Abstract
Background
Single-site laparoscopic colectomy (SLC) is increasingly performed for colon cancer. There are few reports on invasiveness in SLC. This study aimed to evaluate the postoperative pain from SLC, as compared to conventional multiport laparoscopic colectomy (MLC).
Methods
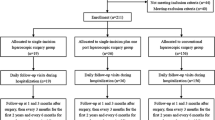
We compared postoperative pain among patients from the SLC group (n = 11) with those from the MLC group (n = 11) who underwent laparoscopic surgery for colon cancer at our institution between May and October 2013. Patients were specifically matched for gender, age, body mass index, tumor size, and performance status. Postoperative pain was evaluated at rest and during mobilization, using a visual analog scale (VAS) on postoperative days (PODs) 1–7, and by postoperative frequency of analgesics; pain intensity was evaluated at rest, using the Pain Vision™ system on PODs 1–7. Other operative outcomes of the two groups were also recorded.
Results
Patient demographics, operative outcomes, time duration before first flatus, and C-reactive protein and WBC count on POD 1 showed no significant differences between groups. Results of sequential VAS during mobilization until POD 7 were significantly less in the SLC group than in the MLC group (p = 0.009). However, sequential VAS at rest did not differ between the two groups (p = 0.11). Measured with the Pain Vision™ system, the difference in pain intensity at rest was statistically significant for the postoperative period (p = 0.003). Total requests for analgesics until POD 7 were reduced in the SLC group compared to that in the MLC group, but lacked statistical significance (three vs. seven, respectively, p = 0.07).
Conclusions
In both quantitative and objective measurements using the Pain Vision™ system, SLC significantly reduced postoperative pain. SLC is a promising procedure, associated with less invasiveness than MLC.





Similar content being viewed by others
References
Jacobs M, Verdeja JC, Goldstein HS (1991) Minimally invasive colon resection (laparoscopic colectomy). Surg Laparosc Endosc 1:144–150
Veldkamp R, Kuhry E, Hop WC, Jeekel J, Kazemier G, Bonjer HJ, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy AM (2005) Laparoscopic surgery versus open surgery for colon cancer: short-term outcomes of a randomised trial. Lancet Oncol 6:477–484
Schwenk W, Haase O, Neudecker J, Muller JM (2005) Short term benefits for laparoscopic colorectal resection. Cochrane Database Syst Rev 20(3):CD003145
Tjandra JJ, Chan MK (2006) Systematic review on the short-term outcome of laparoscopic resection for colon and rectosigmoid cancer. Colorectal Dis 8:375–388
Fleshman J, Sargent DJ, Green E, Anvari M, Stryker SJ, Beart RW, Hellinger M Jr, Flanagan R Jr, Peters W, Nelson H (2007) Laparoscopic colectomy for cancer is not inferior to open surgery based on 5 year data from the COST Study Group trial. Ann Surg 246:655–662; discussion 662–654
Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10:44–52
Jayne DG, Thorpe HC, Copeland J, Quirke P, Brown JM, Guillou PJ (2010) Five-year follow-up of the Medical Research Council CLASICC trial of laparoscopically assisted versus open surgery for colorectal cancer. BJS 97:1638–1645
Remzi FH, Kirat HT, Kaouk JH, Geisler DP (2008) Single-port laparoscopy in colorectal surgery. Colorectal Dis 10:823–826
Bucher P, Pugin F, Morel P (2008) Single port access laparoscopic right hemicolectomy. Int J Colorectal Dis 23:1013–1016
Kim SJ, Ryu GO, Choi BJ, Kim JG, Lee KJ, Lee SC, Oh ST (2011) The short-term outcomes of conventional and single-port laparoscopic surgery for colorectal cancer. Ann Surg 254:933–940
Takemasa I, Uemura M, Nishimura J, Mizushima T, Yamamoto H, Ikeda M, Sekimoto M, Doki Y, Mori M (2013) Feasibility of single-site laparoscopic colectomy with complete mesocolic excision for colon cancer: a prospective case-control comparison. Surg endosc 28(4):1110–1118
Leblanc F, Champagne BJ, Augestad KM, Stein SL, Marderstein E, Reynolds HL, Delaney CP (2010) Single incision laparoscopic colectomy: technical aspects, feasibility, and expected benefits. Diagn Ther Endosc 2010:913216
Trichak S (2003) Three-port vs standard four-port laparoscopic cholecystectomy. Surg Endosc 17:1434–1436
Poon CM, Chan KW, Lee DW, Chan KC, Ko CW, Cheung HY, Lee KW (2003) Two-port versus four-port laparoscopic cholecystectomy. Surg Endosc 17:1624–1627
Gupta A, Shrivastava UK, Kumar P, Burman D (2005) Minilaparoscopic versus laparoscopic cholecystectomy: a randomised controlled trial. Trop Gastroenterol 26:149–151
Kumar M, Agrawal CS, Gupta RK (2007) Three-port versus standard four-port laparoscopic cholecystectomy: a randomized controlled clinical trial in a community-based teaching hospital in eastern Nepal. JSLS 11:358–362
Cerci C, Tarhan OR, Barut I, Bulbul M (2007) Three-port versus four-port laparoscopic cholecystectomy. Hepatogastroenterology 54:15–16
Champagne BJ, Papaconstantinou HT, Parmar SS, Nagle DA, Young-Fadok TM, Lee EC, Delaney CP (2012) Single-incision versus standard multiport laparoscopic colectomy: a multicenter, case-controlled comparison. Ann Surg 255:66–69
Poon JT, Cheung CW, Fan JK, Lo OS, Law WL (2012) Single-incision versus conventional laparoscopic colectomy for colonic neoplasm: a randomized, controlled trial. Surg Endosc 26:2729–2734
Fung AK, Aly EH (2012) Systematic review of single-incision laparoscopic colonic surgery. BJS 99:1353–1364
McCormack HM, Horne DJ, Sheather S (1988) Clinical applications of visual analogue scales: a critical review. Psychol Med 18:1007–1019
Seymour RA (1982) The use of pain scales in assessing the efficacy of analgesics in post-operative dental pain. Eur J Clin Pharmacol 23:441–444
Babul N, Darke AC, Johnson DH, Charron-Vincent K (1993) Using memory for pain in analgesic research. Ann Pharmacother 27:9–12
DeLoach LJ, Higgins MS, Caplan AB, Stiff JL (1998) The visual analog scale in the immediate postoperative period: intrasubject variability and correlation with a numeric scale. Anesth Analg 86:102–106
Jefferson JK (1998) Electrodiagnostic functional sensory evaluation of the patient with pain: a review of the neuroselective current perception threshold and pain tolerance threshold. Pain Digest 8:219–230
Shimazu H, Kobayashi H, Seno S, Kato S, Akimoto M, Aizawa S et al (2004) Quantitative Analysis of the Degree of Pain Using Pain-less Electrical Stimuli. 11th International Pain Clinic World Society of Pain Clinicians 451–455
Osada K, Oka H, Isomura T, Nakamura I, Tominaga K, Takahashi S, Kojima A, Nishioka K (2011) Development of the Japanese version of the fibromyalgia impact questionnaire (JFIQ): psychometric assessments of reliability and validity. Int J Rheum dis 14:74–80
Lee HJ, Seo JC, Kwak MA, Park SH, Min BM, Cho MS, Shin I, Jung JY, Roh WS (2014) Acupuncture for low back pain due to spondylolisthesis: study protocol for a randomized controlled pilot trial. Trials 15:105
Matsumura H, Imai R, Gondo M, Watanabe K (2012) Evaluation of pain intensity measurement during the removal of wound dressing material using ‘the PainVision system’ for quantitative analysis of perception and pain sensation in healthy subjects. Int Wound J 9:451–455
Ota S, Ogawa K, Shimbori H, Oki H, Nakahashi Y, Goto T (2009) Application quantitative measurement device for perception and pain (Pain Vision) to pharmacological challenges. Pain Clin 30:209–214
Takemasa I, Sekimoto M, Ikeda M, Mizushima T, Yamamoto H, Doki Y, Mori M (2010) Video. Transumbilical single-incision laparoscopic surgery for sigmoid colon cancer. Surg Endosc 24:2321
Makino T, Milsom JW, Lee SW (2012) Feasibility and safety of single-incision laparoscopic colectomy: a systematic review. Ann Surg 255:667–676
Papaconstantinou HT, Sharp N, Thomas JS (2011) Single-incision laparoscopic right colectomy: a case-matched comparison with standard laparoscopic and hand-assisted laparoscopic techniques. J Am Coll Surg 213:72–80; discussion 80–72
Chen WT, Chang SC, Chiang HC, Lo WY, Jeng LB, Wu C, Ke TW (2011) Single-incision laparoscopic versus conventional laparoscopic right hemicolectomy: a comparison of short-term surgical results. Surg Endosc 25:1887–1892
Chew MH, Chang MH, Tan WS, Wong MT, Tang CL (2013) Conventional laparoscopic versus single-incision laparoscopic right hemicolectomy: a case cohort comparison of short-term outcomes in 144 consecutive cases. Surg Endosc 27:471–477
Lu CC, Lin SE, Chung KC, Rau KM (2012) Comparison of clinical outcome of single-incision laparoscopic surgery using a simplified access system with conventional laparoscopic surgery for malignant colorectal disease. Colorectal Dis 14:e171–e176
Moraca RJ, Sheldon DG, Thirlby RC (2003) The role of epidural anesthesia and analgesia in surgical practice. Ann Surg 238:663–673
Wolthuis AM, Penninckx F, Fieuws S, D’Hoore A (2012) Outcomes for case-matched single-port colectomy are comparable with conventional laparoscopic colectomy. Colorectal Dis 14:634–641
Stener-Victorin E, Kowalski J, Lundeberg T (2002) A new highly reliable instrument for the assessment of pre- and postoperative gynecological pain. Anesth Analg 95:151–157, table of contents
Lahoda R, Stacher G, Bauer P (1977) Experimentally induced pain: measurement of pain threshold and pain tolerance using a new apparatus for electrical stimulation of the skin. Int J Clin Pharmacol Biopharm 15:51–56
Disclosures
The authors have declared that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hiraki, M., Takemasa, I., Uemura, M. et al. Evaluation of invasiveness in single-site laparoscopic colectomy, using “the PainVision™ system” for quantitative analysis of pain sensation. Surg Endosc 28, 3216–3223 (2014). https://doi.org/10.1007/s00464-014-3594-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3594-7