.001). A multivariate analysis revealed the amylase level and ascitic bacterial contamination on POD 4 to be independent risk factors.
Conclusions
In the CR-POPF group, ascitic bacterial contamination was not observed in the early postoperative stage, but the bacterial contamination rate increased after pancreatic juice leakage occurred. Therefore, CR-POPF-related infections in distal pancreatectomy may be caused by a retrograde infection of pancreatic juice.
Similar content being viewed by others
References
Ohgi K, Sugiura T, Yamamoto Y, Okamura Y, Ito T, Uesaka K. Bacterobilia may trigger the development and severity of pancreatic fistula after pancreatoduodenectomy. Surgery. 2016;160:725–30.
Nagakawa Y, Matsudo T, Hijikata Y, Kikuchi S, Bunso K, Suzuki Y, et al. Bacterial contamination in ascitic fluid is associated with the development of clinically relevant pancreatic fistula after pancreatoduodenectomy. Pancreas. 2013;42:701–6.
Yamashita K, Kato D, Sasaki T, Shiwaku H, Ishii F, Naito S, et al. Contaminated drainage fluid and pancreatic fistula after pancreatoduodenectomy: a retrospective study. Int J Surg. 2018;52:314–9.
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery. 2016;161:584–91.
Kitahata Y, Kawai M, Tani M, Hirono S, Okada K, Miyazawa M, et al. Preoperative cholangitis during biliary drainage increases the incidence of postoperative severe complications after pancreaticoduodenectomy. Am J Surg. 2014;208:1–10.
Akashi M, Nagakawa Y, Hosokawa Y, Takishita C, Osakabe H, Nishino H, et al. Preoperative cholangitis is associated with increased surgical site infection following pancreaticoduodenectomy. J Hepatobiliary Pancreat Sci. 2020;27:640–7.
Sivaraj SM, Vimalraj V, Saravanaboopathy P, Rajendran S, Jeswanth S, Ravichandran P, et al. Is bactibilia a predictor of poor outcome of pancreaticoduodenectomy? Hepatobiliary Pancreat Dis Int. 2010;9:65–8.
Kawaida H, Kono H, Watanabe M, Hosomura N, Amemiya H, Fujii H. Risk factors of postoperative pancreatic fistula after distal pancreatectomy using a triple-row stapler. Surg Today. 2018;48:95–100.
Ecker BL, McMillan MT, Allegrini V, Bassi C, Beane JD, Beckman RM, et al. Risk factors and mitigation strategies for pancreatic fistula after distal pancreatectomy: analysis of 2026 resections from the international, multi-institutional distal pancreatectomy study group. Ann Surg. 2019;269:143–9.
Nagakawa Y, Hijikata Y, Osakabe H, Matsudo T, Soya R, Sahara Y, et al. Why does postoperative pancreatic fistula occur after hand-sewn parenchymal closure and staple closure in distal pancreatectomy? Surg Laparosc Endosc Percutan Tech. 2019;29:e15–9.
Povoski SP, Karpeh MS Jr, Conlon KC, Blumgart LH, Brennan MF. Association of preoperative biliary drainage with postoperative outcome following pancreaticoduodenectomy. Ann Surg. 1999;230:131–42.
Lankelma JM, Nieuwdorp M, de Vos WM, Wiersinga WJ. The gut microbiota in internal medicine: implications for health and disease. Neth J Med. 2015;73:61–8.
Nagakawa Y, Tsuchida A, Saito H, Tohyama Y, Matsudo T, Kawakita H, et al. The VIO soft-coagulation system can prevent pancreatic fistula following pancreatectomy. J Hepatobiliary Pancreat Surg. 2008;15:359–65.
Tjaden C, Hinz U, Hassenpflug M, Fritz F, Fritz S, Grenacher L, et al. Fluid collection after distal pancreatectomy: a frequent finding. HPB (Oxford). 2016;18:35–40.
Nahm CB, de Reuver PR, Hugh TJ, Pearson A, Gill AJ, Samra JS, et al. Intra-operative amylase concentration in peri-pancreatic fluid predicts pancreatic fistula after distal pancreatectomy. J Gastrointest Surg. 2017;21:1031–7.
Marchegiani G, Perri G, Pulvirenti A, Sereni E, Azzini AM, Malleo G, et al. Non-inferiority of open passive drains compared with closed suction drains in pancreatic surgery outcomes: a prospective observational study. Surgery. 2018;164:443–9.
Yang F, Jin C, Hao S, Fu D. Drain contamination after distal pancreatectomy: incidence, risk factors, and association with postoperative pancreatic fistula. J Gastrointest Surg. 2019;23:2449–58.
Acknowledgements
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Osakabe, H., Nagakawa, Y., Kozono, S. et al. Causative bacteria associated with a clinically relevant postoperative pancreatic fistula infection after distal pancreatectomy. Surg Today 51, 1813–1818 (2021). https://doi.org/10.1007/s00595-021-02287-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-021-02287-5