Abstract
Purpose
We evaluated the perioperative inflammatory mediators in a right hemicolectomy performed with single-incision laparoscopic surgery (SILS) and traditional multi-port laparoscopic surgery (MLS) to compare the postoperative inflammatory response and feasibility of SILS with that of MLS.
Methods
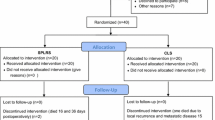
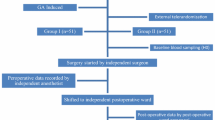
In this retrospective study, we enrolled 56 consecutive colorectal cancer patients who underwent right hemicolectomy prospectively. Twenty patients underwent SILS, and 36 underwent MLS. The preoperative and postoperative levels of plasma vascular endothelial growth factor (VEGF), serum interleukin-6 (IL-6), and C-reactive protein (CRP) as well as the number of platelet cells were measured in all patients. The operation duration, number of harvested lymph nodes, length of the resected bowel, blood loss, and duration of hospital stay were also compared between the two groups.
Results
Neither SILS nor MLS had any conversion cases. The operation duration was longer for MLS than for SILS. Blood loss tended to be lower among patients who underwent SILS than among those who underwent MLS. However, the number of harvested LNs was significantly lower with SILS than with MLS. In both pre- and postoperative blood examinations, there was no marked difference in inflammatory mediators between MLS and SILS.
Conclusion
There was no systemic inflammatory advantage associated with SILS compared with MLS.




Similar content being viewed by others
Data availability
The patients’ clinical data used to support the findings of this study have not been made available because of the patients’ privacy.
References
Chen WT, Chang SC, Chiang HC, Lo WY, Jeng LB, Wu C, Ke TW. Single-incision laparoscopic versus conventional laparoscopic right hemicolectomy: a comparison of short-term surgical results. Surg Endosc. 2011;25:1887–92.
Hiraki M, Takemasa I, Uemura M, Haraguchi N, Nishimura J, Hata T, Mizushima T, Yamamoto H, Doki Y, Mori M. Evaluation of invasiveness in single-site laparoscopic colectomy, using “the PainVision system” for quantitative analysis of pain sensation. Surg Endosc. 2014;28:3216–23.
Keshava A, Young CJ, Richardson GL, De-Loyde K. A historical comparison of single incision and conventional multiport laparoscopic right hemicolectomy. Colorectal Dis. 2013;15:e618–22.
Ramos-Valadez DI, Patel CB, Ragupathi M, Bartley Pickron T, Haas EM. Single-incision laparoscopic right hemicolectomy: safety and feasibility in a series of consecutive cases. Surg Endosc. 2010;24:2613–6.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M. The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–96.
Esposito C. One-trocar appendectomy in pediatric surgery. Surg Endosc. 1998;12:177–8.
Navarra G, Pozza E, Occhionorelli S, Carcoforo P, Donini I. One-wound laparoscopic cholecystectomy. Br J Surg. 1997;84:695.
Piskun G, Rajpal S. Transumbilical laparoscopic cholecystectomy utilizes no incisions outside the umbilicus. J Laparoendosc Adv Surg Tech Part A. 1999;9:361–4.
Chen CW, Hsiao KH, Chang YJ, Lai CW. (2013) Single-incision laparoscopic surgery using a homemade transumbilical port for synchronous colon and hepatic lesions: a case report. Surg Laparosc Endosc Percutaneous Tech 23:e164–167.
Curro G, Cogliandolo A, Lazzara S, La Malfa G, Navarra G. Single-incision versus three-port conventional laparoscopic right hemicolectomy: is there any real need to go single? J Laparoendosc Adv Surg Tech Part A. 2012;22:621–4.
Chew MH, Chang MH, Tan WS, Wong MT, Tang CL. Conventional laparoscopic versus single-incision laparoscopic right hemicolectomy: a case cohort comparison of short-term outcomes in 144 consecutive cases. Surg Endosc. 2013;27:471–7.
Lim SW, Kim HR, Kim YJ. Single incision laparoscopic colectomy for colorectal cancer: comparison with conventional laparoscopic colectomy. Ann Surg Treat Res. 2014;87:131–8.
Mufty H, Hillewaere S, Appeltans B, Houben B. Single-incision right hemicolectomy for malignancy: a feasible technique with standard laparoscopic instrumentation. Colorectal Dis. 2012;14:e764–70.
Su Y, Wu, Kong J, Yu H, Fan Y, Tian Y. Single incision laparoscopic colorectal surgery using conventional laparoscopic instruments: initial experience with 44 cases. J Investig Surg. 2015.
Chambers WM, Bicsak M, Lamparelli M, Dixon AR. Single-incision laparoscopic surgery (SILS) in complex colorectal surgery: a technique offering potential and not just cosmesis. Colorectal Dis. 2011;13:393–8.
Stage JG, Schulze S, Moller P, Overgaard H, Andersen M, Rebsdorf-Pedersen VB, Nielsen HJ. Prospective randomized study of laparoscopic versus open colonic resection for adenocarcinoma. Br J Surg. 1997;84:391–6.
Harmon GD, Senagore AJ, Kilbride MJ, Warzynski MJ. Interleukin-6 response to laparoscopic and open colectomy. Dis Colon Rectum. 1994;37:754–9.
Pascual M, Alonso S, Salvans S, Mayol X, Mojal S, Gil MJ, Grande L, Pera M. Postoperative serum vascular endothelial growth factor is an independent prognostic factor of disease free survival and overall survival in patients with non metastatic colon cancer. Am J Surg. 2018;216:255–9.
Luna RA, Nogueira DB, Varela PS, Rodrigues Neto Ede O, Norton MJ, Ribeiro Ldo C, Peixoto AM, de Mendonca YL, Bendet I, Fiorelli RA, Dolan JP. A prospective, randomized comparison of pain, inflammatory response, and short-term outcomes between single port and laparoscopic cholecystectomy. Surg Endosc. 2013;27:1254–9.
Ypsilantis P, Didilis V, Tsigalou C, Pitiakoudis M, Karakatsanis A, Margioulas A, Simopoulos C. Systemic inflammatory response after single-incision laparoscopic surgery versus standard laparoscopic approach. Surg Laparosc Endosc Percutaneous Tech. 2012;22:21–4.
Froghi F, Sodergren MH, Wright VJ, Coomber R, Courtney AP, Darzi A, Paraskeva P. Single-center experience in systemic stress and short-term morbidity of single-incision cholecystectomy. Surg Innov. 2012;19:117–22.
Sohn DK, Jeong SY, Park JW, Kim JS, Hwang JH, Kim DW, Kang SB, Oh JH. Comparative study of NOTES rectosigmoidectomy in a swine model: E-NOTES vs. P-NOTES. Endoscopy. 2011;43:526–32.
Wolthuis AM, Fieuws S, Van Den Bosch A, de Buck van Overstraeten A, D’Hoore A. Randomized clinical trial of laparoscopic colectomy with or without natural-orifice specimen extraction. Br J Surg. 2015;102:630–7.
Guo J, Pasricha NP, Shenoy MM, Liu L, Mehta K, Pasricha PJ. Transgastric versus laparoendoscopic single-site peritoneoscopy in a rat model: effects on motility, inflammation, and nociception. Surg Endosc. 2012;26:747–53.
Funding
Nothing to declare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest regarding the publication of this paper.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hara, M., Shiga, K., Yanagita, T. et al. No inflammatory benefit obtained by single-incision laparoscopic surgery for right hemicolectomy compared with conventional laparoscopy. Surg Today 49, 621–628 (2019). https://doi.org/10.1007/s00595-019-01777-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-019-01777-x